ENDGAME: AIDS in Black America
July 10, 2012
1h 53m
A groundbreaking two-hour exploration of one of the country's most urgent, preventable health crises
ENDGAME: AIDS in Black America
July 10, 2012
1h 53m
Share
Every 10 minutes, someone in the U.S. contracts HIV. Half are black. Thirty years after the discovery of the AIDS virus among gay white men, nearly half of the 1 million people in the United States infected with HIV are black men, women and children. A FRONTLINE special presentation, ENDGAME: AIDS in Black America, is a groundbreaking two-hour exploration of one of the country’s most urgent, preventable health crises.
Support provided by:
Learn More
Most Watched
The FRONTLINE Newsletter
Related Stories

Who’s Winning (and Losing) The Global Fight Against HIV/AIDS

CDC Reports Troubling Rise in HIV Infections Among Young People

Despite Show of Support, Federal Funding Ban on Needle Exchange Unlikely to Be Lifted Anytime Soon

What Is President Obama’s Track Record on HIV/AIDS?

“It’s a Part of Me”: Meet the Young People Born with HIV

Report: Oversight Lacking for HIV/AIDS Funding

Why Some with HIV Still Can’t Get Treatment

Live Chat Wed. 2:00 p.m. ET: The Hidden Story of AIDS in Black America

Timeline: 30 Years of AIDS in Black America

Making ENDGAME: A Conversation With Filmmaker Renata Simone

HIV and Disclosure: A Doctor’s Moral Dilemma

Remembering the Lost
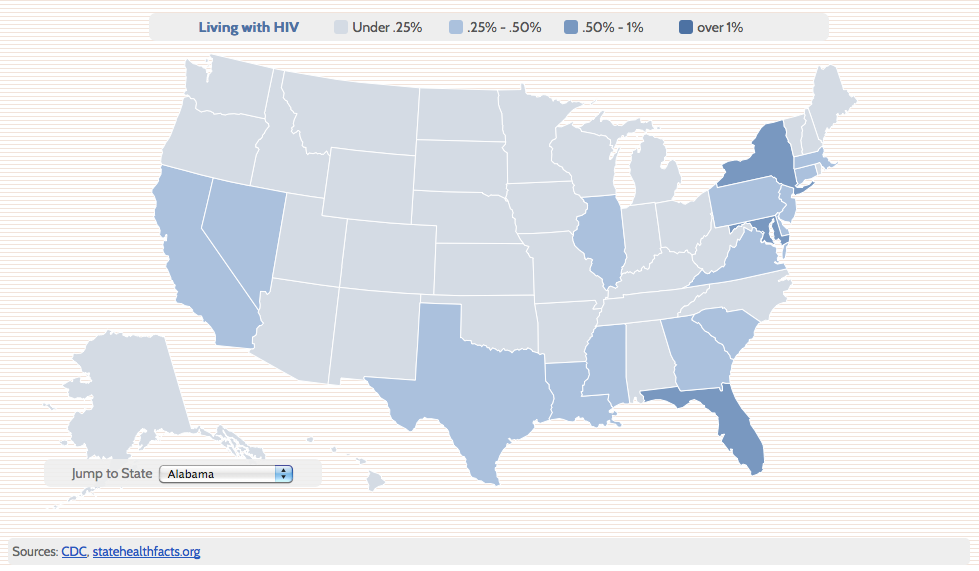
Map: HIV/AIDS in Your State

Learn More: HIV/AIDS Resources

Phill Wilson: “We Have the Tools To End the AIDS Epidemic”

Julian Bond: HIV/AIDS Is “A Civil Rights Issue”

Robert Fullilove: Inside the “Two Worlds of AIDS” in America
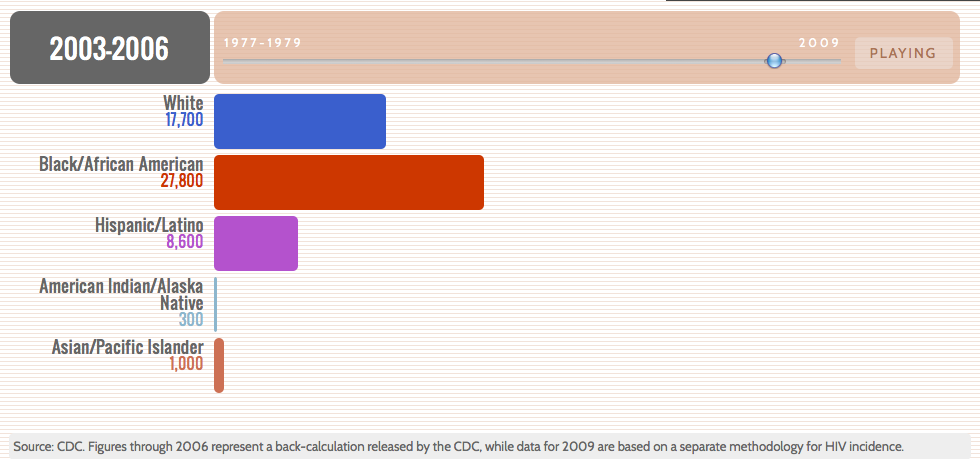
Interactive: The Spread of HIV in Black America

Race and America’s HIV Epidemic

“ENDGAME” on NPR’s “Fresh Air”

Why People Still Won’t Get Tested for HIV

AIDS in Black America: The World’s 16th Worst Epidemic

20 Years After HIV Announcement, Magic Johnson Emphasizes: “I Am Not Cured”
Related Stories

Who’s Winning (and Losing) The Global Fight Against HIV/AIDS

CDC Reports Troubling Rise in HIV Infections Among Young People

Despite Show of Support, Federal Funding Ban on Needle Exchange Unlikely to Be Lifted Anytime Soon

What Is President Obama’s Track Record on HIV/AIDS?

“It’s a Part of Me”: Meet the Young People Born with HIV

Report: Oversight Lacking for HIV/AIDS Funding

Why Some with HIV Still Can’t Get Treatment

Live Chat Wed. 2:00 p.m. ET: The Hidden Story of AIDS in Black America

Timeline: 30 Years of AIDS in Black America

Making ENDGAME: A Conversation With Filmmaker Renata Simone

HIV and Disclosure: A Doctor’s Moral Dilemma

Remembering the Lost

Map: HIV/AIDS in Your State

Learn More: HIV/AIDS Resources

Phill Wilson: “We Have the Tools To End the AIDS Epidemic”

Julian Bond: HIV/AIDS Is “A Civil Rights Issue”

Robert Fullilove: Inside the “Two Worlds of AIDS” in America

Interactive: The Spread of HIV in Black America

Race and America’s HIV Epidemic

“ENDGAME” on NPR’s “Fresh Air”

