A decade before last year’s Ebola epidemic, the United States Department of Defense embarked on a research program that eventually produced a promising drug to treat the disease, one that was fast-tracked for review by the Food and Drug Administration. Then, in late 2012, a year and a half before the first case of Ebola was reported in West Africa, the program was abruptly halted, the victim of political brinksmanship in Congress.
The U.S. government’s interest in Ebola treatments intensified in 2004, when a virologist at Fort Detrick in Frederick, Maryland, was quarantined because of the virus. She was working at an army laboratory designated “biosafety level 4”—a lab equipped with the highest level of precautions needed to isolate dangerous biological agents—with mice that had been infected with the Ebola virus. While injecting them with immune globulin, the fifth mouse fought back—kicking the syringe and pushing the needle through the woman’s gloves and into her left hand.
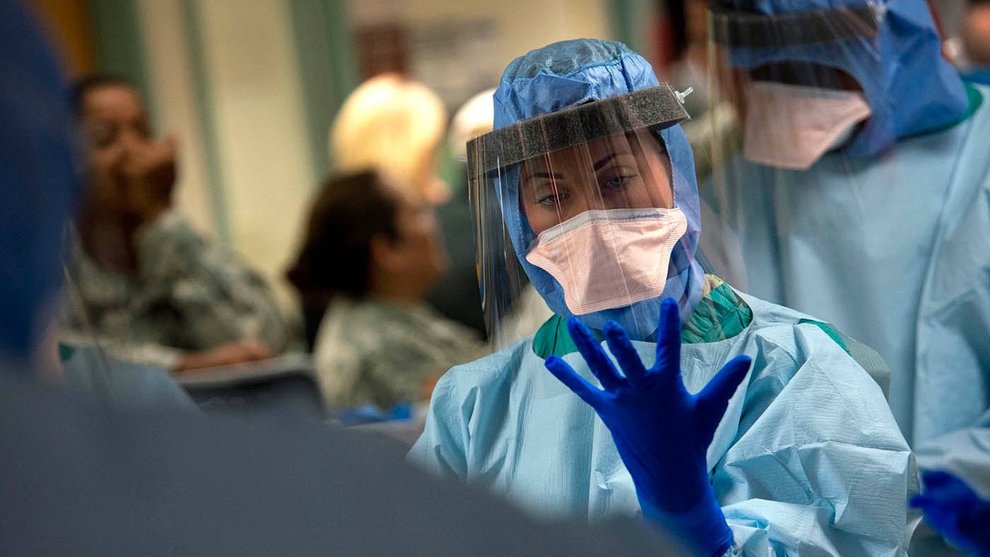
The virologist spent 21 days in isolation in “the slammer,” a 1,288-square-foot medical containment suite complete with its own ventilation system, air-tight doors, and three levels of containment through which food and supplies passed.
During those 21 days, the United States Department of Defense reached out to Sarepta Therapeutics, a small pharmaceutical company based in Cambridge, Massachusetts, that focuses on developing drugs for rare diseases. The department wanted to know if Sarepta could quickly turn around an emergency treatment if the scientist were to contract Ebola.
“The company worked over the weekend, and in about five or six days, Sarepta was able to synthesize several compounds, enough drug material to administer in this woman,” says Chris Garabedian, who was chief executive officer of Sarepta Therapeutics from 2011 to 2015. The drug was given emergency approval by the U.S. Food and Drug Administration and was ready for use.
But the scientist didn’t end up contracting Ebola and was eventually released. Sarepta’s experimental drug went unused.
After that close call, the Department of Defense continued to work with Sarepta to develop a drug that could cure Ebola. By 2010, Sarepta landed a $291 million contract for the advanced development of the company’s virus therapeutic candidates for Ebola and Marburg, a similar hemorrhagic fever.
