After the initial shock of the Boston Marathon bombings wore off, many people began to wonder—quite rightly—what the future would hold for those who lost limbs in the explosions. In the past, the prognosis wouldn’t have been that promising. Amputees still have a long road ahead of them, but in recent years, amputation prostheses have come a long way. The technology still has its limitations, but you’d be surprised how well it can assist amputees in recovering their ability to work, participate in their favorite hobbies and pastimes, and otherwise go about their daily lives.
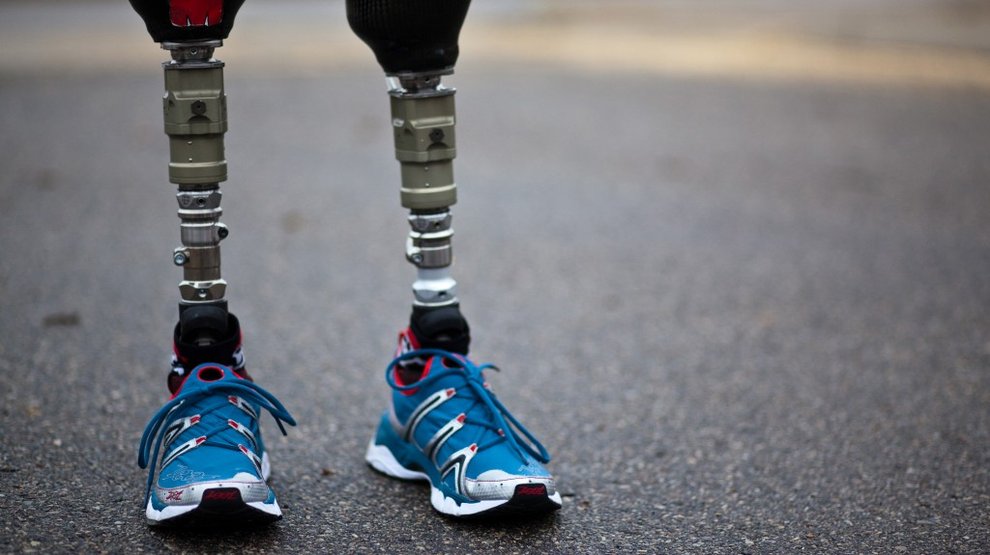
Successful assistive technologies, including amputation prostheses to replace lost limbs, are not mass-produced “cookie-cutter” technology. One size does not fit all, a fact that raises costs but also makes prostheses better suited to an individual’s body and activities. Regardless of their specific application, all amputation prostheses need to help a person move and sense. They also must be comfortable, and they should reasonably approximate the human form. Today, there are myriad different prostheses that address different needs, but they all have one thing in common—they’re better, in nearly every way, than their predecessors of just a decade ago.
Moving
An amputation prosthesis has to serve many functions, which vary depending on the limb it’s replacing and the context in which it’s used. Leg prostheses must provide mechanical support, shock absorption, balance and propulsion, while arm prosthesis must provide dexterity.
In the past, it wasn’t uncommon for someone to rely on a single, awkward prosthesis. Today, specialized prostheses allow users to swap one for another depending on what they want to do. For example, the sprinter Aimee Mullins uses “Cheetah legs” when she wants to go for a run. Though they look nothing like human legs, they absorb the energy of foot-ground collisions and return most of it, similar to how unimpaired tendons store and release elastic energy. Even the body’s metabolism can’t tell the difference—such running-specific prostheses enable leg amputees to jog with the same metabolic energy requirements as non-amputees. Although these prostheses perform well for running, they are not well suited to more mundane applications like driving a car or standing.
While we’ve made great strides with computer-controlled amputation prostheses, we still can’t match the versatility of an unimpaired limb. There are several reasons why, and many relate to the way our muscles work.