Why People Still Won’t Get Tested for HIV

AIDS in Black America: The World’s 16th Worst Epidemic

20 Years After HIV Announcement, Magic Johnson Emphasizes: “I Am Not Cured”
WRITTEN, PRODUCED AND DIRECTED BY Renata Simone
ANNOUNCER: Tonight on FRONTLINE, an intimate journey.
MARVELYN: I was a heterosexual all-American teenager. HIV and normal didn’t go together, so I thought.
JOE HAWKINS, Bench and Bar Nightclub: The minister put his hand on my head and started trying to cast the homosexual demon out of me.
NEL: How could you love me and keep such a secret from me? This is not love.
MAGIC JOHNSON, LA Lakers: I told her, “I could understand if you want to leave me.” And she hit me upside my head and she said, “No, we’re going to beat this together.”
ANNOUNCER: Tonight, the dramatic story of how a disease took hold.
PHILL WILSON, Black AIDS Institute: If black America were a country itself, it would have the 16th worst AIDS epidemic in the world.
ANNOUNCER: Of a challenge for the future.
Dr. LISA FITZPATRICK: Ending the epidemic is entirely within our power. We have to have courage.
PHILL WILSON: We’ve been at this for 30 years and we need to be talking about endgame.
NARRATOR: Hollywood, California, December 1st. There are a lot of red-carpet galas in this town, but this one is different.
PHILL WILSON, Black AIDS Institute: This has been a remarkable journey. Today is World AIDS Day, and today in America, 152 people will become infected with HIV. Half of them will be black. Today in America, two thirds of the new HIV cases among women will be black. Today in America, 70 percent of the new HIV cases among youth will be black. That is why our resolve to end AIDS must not end tonight! [applause]
NARRATOR: AIDS in America has become a crisis no one imagined when a mysterious new disease was first noticed 30 years and three miles from here.
MICHAEL GOTTLIEB, M.D., UCLA Medical Center, 1980-87: Thirty years ago, I was a junior professor at UCLA teaching immunology. And we wanted to have a case to discuss on rounds, and so I asked the resident if there were such a case, and he came back with our UCLA patient zero, if you will.
DAVID HO, M.D., Aaron Diamond AIDS Research Center: My recollection of the very first case was a white young man who presented to the hospital with shortness of breath. He was hungry for air.
Dr. MICHAEL GOTTLIEB: This is someone who was previously healthy, who all of a sudden has dropped 25 pounds and looks like a scarecrow.
NARRATOR: When every patient with the new disease died, alarmed officials sent out an international alert. But from the start, something was missing.
Dr. MICHAEL GOTTLIEB: In medicine, when we describe a patient, we say, “This is a 31-year-old white, single, gay male.” But in our reports, we said nothing whatsoever about race. It really is an omission on our part.
The first five patients were white. The next two were black. The sixth patient was a Haitian man. The seventh patient was a gay African-American man, here in Los Angeles. Most of those first patients died within months. We had no information and treatment.
In June of ’81, we were thinking, “Oh, this is something among gay men here in Los Angeles. And yes, some are white and a couple are black. No big deal.”
NARRATOR: But it was a big deal. The media ran headlines of a killer plague among gay men. But the stories and the images were white.
PHILL WILSON: I was a young, black, gay man from the south side of Chicago. I had never even heard of Fire Island. I was not a West Hollywood person. I had, you know, barely ever been— barely ever been to San Francisco. I was in San Francisco when I was 10 years old. So none of this mattered to me.
My thought was, you know, “Thank God it is them and not us. For once in a lifetime, it is about white people and it’s not about black people. “
NARRATOR: Around the country, in gay communities like San Francisco’s Castro district, word spread about the mysterious killer disease. But on the other side of the bay, in Oakland, it was a different story.
JOE HAWKINS, Bench and Bar Nightclub: That bridge really is a divider. They are literally two different worlds. When a black person would go to the door of the white gay clubs in San Francisco back in the ’80s and ’90s, we would be asked for two, three, four pieces of ID before we could get in.
We weren’t considered a hot spot — it was San Francisco — even though we were burning, too.
JESSE BROOKS: All I can say about the difference in the early ’80s from San Francisco and Oakland is that it was silence. While in San Francisco they were acting up, literally, and talking about HIV, over in Oakland, it was silence and fear.
MARSHA MARTIN, D.S.W., Get Screened Oakland: We sit in Oakland, across the bay from San Francisco. San Francisco is known around the world as a gay community. San Francisco is 4 percent African-American. Oakland, on the other hand, is 45 percent African-American.
So they’re going to live in Oakland and they’re going to use the proximity of this positively identified gay community to feel OK and safe about their sexual identity. And they’re going to do it silently in Oakland. And they’re going to live here and they’re going to socialize here, and they’re going to be attached to a San Francisco environment.
That is very important in the African-American community. We don’t have the safety of numbers or resources to have an out, active community.
JESSE BROOKS: We grow up in families that say you don’t tell people your business. So that prevailed, about spreading your business around and the distrust of, if you tell your business, how someone would take that and use it against you.
NARRATOR: In the 1980s, Jesse was an A student, a National Guardsman, and a model. And he was hiding.
JESSE BROOKS: The African-American community, and a lot of communities, have stigma around being gay. I had an uncle, and I remember being in the car with him, and he pointed to an obviously gay man and said, “I hate them.” And this is my uncle who was my favorite uncle, and it crushed me.
And so it also led me to not want to open up about who I am and for me to be ashamed about who I am.
PHILL WILSON: We all grow up with, “Don’t put your business on the street,” you know, and “Don’t hang out your dirty laundry,” and all these phrases around keeping secrets.
You don’t tell other folks how poor you are. You don’t tell other folks, you know, that you can’t pay the rent. You don’t tell other folks, you know, that so-and-so is sick. And you certainly don’t tell other folks that there’s a gay son. And you don’t tell other folks that someone in the family has AIDS.
It’s all about those things, you know, that you think, you know, are ways to protect yourselves. You know, going all the way back to slavery, you know, that the slaves kept secrets that you didn’t take— you didn’t tell the master about the conversations that were happening in the slave quarters, you know?
And while, thank God, you know, we’re not in that place, but some of that cultural baggage travels with us.
JULIAN BOND, NAACP Chairman Emeritus: I think we thought about AIDS as afflicting only white people, and then only white gay people, and there were no black gay people. It meant that as the disease grew and grew and grew and grew, and we tended to ignore it and pay no attention to it, or to think it was something that didn’t affect anybody that we knew, and therefore not a matter of concern for us.
Which is foolish, and criminal even. But nonetheless, I think that was pretty much the attitude.
GAIL WYATT, Ph.D., Psychiatry Dept., UCLA: I was aware as a sexologist that if you have a disease that spreads through sex, it’s going to spread everywhere. It’s not going to stay in one community. And sexual orientation has nothing to do with the spread of AIDS.
And I think that some of the people in the public health field really didn’t have a very realistic sense about how AIDS was going to affect men, women and children.
NARRATOR: And in time, that’s exactly what would happen.
NEL: I have 5 children and I have 17 grandchildren and I have 5 great-grandchildren. Yeah, a lot of babies. A lot of babies.
NARRATOR: Nel’s retired now after a full career as a nurse. Her focus is on her family, and as always, on her church.
Rev. EDWARD FIELDS, New Hope Baptist Church: You know, there are a lot of churches where people come to church, they do their work at the church, and then they go home and that’s it. But New Hope is a church where we come together, we feast together, you know, we enjoy one another’s friendship and fellowship.
It’s almost like, you know, when I was growing up, “Don’t mess with me because I got my two brothers.” And that’s the way it is at New Hope, which is sort of like a family.
NARRATOR: So it seemed natural when, 14 years after she was divorced, someone in the parish caught Nel’s eye.
NEL: Well, actually, I didn’t meet him. He was in my church all along. He was a deacon in my church, but I didn’t know his name. And you know, it was just passing and going, so— so anyway, he finally introduced himself.
Rev. EDWARD FIELDS: Well, Rodney was one of the nicest guys in this church, a good-looking guy, and he was a good catch. And I think that there were many ladies in this church that would have jumped at the chance.
NEL: It was a happy time. We had a lot in common— +great sense of humor. We liked to do a lot of things together. The only thing that was kind of different, he was a Raider fan and I’m a Dallas Cowboy fan, so that was a little— you know, didn’t quite— didn’t quite mix too well, but we got through that.
So he asked me to marry him and I said yes. And so we was engaged for about a year, you know, so we prepared. You know, if you’re going to married in a church, you have to go through the six-week marriage counseling. So we went through all of that.
Rev. EDWARD FIELDS: The first thing we do is we go over the biblical concept of love. And then we deal with finances, keeping the excitement in your marriage, and then, you know, talking and how to communicate with your wife— six major subjects that it deals with.
NEL: After the six weeks, we was fine. So then we got married. The children was there, the grandchildren— actually, my grandchildren was my wedding party and my granddaughters was the little flower girls. So from there, we took off. And he wanted to go on a cruise and I wanted to go to DisneyWorld because I’m afraid of the water. So we went to DisneyWorld.
And the whole while I was there, I was sick. And I didn’t think too much about it because, you know, the hustle and bustle, trying to get through the wedding, and we both had bad colds. So I was in bed. You know, basically, the whole while, I was in bed and couldn’t eat and just— you know, just really sick.