The research would lead to a promising drug candidate that, like many other drugs for rare diseases, would be abandoned before its potential could be fully understood. In 2012, Sarepta’s therapeutic become the first Ebola drug candidate to be given fast-track designation by the FDA, a designation meant to expedite the review of a drug that addresses a serious condition and fills an unmet medical need. One month later, as Congress was locked in a standoff over the debt ceiling and the federal government faced austere budget cuts, development of the promising Ebola treatment was suddenly halted.
The Bioterrorism Threat
Ebola has been classified as a Category A bioterrorism threat by the U.S. Centers for Disease Control and Prevention (CDC) since at least 2004. The status was supposed to help prepare the government, scientific, and medical community for a potential outbreak, according to Adel Mahmoud, a senior policy analyst and professor of molecular biology at the Woodrow Wilson School of Public and International Affairs at Princeton University.
“The U.S. government has identified Ebola as a threat,” Mahmoud says. “You knew by the end of the 20th century that you have a potential to make a vaccine for that virus. Why didn’t it go beyond that?”
Mahmoud isn’t alone in wondering why an Ebola therapeutic has taken so long. Dr. Daniel Bausch, a leading doctor in infectious disease medicine and a frequent consultant for the World Health Organization, has spent years waiting for a vaccine or cure. “It’s been frustrating for me being in the field in Africa over the course of outbreaks dating back decades and people saying, ‘What about a vaccine for Ebola?’—and me saying for ten years, ‘Oh, we actually have a vaccine that looks pretty good in animal models, but it just languished there because of course there was no real economic incentive,’ ” Bausch says. “If you were going to start at the beginning and say we want to have a research and public health program that is designed to maintain or improve people’s health, you wouldn’t design the system as we have it right now.”

Today, people stricken with Ebola can be given only supportive care, which consists of keeping patients hydrated and treating their symptoms in the hope that their immune system can fight off the virus. Since the most recent outbreak, which has killed more than 11,300 people, the world still has no approved treatments or vaccines for the disease.
That’s partially because the way we develop drugs and vaccines is expensive and cumbersome. It can take 12 years from when a drug is patented to when it is available commercially, and the average cost of taking one drug from concept to market is estimated to reach over a billion dollars. Less than 8% of all new drugs and vaccines in preclinical trials ever reach consumers.
When it comes to luring investors for something like an Ebola drug, “there’s no way you can really make a case for it,” says Steve Brozak, a biotech analyst and founder of WBB Securities. “These are doomsday products,” he says. “Nobody wants them. The irony is, when you really need them, there’s no price that you won’t pay for them.”
The World Health Organization (WHO) has a list of 17 similarly “neglected” tropical diseases that impact mostly the poorest populations in the world. The 1.2 billion people living in extreme poverty today comprise nearly a fifth of the world’s population—but since they make less than $1.25 a day, they’re easily overlooked by for-profit companies.
Because treatments for diseases like Ebola have failed to attract investors, the United States government has become the biggest funder of research and development for neglected and emerging infectious disease. But even federally funded research is often abandoned before a complete product can be developed and rolled out.
If a disease occurs in sporadic, unpredictable patterns and in poor communities, “these two things are a toxic mix,” says Dr. Manica Balasegaram, director of Doctors Without Borders’s Access Campaign.
Most drug and vaccine candidates, and particularly those for neglected diseases, languish in what’s called the pharmaceutical “valley of death”—the transition between basic research and product development that many potentially life-saving drug candidates never come out of. “What you see is underinvestment and investment taking a long time to produce results,” Balesagaram says. That track record is not only killing promising drugs, it’s taking a deadly toll on people whose lives depend on a cure.
“Protect the Warfighter”
Neglected diseases tend to be picked up by interests that may have motivations other than public health, another byproduct of the “toxic mix” Balasegaram describes. In the case of Ebola, he says, “big money came from biodefense.”
The Pentagon’s interest in biodefense began in the 1990s when the U.S. learned about a Soviet biological and chemical weapons program. Then the world faced a series of bioterrorism threats, including a sarin attack on the Tokyo subway in 1995 and an anthrax attack in Washington, D.C., in 2001. Since then, both the Pentagon and the Department of Health and Human Services have kept a running list of biological threats and have housed programs to create defensive drugs.
