Watch the Trailer
TB Silent Killer
Premieres March 25, 2014
FRONTLINE presents an unforgettable portrait of lives forever changed by tuberculosis, once thought to be a disease of the past
TB Silent Killer
Share
Tuberculosis was once thought to be a disease of the past. But with virulent new drug-resistant strains emerging faster than ever, TB — passed simply by a cough or a sneeze — is the second leading cause of death from an infectious disease on the planet. In TB Silent Killer, FRONTLINE presents an unforgettable portrait of the lives at the pandemic’s epicenter.
This documentary is no longer available to stream.
Produced by
Transcript
Credits
Journalistic Standards
Support provided by:
Learn More
Most Watched
The FRONTLINE Newsletter
Related Stories

WHO Report: TB Epidemic “Even Bigger Than We Thought”

How Can We Stop The TB Pandemic? Live Chat 3/26 3:30 pm ET
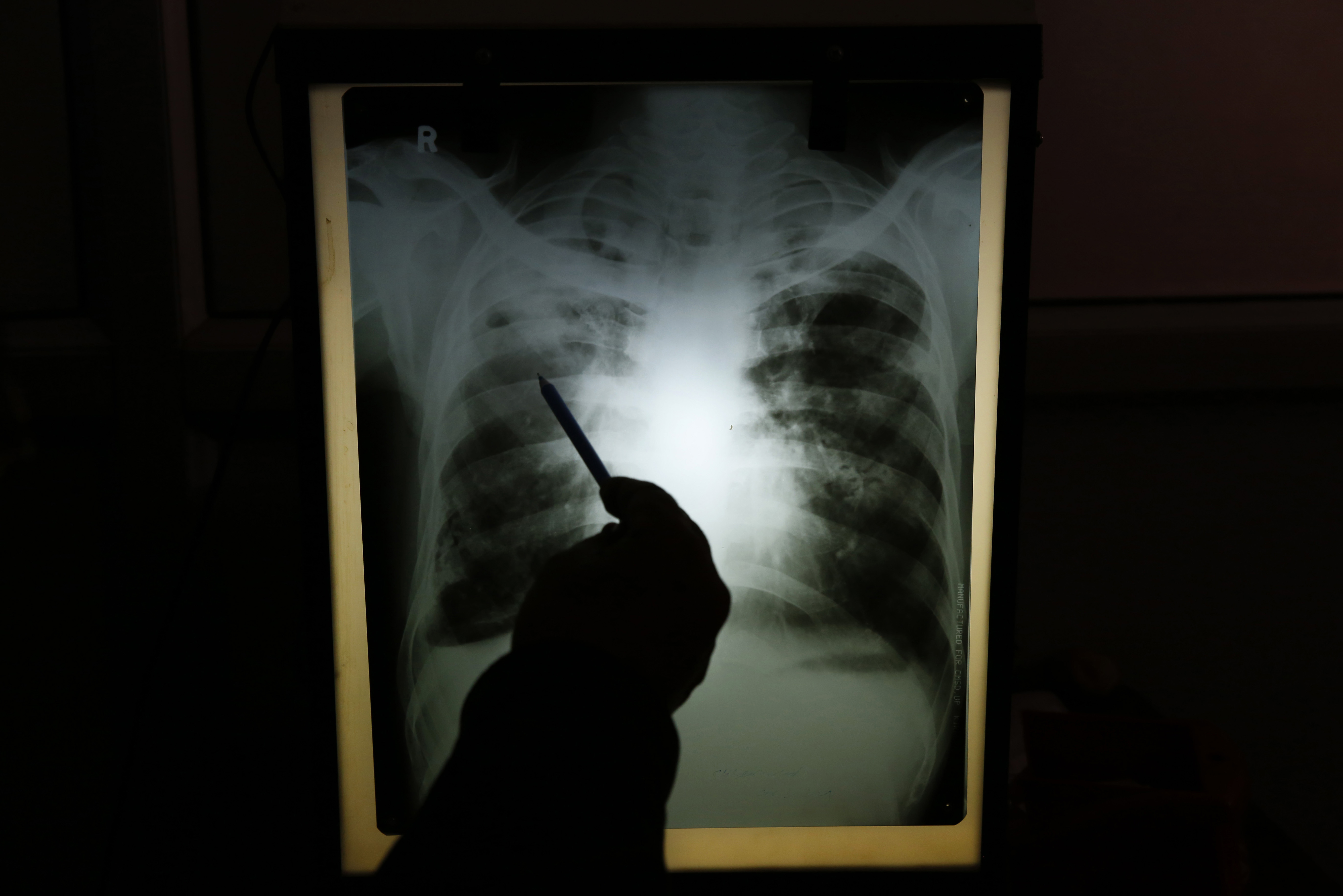
In Race Against TB, Testing Struggles to Keep Up
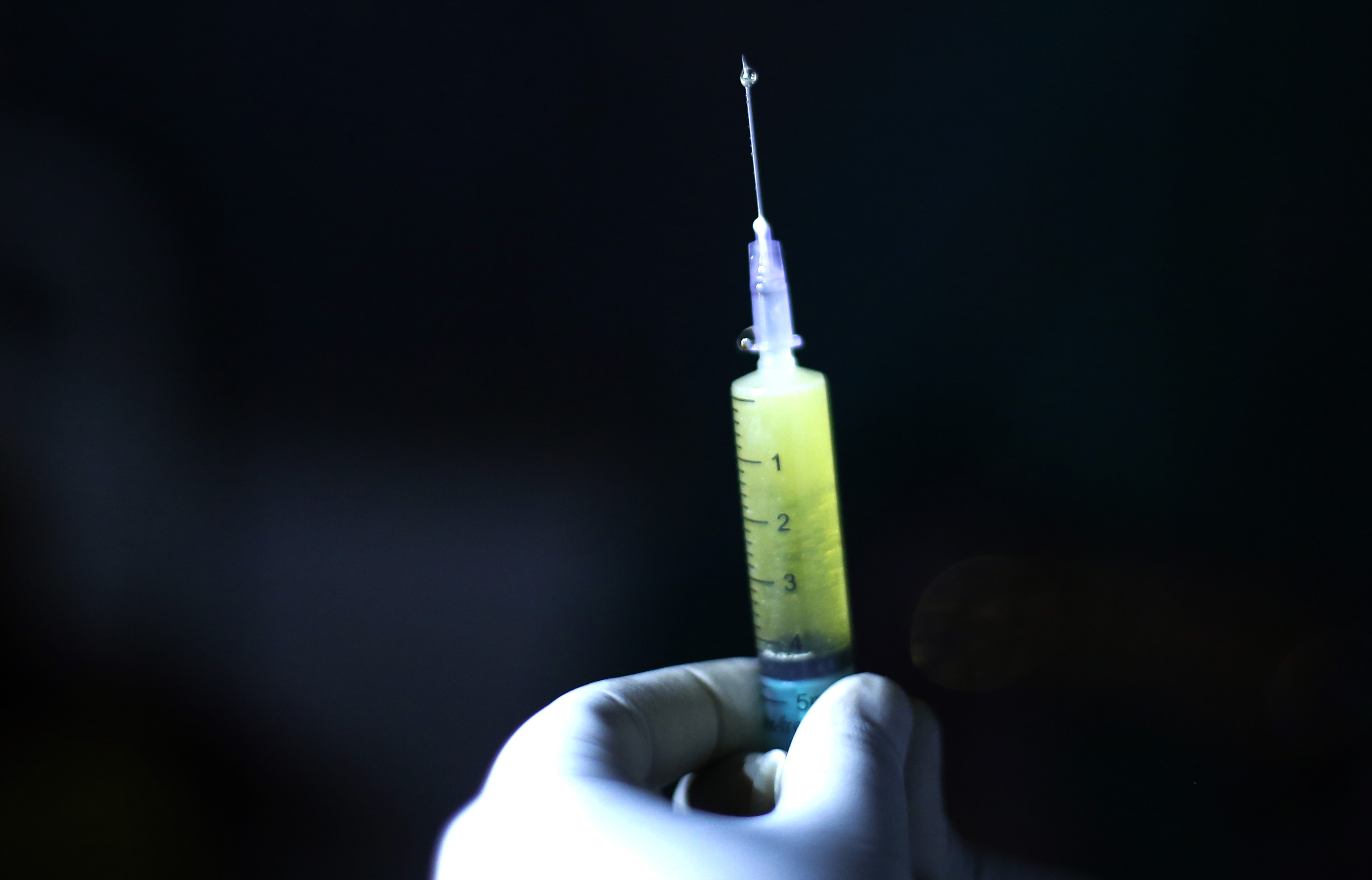
What’s the TB Threat in the U.S.?