NARRATOR: After the honeymoon, months went by and Nel didn’t feel any better. But she settled into married life.
NEL: So this one particular morning I was making the bed, making our bed. And on his side of the bed was his Bible. So— and you know, just kind of disrupted the Bible it was unzipped. So all of the content of it fell out, so— and I was trying to get it back in. You know, he wasn’t there. I was tying to get it back in. I just felt like I had been invading his privacy, so I was hurrying up, trying to get it back in.
And this letter that I could not put back in its proper place, it was a letter from the blood bank, so— and at first, I didn’t want to open it. But I had this burning— it was, like, “You need to read that.” I can’t express to you what that feeling was, but it was, like, “You must read this.”
So I— I did. I opened it up and I read it. And it started off saying— you know, informing him that— that he had been diagnosed with HIV/AIDS and that he should, you know, seek medical, you know, attention. And this letter was dated a year before we got married.
So at that time, I— I read it and I read it. I could not believe it, so— excuse me. [sighs] But during that time, I still didn’t put it together, you know, why I had been sick or ill or anything.
So I sat him down and I asked him was there something that he forgot to share with me before we got married. And he said, “No, no, no, we have no secrets. I told you everything.” And I said, “I’m going to ask you again, is there something that you forgot to tell me before we got married?” And he said, “No” again.
And I said, “Now I’m going to ask you again. Think about this before you answer this time.” And I asked again, and he said, “No, no. No, there is nothing. I’ve— you know, everything about me you know.”
And that’s when I showed him the letter. I said, “Well, did you forget to tell me this?” And— [sighs] At that time, he said, “I tried to tell you, but I was afraid I would lose you if I had of told you.”
And I said at that time, “No. How could you love me and keep such a secret from me? This is the worst kind of betrayal that anyone could do, you know, to anybody.” I said, “This is not love.”
NARRATOR: Nel knew she had to get an HIV test for herself. The results would come in two weeks.
NEL: And that was the longest two weeks that I’ve ever had to wait for anything in my life.
Rev. EDWARD FIELDS: One morning, we were coming for Bible study. And I walked up and I just put my arm around her and asked her how she was doing. And she said, “Oh, I don’t know.”
NEL: But during that time, I knew that it was going to come back positive because it had been too much time. And it did. It came back positive. And I— [sighs] I went through such a roller-coaster ride.
I didn’t want to live. I wanted to commit suicide. I didn’t know how I was going to tell my children, my grandchildren. I didn’t know enough about HIV/AIDS. I was under the impression I was going to die immediately. I had lost about 20-some— about 23 pounds. I couldn’t sleep. I couldn’t eat. I couldn’t focus on my job.
I mean, I was just a mess. I mean a mess. I was a total mess.
Rev. EDWARD FIELDS: I think the thing that was so painful to me was the fact that he knew this. He knew this before he ever asked her out.
It was frustrating. It was extremely difficult and it took a lot of prayer for me to be able to— to even treat him like a human being, much less be there for him and meet his needs. But I had to do it because I was his pastor.
But I felt like Nel ought to go down and report it and have him arrested for it. That’s what I felt. And I know, you know, when I go to give blood, there’s a little thing that says, you know, if you knowingly do this and if you knowingly have relationships— you know, I mean it’s illegal!
But Nel didn’t want to do anything, and she did tell me that. She said, “You know, because I love my husband.”
NEL: I trusted him with my life. I did. I just trusted him with my life. That’s how much I loved him. And after I found out, and the manner that I found out, I still loved him, but I could never trust him again. My respect was gone and just so much was gone.
And to this day, I love him. I still love him. But that’s not enough.
RADIO INTERVIEWER: Wake up, everybody. KPOO San Francisco, Oakland, Hayward, Marin. Joining me now on the “Limeline,” it’s a pleasure to welcome back to the program Mr. Jesse Brooks, who is an AIDS activist. Good morning, sir.
JESSE BROOKS: Good morning, Donald.
RADIO INTERVIEWER: Hey, how you doing?
JESSE BROOKS: I’m great, man. Awesome.
RADIO INTERVIEWER: Good to hear from you, man. And as a lot of our listeners know, Thursday is World AIDS Day. And lately, it seems that the focus isn’t there as much as it was.
JESSE BROOKS: Yes.
RADIO INTERVIEWER: Talk about that whole struggle.
JESSE BROOKS: Well I think one is the mindset that this was a white man’s— a white, gay man’s disease.
RADIO INTERVIEWER: Absolutely.
JESSE BROOKS: So people still have that mindset that it’s a gay disease. But it’s not, it’s a sex disease. You know, I’ve been positive since 1993. So to look at me, I could be any brother from the street.
RADIO INTERVIEWER: That’s right.
JESSE BROOKS: And so that’s what the face of HIV looks like. And that’s why I do what I do. My brother died of HIV.
Leon Anthony Brooks was my oldest brother. And he was an awesome brother— very creative, very handsome. He was my idol. In the early ’80s, when people were first getting HIV and AIDS, it was a visual thing. You can see people with AIDS. There was so much stigma.
And he got sick in front of our whole family. So you know, we saw him die as a family and so— but it also instilled fear in me that when I became positive I— I just knew I was going to die.
And Leon’s story is like so many of my friends and people that I was maturing with at— at the age of 18, 19. So many of those people I danced with in the clubs didn’t make it. They’re not here today.
JOE HAWKINS, Bench and Bar Nightclub: The clubs were our home, our place to come out, and get support from one another. It was like our community center. But of course, it was a nightclub.
NARRATOR: The clubs were a refuge from the outside world where they lived a double life.
JOE HAWKINS: At the time, I was very much into religion and— you know, I was raised that way. But one day, my roommate, he asked me to come to his church. And there was a minister standing in front of me and he said, “There’s a demon here, a homosexual demon.”
And I thought— I mean, you know, usually in church, often you will feel it’s you and they’re not talking about you directly, But he was talking about me. And he said, “We learned that there’s a homosexual demon here.” And he walked right in front of me and put his hand on my head and started trying to cast the homosexual demon out of me.
And I felt so crushed and so betrayed by my roommate, you know, I literally got up and I grabbed the guy’s— the evangelist’s arm and twisted it. And I said, “There’s a demon in here, and it’s you.” And I just walked out of the church.
JESSE BROOKS: I remember growing up in the church and being a part of it, with my mother, with my brothers, and hearing a homophobic sermon that would just make me want to shrink in the pews and be silent and look around and see other men feeling the same way.
And then after church, no one talks about it. I mean, we just go on to our homes. And what I finally realized is how damaging that was to me as a young person trying to accept his identity.
And I was in so much pain. And I carried this silently around, and I was looking for a pain release. And people used to say that you use drugs because you have all this stuff inside. And so the drugs took away the pain, but then it started taking away everything else. And it just led to this whole cycle, years of deterioration for me. I was involved in the cycle for a long time.
NARRATOR: It was during those years that Jesse contracted HIV. At the same time in the ’80s, drug use in cities like Oakland had become its own epidemic.
WILLIE DUDLEY:: And this is a local area where folks come and hang out. A little drug use goes on here, intravenous drug use, smoking the crack. A lot of the sex workers come here also.
My name is Willie Dudley. I’m a recovering addict. I have 11 years clean. I have a different life now. I can see life through life’s terms. So not that I don’t think about it, because there were some good times with the drugs now. There was some good times. But there was more bad times, which led me to get various things such as herpes, HIV.
NARRATOR: Back when Willie was infected, HIV was spreading fast among addicts, but it was invisible. Deaths were mounting and no one was paying attention.
WILLIE DUDLEY: A lot of our clients, the first thing they’ll say is, “God bless you. Thank you all. I wish you all had been here back when I first started in the ’60s or the ’70s. This—I’ve got 15 to 20 friends that are in the ground now.”
NARRATOR: Drug addicts were vulnerable to HIV because the virus entered the community at a particular time in history.
ROBERT FULLILOVE, Ed.D., Columbia University: In the 1980s, it’s important to recall that with communities becoming increasingly poor, with high rates of unemployment, with ferocious housing segregation, the jobs were no longer there.
And all of a sudden, the drug guy, the dope man, became the person who for all intents and purposes was the employer of first choice.
NARRATOR: The business boomed. People got hooked, and overdosed. Hospitals were overwhelmed.
ROBERT FULLILOVE: So we’re at this crisis point. We can recognize that drug abuse is a public health challenge and treat people who are dealing with this challenge. Or we can do what was ultimately decided, we can declare this as a criminal justice issue, that this is a crime that’s being committed within the community that requires a massive police response.
NARRATOR: The law that mattered most to the spread of HIV was known as the “drug paraphernalia law.” It made it illegal to carry a needle.
ROBERT FULLILOVE: So it became clear to drug users that if you’re going to have a spike on you, you were really running a terrible risk. So somebody said, “Why don’t you come into my building, and I will sell you the drug of your choice and I’ll also rent you some equipment that you can use to shoot it up.”
MAN IN SHOOTING GALLERY: Well, it’s a shooting gallery, OK?
INTERVIEWER: How many people are coming in here today?
2nd MAN IN SHOOTING GALLERY:Up to 100 a day or more.
NARRATOR: It was the perfect way to transmit the virus.
ROBERT FULLILOVE: With the sharing of needles, if you had just one person in a network of people who were sharing needles become infected with HIV, that virus is going to be passed to everybody.
NARRATOR: And that’s what happened. The virus spread between users, to their partners, and deep into the community. It was the unintended consequence of the drug paraphernalia law.