The Department of Defense is the only U.S. government agency that oversees research from basic science all the way through to product development. Over the past century, the Department of Defense has been involved in the development of one in every four vaccines approved by the FDA, including vaccines for polio, mumps, measles, typhoid, meningitis and yellow fever. The National Institutes of Health has a history of Ebola research and has pursued the development of a vaccine since 1999. However, research within the NIH is typically focused on understanding a disease rather than advanced drug or vaccine development.
Sarepta’s Ebola research was part of a little-known program within the Department of Defense called the Transformational Medical Technologies Initiative, or TMTI as it was called. At the time, the company’s $291 million agreement was the largest contract the Pentagon had funded through the then-new initiative.
The initiative’s mission was to “protect the Warfighter” from biological threats through the development of medical countermeasures, according to a planning briefing presented to industry.
“The infectious disease threat keeps evolving,” says Commander Franca Jones, the director of medical programs at the Department of Defense. “Our program tries to focus on looking at countermeasures against threats that we know exist as well as trying to anticipate emerging threats in the future.”
The program was also meant to streamline the drug development process and support research all the way through to FDA approval. The hope was that the department would be able to create a drug more quickly than in the past, Jones says.
TMTI was supposed to move fast enough to produce an H1N1 drug candidate in just one week, for instance. In 2009, Sarepta completed a “rapid response exercise” for the program—it was the only pharmaceutical company that participated. The drill was meant to demonstrate both the company’s and the Department of Defense’s ability to respond to a real-world threat of emerging infectious disease or biological terrorism. Sarepta turned around a drug candidate for H1N1 in seven days and later completed rapid response exercises for dengue virus and two other undisclosed microbes.
Sarepta was making impressive strides in its ongoing Ebola research, too. The company’s drug showed a 60–80% survival rate in primates infected with Ebola. It progressed into Phase I clinical trials where the drug was given to healthy volunteers at increasing doses. It proved to be safe in human beings.
In September 2012, Sarepta’s drug, AVI-7537, received fast-track designation by the FDA—a major milestone that would expedite the approval process for the drug. Over $89 million federal dollars had already been spent on Sarepta’s Ebola and Marburg program.
But federally funded research is vulnerable to political upheaval, and in October progress came to an abrupt stop. With the fiscal cliff looming, the Department of Defense terminated the Ebola portion of its contract with Sarepta. “Ultimately there was a decision made to end the relationship,” Jones says. “Not because there was anything wrong with their countermeasure,” she adds. “There were cost constraints that were not rectifiable.”
Unlike many other drugs, it wasn’t the results of clinical trials that killed AVI-7537, but the fallout from a game of political brinksmanship.
The Scramble for a Cure
Nearly two years later, in the summer of 2014, the world was in the middle of the worst Ebola outbreak in history. With thousands dying in the span of months, scientists were racing to bring successful drug and vaccine candidates through clinical trials.
“I went on the news telling the world we had the drug and we were ready,” says Garabedian, the former Sarepta CEO. Although Sarepta had halted its Ebola program, the company had enough of its experimental drug left to treat up to two dozen patients within a week. In a few months, the company thought it could manufacture enough doses for 100 patients. AVI-7537 was a leading candidate in potential Ebola treatments.
Sarepta said all that it needed to move forward was funding and FDA approval. Garabedian says executives approached the White House, the Department of Defense, the CDC, and the FDA about the possibility of using AVI-537 during the outbreak, but there were no takers.
Instead, federal money flowed to the experimental drugs ZMapp and TKM-Ebola. Both had been funded by the Department of Defense and, unlike Sarepta, had active contracts that survived 2012’s fiscal cliff debacle.