Map: TB’s Global Reach
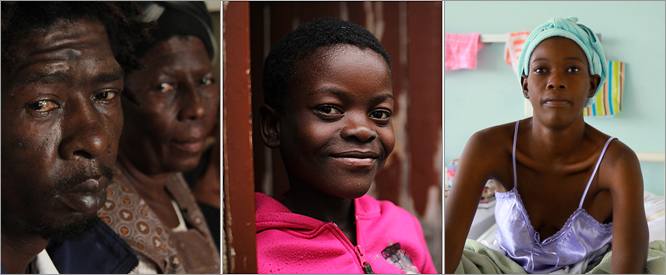
What’s Happened To Bheki, Nokubheka and Gcebile?

The Slow-Motion Search for a New TB Treatment

I Was the Man in the Mask
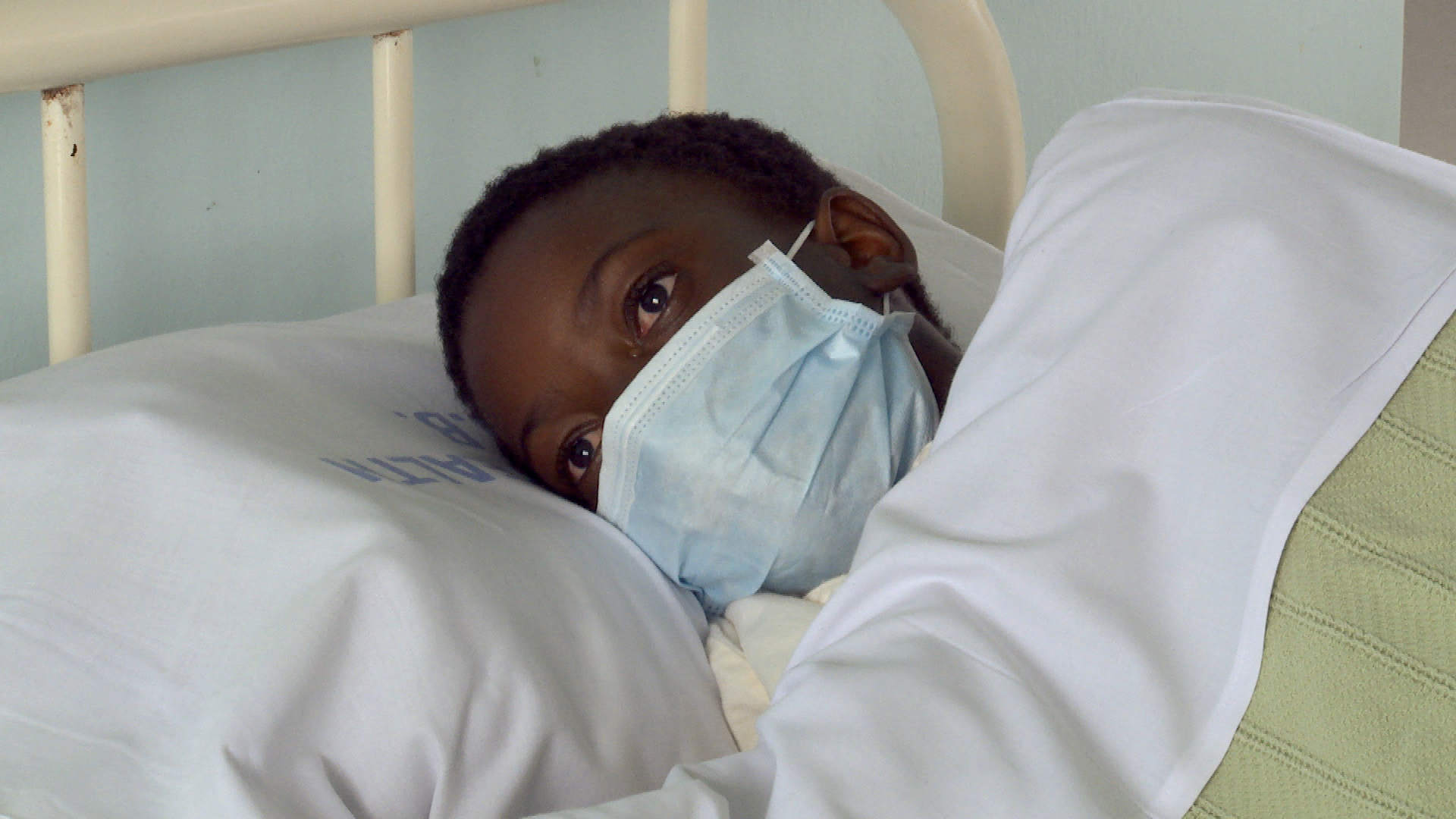
Childhood TB is Twice as Bad as Once Thought, Study Finds
Related Stories

WHO Report: TB Epidemic “Even Bigger Than We Thought”

How Can We Stop The TB Pandemic? Live Chat 3/26 3:30 pm ET

In Race Against TB, Testing Struggles to Keep Up

What’s the TB Threat in the U.S.?

Map: TB’s Global Reach
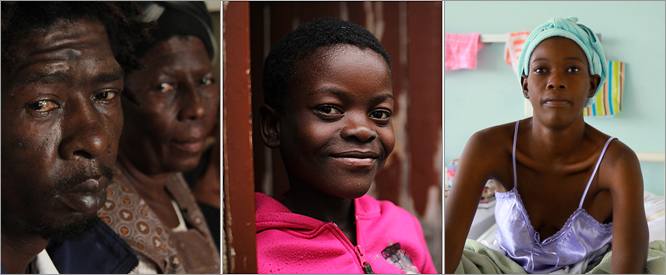
What’s Happened To Bheki, Nokubheka and Gcebile?