Our muscles’ primary function is to produce force and do mechanical work. For example, the muscles that drive the ankle provide more than half of the mechanical work required for unimpaired humans to walk on level ground. If those muscles are lost, as they are in trans-humeral (above-knee) and trans-tibial (below-knee) amputations, which are common among marathon bombing victims, something has to make up the difference. Some of that lower-limb ability to produce mechanical work can be provided by battery-powered motorized amputation prostheses.
But muscles do more than just generate force—they also absorb it in a controlled manner. To understand how, think about your arms when you’re riding a roller coaster. If you don’t tense your muscles, your arms will fly all over the place as the coaster twists and turns. By tensing your muscles, you can keep your arms from flapping about. In day to day life, muscle control is especially important when we use tools—such as driving a car—or when we walk by managing the collisions between the foot and the ground. Recently, scientists and engineers have been able to add this resistance to lower limb amputation prostheses, substantially improving their function.
Providing amputees with all the different ways you can move your limbs, known as degrees of freedom, is another major challenge. This is especially important for upper-extremity prostheses. The hand, for example, has tens of degrees of freedom alone. In general, more degrees of freedom mean more motors, more power required to drive them, and more mechanical complexity. Plus, you have to figure out how people are going to control them. Our field hasn’t solved all these problems yet, but we’re actively working it.
Sensing
A good amputation prosthesis doesn’t just let a person move, it should also help him or her sense the world around them. Humans are very good at interpreting patterns of pressure on the skin, a fact that we can use to our advantage. Even though the skin of a residual limb may be missing, skin on the point of contact for an amputation prosthesis can substitute. Properly designed amputation prostheses can transmit forces to the skin in a way that can make up for the loss of the limb. In one study, an amputee could position their prosthetic arm—with their eyes closed—just as well their unimpaired arm. Humans can be astonishingly adaptable.
To enable this level of performance, we have to ensure that the prosthesis transmits forces and pressures clearly and accurately. We’re still working on that. The most versatile and adaptable prostheses require motors, but due to friction and other undesirable mechanical behaviors, motorized prostheses tend to “blur” sensory information.
That brings us to another unfortunate tradeoff. How do we balance motor function against sensory acuity? Will it be more important for Adrianne Haslet, the dancer who lost her left leg below the knee, to know where on her foot her weight is concentrated? Or is it more important for her to be able to adjust her balance point by voluntary activity?
Someday soon, Haslet may not have to worry about that tradeoff. Recent advances in robotic motor technology promise to provide the best of both worlds. Engineers are developing motors that can change how they respond to mechanical perturbations and communicate those disturbances as mechanical stimuli to the skin. There’s another undeniably exciting possibility on the horizon—direct electronic connections with the nervous system. We know it’s possible, but we have to be cautious. Directly “reading from” or “writing to” the central nervous system, including the brain, is technically feasible but highly invasive. The risks for infection are high, and as a result it is only appropriate for patients with no reasonable alternatives for whom the risks may be acceptable.
Fortunately, most amputees can rely on muscle contractions, a simpler and safer way to sense and respond to the world around them. Each contraction is accompanied by electrical activity that is roughly proportional to the neural activity that excites the muscle. Muscle electrical activity can be easily and non-invasively measured by electronic sensors placed on the skin over the muscles, a technique known as electromyography, or EMG. It picks up and amplifies a copy of the neural activity sent to a muscle. The downside is that EMG relies on muscles the amputee isn’t using for something else, which typically leaves few options.
One workaround for upper-extremity amputees has been to take the brachial nerve plexus, which runs down your neck to your shoulder and supplies the entire upper extremity, and “reroute” it to the pectoral muscle. From there, the electrical activity of the re-innervated muscle can be easily monitored non-invasively. This makes it relatively easy to use neural commands to control the missing upper limb. Scientists have also discovered that sensory and motor nerves are often bundled in the same nerve plexus. In amputees, some of the rerouted nerves were sensory, too. As a result, after surgery, stimulating appropriate parts of the skin over the pectoralis muscle evoked sensations associated with mechanical stimulation of the missing limb. To the amputee, it feels as though the limb is still there.