JEFF McDOWELL, Atlanta Harm Reduction Center: I think that our lawmakers had very good intent when they wrote paraphernalia laws. But our lawmakers are not public health experts.
NARRATOR: Public health advocates like Jeff McDowell decided they had to break the law. A former Marine turned social worker, Jeff has been setting up shop for 17 years in this neighborhood of Atlanta called “the bluff.”
JEFF McDOWELL: One thing we do is the needle exchange. What we want to do is create an environment, a way of thinking amongst drug users that says, “One clean needle, one shot,” and provide the disposal services for people to be able to come and properly dispose of the syringes.
NARRATOR: Here in Atlanta, syringe exchange is still illegal, as in many places in the country. And it’s controversial.
JEFF McDOWELL: It’s always the age-old question, the age-old argument, that we’re encouraging drug use.
NARRATOR: But over the years, study after study has proved syringe exchange programs do not increase drug use.
JEFF McDOWELL: It’s not about debating the legitimacy of it. We know that it works. We know that it’s necessary. And we know that with every clean syringe we give, that’s one less chance or risk of not only drug users being infected, but their partners being infected.
Your partner uses now?
CRUZ: Uh-huh.
JEFF McDOWELL: When was the last time— have you been sharing any needles?
CRUZ: No.
JEFF McDOWELL: So you’ve been coming and getting needles from us, and then using your own clean works. What about— the unprotected sex is what you’re concerned about?
CRUZ: Yeah. Yeah.
JEFF McDOWELL: What happened that you decided to get a test today?
CRUZ: Just to get me out of the house and actually go and do it. The system’s right here and ready, you know?
JEFF McDOWELL: Yeah. So in the event that this test doesn’t turn out the way you want it to turn out, then what?
CRUZ: Cry like a baby. No, I wouldn’t know what to do.
JEFF McDOWELL: One thing I want you to know is—
CRUZ: Honestly, I wouldn’t know what to do.
JEFF McDOWELL: Either way, I want you to know that you will not be alone from the moment you walk from this truck, OK? We’re definitely going to stay with you and provide our support for you that you need, OK?
What we want to do is engage folks in their own environment, just as they are, wherever they are, on their terms.
OK, you ready for her? OK. I’m pulling for her. I think it’s going to work out for her and that she does get a negative result, and we’ll go from there. We’ll go from there.
NARRATOR: Her HIV test results will be ready in 10 minutes.
JEFF McDOWELL: We’re not here to tell them to get off of drugs. I mean, you know, we’re not drug counselors. Some of us are in our own right, but we’re here from a public health standpoint, that we want to see the community healthier. And right, now that mission just happens to be HIV/AIDS.
PASTOR JEFFREY: This is unbelievable. Fifteen churches in the local area?
JEFF McDOWELL: Yeah. Twenty-two, actually.
PASTOR JEFFREY: Twenty-two churches in the local area?
JEFF McDOWELL: Yeah.
PASTOR JEFFREY: This is the mission of the church. We should put a cross on.
JEFF McDOWELL: It’s really difficult for a lot of the older pastors. The political fall-out is too much for them to become involved with HIV/AIDS and some of the techniques that we use.
PASTOR JEFFREY: For a lot of churches, and being a pastor myself, we’ve missed the mark. You know, it’s a documented fact throughout America the black church was the avenue which all social ills came through.
JEFF McDOWELL: Uh-huh.
PASTOR JEFFREY: And it really saddens me, man, because the church— we’ve— we missed it.
JEFF McDOWELL: How you feeling? How you feeling?
CRUZ: Oh, a lot better! [laughs]
NARRATOR: Her HIV test is negative.
JEFF McDOWELL: I’m real proud of you, man! I’m so proud of you.
NARRATOR: Interventions like this have been one of the success stories of the past 30 years, radically reducing the spread of AIDS among addicts, their partners, and the most vulnerable, their children.
TOM: Check, one, two, three— check, check, check.
[singing]
It started off in the emergency room,
Delivery’s by the womb,
Epidemic baby destined for doom.
Moments passed as the doctors expecting me to lay in my tomb,
But as seconds passed, birth, it was too late,
Seconds passed curse,
Four years later, didn’t know life for what it’s worth
But the stressin’ get worse,
The lessons got worse, confessions got worse,
Brother Jeffrey dispersed.
Seven days later, he returned to the earth,
Shattered hopes and dreams
Now he rest in the casket engraved in dirt.
Shed tears, reminisce on a past that hurts.
And that’s my darkest pain.
That’s my darkest pain.
It’s my darkest pain.
The song is called “The Darkest Pain,” and it explains how I have a little brother that died from AIDS, and how my mother passed away and sort of how I felt about that.
[singing]
Night sweats, woke up to a nightmare,
Just to realize what you petrified about is living right here.
Mom losing weight
She’s only 26 years old and she’s dying of AIDS
Karma came back rougher, life’s switched up—
I think I was maybe probably 5 or 6 when I knew that I had HIV, but I did not understand exactly what HIV was and what it did to the body.
NARRATOR: No one knows how many babies were born to mothers with HIV in the early years. Not many survived.
TOM: [singing]
Life’s full of criticism, I’m on a mission.
Taking medication by the prescription.
NARRATOR: Tom and his friend Keith have a name for it. They call themselves “bornies.”
KEITH: Being a borny, being born with HIV, is a lot. I was the last one born in my family, and I was the only one born with HIV. And my mom at the time was not doing well. She was doing drugs, I believe. So she couldn’t take care of us, so they put us into foster care, all of us. But they were going to split us all up into different houses, me and my brothers. I have three brothers. So they were going to split us all up. But my grandmother was just, like, “We’ll take them all.”
MISS IDENE: Altogether, at least about 25 of my grandkids, 25, and all of them come from from— from— into this house. Yes, all of them come into this house.
So Keith’s mother, she passed away with the virus. She didn’t take care of herself, that’s the main thing. That’s what— what I mean by she didn’t take care of herself, she was still using. And she knew she had it. She was still using it, crack cocaine. She was the sweetest. But the only thing, the drug just overpower her.
Keith come to me when he was 2 weeks old. I’ve been having him ever since he was 2 weeks old. And we spoiled him because Boston Medical and the doctors said he wouldn’t make it no more than three years. And he’s 20 years old now.
And he always got a nice word to say, never get into no problem, never have to go to school for him. The only thing, if he just could keep this room clean.
Why you have such a fit about not wanting to do your room?
KEITH: If I get up and it’s dirty and I clean it, when I come back home, I’m just going to dirty it again.
MISS IDENE: Oh, that’s it.
KEITH: She’s got that toughness about her. [laughs] I think if she wasn’t so tough, people would run all over her. So I think that’s a good thing. I like it.
My grandmother didn’t like for people to be, like, afraid of me. So she would— she would tell them before they got to— got around me so they wouldn’t be all, like, “Oh, I’m not going to eat near him because he’s got something.” And she’d be, like, “Well, if you’re not going to eat near him, than you can’t eat near any of us because we eat near him.”
MISS IDENE: Well, we’re going to have a big dinner, Thanksgiving.
KEITH:: So I feel like I was always just me. Like, if you don’t like me, then that’s too bad. But there was this one girl that was in my neighborhood and I liked her. And so I was, like, “Oh, I like you a lot, blah, blah, blah, but I should kind of tell you”— and this is when I was first starting to do this. So I was, like, “I should tell you that I have HIV.” And she was, like, “Oh, yeah?”
And she was, like, cool with it that night. But then the next night, she was, like, “Oh, I don’t know. I’ll talk to you later.” Like, “All right, I’ll see you later.”
I was, like, “Oh, wow.” It’s never happened. But then I was, like, “OK, OK, whatever, though, because I’m still a cool person. You don’t want to chill, that’s fine.”
NARRATOR: So for a while now, Keith’s been dating a young woman who is also HIV-positive.
WOMAN: Actually, I knew Keith for a very long time, you know, playing as kids, and I really got close to him. I think I find it more easier to date someone who’s HIV-positive because you have a lot in common. You know, you don’t have to hide certain things from them. They know how you feel if you’re sick. You know, they— they experience a lot.
It’s really hard because you feel like you’re living a double life. And it’s a crappy secret to keep because it’s so hard to keep up with every single thing you tell everybody. So it just becomes this intricate web of lies.
And so when it comes to romantic relationships, it’s— it sucks. I just don’t even want to deal with those as of right now because it’s a lot because you have to think about, “Do I like you enough to tell you this? Do I trust you enough to tell you this?”
TOM: You know, sometimes you would make a friend, and you would lose a friend. Like, I would have friends that had HIV or AIDS, and then, you know, next year, you would go to camp and you would wonder why they’re not there, but you would know why they’re not there, if they’re not there. You know, it’s because they had passed away.
I’ve seen my mother pass away from AIDS, so I always kind of carry that with me.
[singing]
Life’s switched up. Now it’s her time to suffer.
Hated the choices that she made, but I loved her.
Hated the choices that she made, but I loved her.
Yeah, still loved her. Still loved her. Had to learn to forgive. I still loved her.
NARRATOR: The number of babies born with HIV peaked in the early 1990s, when many women were swept up in the twin epidemics of HIV and crack.
JEFF McDOWELL, Atlanta Harm Reduction Center: Crack cocaine came along. Of course, you know, one of the first communities we saw all the devastation in was the African-American communities. There was just a huge supply of the drug, and just the mere addictive nature of the drug, a lot of people latched on very, very quickly.
ROBERT FULLILOVE, Ed.D., Columbia University: The most important thing about the crack cocaine epidemic was the degree to which it was marketed in black and in some Latin communities as an aphrodisiac. This is a drug that will enhance sexual pleasure. This is a drug that will make you forget all the cares and woes of everyday life. And it will help you forget because the nature of the sexual experience you’ll have will be just mind-blowing.