The Slow-Motion Search for a New TB Treatment

I Was the Man in the Mask

Childhood TB is Twice as Bad as Once Thought, Study Finds
PRODUCED BY Jezza Neumann Rebecca Stewart
DIRECTED BY Jezza Neumann
[Nokubheka, age 12, infected with one of the world’s deadliest diseases]
MELUSI: When they told me she had TB, I felt so miserable. TB is the disease that can kill my sister.
ANNOUNCER: Tonight, a FRONTLINE special presentation. From the valleys of Swaziland in southern Africa, the story of a brave community who let us into their lives to shed light on a new epidemic of a very old disease—
GCEBILE: They take us away from our homes so that we cannot be dangerous to the people outside.
ANNOUNCER: —a disease that is becoming resistant to treatment, and is spreading.
ERKIN CHINASYLOVA, M.D., Doctors Without Borders: Developed countries should be threatened by the worldwide spread of TB.
Dr. CHARITY NEWTON, National TB Hospital: Anyone can get TB. Anyone can die from TB.
ANNOUNCER: Intimate stories of people fighting to survive, stories of courage, loss, and hope that the world will pay attention.
Dr. ERKIN CHINASYLOVA: In the 21st century, we shouldn’t have people dying from TB.
ANNOUNCER: Tonight, TB Silent Killer
NARRATOR: Twelve-year-old Nokubheka lives here in Swaziland with her 17-year-old brother, Melusi. Recently, their mother died of tuberculosis, leaving them orphans.
NOKUBHEKA: [subtitles] People from church told her to go to hospital and gave her money. She then stayed in the hospital for ages. We would go visit her. Then eventually she died. Mother—now that she has left this earth, we have to do a lot of things ourselves. But we will never forget our mother. The empty space my mother left will never be filled. I think about her all the time.
MELUSI: [subtitles] Living alone is hard. Anyone my age would find it hard to take care of their little sister in this situation.
NOKUBHEKA: [subtitles] I love dancing and singing along to the song. When I’m dancing, I forget that my mother passed away. When I’m dancing, I feel happy and I don’t think about anything else. I love dancing.
My brother, Melusi, was told at the hospital that I have TB. I cough really hard at night and I sweat. I don’t feel myself sweating, I just wake to find the blankets soaked.
I think anybody can have TB. It’s not choosy. I’m young. I don’t know why it affects the young.
MELUSI: [in English] When they told me that she has TB, I felt so miserable, so dejected, so—so—so bad, because TB, I know TB. It’s a common disease, which destroys people. If TB isn’t treated, it can eventually kill the individual. TB is the disease that can kill my sister.
[reading to Nokubheka] One day a man was sitting on the tallest tree in the forest, forgetting he is the—
NARRATOR: Their mother died from a multi-drug-resistant mutation of tuberculosis known as MDR-TB. This form of the disease is far harder to treat. Melusi’s greatest fear is that Nokubheka may also have the drug-resistant strain. She is already being treated for regular TB. Today, the nurse is bringing news about her latest test results.
[subtitles]
NURSE MBINGO: When Nokubheka came to the hospital, we took her sputum and analyzed it to see what was causing the coughing. From that, we found she has TB. But we discovered have discovered that the TB is multi-drug-resistant. There is normal TB, and then there is MDR. So Nokubheka’s TB is MDR.
MDR-TB is not as easy to treat as the normal TB. She’ll have to have injections for a long time, for maybe four to six months.
MELUSI: I see.
NARRATOR: The brother and sister share one room, so to protect Melusi from catching the potentially lethal infection, Nokubheka now has to go and live in an isolation hospital two hours away.
MELUSI: Being in the hospital for months, does that mean no school?
NURSE MBINGO: Yes, that’s a problem.
How do you feel about going to the hospital? Nokubheka? We want you to go to hospital so they can take really good care of you, so you can have your injections and take all your pills properly. It’s important that you go to the hospital. Don’t cry. You will get well. You will get well, my love.
MELUSI: I think the injections are frightening her.
NURSE MBINGO: It’s important that she stays in the hospital until it’s less infectious. The hospital said the treatment is likely to take 18 months.
MELUSI: Almost two years.
NARRATOR: Swaziland now has the highest rate of TB infection in the world, partly because around a quarter of all adults are also HIV-positive. With so many people already living with weakened immune systems, tuberculosis has been spreading around the country.
Sixty miles south of the capital, near the border with South Africa, lives Bheki, a builder who loves soccer. Bheki recently learned that both he and his sister, Zandile, have MDR-TB.
BHEKI: [subtitles] I have never been employed. I survive by building. What’s worrying me now is that I have TB and that is affecting my work. My ability to work is going down.
Sometimes I go down to the soccer field and watch them training. I still go to soccer matches because I can still walk, but I can’t play. Soccer—there’s nothing like it. Separating me from soccer would be like separating me from my wife. Soccer is where I worship. Some people have their churches. My church is soccer. Soccer is in my blood. It’s in my blood. I won’t stop until I’m dead.
My sister is harder hit by the TB. It affects her a lot. I think with my sister, it was diagnosed late and had advanced a lot. She can hardly do anything. She needs help with everything.
ZANDILE: [subtitles] It is painful living with the disease. It’s really painful. You think back to the time before you had the disease, how you could run as far as you wanted whenever you liked. But now that’s impossible. I have no energy. Even standing up is a challenge. Every move has to be planned.
I’ve been on the treatment for two months. The biggest problem is that I vomit. I haven’t had some of the side effects that I see in other people. It’s just the weakness that affects me.
NARRATOR: Bheki and Zandile are unusual in being so open about their TB and also that they are HIV-positive. There is as great a stigma with TB as there is with AIDS in southern Africa, so many people here keep their diagnosis secret and delay getting treated. As a result, they risk continuing to infect those around them.
BHEKI: [subtitles] For us, it’s helped that our mother is a caregiver so we can talk about things here at home as a family. If people talked more openly, it would be easier to prevent the spread of this disease.
NICHOLIN DLAMINI, Mother of Bheki and Zandile: [subtitles] In 1990, I was trained for three months. The community leaders gave me a course on how to be a caregiver in the community. Diseases were not this bad then. It was just normal diarrhea and vomiting in children, and immunizing them.
As time went by, things started to get worse. AIDS came along. I worked so hard, I didn’t sleep day or night. People didn’t know they had to get tested and go to the clinic. Now there is this chest disease, and we didn’t see it coming. It’s not easily detected, even in the hospitals. It has spread far and wide. The work has started all over again.
[www.pbs.org: The challenges around testing]
NARRATOR: Although cases of TB have been falling worldwide in recent years, now new drug-resistant strains are emerging and spreading. As with HIV, the only effective way of tackling these drug-resistant strains is to use a combination of medications. But the treatment is complex and the side effects toxic. What’s more, because many countries lack good diagnostic testing, few people with multi-drug-resistant TB get the right treatment.
Bheki and Zandile are being treated by the relief group Medecins Sans Frontieres, Doctors Without Borders, which works closely with the Swazi government on TB management.
ZANDILE: I feel this month, unlike last month.
ERKIN CHINASYLOVA, M.D., Doctors Without Borders: What is better?
ZANDILE: I’m not vomiting as much.
Dr. ERKIN CHINASYLOVA: How often are you vomiting, like once a month or once a week?
ZANDILE: One—maybe once a week.
Dr. ERKIN CHINASYLOVA: Once a week?
ZANDILE: Yes.
Dr. ERKIN CHINASYLOVA: What else? Diarrhea?
