A hospital room may feel sterile, with its recycled air and scrubbed smooth surfaces. But underneath that antiseptic veil is a teeming, invisible world of microbes, the composition of which constantly changes.
Each new patient brings their own microbiome—the collection of bacteria and other microbes that live in and on the body—which they shed on the hospital bed, the television remote, and anything else they touch. Each nurse, doctor, and visitor that enters the room drops microbes, too. The tiny organisms also circulate through ventilation systems and travel through the air. Some come not from humans but water systems, heaters, and other human-made niche environments. Collectively, these microbes make up the built microbiome, which exists in a unique and dynamic form in every single building on the planet.

Not all microbes are bad, of course. Most are benign or even beneficial. But disease-causing agents are a constant in hospitals, and every day one out of 25 patients gets at least one inadvertent infection during their hospital stay.
Some researchers suspect that hospitals’ microbial ecosystems may influence the spread of pathogens, which in turn may affect human health. While the research is in early stages, it may lead to changes in hospital design or practice to promote healthier built microbiomes.
Broadening Focus
Researchers have been interested in microbes in hospitals since at least 1847, when Ignaz Semmelweis, a German-Hungarian doctor, discovered that medical students in a Vienna hospital were inadvertently transmitting puerperal sepsis from autopsy rooms to maternity wards, leading to high death rates. Semmelweis introduced mandatory hand washing, the first intervention for a hospital-acquired infection on record.
Since then, most work on microbes in hospitals has similarly focused on preventing outbreaks of specific pathogens, especially those that are dangerous to people who are already ill or have weakened immune systems. In 1976, for example, scientists first discovered the bacteria that cause Legionnaires’ Disease, Legionella pneumophila , after an outbreak at an American Legion convention in Philadelphia. The bacteria, which can cause fatal pneumonia, lived in the cooling tower of a hotel and circulated through the building’s air conditioning.
The pathogen can similarly thrive in in drinking fountains and hot water heaters, and is a particular concern in hospital water systems. Since its discovery, outbreaks have been identified in hospitals across the world. To prevent the bacteria from taking hold and spreading from its source to patients’ rooms, hospitals regularly clean and maintain ventilation systems and position cooling towers so that potentially infected air can’t circulate.
Today, other examples of hospital pathogens include black mold from the Stachybotrys genus, which may spark respiratory illness and can be controlled with ultraviolet sanitation systems, and the bacteria Clostridium difficile , which cause severe gastrointestinal distress and may be wiped out of contaminated rooms by robots spewing hydrogen peroxide vapor. Antibiotic resistant bacteria such as methicillin-resistant Staphylococcus aureus (MRSA), which can cause untreatable infections, may be tracked with genomic sequencing techniques. Finding the source of the bacteria with genetic maps to see how they mutate over time can encourage changes in behavior of hospital staff, such as taking extra care to wash hands and keeping infected patients quarantined.
But these bacteria and fungi do not live in a vacuum. They interact with other microbes just as a murderer may have a network of co-conspirators and bystanders who help or hinder their actions. Understanding these relationships can help illuminate the pathogen’s success or failure.
“What is new—and is critically important and interesting—is that some people are trying to understand the entire ecosystem instead of just the impact of pathogens,” explains Jonathan Eisen, an evolutionary biologist at the University of California, Davis who specializes in microbes in the built environment. “If we want to understand why MRSA is spreading in a hospital, we probably should understand the entire collection of microbes in the hospital.”
Early Steps
Eisen’s lab oversees the Microbiology of the Built Environment Network (microBEnet), an online resource that tracks around two dozen groups working to understand microbes not only in hospitals, but also in other built environments including various buildings, cars, and airplanes.
Although we spend around 90 percent of our time indoors, the microbiome of the built environment is one of the last that scientists have explored. Like other work that came before—including microbial research in the ocean, soil, and even humans—Eisen and his collaborators have benefited from advances in genome sequencing technology, which can identify an organism’s genetic code relatively quickly and cheaply. Swabbing a room and then running the samples through a sequencing machine can identify microbes, and tracking where the swabs came from can show where they live.
