Why Rising Temperatures Could Make Life Harder for Lupus Patients
Rheumatologist George Stojan says that many of his lupus patients know their joints are going to swell or go stiff when the weather shifts, particularly when the temperature or humidity changes. It got him thinking about how climate change could exacerbate their disease, and prompted him to take a closer look at the possible connection.
Stojan, an assistant professor of medicine at the Johns Hopkins University Medical School and co-director of its lupus center, studied more than 1,600 patients, and he found a relationship between their worsening symptoms and changes in the weather or air quality, such as intense heat or cold, high humidity, wind and severe air pollution.
“Ultimately, if our results are confirmed in future studies, it is inevitable that rising temperatures and weather extremes expected as a result of climate change will have an effect,” Stojan said, adding that climate change ultimately could be a key factor in treating lupus.
Systemic lupus erythematosus, usually just called lupus, is a chronic, disabling and potentially life-threatening autoimmune disease that damages the joints, skin, heart, lungs and kidneys, and can also cause depression and cognitive problems. It affects about 5 million people worldwide, disproportionately women and people of color, and African-American women in particular. Although researchers don’t know why, they suspect it has to do with the interplay among genetics, environment and factors like income and education.
“Early in the disease it affects a patient’s life by causing joint swelling, fatigue, rashes, shortness of breath and a myriad of other symptoms,” Stojan said. “Late complications include a higher risk of heart attacks and strokes.”
Stojan, who presented his research at a recent meeting of the American College of Rheumatology (it has not yet been published in a medical journal), obtained data from the Environmental Protection Agency on temperature, wind, humidity, barometric pressure and air quality to study the relationship between those factors and patients’ symptoms in the 10 days prior to their visit to the lupus clinic.
“My study is the first evidence to my knowledge that these atmospheric factors affect the expression of an autoimmune disease,” he said. In the study, he noted that high temperatures and wind have been shown to influence the immune systems in other diseases, and could play a similar role in lupus, although the exact mechanism remains unclear.
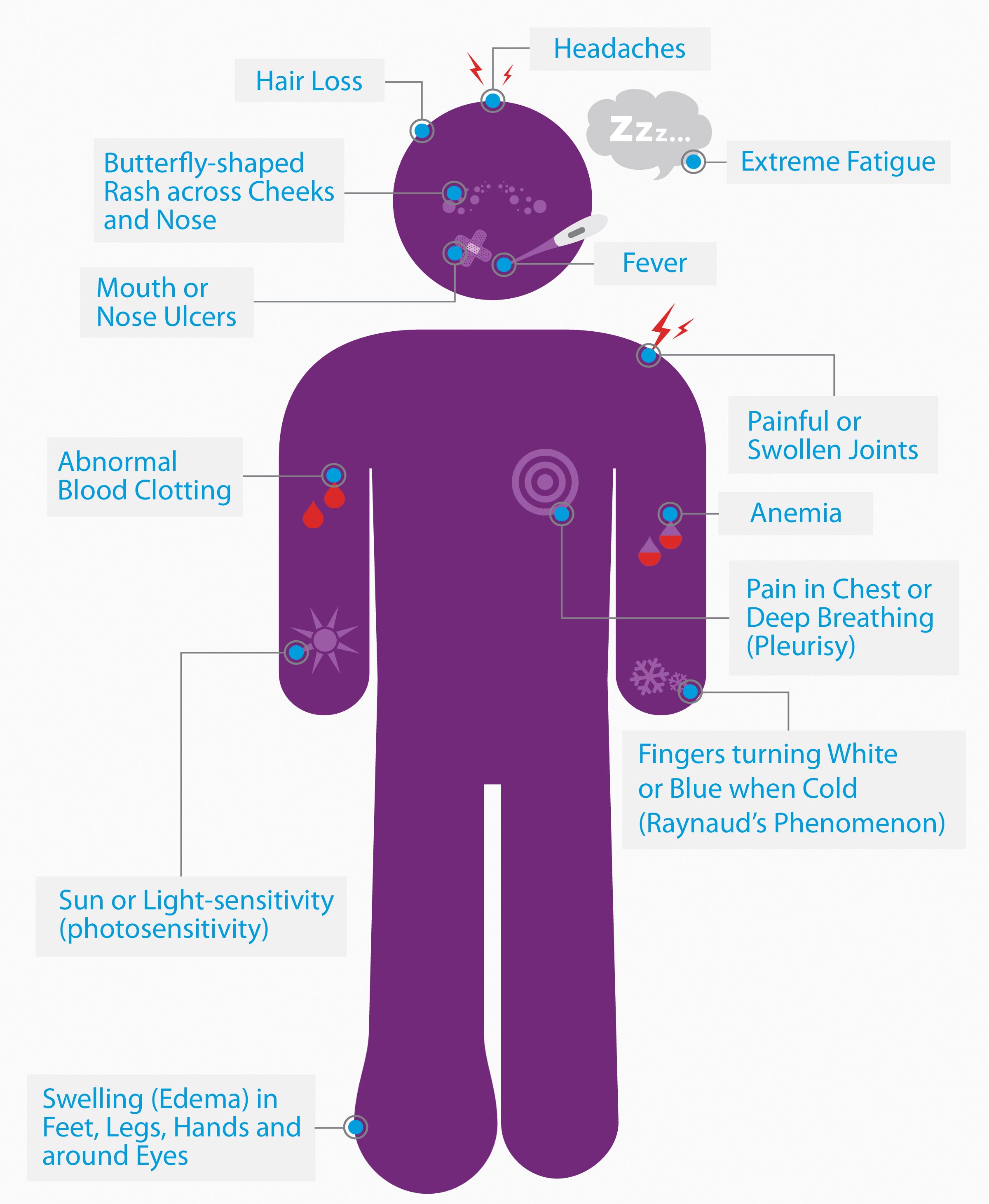
The symptoms of lupus. | Source: Lupus Foundation of America
Different atmospheric changes had different effects. Rising temperatures caused joint swelling, inflammation of the tissues that surround organs, rashes, and a decline of important blood cells, including white and red cells and platelets. High humidity resulted in joint swelling and inflammation. Air pollution also produced inflammation, as well as new rashes, blood abnormalities and joint flares (a worsening of joint stiffness and swelling). Wind caused joint flares, lung, blood and neurologic problems.