ZANDILE: No.
Dr. ERKIN CHINASYLOVA: And you were complaining of cramps, pain in your leg.
ZANDILE: [subtitles] They are much better.
Dr. ERKIN CHINASYLOVA: Do you feel you’ve started gaining weight or not?
ZANDILE: [subtitles] I feel I’m gaining weight, but I can’t actually see it. But I feel all right.
Dr. ERKIN CHINASYLOVA: OK. Do you still have cough?
ZANDILE: No.
Dr. ERKIN CHINASYLOVA: Almost all our patients experience some side effects, adverse reaction of the treatment. In case of Zandile, she has been experiencing the most common side effect, like vomiting, for quite a long time. But she is eating now well, and she has got good appetite. She’s slowly gaining weight.
ZANDILE: [subtitles] There has always been TB. But this new MDR-TB really scares me. It’s spreading.
TENGETILE NSELE: [subtitles] My name is Tengetile Nsele. I’m a counselor here. I have been treated for MDR. I was treated for normal TB. I didn’t respond to the treatment, and then I was treated for MDR.
NARRATOR: The side effects of the treatment make many patients so ill that they stop taking their pills. But without treatment, the disease is almost always fatal. The clinic has support groups to encourage patients to stick with their medication, no matter how grim the side effects.
[subtitles]
TENGETILE NSELE: When you start taking the treatment, it seeks out the disease in the body. Your body feels like it’s being tortured because the pills are battling against the disease in your body. The pills are fighting at that point, telling the disease that they will conquer it. So you are bound to experience side effects because the body is being tortured.
BHEKI: How long after you start taking the pills do the side effects start?
TENGETILE NSELE: We are all different. We are not the same. Our bodies are different. We have to be patient with the treatment.
NARRATOR: Worldwide, around one in three people carry the TB bacteria but have strong enough immune systems so they don’t get sick. Multi-drug-resistant TB developed when patients who did get sick failed to get treated or complete their antibiotics. Now people are being directly infected with MDR-TB.
Living in one room with her sick mother, this is what happened to Nokubheka, so she’s being sent to an isolation hospital to protect her brother, Melusi, from being infected, as well.
NOKUBHEKA: [subtitles] This disease is bad because the way you get it is just by people breathing on each other. Then it gets into a person and means they have to leave this earth.
At school, we’re packed into the classrooms. When it’s cold, the teachers say we can’t open the windows. Then other people can be infected by the disease. There are lots of places you can get TB. You can get TB in a bus. If someone is infected and they cough, you get it, in a crowded shop or in a town where there are crowds.
[subtitles]
NURSE: She has TB, which is affecting her lungs. She has a TB infection which is drug-resistant. It requires strong drugs. The doctor says the drugs will include injections.
You will receive injections in your buttocks for six months.
MELUSI: Every day?
NURSE: Every day. On Christmas Day, New Year’s, every day.
MELUSI: Any holiday breaks?
NURSE: There are no holidays. She gets injections every day.
DOCTOR: [in English] The drugs we are going to give her to cure the TB have the side effects. She can have, let’s say, diarrhea, vomiting, stomach upsets, which she can get past. But she can have some side effects which are permanent, and the most fearsome is she can have problems with hearing. Some patients do experience permanent loss of hearing with the injection we are going to give.
NURSE: Do you understand? At times, you will hear a ringing noise in your ears. You must report it. Tell the doctor that there is a noise. Quickly, don’t wait. Do you understand?
Your brother will go home now. He will come visit you. You won’t cry, will you? He will come visit you.
DOCTOR: [in English] Be good, take your medication, and you’ll be OK.
NURSE: Say good-bye to the doctor.
DOCTOR: Bye-bye.
NURSE: Let’s go.
NARRATOR: Nokubheka will have to stay in the TB hospital for at least the first six months of her treatment. She will only go home if tests show she is no longer infectious.
[subtitles]
BHEKI: Zandile. I took this picture a long time ago. I was young. She’s changed a lot since then. Here’s another one. She’s not the same. I think she was already sick in this one.
FRIEND: You can see it in this one. If you look closely, you can see she was already sick.
BHEKI: She isn’t right. You can see it in her eyes. I believe that when she gets well, she’ll go back to being like this.
NARRATOR: Three months have passed, and Bheki is missing his sister, Zandile. She’s been taken to the local hospital. The side effects of her drugs have gotten worse and she’s lost too much weight. Their mother is looking after her.
NICHOLIN DLAMINI, Mother of Bheki and Zandile: [subtitles] She was vomiting continuously. No food would stay down. She vomits both pills and food. So the doctor stopped her TB pills so that she can gain some weight because her body could not take the pills. She was just too weak.
Dr. ERKIN CHINASYLOVA: In case of Zandile, she has been experiencing vomiting, but at the beginning, it was manageable. But recently, she vomiting worse, and like dramatically, and it became intractable, not responding to treatment. So that’s why she end up in the—in the hospital with dehydration, significant weight loss. She’s vomiting out the drugs, as well, and the drug concentration in her body is much less than it’s supposed to be.
So there are so many things you have to consider to take a decision to suspend TB treatment temporarily in order to stabilize her condition and to improve her nutritional status.
NARRATOR: Zandile’s doctor faces an impossible choice. If Zandile maintains TB treatment, she will continue to lose weight and fluids and may die. But suspending treatment means the infection might mutate into an even more drug-resistant form, which could also kill her.
Dr. ERKIN CHINASYLOVA: Do you have any complaints today?
NICHOLIN DLAMINI: [subtitles] Her knees are weak.
Dr. ERKIN CHINASYLOVA: Oh, she’s losing strength. Can she walk? She can’t walk.
NICHOLIN DLAMINI: [subtitles] She can’t walk when I’m not here.
Dr. ERKIN CHINASYLOVA: Because of here?
NICHOLIN DLAMINI: [subtitles] The strength is lost.
Dr. ERKIN CHINASYLOVA: To suspend the TB medication was a very difficult decision for me. We should not stop TB treatment. But also, if we keep continue giving the drugs, then we anyway, we put you at risk to die.
I want to check your weight.
ATTENDANT: [subtitles] Can she stand up straight?
ATTENDANT: [subtitles] Can she stand?
NICHOLIN DLAMINI: [subtitles] She’s trying.
ATTENDANT: [subtitles] Stand steady. Put your foot up, then the other one, too. Don’t look down, look up.
Dr. ERKIN CHINASYLOVA: Are you dizzy? No? You gained one KG.
NARRATOR: Bheki is also struggling with the side effects of the drugs. The treatment is so grueling, it’s estimated that fewer than half of those who start successfully complete it.
BHEKI: [subtitles] You have to kneel to do this job. My knees hurt too much. Dealing with manual jobs is hard. My knees—it bothers me every day, morning and evening. I’m not convinced that all these pills are going to make me better. The way things are going—I’m just doing it because they tell me that I’ll get well. Before, at least I could still kneel to build a house. Now I can’t do that.
Dr. ERKIN CHINASYLOVA: Bheki is not unusual. He’s not able anymore to do all the usual activities he used to do. And that’s—I think make—make him frustrated. He has a potential to get even depressed because of the treatment.
I think those who used to work and be active, and suddenly they become inactive, I’d say a huge difference in their lifestyle. And of course, they—it affects their mental and psychological condition.