NARRATOR: A crack habit took everything. You’d sell whatever you had for the next hit.
ROBERT FULLILOVE: When there was nothing left, women were told, “Well, baby, if you ain’t got no money, you’ve always got you.” And then there’d be a negotiation for a crack for sex exchange. In many instances, this kind of sexual bargaining, this kind of crack-related sex work, was carried out without there being any kind of protection taken.
If you’re the demander, you get to call the tune. And if you say, “We’re going to have sex without a condom,” that was what you were going to do because the addiction was that powerful.
NARRATOR: Crack and sex work is a lethal combination.
WILLIE DUDLEY: This is East 14th. It’s mostly everything from selling crack to sex work to hustling, whichever form that they can get that in. That’s what— this is the main street that it mostly goes down on.
Yeah, she’s one of our regulars. She’s about 16.
When you’re under the influence of crack, sometimes if a guy says, “I’ll give you $20 more if you don’t use a condom,” generally she’ll say, “Well, OK.” Whereas if she’s got a lot of money, she’ll be, like, “Naw, dude. If you ain’t got no condom— that’s the only way we going to do it.” Unless, of course, he said, “50 bucks.” Then she’ll be, like, “OK, but I’m going to remember you.” She’ll try to put a fear in him.
But generally, they’ll do what they have to do. And that puts them more at risk.
NARRATOR: By the late ’80s, the crack epidemic was being blamed for the tremendous rise in violence and crime in the inner city.
JEFF McDOWELL: America was not prepared. We didn’t know how to treat addiction. So with this whole crack thing hitting the neighborhoods, it literally destroyed neighborhoods.
NARRATOR: Under pressure, Congress pushed through tough new laws. Sentences for crack would be 100 times more severe than for cocaine offenses. The number of arrests skyrocketed.
JEFF McDOWELL: The only problem with that is that they were mostly young African-American males rounded up and thrown into jail. Many of them were getting sentences of 10, 15 and 20 years for $10 worth of crack cocaine. But it was about showing a response.
It was the beginning of an unbreakable chain of young African-American men going to jail for drugs.
GEORGE HERRON, Fulton County Jail: Take you down the hall here and show you the chronic care unit—
NARRATOR: In Atlanta’s Fulton County jail, like many correctional facilities around the country, inmates with HIV are not segregated.
GEORGE HERRON: Our policy has never been to segregate individuals that are HIV-positive. It’s communicable, but it’s a disease that a person has to have intimate contact in order to catch. Since this is a body-to-body, fluid-to-fluid type of a disease, we don’t feel it would be right to segregate individuals that are HIV-positive.
NARRATOR: The warden says inmates don’t have intimate contact. Dr. Earl Joyner says they tell him something else.
EARL JOYNER, M.D.: They do have sex. They have more than a little. And the party line is giving out condoms is considered condoning sex. And I know in Alabama, it’s supposed to be against the law to have sex in prison. So if you give them a condom, then you’re facilitating them breaking the law.
Tripp? Tripp?
Dr. EARL JOYNER: People ask me sometimes do I supply condoms. And I think that would be the surest way for me to get fired.
Tripp, you got something more important to do?
But for reasons even other than HIV, it would make good medical sense to allow people to protect themselves.
TRIPP: I been locked up 11 months.
Dr. EARL JOYNER: So where were you before you got here? Were you at another jail? Were you on the street?
TRIPP: Yeah. Yeah. I went to Tennessee, from Tennessee to Gainesville.
Dr. EARL JOYNER:: But you got here in September.
TRIPP: I was on the front page down there in Tennessee. [laughs]
Dr. EARL JOYNER:: Oh. Front page news.
TRIPP: Front page of the news.
Dr. EARL JOYNER: You know, some of the guys do bad things and they don’t have good intentions. But some of them have been through some really bad stuff. So there’s no room for judgment. It’s just, listen and take care of the problems.
TRIPP: What was my T-cell?
Dr. EARL JOYNER:: T-cell was 289 back in September, and now it’s 276. So you’ve not been taking meds consistently. So if you’re here long enough, we’ll see. I bet you we’ll get you up in the 400s.
TRIPP: Well, I hope so.
You’re all right, Doc. I don’t care about the rest of them. You know what I’m saying? The rest of them, they ain’t going to do nothing for you, you know what I mean? They’ll sit there and let you die. You’re all right, Doc.
Dr. EARL JOYNER: People should care about inmates that are HIV-positive. If I showed you a list of inmates that are being paroled out of state prison per month, it would take up two pages. So these people don’t stay here indefinitely. They’re not here for life. They go back to the community.
ROBERT FULLILOVE, Ed.D., Columbia University: This period in the 1980s is when you first started seeing men who were infected with HIV finding their way to prison who would ultimately return to the community— maybe for two or three years. Then they’d be part of the recidivism statistics, where you had a 7 in 10 chance of going back to prison, creating this cycle that took you from the community to the prison, then back to the community again.
I mean, think about it. There are many communities where on any given day, somewhere between 55 to 60 percent of all the young men are in jail, on probation, or under the supervision of the courts. They’re no longer in the community.
If there are more women than there are men, there are going to be changes in what happens in the competition for a man. Men who are sexually active aren’t necessarily going to be forced to use condoms because, after all, “Well, baby, if you don’t want to give me what I want, there’s always your girlfriend over here who’s made it real clear that she’ll do whatever in order to keep me around.”
GAIL WYATT, Ph.D., Psychiatry Dept., UCLA: For males, that means that they have a shopping spree. They can find a partner who wants to do what they want to do. I may have to take some risks to prove to that person that I really care about them, that I trust them, that I’m not the type of woman who’s going to create a lot of drama, that I’m pretty even-keeled, I don’t ask for a lot.
And I’m not going to bother that person with having to make troublesome decisions about condom use or contraceptive use, or really the consequences of having sex with me. I’m going to handle that on my own.
ROBERT FULLILOVE: The fact that you’re starting to see in the 1980s a real increase in the number of women who were infected with HIV because of heterosexual sex, not because of drug use, has to be because the whole nature of the mating game has changed in the community because so many men are gone.
NARRATOR: No one knows how many women were infected by the early ’90s because there was no way to count.
MARSHA MARTIN, D.S.W., Get Screened Oakland: At that time, we had women who were having children, women who were pregnant, women who were on the outside, women who were impacted by this disease. And they were invisible and hidden.
Women had HIV. However, the government didn’t have a way to classify the illnesses people were dying from, the women were dying from.
NARRATOR: Women were dying from illnesses the government didn’t classify as AIDS, like ovarian cancer.
DAZON DIXON DIALLO, M.P.H., Sisterlove, Atlanta: You must look at us differently because we are experiencing this thing differently. We’re dying faster. We’re having babies that are born sick and are dying fast. We know that women are dying of diseases and opportunistic infections that they’re not getting AIDS diagnoses for.
NARRATOR: The official definition of AIDS was based on the early cases in men, not women.
DAZON DIXON DIALLO: They may be dying without access to care and treatment.
MARIA: I’ve been, like, having problems, like, with my medicine and stuff, you know? They don’t want to give me the medicine. Like, AZT— he will not order that in.
DAZON DIXON DIALLO: They also may be dying without getting any benefits that are available to people with AIDS.
MARIA: No, me and my husband, we sleeping on the floor for now because it’s overcrowded, my four kids.
COUNSELOR: The kids are there, too?
MARIA: Yeah. The court placed them in my mother’s for now.
DAZON DIXON DIALLO: I was just right here in Atlanta trying to help women protect themselves or help women get into care because they were sick and they needed services. And so in the late ’80s, we were, like, “No, we won’t stand for this. Women must be counted.”
PROTESTERS: How many women have to die before they say we qualify?
DAZON DIXON DIALLO: It was a two, almost a three-year campaign that was waged.
NARRATOR: BY 1991, a pro bono lawyer concerned about her clients who were dying without services decided to take the government to court. They sued Louis Sullivan, the secretary of Health and Human Services, for wrongfully denying women the care and treatment available to men. Still, there was no reaction from officials. At the CDC, the demonstrations escalated.
Finally, officials responded. From now on, the definition of AIDS would include women’s diseases, too.
MARSHA MARTIN: That activism saved lives, saved women, saved women and their children, and also protected them and their rights.
NARRATOR: Under the new definition, the number of women with AIDS jumped more than 60 percent.
DAZON DIXON DIALLO: That spike happened simply because people who had not initially been included in the overall surveillance and in the diagnosis of AIDS were finally being included.
NARRATOR: It was a tipping point. Within two years, half the new cases were black, and it’s been that way ever since. Still, it remained a hidden epidemic inside black America. To break the silence, it would take a celebrity.
MAGIC JOHNSON, Los Angeles Lakers: First of all, let me say good after— good after— late afternoon. Because of the HIV virus that I have attained, I will have to retire from the Lakers today.
MARSHA MARTIN: Magic Johnson goes public. And it was absolutely extraordinary. People saw this spectacular person and it’s, like, “Wow. Wow, Magic?”
MAGIC JOHNSON: We were into the exhibition season, and I got a call from our doctor who said, “You got to come home.” And we were in Utah and I said, “Well, can I come home after the game?” We were coming home anyway. He said, “No, you got to come home right now.”