Climate change could make things worse in the years to come, as rising temperatures will yield higher humidity. This may be one more way that the carbon crisis disproportionately harms women and people of color.
Judith James, professor of medicine and pathology at the Oklahoma University Health Sciences Center — and a lupus expert not involved in the research — said the study provides new insights and confirms much of what she sees among her own patients.
“Many consistently report that they feel that their symptoms are impacted by changes in the weather or other aspects of their environment,” she said.
She called for further studies to investigate how the weather affects the immune system and determine what changing conditions might mean for treating diseases like lupus.

Nick Cannon (left) and Selena Gomez (right) both have lupus. | Source: Loren Javier
Sasha Bernatsky, a rheumatologist and professor of medicine at McGill University, who also was not involved in the study, said she hasn’t seen a strong connection between weather and lupus symptoms within her own practice, but acknowledged that at least 5 percent of her patients do complain that the weather affects their muscles and bones. Moreover, “there is a lot of interest in the possibility,” she added.
Stojan agreed that more studies are needed, saying the relationship between weather and lupus is not simple. Also, he pointed out that the study was confined to patients in Maryland, meaning it only looked at weather conditions in that state.
“We need bigger populations and areas with different weather patterns to confirm our findings,” he said.
He also hopes to delve more deeply into how one’s genes may affect their response to changing weather conditions to better understand why certain groups are more vulnerable to lupus than others.
“The interplay of genetic background and environmental factors could potentially explain the high incidence and increased severity of lupus in some ethnic minorities in the United States, like African Americans and Hispanics,” he said. He added that differences in weather could explain why lupus is more prevalent in some regions and less prevalent in others, even where the demographic makeup of those regions is the same.
His preliminary results give credence to this idea. They also seem to validate what he has been hearing anecdotally from patients for years.
“Ultimately, these findings are the first step to vindicating the great majority of lupus patients who are convinced that their disease is influenced by weather changes, and who inspired this research,” he said.
Marlene Cimons writes for Nexus Media, a syndicated newswire covering climate, energy, policy, art and culture.