BHEKI: [subtitles] I take almost 20 pills a day. If it were up to me, they should leave me to die. I don’t know which ones are causing me pain. And there are injections, too. It’s a real problem having to take so many pills.
NARRATOR: Nokubheka has been in isolation in the TB hospital for three months.
[subtitles]
NOKUBHEKA: Living here is boring. It’s boring. People are fenced in here like cows. I have to be patient so that I get well, finish the treatment so that I can go home. But staying here is not nice. Every morning, they inject me, and then I take some pills, just like that.
NURSE: OK, let’s take the pills.
NOKUBHEKA: I’ve taken them.
NURSE: You’ve taken them? [in English] Very good girl! [subtitles] You’re not going to vomit, are you? Let’s eat bread. What will you have to drink, juice?
NOKUBHEKA: Juice.
The food is not good here. It is not good because you eat the same thing every day, the same thing every day, every day, every day. So you don’t get fruit when you need it. No greens, no vegetables. They just give us soup.
Where are the leafy vegetables? Here is some ligusha. Let’s pick it. If only we had peanuts or butter. We need greens. We don’t have greens here at the hospital. We get meat and soup.
GCEBILE: [subtitles] There are greens, but we want vegetables we eat at home.
NARRATOR: There are no other children Nokubheka’s age in the TB hospital, but 27-year-old Gcebile has befriended her.
Gcebile was herself orphaned at the same age as Nokubheka. She’s been fighting TB for over two years. But when the side effects of the drugs became too much for her, she stopped taking the tablets, and what was initially ordinary TB mutated into the multi-drug-resistant strain. With none of her family willing to risk looking after her, Gcebile had no choice but to come to the TB hospital.
GCEBILE: It’s like a prison sometimes because you don’t get what you want any time. You don’t get—sometimes you don’t want the—the food that they have given you, but you have to eat it because it—there’s no way you can get another food.
Sometimes we need fruits from outside. They don’t always give us fruits. Who will give us the fruits?
They take us away from our homes to be here so that we cannot be dangerous to the people outside. So we are here now. They don’t want the people to come here to visit us. Why?
NARRATOR: TB is highly infectious and can be passed through the air with a cough. Despite masks, beds spaced 13 feet apart and numerous other precautions, two nurses at the TB hospital have already been infected, and persuading anyone to work here and care for these patients is an ongoing challenge.
CHARITY NEWTON, M.D., National TB Hospital: MDR is contagious. So our fear is getting the sickness ourselves. Some of our nurses have been treated for MDR, too. They get it from the patients. In our areas, once you say you are working here, they say, “Ah! You are going to infect us!” So you see, they just turn away from you.
Then we say, “Uh-uh. That’s not it. MDR is the same as—you can get TB even in the combis [buses]. You can get it anywhere,” because TB’s just in the air. You can get TB from the bus, from whoever.
NARRATOR: Nokubheka’s quarantine is having an impact on her brother, Melusi, as well.
MELUSI: [subtitles] I find it very difficult being here alone.
[in English] When I had my sister, we would tell stories and joke, no. Being with the company of someone, you talk a lot. When you are alone, shut up. You remain silent, maybe listen to music. Nobody to laugh with. Yeah, I miss her a lot. I miss my sister. It’s my sister. It’s my sister always liked making things like this, planting trees and things. She enjoys it very much. She’s left her mark. When I’m feeling lonely, I play music.
NOKUBHEKA: [subtitles] I miss my brother a lot. The last time I saw Melusi was last year. He keeps saying he needs to get money together to come and see me.
I do feel lonely a lot and I miss other children my age. I think some of my friends are about to finish school. But I’m going to have to start again in a lower grade. This makes me very sad.
I’m the only child here. It’s just full of adults. They talk about things I don’t understand and I don’t like.
NARRATOR: Her friend, Gcebile, also feels the hospital is having a bad effect on Nokubheka.
GCEBILE: I don’t think it’s a good place for her. There are old people here, people with a lot of problems, and they talk about boys and husbands, you know? I wish she could have a better life. I know that this place has influenced her so much, she has changed a lot. We can even hear from her language.
Having TB has changed her life so much. I think she is losing her childhood. I think it’s sad.
CHARITY NEWTON, M.D., National TB Hospital: Hello, Nokubheka.
NOKUBHEKA: Hi, Doctor.
Dr. CHARITY NEWTON: How are you?
NOKUBHEKA: I’m fine.
Dr. CHARITY NEWTON: How are you feeling? Sit up, Nokubheka. [unintelligible] Are you still vomiting?
NOKUBHEKA: [subtitles] No, not today.
Dr. CHARITY NEWTON: You didn’t? You didn’t vomit today? OK.
NOKUBHEKA: [subtitles] I haven’t taken my pills yet.
Dr. CHARITY NEWTON: Are you eating well?
For anyone who had—who had to be on treatment for two years, you’d agree with me that’s a lot of time, so a long duration of time to be taking toxic drugs. So we’ve had so many of those patients that stop treatment, and we’ve actually had a patient that committed suicide because of the diagnosis of the MDR-TB. So that’s pretty bad.
[subtitles]
NURSE: How are you managing with these pills, Bheki?
BHEKI: There are just too many. I take them, but there are just too many. I’m going to tell the doctor.
NURSE: What are you going to tell her?
BHEKI: To give me just the drug that will cure me instead of this whole concoction.
NURSE: Bheki, no drug has been invented that can replace all these drugs.
BHEKI: I think it’s best if I stop taking these drugs.
NURSE: So are you thinking of giving them up?
BHEKI: Yes. I’m tired of these drugs. They’re just too much.
NURSE: Just too much.
BHEKI: Just too much.
ERKIN CHINASYLOVA, M.D., Doctors Without Borders: If the patient don’t take properly drugs or miss drugs, it’s an— one of the very dangerous risks is amplification of the resistant— its resistance is growing.
NARRATOR: To treat his MDR, Bheki is on a cocktail of medications developed between 40 and 70 years ago. Two of the drugs are to reduce the impact of the side effects.
[subtitles]
BHEKI: Go and tell that doctor she’s giving me too many drugs. Let’s see her take them all! I’d like to see her take them all at once. Go over there and show her all these drugs listed here and tell her to take them all at once.
NURSE: Please be quiet and listen.
BHEKI: No, I’m tired of listening! Let me die if I’m supposed to die. I can see I’m being made a fool of here. I’ll go over there and ask her myself. I have really had enough.
Please ask the doctor which of these is the one that’s going to cure me?
DOCTOR: [unintelligible]
NURSE: Sit down.
BHEKI: Does she expect me to take all these drugs at once?
Dr. ERKIN CHINASYLOVA: [in English] But everybody takes the same amount of drugs. It’s not only you.
NURSE: Bheki, you are not the only one taking this many drugs. Everyone who is being treated for TB is taking the same amount of drugs.
BHEKI: You don’t seem to understand. Has she ever felt the pain of taking so many drugs?
NURSE: They are all important, and you cannot isolate one from the other. They work together in combination.
Dr. ERKIN CHINASYLOVA: [in English] We can do for night— more for night than morning.
NURSE: She’s going to decrease the number you take in the morning and add them on at night.
BHEKI: That will makes no difference. I’ll still be taking the same amount.
Dr. ERKIN CHINASYLOVA: [in English] It’s better to take before going to sleep, eh?