Some researchers are already using these techniques to explore hospital microbiomes. In 2012, researchers at the Biology and the Built Environment (BioBE) Center at the University of Oregon published a paper that looked at the microbial content of the air at Providence Milwaukie Hospital in Oregon. The researchers took air samples from hospital rooms that were ventilated either by open windows or mechanical systems and found that the former had greater bacterial diversity. But rooms that were mechanically ventilated and thus exposed to a smaller amount of outside air also had more bacteria related to human pathogens. While this doesn’t mean that an open window will definitely benefit a patient’s health, the work did demonstrate how different ventilation systems can impact a room’s microbial content.
People who spend time in a room may be affected by its microbiome, including non-pathogenic microbes. Earlier this year, a team led by researchers at the University of California, Berkeley published research that looked at the relationship between environmental microbes and babies in the neonatal intensive care unit at Magee-Womens Hospital of the University of Pittsburgh Medical Center.
Babies are typically colonized with the bacteria that prime their microbiome when they are born. But the premature infants in a neonatal unit are a special case—they are underdeveloped and often must be treated with antibiotics, which means their microbiomes may have a slow start. Although neonatal units are kept as sterile as possible to help prevent the babies from getting sick, the Berkeley researchers found that the microbes on various surfaces in the Pittsburg unit—mostly associated with human skin—were highly genetically similar to those in the gastrointestinal tracts of premature babies who lived in the unit during the first month of their life. The environmental microbes were likely colonizing the infants, just as a mother’s microbes would typically infiltrate their bodies during birth.
Similar scans of other hospital rooms, from where patients sleep to where they are treated, may reveal similar ways that people and the built environment swap microbes.
Vast Samples
Larger projects are on the way. The Hospital Microbiome Project , for example, recently wrapped up a year’s worth of data at the Center for Care and Discovery, a new hospital associated with the University of Chicago. Samples were collected daily in ten rooms virtually identical in terms of layout and ventilation.
“This is 15,000 samples in one environment with daily resolution across a year,” says Jack Gilbert, a microbial ecologist at the University of Chicago and one of the project’s leaders, “It will be one of the most microbially characterized environments on Earth.”

Gilbert’s team was able to start data collection after the hospital was built but before patients arrived, to see how the people changed the environment. The group also worked with building scientists including Brent Stephens from the Illinois Institute of Technology, who characterized key features of the building and designed ways to collect a broad range of environmental data that may play a role in the life of a microbe.
“What do we need to know about the building we’re sampling from a microbial perspective? There is a bunch of evidence that shows humans are a huge source of bacteria, and a lot of that is pretty new,” Stephens says. “So perhaps the number of people in these environments is important. And as far as survival on surfaces, we know that both temperature and humidity have a big influence on microbial communities.”
To collect all that information, Stephens’s team put several types of data loggers in each of the study rooms to measure temperature, humidity, pressure, and light. They also added infrared sensors to each doorway that, along with carbon dioxide sensors, could estimate how may different people entered the room on a daily basis.
Coupled with the genetic information that will identify specific bacterial species and their locations, the environmental data might reveal how these factors influence the microbes’ presence and growth.
Although a paper on the study likely won’t be published until at least 2015, Gilbert says the preliminary results show a huge boost in microbial diversity after the hospital started admitting patients, which is no surprise. Early results also suggest that the microbes in a hospital room might not only depend on how long a patient stays in the room but on what treatments the patient receives—how they are treated with antibiotics, for example, or whether they are going through chemotherapy. These different microbial ecosystems may influence how hospital-acquired infections spread.
“We think that the rest of the microbial community in the hospital impacts how pathogens are transferred in much the same way as when a pathogen that finds its way into a river suddenly finds itself surrounded by soil bacteria and often is outcompeted and unable to survive,” Gilbert says. “We think the same occurs in hospital environments. If there is a rich microflora, the pathogen can’t compete. But if that microflora is absent due to sterilization of the facilities, for example, it finds it can persist for a lot longer.”