TKM-Ebola, created by the Canadian company Tekmira, was a direct competitor to Sarepta’s drug and was also part of TMTI. At the time that Sarepta’s work on its Ebola drug was halted, the company was also working on a drug for Marburg, a similar hemorrhagic fever. Sarepta’s Marburg research was further along than its Ebola program, with successful safety trials in healthy humans and a 100% survival rate in Marburg-infected, non-human primates. Sarepta’s Marburg and Ebola candidates both used the same basic chemistry—they block the production of a protein to prevent the virus from replicating in its host.
Garabedian and biotech analysts speculate that the Pentagon didn’t want to rely on one technology for both viruses. It kept Tekmira’s program alive while axing Sarepta’s Ebola contract, allowing it to maintain a Marburg program through Sarepta and an Ebola program through Tekmira. At the time of the decision, TKM-Ebola was a strong candidate with a 100% survival rate in Ebola-infected monkeys, though the FDA briefly placed a hold on the drug due to concerns about how safe higher doses would be in humans.
Another company’s drug, ZMapp, received a lot of attention after being administered to Americans who contracted Ebola and then survived. Last month, the drug was given fast track designation by the FDA. The drug, produced by Mapp Biopharmaceutical, a small company supported by the Pentagon and the National Institute of Allergy and Infectious Diseases, was in limited supply during the Ebola outbreak. It soon ran out after treating the two Americans because the way the drug is produced—using tobacco plants—is difficult to scale up quickly.
Some think that Sarepta had advantages over the other drugs. “ZMapp was a very elegant product, but the manufacturing was quite exotic, whereas Sarepta could have—in theory—been manufactured fairly quickly by comparison,” says Brozak, the WBB analyst. “Sarepta was much more advanced,” he says.
At the time of the Ebola outbreak Sarepta was in late-stage clinical trials for its lead drug, a treatment for Duchenne muscular dystrophy, and some have contended that the company’s experience made them more likely to succeed in manufacturing and scaling up production.
Sarepta’s advantage, according to Brozak, was “understanding how to deal with new types of therapeutics, understanding what you need to do to develop them, to test them, to manufacture them, and then to deliver them.”
Tekmira tested its drug in Sierra Leone in the midst of last year’s outbreak, but shut down clinical trials after results failed to show efficacy. Soon after, the company changed its name to Arbutus Biopharma Corp., stopped its work on Ebola, and announced that it would focus on hepatitis B instead.
In Sarepta’s annual report for 2014, the company stated that it was exploring possibilities for funding to further its Ebola research. The Pentagon told me that it had extended an invitation to Sarepta in April this year to submit a proposal for Phase II clinical trials of its Ebola drug, shortly after Garabedian left the company. However, the company’s new leadership chose not to continue with AVI-7537 and is instead focusing on a commercial drug for Duchenne muscular dystrophy. Sarepta has refused repeated requests for comment.
TMTI has ended, although similar activities have been absorbed by other agencies within the Department of Defense. None of the drugs funded by the program ever reached FDA licensure. TMTI’s rapid response exercises that were supposed to prepare the U.S. for a real-world threat exactly like last year’s epidemic proved to have significant failings. The exercises created candidate drugs in a matter of days, but they only produced enough to treat one patient. “The part the exercises did not address is if there was a true pandemic, you need thousands of doses immediately. You would need the scale up manufacturing, and that’s something that was never funded,” Garabedian says.
Commander Jones believes the that TMTI’s main goal was to quickly develop a drug candidate for FDA approval in the midst of a crisis. “The issue with the TMTI program or programs like it, moving forward, is at the end of the day we need a platform that the FDA is comfortable with,” she says.
The FDA is admittedly cautious about approving the use of experimental drugs that haven’t proven to be safe and effective, especially over long periods of time. “We didn’t want to do anything that would undermine trust in medical products or vaccines by perhaps undermining the scientific validity,” says Dr. Luciana Borio, acting chief scientist with the FDA. “We haven’t quite figured a way to do trials very fast in an emergency. We did it as fast as we could as a community for Ebola, but can we make it even faster? That’s something I’d like to see us working toward as a global community.”