BHEKI: If she gives me any more, I’m going to throw them away. I just want to get better and have a good life and not a bad one. I’m going over to visit Zandile.
[subtitles]
ZANDILE: I can see, but sometimes I can’t hear properly. When someone speaks, I can hear they’re talking, but can’t make out what they’re saying.
NICHOLIN DLAMINI, Mother of Bheki and Zandile: Hold onto me so I can help you up. OK, let’s try to help each other up. Move back.
She says strange things. Her mind is in chaos. She can no longer walk properly. She can’t even go to toilet. She can’t do anything.
ZANDILE: I wish that God would give me a new life. And I could just live it to the fullest.
NICHOLIN DLAMINI: Open your mouth and take your medication.
BHEKI: Sorry I haven’t brought anything. I don’t have anything. I don’t even know what money looks like anymore. When I stand, my knees ache. By the way, did you say you can’t hear?
ZANDILE: I can hear slightly, but not clearly.
NICHOLIN DLAMINI: What’s wrong, Bheki? Hey? What’s wrong? You look like you’re in a lot of pain.
BHEKI: This life that I’m living is terrible. At the moment, I just feel like killing myself. It’s better to die. When you’re dead, then it will be all over. It’s so hard.
NICHOLIN DLAMINI: Never mind. I’ll be home next week.
BHEKI: I’ll be OK.
NICHOLIN DLAMINI: MDR is really bad. It has given me a tough time with my two children. TB is common in this area. There are so many of us. But when it’s your family affected, it stabs you in the heart.
PRIEST AT BEDSIDE: [subtitles] Father, at this time, we hand Zandile over to you, in the name of God. Have mercy on her, Almighty. The doctors are still trying to cure her in the way they know how. Father, even today, you can do miraculous work. Father, give her life that comes from you. In the name of Jesus Christ, Father, we thank you. Amen.
BHEKI: [subtitles] Sometimes when I think I’m sleeping, I often think about getting a piece of rope to go and hang myself. This life that I’m living is terrible. I sometimes feel sorry for my mother because she will be left alone. She won’t have any children. Life is not good. It’s so hard, I don’t know how to explain it. If death was something you could build, I would have built it by now. If it didn’t come with pain, I would have built it long ago. But it comes with pain.
NARRATOR: Nokubheka has been at the TB hospital for almost six months. If her sputum tests negative for the tuberculosis bacteria, she’ll soon be able to leave the hospital and continue her treatment at home.
NOKUBHEKA: [subtitles] I really don’t want to be here anymore. Whether I’m sick or not, I want to be outside. I often feel trapped in here. It feels like a jail because I am not allowed out of the gates.
NURSE: Hi, Noku. How are you?
NOKUBHEKA: I’m fine.
NURSE: How have you been doing? Huh? I hear you’ve been vomiting. How’s the vomiting now? How’s the medication going? Are you taking your medication every day? At the same time? Correctly? Yes. And do you report when you vomit?
NOKUBHEKA: [subtitles] Things were going well. But I had a relapse. And I really suffered. I was vomiting. I even vomited today.
CHARITY NEWTON, M.D. : Having that chronic lung disease has its own problems in terms of, you know, functioning. But I cannot ignore the fact that the treatment has got severe side effects, as well, which makes it quite difficult for patients to adhere to the treatment.
[www.pbs.org: More on TB drug research]
NARRATOR: Nokubheka’s daily injection, Amikacin, is a 40-year-old drug that has severe side effects. It can cause serious kidney problems, as well as nerve damage that can lead to permanent deafness.
NURSE: [in English] How are the ears?
[subtitles]
Are you hearing any strange noises?
NOKUBHEKA: Yes, there are some strange noises.
NURSE: How long has this been happening?
NOKUBHEKA: Almost a week now.
NURSE: How does the noise sound?
NOKUBHEKA: It sounds like “cch, cch, cch.”
I don’t deserve this thing. I really don’t deserve it. Why should it attack Nokubheka? But I have learned a lot about TB. We mustn’t do big jobs when we go home because we could relapse then have to come back here again. And if you come back here, you might die.
These shoes remind me of my mother’s. She had a pair just like these. Her shoes had the same bottoms.
PATIENT: Did you attend her funeral?
NOKUBHEKA: Yes.
PATIENT: Did you see her in her coffin?
NOKUBHEKA: No I didn’t go because I didn’t want to see her. Why should I look at a dead body?
PATIENT: See, you messed up this thing here. [some needlework]
NOKUBHEKA: It looks like a spider’s house.
PATIENT: You messed up here.
NARRATOR: The rules on how far apart beds have to be to reduce the risk of cross-infection mean that despite its size, the hospital can only take 70 patients. So there is always pressure for beds.
A new patient has just been admitted into the bed across from Nokubheka. She has scrofula, a complication of TB caused by the bacteria infecting the lymph nodes in the neck. Nokubheka’s mother also had scrofula before she died.
NEW PATIENT: [subtitles] It grew into a big lump, and on this side. Two on this side. They could not cure it in Mbabane, so they told me to come here for treatment. They told me I had TB and that I had to come here for my injections, and for this.
NARRATOR: The same night she arrived at the hospital, Nokubheka’s new neighbor lost her battle with TB.
NOKUBHEKA: [subtitles] When I woke up in the morning, I found that she had gone. I overheard people talking. They said she died at 3:00 o’clock this morning. For me as a small child, it’s hard to see these things happening in front of me. The first time I saw someone die was here at this hospital.
It’s not right, but people die here all the time. That sort of thing is not something that frightens me anymore because there is no one who will escape death.
NARRATOR: Nokubheka’s friend, Gcebile, is living in fear. Her sputum tests have remained TB-positive, and she’s worried she may be one of the estimated 10 percent of patients whose MDR-TB is actually the even more deadly form known as XDR, or extensively drug-resistant.
GCEBILE: Now they are waiting for the culture results to see if the treatment is still helping me. If the treatment is still helping me, she say then I will stay for— two months is left. Only two months is left to finish my MDR treatment. But if the culture result comes back positive, I will start the XDR treatment. That takes about two years of injections and then a year of tablets. Three years, I think like three years.
CHARITY NEWTON, M.D.: We do have a regime for XDR, but I should say it’s very difficult to cure XDR because we’re just giving what we have on the table. The reality of XDR is that it’s almost incurable.
NARRATOR: In a 2006 XDR outbreak in South Africa, 52 of 53 patients, many who also had HIV, died. Even for those without the HIV, the prognosis is grim.
GCEBILE: So it’s really hurting when I think that I might be an XDR patient. When you start on XDR treatment, you go down. You go down because it’s another treatment that have new side effects. It’s really bad, yeah. So I don’t know what is going to happen. I don’t know.
CHARITY NEWTON, M.D.: Those patients, they have MDR, and one mistake, they can easily go into XDR TB treatment— I mean diagnosed with XDR, which is sad to see patients fading away day by day with not much hope that you will cure them.
There is a patient unfortunately developed XDR TB that she had contracted from her parents within the same household. Apparently, she was on XDR TB treatment, and she’s lost her parents, she’s lost her hearing, and she’s actually not doing so well on the treatment.
NARRATOR: The patient, Gcinekile, discharged herself, not wanting to spend what may be her last weeks in the hospital. Unable to return to her university, she now lives in isolation at the home of her deceased parents.