Comfort
While easy to forget, comfort is critical in amputation prostheses. For those who have had a limb amputated, it’s easy to be reminded of the loss. Making a prosthesis as comfortable as possible can help the device do its job without being a bother. In practice, true comfort is remarkably difficult to achieve and maintain. The main challenge is to distribute forces and pressures on the skin. Human skin is a sophisticated organ that doesn’t tolerate sustained and concentrated pressures. It is also highly vulnerable to chafing, which tends to occur if the fit is too loose. Fortunately, we can now create precise, customized fits using computer-controlled fabrication.
But even with a good fit, we have to worry about perspiration. Allowing sweat to build up can lead to chafing and discomfort. To manage perspiration, we can turn to a wide range of materials that can absorb and disperse sweat from the surface of the skin. More than one of them may seamlessly be integrated into a single prosthesis, but they don’t solve the problem entirely. Comfort remains a challenge.
Moreover, comfort can be traded, at least in part, in favor of other benefits. Shoes provide a useful analogy. Though footwear is an ancient technology, finding comfortable shoes is a perennial challenge; most of us will tolerate some level of discomfort, at least temporarily, in favor of competing interests such as style.
Ideally, the best way to attach an amputation prosthesis is directly to the bone or bones of a residual limb. Though such an attachment has been demonstrated through research, it is not yet commonly available. Skin, again, is the main obstacle. To paraphrase the comedian Allan Sherman, skin is there to keep your outsides out and your insides in . Penetrating that barrier raises the risk of infection.
Comfort is a moving target. Comfort—or more accurately, our willingness to tolerate discomfort—changes with fatigue. That’s part of the reason why the weight of an amputation prosthesis is a major mechanical design challenge. The heavier a passive, low-tech limb prosthesis becomes, the greater the forces and pressures between the machine and the person, increasing fatigue. Motorized prostheses, however, can be heavier since they carry their own weight and then some by propelling their human wearer into each walking stride. Provided the additional weight doesn’t create undue pressure or discomfort, the upsides are huge.
Appearance
Appearance in prostheses is, like in other matters of taste, highly personal. Amputees from the marathon bombing will doubtless run the gamut, with some valuing appearance more than function and others less so. Again, multiple prostheses can help navigate the tradeoffs between comfort, function, and appearance. Shape and visual appearance are obviously critical to making a lifelike amputation prosthesis, but movement is just as important. A prosthetic limb that requires unseemly contortions is clearly less desirable.
The degree to which a prosthesis restores a person’s appearance is a moving target, too. We’ve found that a prosthetic wearer’s desire for a human-like appearance is inversely related to its functional performance. As prosthetic function improves, so does a wearer’s acceptance of their physical difference. Essentially, the better a prosthesis works, the less a person cares about its appearance. Using highly functional computer-controlled prostheses, prosthetic wearers often forgo the use of synthetic skin-like coverings, revealing the artificial part of their body in a proud display of titanium and electronics.
Prospects
People recovering from the trauma of the Boston Marathon bombings face many challenges. But in prevailing over adversity, they will also represent the best of the human spirit. Humans are spectacularly adaptable. Many of those who were hurt are accomplished athletes—distance runners, cyclists, dancers, and more—so they’ll certainly respond positively to this new challenge. They’re not alone in their recovery, either. The marathon bombing amputees have much in common with people recovering from stroke—an increasingly common disorder of our aging population—and with children coping with childhood disorders such as cerebral palsy. In both cases, appropriate robotic technology has been remarkably effective, and in the case of stroke, has been endorsed by the American Heart Association and by the U.S. Veteran’s Administration .
If there’s an important point to draw from this, it’s that anyone coping with a physical or mental challenge—due to a biomechanical injury such as limb loss or a neurological injury such as stroke—is essentially an athlete. What the rest of us might consider normal daily activities requires more of their physical and mental resources. Technology may help them meet this challenge, but ultimately it is their spirit which will prevail.