A Global Priority
Today, drug research for Ebola continues in West Africa. This summer, a vaccine candidate, VSV-EBOV, manufactured by the pharmaceutical companies NewLink Genetics and Merck, made headlines. Preliminary clinical trial results showed that the vaccine was 100% effective in protecting people from the disease.
In 2005, early trials of VSV-EBOV, showed 100 percent effectiveness in preventing monkeys from contracting the disease. Researchers hoped that the vaccine might be licensed by 2010 or 2011, the New York Times reported. But with no new funding, development of the vaccine was put on hold until last year’s deadly outbreak.
Still, experts worry that the world may not be ready if another large-scale Ebola epidemic occurs. In the scramble to find a cure, clinical trials were implemented in West Africa without much prior planning.
“Ultimately my fear is that we may not be prepared for the next one,” Commander Jones says. “We may not have enough data to have a licensed product,” she says. “So much of the population was treated with multiple drugs. We’ll never know what was really efficacious.”
The most promising drugs and vaccines—ZMapp, TKM-Ebola, and VSV-EBOV—all have roots in programs run by the Department of Defense. The world would have been much farther behind without the Pentagon’s history of research, but experts in the global health community warn that it’s not wise to rely on a single source of investment.
“With Ebola, big funding came from bio-threat biodefense, which would have then funded products with that particular lens and not necessarily for the public health needs in West Africa,” says Dr. Balasegaram, the Doctors Without Borders director.
All of the drug candidates funded by the Department of Defense were meant to protect deployed troops. Medical innovations developed within this context can trickle down, but they are designed with the military’s needs in mind, not necessarily those of the general public. Take Sarepta’s promising AVI-7537, for example. It was an injectable drug that needs to be refrigerated. This isn’t a problem in a developed country’s healthcare system, but it’s not ideal for places without a reliable electrical grid or for controlling an outbreak in Sierra Leone, Guinea, or Liberia.
“We argue that for global public health needs-driven research and development, we need to look at pooled funding that comes from all member states, not just U.S. This is an important part that, in itself, would allow us to determine priorities that are global in nature rather than looking at a more narrow perspective or need,” Balasegaram says. He co-authored an essay in the journal PLOS Medicine calling for a global biomedical research and development fund, and Dr. Mahmoud of Princeton co-authored an article in the New England Journal of Medicine with other health experts and the Wellcome Trust to propose a $2 billion vaccine development fund for infectious diseases, including Ebola and MERS.
Even the Department of Defense admits that it shouldn’t be alone in preparing for the next outbreak. “If we could figure out a way to globally sit around the table—maybe facilitated by the WHO—and think about all the threats we need to work on, then perhaps we would be in a better place when the next epidemic happens,” Jones says.
In the U.S., proposed legislation aims to increase funding for the NIH and make it easier for drug candidates to get to FDA approval. Although some worry that the legislation could make it easier for unsafe drugs to get licensed, The 21 st Century Cures Act passed in the House of Representatives with bipartisan support and is now under deliberation in the Senate.
“Just last year, we again witnessed the real threat that infectious diseases pose on humanity with the Ebola outbreak,” says Fred Upton, a Republican representative from Michigan who introduced the bill to the House. “Infectious and deadly diseases require a sustained research and development effort. With 21 st Century Cures, we are investing in the best and the brightest scientists with the goal of finding cures and treatments.”
When it comes to the next outbreak, the promise for a prevention or cure may already be underway. The question is whether the promise can be realized in time. “The reason you have two or three vaccine candidates today is not because we started from scratch. We just pulled stuff that’s in the freezer and started looking at it,” Mahmoud says.
“I would imagine there must be some potential vaccines that are sitting in freezers everywhere in the world.”
This article is part of the “ Next Outbreak ” series, a collaboration between NOVA Next and The GroundTruth Project in association with WGBH Boston.