GCINEKILE: Imagine waking up in the morning, you’ve totally lost your hearing. I wouldn’t wish that on anyone. I’m a person who loves music a lot, especially gospel from my church. So I miss listening to that music. I had my own favorite songs, and you know, I found myself taking my phone, trying to listen. There’s nothing I can hear.
My mind is so suicidal, and I also hated myself. You know, when I look at a rooftop, I think to myself, “I wish I knew how to tie that knot.” And I try remembering—you remember—I tried remembering how we used to do it as girl guides, but it just doesn’t come back. But I remember all the other knots. So to me sometimes tell me that it’s God’s work that I can’t remember that knot because if I would, I know myself I would do it.
My dad, then the older one, me, and my brother. It crushes me. My friends have boyfriends or husbands. What man would want a girl with TB, skinny and bones?
You see how hard it is. It’s very hard because even if people just see the face, think, like, “Wow, she’s beautiful,” but come see the whole body, scary. No guy would fall for that.
I’ve took every single injection they have on the regime, every tablet. I’m not going to win this battle. That’s it. I’m not going to win it. I never will. Instead, it’s just killing me slowly. Next thing, I’ll be crazy out there because this thing’s slowly eating me up.
CHARITY NEWTON, M.D. : It will take a while, but the disease is progressing. It’ll progress to a point where she probably cannot use the bit of lungs she’s left with.
GCINEKILE: I am deaf because of TB. I lost my parents and my sister because of TB. I’ve been out of school now because of TB. I can’t enjoy my youthful days because of TB. I’ve been out of school now because of TB. I can’t enjoy my youthful days because of TB. I’m not living like every other people with their siblings in the same house because of TB.
Like, seriously now, how many things are going bad for me just because of TB? You see, I really don’t care about the stigma because I’m now able to stay alone. But like, seriously, all these things just because of TB. It’s not fair. It’s really not fair.
NARRATOR: By 2013, XDR-TB cases, although few in number, had been reported in 92 countries.
BHEKI: [subtitles] The coffin’s length and width are this much. It has to be one meter. It has to be one meter.
I’m still alive. I still have my power. The pain is there, but I don’t want strangers and passersby to notice. I don’t want people to see. It’s impossible not to be frightened by this. You never know when it will end for you.
In her case, it started long ago. But in my case, it was quite recent. It went on and on until I ended up like this and came back here. Then I avoided it because I wanted it to end. We will just have to wait and see how it turns out. We are patient.
The old man is hiding his feelings about it. But it’s painful and even he cried. He said that his child had suffered too much. If she were an animal, he said he would have put her to sleep. Mom is in shock. It’s easy to see she’s very anxious.
PRIEST: [subtitles] We pass our condolences to the community and to everyone who has been affected by Zandile’s death. Rest in peace. We shall forever miss you, Zandile. The gap you’ve left will never be filled.
On this path we are still moving, and we are still living. We ask for things to happen but they don’t happen the way we expect them to. We have a high priest who feels our pain. He also feels our pain. He feels our pain. When our relatives die, there is a high priest who feels our pain.
NEIGHBOR: [subtitles] A man said, “The house is on fire!” The fire was huge. I guess they must have left a candle burning.
NARRATOR: During Zandile’s funeral, a fire started inside Bheki’s house, and many of his possessions and some of his TB medications were caught in the flames.
[subtitles]
BHEKI: Where are my pills? I never took them. My pills got burned. Eish!
NICHOLIN DLAMINI: No Bheki, think about us. You know that I always make a plan. Don’t worry, no matter what got lost.
BHEKI: Mother, I am trying. You know that I’m trying.
NICHOLIN DLAMINI: No, Bheki. No, Bheki! You usually comfort me and tell me “Mother, be strong.” Now you’re not being strong. No, Bheki. No, Bheki.
BHEKI: I never took my pills. This has come like a bolt out of the blue.
NICHOLIN DLAMINI: These things happen. But you must face it with courage, like a man.
BHEKI: What have I done to deserve this?
NARRATOR: While Bheki struggles to get back on his medicines, there is new hope for Nokubheka. After six months of daily injections, her sputum tests are now negative. Her brother, Melusi, is still at school, being supported by a local church. He can’t afford to look after Nokubheka, but the church has found a family willing to take care of her for now.
NOKUBHEKA: [subtitles] When they told me I could leave the hospital, I was very happy. I felt like flying away somewhere. Life is much better now that I’m staying here instead of at the TB hospital.
MELUSI: [in English] TB divides families, because that’s the case with us. Since Nokubheka left, I’ve been living alone. I prefer her to be here, of course, if I had a separate room. It’s such a long time that I have missed her, you know. She’s the only little sister I’ve got.
NOKUBHEKA: [subtitles] I miss my brother a lot. We used to chat together. I’m happy now that I’m back at school.
[in English] I like school because tomorrow I will be in university, and then I’m supposed to get to work.
[subtitles] One day, I’ll be working at the headquarters of a big company, in a computer lab.
NARRATOR: Nokubheka still has at least a year of taking numerous drugs every day, and if she lapses, the disease will come back. So a normal life, free from TB, is still a long way off.
NOKUBHEKA: [subtitles] I’ve been taking these pills for a long time. I wish it could come to an end. Then I could focus on my education and be like a normal school girl and not have to take these pills and go to the hospital all the time. The day I stop taking these pills, I will be very happy. My heart will be overjoyed.
NARRATOR: But things are not going so well for Nokubheka’s friend from the hospital, Gcebile.
GCEBILE: My TB is not getting well. It is not being treated. Most of the XDR patients, they die. I’m scared. I’m really scared of XDR. I wish my culture results can come back negative.
MIRIAM ABDUL, M.D., National TB Hospital: How are you today? We are following on your results and your clinicals. You have been on medication for more than a year now. It’s a year almost, yeah? But each time we are taking your sputum, that is also coming back positive. They’re not changed. So it show that the drugs are not working on you because it’s not possible that the drugs are working and you are fine clinical, but each time we are testing it, we come in positive and positive and positive and not change.
So it’s true that we know you feel bad. No one can be ready to be told that, OK, my results are not bad, they’re not right, but that is the reality. You are not doing OK. The drug we are giving you are not giving us any change, as long as when you monitor the bacteria, still there always. You are going to move from this ward to other ward because this side, we are keeping those patients who are culture-negative, smear-negative, but you are not among them now.
Forget about going home now. This now, it’s XDR. I know you need to cry now. It’s a sad—it’s a sad news, I admit. So yes, have your time. And we’ll talk later. This is now XDR. That’s the information we wanted to deliver to you today.
NICHOLIN DLAMINI: [subtitles] Let me unroll that for you.
BHEKI: [subtitles] Can you unroll that?
NICHOLIN DLAMINI: [subtitles] Yes.
BHEKI: [subtitles] You need to snap it. Be careful it doesn’t prick your hands.
NICHOLIN DLAMINI: [subtitles] I really believed Zandile would get better. They worked so hard to try and cure her. I’ve surrendered everything to God. I’m just praying for Bheki to live. It would hurt me terribly if Bheki also reached this stage.
NARRATOR: Bheki is still struggling to adhere to his complex drug regimen. New TB drugs are finally coming to market, but health officials worry that affordable, more effective treatment is still years away.
[subtitles]
HEALTH WORKER: We have come to visit you. Where would you like us to sit?