So I flew back to LA, and when I walked in his office and sat down in his chair and said, “Hey, what’s up?” he begins to tell me that I had HIV. And so, you know, a lot of times in your, you’d thought— I thought I’d made all the right moves and right decisions, and I was really careful about what I was going to get into and what I decided to do. And I thought I’d made all the right moves.
And then just at that moment, you found out that you didn’t make all the right moves, and your life is turned upside-down just in a matter of seconds. And it was a difficult thing to hear. And I have to be honest. At that time, I knew about AIDS and HIV, but I didn’t know a lot about it, so—
RENATA SIMONE, Producer/Director: What did you think?
MAGIC JOHNSON: You know, I was like most people, “Oh, I’m going to die,” you know? At the very first, when he first announced it to me, I thought, “Oh, man, I’m going to die. I think it’s over.” And no, he said, “Whoa, whoa, no, no it’s not like that,” he said. “So what we have to do is run a series of tests.”
But the hardest thing I had to do was tell Cookie. Nothing was more difficult than hurting the person who loved me the most. And she was pregnant with our son, E.J.
And she started to cry, of course, and wanted to know what that meant for her and the baby. And you know, I really think that God looked out for me with Cookie and the baby, our baby, who is now 19, E.J., because when we found out the news that she did not have HIV and the baby was fine, as well, I told her, “I could understand if you want to leave me.” And she hit me so hard upside my head and she said, “No, we’re going to beat this together.”
NARRATOR: In 1991, there weren’t a lot of medical options, but Magic’s doctor had an idea.
MAGIC JOHNSON: He said, “Let me get you in touch with, you know, a private, a leading doctor in HIV and AIDS, Dr. Ho. And I’m going to send you out to New York, and also you can talk to him.”
DAVID HO, M.D., Aaron Diamond AIDS Research Center: I mean, I think I reflected my thinking to him, in that this, at that time, was a death sentence, and yet research was progressing quickly, and because we and others were working on a number of new compounds which we felt were great and could possibly make it to the clinic in a few years.
NARRATOR: For a decade, doctors had tried to stop the virus without success. But Magic was diagnosed when David Ho and others were just starting to test a new approach.
Dr. DAVID HO: So I wanted to— while presenting him with very tragic news, wanted to give him something on the positive side, in a realistic way, and said that, “There are a number of promising drugs coming down the pike,” and, “Just, you know, take good care of yourself. Hang on, and these drugs may help you out someday.”
MARSHA MARTIN: But remember, no one wanted to play with him. And no one wanted to be on a basketball court with Magic Johnson. And it frightened everybody. “What if he fell, what if he slipped, what if we got sweat on us?”
NARRATOR: Magic wanted to stay in the game, but players across the country balked. Even his best friend, A.C. Green, rejected him.
MAGIC JOHNSON: That really hurt me. A.C. is a very religious man, so he felt that the way I got the disease, you know, sleeping with a lot of women— he had a problem with that, and so then he had a negative reaction.
So as I began to talk to A.C. — because we had a close relationship before this went down — I said, you know, “We all make mistakes. You know, I made a mistake and it’s costing me.” I said— you know, I told him, “I’m giving up the game that I love.”
At that time, I said I didn’t know how long I was going to be on earth, so “I need you to support me, not be upset and not be disappointed because there’s no man that’s perfect. You’re not perfect.” And I told him he’s not perfect. And so, “You’ve made mistakes and so have I.”
And so, oh, man, when I told him that, he just broke down and started crying and hugged me and prayed for me. And that was a big step for both of us.
CRAIG WASHINGTON, AID Atlanta: Magic Johnson’s disclosure made it OK for millions of people to say “AIDS.” It wasn’t just that he was a basketball legend. He was so, in many ways “John Black Man Next Door,” or “Joe Every Guy,” you know, for— you know, for people who are not black, perhaps, someone that so many could relate to.
And if this could happen to Magic Johnson, this could happen to me or my son or my father or my brother or my teacher, and so forth.
And on the other hand, I was resentful because by that point, countless gay men, women, people who had done injection drugs, what have you, had died or were living with HIV, courageous people who were speaking out in as early as ’83 and ’84, taking the risk before it was acceptable to speak just about AIDS, period, much less living with HIV. And they lived and died without much of a line in the media.
PHILL WILSON, Black AIDS Institute: We could have nipped this epidemic in the bud. We could have gotten ahead of the curve, and we didn’t because we did not have the political will to do so.
In the very, very beginning, black leaders didn’t know, absolutely didn’t know. Every message that was being communicated to black leaders is that it was not about them.
Now, granted, you know, they were glad that it was not about them. They embraced that. And so when we got to the point where we could provide data to say, “That’s a mistake,” you know, “It is, in fact, about you, it is, in fact, about us,” you know, black leaders were slow to respond.
JULIAN BOND, NAACP Chairman Emeritus: Was it on my radar? I don’t really know if it was something that I felt I didn’t want to get engaged in, or what the reason was. But anyway, I didn’t do what I could have done and should have done.
RENATA SIMONE, Producer/Director: What do you think about that?
JULIAN BOND: Well, I feel badly about myself. It’s a bad reflection on me that I didn’t take a more leading role than I did. I could have. I should have. I was in a position of responsibility. I could have done it, and I didn’t.
ROBERT FULLILOVE: Now, in their defense, it’s very clear that if you’re a black leader, there are a bunch of things that your constituents are asking you to do. There’s a list of problems that people in the black community face. And not surprisingly, black folks want their leaders to do something about them.
So when you show up in the mid-’80s saying, “Excuse me, you now need to add AIDS to the list,” they said, “Where am I going to put it? I’m already doing all this stuff, and I’m not being very effective in any of my efforts. I’m not improving the quality of housing, I’m just talking about it. I haven’t done anything to lower the high rates of unemployment. I haven’t done anything to improve the quality of the education that kids in this community are getting. And now you’re asking me to add yet another thing to my list of things to do?”
NARRATOR: And for leaders, there was another, deeper problem.
ROBERT FULLILOVE: In the 1980s, it’s important to recall that we no longer have a major Civil Rights movement. And the trauma of the ’60s — the lynchings, the killings, the riots that characterized the long, hot summers — yeah, that stuff was all behind us.
And when you raise them in community settings, people say, “Oh, man, you know, aren’t we done with that? Isn’t that all behind us? Can’t we just, like, move on?” That shift made us unable to speak collectively about the threat that HIV was posing.
NARRATOR: And so the virus continued to spread. Meanwhile, in research labs across the country, David Ho and other scientists had been testing their new way to attack the virus. By the mid-1990s, they were about to make a breakthrough. It was a combination of old and new compounds, a drug cocktail.
Dr. DAVID HO: By 1995, we were able to formulate the first cocktail therapy.
NARRATOR: The idea was to attack the virus in three ways at the same time— three drugs, three weapons.
Dr. DAVID HO: And within a matter of weeks, we realized that such a new approach to treatment was much more promising. And certainly, a year later, we recognized that the new therapies were controlling HIV very, very well.
Over the years, we simply had to make some adjustments on Magic’s medications, and he’s done remarkably well. But I want to stress that his therapies from 1995 on was really no different from what a typical HIV patient was taking.
Which arm do you—
MAGIC JOHNSON: I’m going to let you decide. Whichever one.
Dr. DAVID HO: This is usually big enough for most of our patients, but let’s see. [laughter]
I have worked with Magic Johnson for 20 years, and so we developed a pretty good rapport.
You probably have the biggest veins of any patient I ever had. [laughter]
But each time, I still emphasize to him that the biggest reason for drug failure is patient non-adherence. And so it’s really crucial for him to stick to the prescribed regimen and take his medications religiously so that the virus doesn’t get chances to escape from the drug action. I think he’s got this drilled into his head and I think he’s done a pretty good job.
MAGIC JOHNSON: Well, I’m not cured, I’m just— I’ve been taking my meds. I’ve been doing what I’m supposed to do. So no, there’s no cure, and I’m living with this virus in my blood system and in my body. I got to be careful.
[Twitter #frontline]
NARRATOR: Over the next few years, researchers developed medicines that transformed AIDS from a death sentence to a chronic manageable illness. Headlines called them miracle drugs and declared that AIDS was over. The media spotlight moved on.
But in many countries around the world, there were no medicines. AIDS was still a killer. By the end of the decade, millions had died.
Then in 2003, in the middle of the annual State of the Union address, President George Bush shocked the world with an unexpected announcement.
Pres. GEORGE W. BUSH:Today on the continent of Africa, nearly 30 million people have the AIDS virus. Many hospitals tell people, “You’ve got AIDS. We can’t help you. Go home and die.”
In an age of miraculous medicines, no person should have to hear those words. [applause] I ask the Congress to commit $15 billion over the next five years, including $10 billion in new money, to turn the tide against AIDS in the most afflicted nations of Africa and the Caribbean. [applause]
NARRATOR: It was unprecedented. After decades of begging for funds for their own projects, activists were stunned.
MARSHA MARTIN: I was working at AIDS Action at the time. I was at that State of the Union. I was there. We had prepared a press release that said, “Mr. President misses an opportunity to talk about HIV.”
We had to leave. I left the State of the Union early, got in a cab, got back to the office and we wrote the press release that said, “Thank you, Mr. President for your leadership on HIV,” because it had never happened before in the history of this country and the world that a single health issue had been given this kind of attention. It’s extraordinary.