It’s possible, then, that less sterile rooms could reduce the prevalence of harmful microbes. “More work has to be done to validate the hypothesis, but at least now we have the context of a very richly characterized hospital,” Gilbert says.
The Future of Hospital Design?
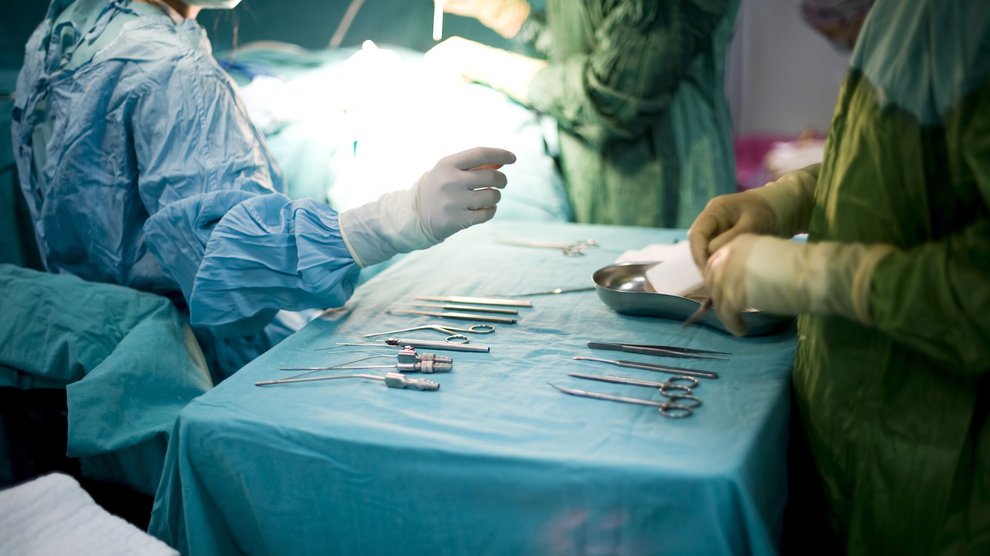
Of course, some parts of the hospital will always require careful sterilization, such as operating rooms. And in general, infection control is a major goal throughout any hospital. “We’re trying to kill all the pathogens,” says Nancy Iversen, the Director of Patient Safety and Infection Control at Billings Clinic in Montana. “That’s what we’re after in hospitals, we’re trying to kill them all and keep microorganisms out of the air and provide protected environments for our at-risk patients, largely because of outbreaks.”
While Iverson is intrigued by the implications of the built microbiome and the role of beneficial bacteria, she worries about patient safety. Plus, she adds, there are plenty of potential snags involving regulatory guidelines: “How would you get patients to enroll in studies where you didn’t disinfect traditionally under regulator standards—what the Centers for Disease Control requires, what these other bodies require regarding measures you take during construction and cleaning and air flow?”
Still, research on the built microbiome is already influencing how some architects think about building design. “The lens I use in looking at buildings has gained a new dimension since becoming part of this research,” says Jeff Kline, an architectural researcher and building scientist at the BioBE Center at the University of Oregon. “Now I’m understanding, at least a little bit, about how architectural decisions about building form, organization, materials, and systems, especially ventilation, provide mechanisms that affect the composition of indoor microbiomes.”
Kline adds that the research is too new to be applied to building design now. But there are intriguing possibilities for the future. Operating rooms and neonatal intensive care units may need to remain sterile, says Eisen from microBEnet, but it could be beneficial to allow a more diverse microbial ecosystem in, say, the room where a patient sleeps. There may also be better ways to control temperature, humidity, and airflow to encourage beneficial bacteria, or strategies to keep patients on intense antibiotic treatments away from those with compromised immune systems.
“I don’t think we know enough now about building microbial ecology to really say exactly what is going on or exactly what the optimal strategy is for design,” Eisen says. “But I think it’s fair to seriously question the strategy of trying to kill everything when there is no doubt that one of the worst places to be if you don’t want to get sick is a hospital.”