BHEKI: You could have sat under the tree, but I chopped it down. When Zandile died, so did the tree. Are you going to be OK there?
HEALTH WORKER: Don’t worry, we won’t be long. As Bheki’s caregiver, is there anything you would like to ask us?
NICHOLIN DLAMINI: No there isn’t, apart from the PASA drink that he hates.
FRIEND: As soon as he drinks it, he flings the cup at you. He takes it, but once has drunk it, he throws the cup at you! [laughter] But he does take it.
HEALTH WORKER: If you don’t take the PASA because it’s so bitter, then that means you’re not taking your medication properly. That will cause the disease to do what?
NICHOLIN DLAMINI: Resurface.
HEALTH WORKER: Resurface and spread.
BHEKI: [subtitles] At the moment, I’m still taking these pills. I’ll see where they take me. If they work, then life can go on. And if they don’t work—it does cross my mind. Since Zandile is dead, that means I will also follow. Her illness also started slowly, but in the end, she got really sick. Then she ended up dead.
She hasn’t left my heart. It’s going to take a very long time to forget her. I think I will miss her until the day I die. I am really hurt by my sister’s death. I loved her.
FRIEND: Are you going to the game?
NICHOLIN DLAMINI: It’ll be very muddy.
BHEKI: Of course we’re going!
[at the game] Come on, come on, come on! Come on, come on! Ah! That’s it! Come again! Come this way!
NICHOLIN DLAMINI: [subtitles] Hello, Zandi. There where you are, I will be joining you, too. When I come here, it feels like I can sit here and have a conversation with her because my spirit has still not accepted that she’s passed on. If it were possible for those who make the pills to come up with drugs with a shorter period of treatment, then she would have held on and finished her treatment and survived.
ERKIN CHINASYLOVA, M.D., Doctors Without Borders: I feel sorry that in the— in this era of globalization, we still use old, old drugs, and we cannot eliminate TB.
NARRATOR: Nokubheka’s friend, Gcebile, couldn’t face the thought of living in an XDR isolation ward. So she’s discharged herself and is living alone at home.
GCEBILE: I’ve run out of tears. My tears are all dried. I’m just dying inside. This can’t help me. I can’t cry every day, every day, every day. It’s going to cause me a lot of sickness, so I have to— I’ve left everything in God’s hands, right now.
NARRATOR: Gcebile is still fighting her battle with XDR TB.
GCINEKILE: Anyone can get TB. We all use public transport. And even at the workplace, you don’t know whose health is in what condition. You don’t know who’s sick, who is not sick, who’s faithful to their medication and who’s not. So TB’s just in the air. So whether you’re poor or rich, you can’t stop that. There’s no way you can stop it.
NARRATOR: Six weeks after filming, Gcinekile lost her battle with XDR TB.
CHARITY NEWTON, M.D. : TB kills. And you cannot choose the air you breathe. And hence, we’ve got to effectively control TB if we want to make ourselves safe. It’s a major problem because the drug-resistant TB seems to be getting worse and worse, and the rates are becoming more than they were before.
ERKIN CHINASYLOVA, M.D., Doctors Without Borders: In developed countries, in Western countries, they should be threatened with the spread of TB. We are living in the era of globalization. So infectious airborne diseases like TB is given a great opportunity to spread worldwide very rapidly and have a huge impact on global public health.
BHEKI: [subtitles] So long as it is here, a lot of people are going to die.
NOKUBHEKA: [subtitles] What needs to change is that we should get better medicine so we can make all the people in hospitals better.
NICHOLIN DLAMINI, Mother of Bheki and Zandile: [subtitles] Let us accept the fact that we are faced with a TB epidemic. We need to get together and fight for our survival so that there can be a future for the next generation because if we give up the fight right now, the children are finished.
TB SILENT KILLER
March 25, 2014
DIRECTED BY Jezza Neumann
PRODUCED BY Jezza Neumann Rebecca Stewart
PRINCIPAL PHOTOGRAPHY Jezza Neumann
ADDITIONAL CAMERA Rebecca Stewart
EDITED BY Paddy Garrick Jezza Neumann
PRODUCTION MANAGER Pippa White
PRODUCTION COORDINATORS Niki Whewell Rebecca Andrews
PRODUCTION ASSISTANTS Sandile Mashaba Tash Despa
CONSULTANTS Claudia Denkinger, MD, PhD Foundation for Innovative New Diagnostics (FIND)
NARRATED BY Will Lyman
COMPOSER Jamie Perera
ONLINE EDITOR/COLORIST Jim Ferguson
SOUND MIX Jim Sullivan
ASSISTANT EDITORS Tom Read Niki Whewell
TRANSLATION Nicola Vilakazi
EXECUTIVE PRODUCER FOR BBC Clare Patterson
EXECUTIVE PRODUCER FOR TRUE VISION Brian Woods
© 2014 True Vision Productions
FOR FRONTLINE
POST PRODUCTION SUPERVISOR Megan McGough
ON-AIR PROMOTION PRODUCER Missy Frederick
ON-AIR PROMOTION EDITOR John MacGibbon
ASSISTANT EDITOR Eric P. Gulliver
POST PRODUCTION ASSISTANT Kenzie Audette
DIRECTOR OF POST PRODUCTION Chris Fournelle
SENIOR DIRECTOR PRODUCTION TECHNOLOGY Tim Mangini
SERIES MUSIC Mason Daring Martin Brody
DIRECTOR OF AUDIENCE DEVELOPMENT Pamela Johnston
PUBLICITY ACCOUNT MANAGER Patrice Taddonio
PUBLICIST Diane Hebert-Farrell
ONLINE ENGAGEMENT COORDINATOR Nathan Tobey
SECRETARY Christopher Kelleher
EDITORIAL SECRETARY Sophie Gayter
COMPLIANCE MANAGER Caitlin Birch
CONTENT MANAGER Lisa Palone
LEGAL Eric Brass Jay Fialkov Janice Flood
CONTRACTS MANAGER Gianna DeGiulio
UNIT MANAGER Varonica Frye
DIRECTOR OF BUSINESS Tobee Phipps
DIGITAL ASSOCIATE PRODUCER Jason Breslow
DIGITAL TECHNOLOGIST Bill Rockwood
SENIOR DESIGNER Evan Wexler
DIGITAL REPORTER Sarah Childress
ASSISTANT MANAGING EDITOR FOR DIGITAL MEDIA Sarah Moughty
WEBSITE DESIGN AND TECHNOLOGY Entropy Media, LLC
DIRECTOR OF NEW MEDIA & TECHNOLOGY Sam Bailey
POST COORDINATING PRODUCER Robin Parmelee
SERIES COORDINATING PRODUCER Carla Borras
SPECIAL COUNSEL Dale Cohen
SENIOR EDITORIAL CONSULTANT Louis Wiley Jr.
SERIES SENIOR EDITOR Andrew Metz
SERIES MANAGER Jim Bracciale
DEPUTY EXECUTIVE PRODUCER Raney Aronson-Rath
EXECUTIVE PRODUCER David Fanning
A True Vision production for WGBH/FRONTLINE in association with the BBC
© 2014 WGBH Educational Foundation All Rights Reserved
FRONTLINE is a production of WGBH/Boston, which is solely responsible for its content.
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.



