And so here begins PEPFAR. Wonderful. Because, in fact, the epidemic was ravishing the globe.
NARRATOR: The President’s Emergency Plan For AIDS Relief. In the years since, the U.S. has spent nearly $32 billion on AIDS around the world. Although there were controversial political and financial conditions to the funding, PEPFAR has had an impact. The number of new cases overseas has dropped year by year.
GAIL WYATT: I think that America has been very generous about providing health care, as well as HIV/AIDS prevention, to other parts of the world, to people who wouldn’t get those kinds of care. And I think that that’s what makes us who we are as a country, that we do extend ourselves, we do reach out, we try to make the quality of life better for other people.
But I don’t think that we can lose sight of the fact that we’ve never really been able to achieve those goals for Americans.
BAMBI GADDIST, Ph.D., South Carolina AIDS Coalition: I believe we should make an investment in other countries, but I also know that I’m in Africa right now. As a state, I’m there. Sometimes my staff feels like we’re there. Every time we test another young person positive, we’re there. The question is, What is in the best interest of our community?
NARRATOR: At home in the U.S., there were places where the life-saving new medicines were a long time coming, especially in the South, in places like Selma, Alabama.
MEL PRINCE: [on the telephone] I know you’re tired of me, but that’s OK.
NARRATOR: Mel Prince has been running a small clinic in Selma for 17 years.
MEL PRINCE: Our numbers are steadily growing. We bring in as many new patients as we’ve been bringing in all along. And it’s increased in the last, oh, 7, 8 years.
WANDA: He needs to reapply for the program, too, but I don’t have a number for him.
MEL PRINCE: Most of our clients live at or below the poverty level.
It’ sad, but we need to work on them because that’s a mother, father both positive with— with how many kids?
WANDA: Three. Because that was the problem, too. They had an issue with the food.
MEL PRINCE: Sounds like they’re going to be homeless if we don’t get it squared away. The problem is—
WANDA: They will be homeless again. They have transportation problems. And you know, they live, you know, about two hours away, so—
MEL PRINCE: So we’re left with picking them back up again.
WANDA: Yes.
MEL PRINCE: That’s almost to the Mississippi line.
WANDA: Mississippi line.
MEL PRINCE: There’s about three or four counties below us that there’s no doctor, no clinic, no agency that services those counties. Our patients do not have cars. There’s no transit system. We’re having to pick our patients up and take them back home, which can take about two hours down and two hours back.
I don’t think we have a solution for the transportation problem. Funding? We’re never going to have enough funds.
NARRATOR: Mel’s been fighting for funds since the beginning. It was worse back in the ’90s, when the miracle drugs were saving lives, but her patients were dying.
MEL PRINCE: There was nothing I could offer my patients. They were hearing about it, too. They were watching their TVs. They were listening to the radio. The clients felt defeated. They felt like the system always let them down. So what should be different about this?
NARRATOR: She says it took 10 years before she was finally able to get the new drugs for her patients. Meanwhile, suspicions and myths about the cause of the epidemic spread.
MEL PRINCE: Every now and then, we’ll have a patient that comes in and they think they planted HIV in our community. And then we argue, “No, this is not something that was planted in our community.”
NARRATOR: This community is just 80 miles from a place called Tuskegee. Here officials promised poor farmers free treatment for “bad blood.” The truth was they had syphilis, and they weren’t being treated. they were being monitored and studied as the disease ravaged their bodies.
MEL PRINCE: I hate talking about it. I hate thinking about the Tuskegee experiment. And with Tuskegee being right here in Alabama, that just adds fuel to the fire.
NARRATOR: Over the years, many men died. Women and children were infected, too.
BAMBI GADDIST: There’s a question that looms in the minds of people. They say, “Why’d you pick African-Americans to experiment with syphilis?” So they believe if it happened once, it could potentially happen twice. People of color distrust systems, medical systems, because of the Tuskegee studies. And I’m not sure if we’ll ever get over it.
MEL PRINCE: Some of our patients even tell us that HIV’s not real, or that it’s something to scare us. And we just educate them as much as we can.
In the South, in the black belt, there’s a great stigma around HIV. People are afraid to eat behind individuals. They don’t want to live next door. We even had where people threw out refrigerators and stoves after that person died. That’s how ignorant it can get in this area.
PATRICK PACKER, Southern AIDS Coalition: The stigma of HIV has led to a huge outbreak in the South now, that the epidemic has just exploded to where you have almost 45 percent of all of the new HIV cases are in the South.
MEL PRINCE: The sad part is we have people that die alone as a result of somebody being afraid to touch them. Especially at the end of life, they’re wanting some kind of counseling, some kind of confirmation that gives them a peace.
We’ve got one or two ministers in the area that might talk to them on the phone, but that’s basically it. Our patients feel like they’re hypocrites because they teach one thing and they live another.
Rev. MICHAEL JORDAN: I think the African-American church in the area of HIV has really been too quiet.
NARRATOR: Pastor Michael Jordan leads a church in Birmingham, Alabama. In 2004, he made headlines.
Rev. MICHAEL JORDAN: I’m known for my boldness, and God has blessed it. The words was very stern. AIDS is God’s curse to a homosexual life. I think it stinks in the nostrils of God.
Rev. MICHAEL JORDAN: I do extend grace, mercy and forgiveness to that homosexual, OK? I don’t close the door on you. I don’t think it’s the sin of homosexuality that angers God, I think it’s the unrepentant, arrogant spirit about my sin that angers God.
NARRATOR: Clergy like Pastor Jordan cite the Old Testament.
Rev. MICHAEL JORDAN: In Leviticus, around 18:21, it says it’s an abomination. I think it interrupts God’s creation, and we can’t be fruitful and multiply.
PATRICK PACKER: He doesn’t get it. He doesn’t get that God loves all his children. He loves the gay member of his family. God loves the transgendered member. God loves the person that is struggling with drug addiction and gets infected by using needles. God loves them, just like God loves his members of his church that might be struggling with other issues.
Rev. MICHAEL JORDAN: Sometimes you just can’t preach these ear-ticklin’ “God is good, and tell your neighbor that today is your day.” Well, today might not be your day. God is a god of judgment!
Rev. CHRISTOPHER HAMLIN: If God is a god of judgment, let God do the judging. And I think God is better able to judge than we are.
NARRATOR: Pastor Christopher Hamlin leads a church on the other side of Birmingham.
Rev. CHRISTOPHER HAMLIN: As a practicing Christian, my role model is Jesus. I take my cues from him. And when we look at the messages of Jesus, he addressed a lot of moral issues— divorce, fornication— but he never— we never see him talk about homosexuality, or even in descriptive ways. But he does talk about love and forgiveness, and that’s the piece that I draw on.
NARRATOR: For years, Pastor Hamlin lead the historic 16th Street Baptist Church. During a Sunday service in the fall of 1963, the Ku Klux Klan detonated a bomb. Four young girls were killed.
Rev. CHRISTOPHER HAMLIN: There was a lot of damage to the building, a lot of damage to the will of the community. But it also galvanized the community to say, “Enough is enough.” The death of those four girls was, I think, the pivotal point that ignited some very positive change not just in Birmingham but in the nation.
NARRATOR: That tragic event strengthened the bond between the church and social activism.
ROBERT FULLILOVE, Ed.D., Columbia University: In the 1960s, when I was deeply involved in the Civil Rights movement in the South, the church became our most important ally.
I started thinking in the 1980s that now was the time for us to go back to the church to say we have a real struggle on our hands. We’re going to have to deal with the threat that HIV is posing. I came up against the most incredible resistance imaginable.
PHILL WILSON, Black AIDS Institute: I’ll tell you a story. In 1985, I went to do a talk for the black Ministerial Alliance in Los Angeles, to talk about HIV and AIDS. And I’ll never forget this as long as I live. I’m in a church full of black ministers, and I’m talking to them about HIV and why they get involved.
And a minister stood up, and he was absolutely irate. And he said, “We’re not going to let them blame this one on us.” And I was stunned. And I took a deep breath and I said, “OK, can you tell me how many of us have to die? How many of your sons, your daughters, your sisters have to die before this is about us?”
ROBERT FULLILOVE: I think that this strain of conservative thinking goes back to the very origins of the church in the black community, that because it was so important for slaves, for example, to be able to celebrate a marriage, that meant that the children who were born of a union between men and women were going to find some stable environment in which to be raised, that it became impossible to entertain any other version of sexual behavior other than that which was thought to be most highly represented in the Bible.
JULIAN BOND: If an institution that so many people in a community attend weekly and listen to and believe in strongly says that the people who are likely to pass this disease along are engaging in abominable behavior, and they themselves are an abominable people, then it’s easy to say, “Well, they’re the people who ought to be scorned and cast off, and I need to put them to the side, and forget about them, not pay any attention to them.”
That attitude can be blamed for much of the spread of AIDS and the marginalization of AIDS in black America.
PATRICK PACKER: Thirgood CME church, rooted in the Civil Rights movement, dedicated to this community, is not afraid of taking on the issue of protecting this community around HIV.
NARRATOR: Patrick Packer tries to work with churches, to talk about the fastest-growing group of people with HIV.
PATRICK PACKER: The fastest-growing age group is young people, those between the ages of 16 and, like, 24.
I’m glad to have a conversation with young people to talk about how they need to protect themselves.
STUDENT: What are some ways you contract HIV?
PATRICK PACKER: Excellent question. It’s a very hard disease to get because you don’t get it by breathing on someone. You don’t get it by hugging someone or kissing someone. You actually have to pass bodily fluids from—
The young people that I speak with at my local church are the same that I speak with when I’m in Mississippi traveling. The young people are the same as the Catholic students that I speak with when I’m in Florida or the young kids at a small church in South Carolina.
STUDENT: Oh, I was just asking, like, what are some of the symptoms of HIV?
PATRICK PACKER: Excellent question. You can’t look at someone and tell if they’re HIV-positive, OK?
The questions that they’re posing— why don’t we have more education around this issue? Why is it that we only get two hours of HIV education in a year if you are in high school?
NARRATOR: Here in Alabama, as in most states, HIV education is one class a year and focuses on abstinence.
Ms. HERRION:All, right, next question? You can become infected with HIV by sleeping around. Everybody move. You can become infected with HIV by sleeping around. OK, strongly agree, strongly disagree? Reggie, why do you disagree?
STUDENT: Because you can’t catch HIV by just going to sleep all day.
Ms. HERRION:No, sleeping around mean you’re, like, sleeping with different people.
STUDENT: Oh. [laughter]
Ms. HERRION:All right, you still disagree?
STUDENT: Yeah, ma’am.
Ms. HERRION:Why do you disagree?
STUDENT: I disagree because you can sleep around, but you can wear protection, too.
Ms. HERRION:OK. Keana, why do you strongly agree?
STUDENT: Because while you having sex, even with protection, anything can happen. A condom can come off or whatever, and you can catch a virus or whatever.
Ms. HERRION:All right, that’s true. Even though you use protection, you can still catch HIV. Condoms are not 100 percent, 100 percent is what?
STUDENTS: Abstinence.
Ms. HERRION:Abstinence. Abstinence is the what?
STUDENTS: The key!
Dr. HERR, Perry County Schools Superintentent: [staff meeting] One of my primary responsibilities as superintendent is to make sure that we do implement the correct curriculum, and the correct curriculum is abstinence-based.
NARRATOR: Every year, the state director of health education evaluates the HIV and sex education curriculum.
ELAINER JONES: —bring me up to speed as to how you see abstinence playing out in the future with the students.
Ms. HERRION:Abstinence is the key thing that I stress because I tell them that’s the only sure way that you’ll know that you don’t contract an STD, not only just HIV.
NARRATOR: In the abstinence class, students learn information about AIDS and how it is transmitted, but only one way to protect themselves.
STUDENT:: Sex-free is the way to be.
Ms. HERRION:All right, great job, everybody.
ELAINER JONES: I just want you to be honest with me. Do we only want to stick with abstinence? Do you have any other preferences or any ideas about anything else that we can do?
SUPERINTENDENT HERR: I agree we should focus on abstaining, but at the same time, I am concerned about those who have already passed that point.
NARRATOR: For students who are already sexually active, the abstinence curriculum has nothing to offer.
STUDENT: When you all get through having you all’s sex or whatever, she tells you she has HIV, and how do you control that anger that you have?
STUDENT: What if, after y’all have sex, you tell them that you have it, and then they say they have it, too?
ELAINER JONES: Yes, they are having sex. We know that. We know that. And so—
NARRATOR: Despite the fact that they all know it, state law mandates the abstinence curriculum will stay in place for another year.
Ms. HERRION:Brandon, you had a question?
STUDENT: I mean, if you have sex, you know that you are HIV—
PATRICK PACKER: They know that their friends are having sex. They know they need to be talking about condoms. But the leaders on school boards, the leaders in their community are putting up barriers for them to have frank and honest discussions about information that’s going to keep them safe.
MARVELYN: The HIV education I had in school was really non-existent. And at home, my HIV education was, “Don’t bring no babies in this house.” That was my education. I’m from the South. People don’t talk about sex, let alone talk about HIV.
I remember in our wellness book, HIV was a picture of a helpless kid in Africa, and also a white, gay, skinny, skinny man. It was like if I came home with an F in wellness, my mom would think of it no different than an F in lunch. It wasn’t a serious class.
In high school, I was most athletic. My best friend was prom queen. I was a heterosexual, not promiscuous, all-American teenager. I was, you know, just a normal girl. And just HIV and normal didn’t go together, so I thought.
NARRATOR: Right after high school, Marvelyn met a man. He was older, and her first real love.
MARVELYN: I called him Prince Charming because, you know, Cinderella was one of my favorite movies as a child. And he came one night, he told me he didn’t have a condom. And from this moment, I’m thinking, you know, this is not a bad thing. This is my Prince Charming, the guy I want to be with forever. If the worst thing that can happen is pregnancy, that’s not a bad thing, you know, because I wouldn’t mind having his child.
NARRATOR: But what did happen was far worse than pregnancy. Within weeks, Marvelyn lay dying in a hospital bed.
MARVELYN: I was in the intensive care unit, actually unconscious, and the doctors told my family I had 24 hours to live. And the priest was called in to give me my last words, and they just didn’t think I would make it through the night.
NARRATOR: Sometimes when people first contract the virus, they get very sick right away. Finally, her doctors realized Marvelyn’s mysterious illness was AIDS.
MARVELYN: It hit me like a ton of bricks. I was shocked. I wasn’t shocked that I had contracted a virus that there was no cure for, one that was very hard to live with, I was shocked that I contracted a virus that I felt I would never get.
I feel like the community let me down. The school systems let me down. Ignorance makes you more susceptible to the virus because I’m— there’s no shame in my game. I was definitely ignorant and uneducated about the virus. And now I live with it.
DAZON DIXON DIALLO, M.P.H., Sisterlove, Atlanta: We do these things not because we choose to be unsafe or we choose to be on a path of self-destruction. We do these things because we don’t even know we have choices to do otherwise.
A lot of women think that because we have the vaginas, that we have the power. And that’s probably true. We just don’t act like it until we’re out in the public or in certain other spaces.
But when it comes to taking care of ourselves and putting ourselves first, you know, it sort of runs counterintuitive when you’re sitting on the airplane— and I can imagine all the mothers that go through this few seconds of stress when they’re told, you know, that you have to mask yourself before you mask someone else— we are not socialized to think that way.
We are not wired to take care of ourselves first because socially, culturally, economically, even politically, we are more wired to take care of someone else than we are ourselves.
ORRIS: I wasn’t concerned with HIV. I thought I could trust him enough to share with me, but I was wrong and I made that choice.
You think, “Here I am, I’m a clean woman and I’m selective with the men I date. It’s not going to happen to me.” And you think like that, but it did. Here I am and it happened.
NARRATOR: Orris has been dealing with the reality of HIV for more than 10 years now. It’s not easy. All the drugs have side effects, but she has to take them. During work, her friend Evelyn helps her remember.
ORRIS: Evelyn and the other workers encourage me to take my meds because they know that it’s a lifeline.
NARRATOR: Evelyn understands. She lost her brother to HIV when he stopped taking his meds.
EVELYN: Have you took your medication today?
ORRIS: I got to eat something first.
EVELYN: Well, you need to stop and eat something and then can take your medication because if you don’t take your medicine, you know?
ORRIS: OK, Evelyn, I’m going to take it.
EVELYN: All right. I ain’t fussin’ at you. I’m just reminding you because you said the other day you went all day without taking it, and by time for you to take it, it was time to take your second set.
NARRATOR: A few years ago, Orris had fewer side effects because she was taking the whole combination of drugs in just one pill a day.
ORRIS: Because that one pill had me so— had me feeling good, I’m thinking, “Am I really sick? Do I really have HIV?” So I stopped taking the one pill, like I’m supposed to take. And then I end up on 12!
EVELYN: Wow.
ORRIS: And it’s not small tablets. So what I’m trying to do is, I’ve always tried to fit it in with my meals. And it’s so hard because I’m afraid to eat because of gaining weight.
EVELYN: You rather be fat or dead?
ORRIS: I’d rather be neither. I’d rather be healthy.
EVELYN: I know, but you can lose the weight.
NARRATOR: Orris will take the medicines for the rest of her life.
GREGORIO MILLETT, M.P.H., Office of National AIDS Policy: Things have changed, and they’ve changed for the better, but they’ve also changed for the worse. And for the better is that we have medications that keep people living with HIV alive for much longer. They are less likely to get sick. They are less likely to look sick.
But with that comes an invisibility, and that’s where we are paying the price. People are engaging in behaviors that might place them at risk for contracting HIV. And you certainly see that with the younger population of young black men who have sex with men.
NARRATOR: Last year, nearly two thirds of the new infections in young gay men were black.
ANTHONY: It was tough being 15. Being in high school, like, that’s already hard enough, you know, then, like, being gay in high school, and then being openly gay in high school. And then it was around the same time I came out to my family,
NARRATOR: Telling his family did not go as Anthony’d hoped.
ANTHONY: It was a battle. Of course, growing up with siblings, you get into it and you, like, say mean things to each other. But around the time, once I actually came out, everything— everybody’s favorite thing was to say that I was gay or call me a faggot, or stuff like that.
I remember we had this big linen closet. I would go in the closet and just lock the door and sit in the dark and cry. I really didn’t feel loved at that time, so I guess I told myself that I needed to find it somewhere. And I think it was around that time when I got my first boyfriend.
NARRATOR: His boyfriend, Ronald, didn’t tell him he was HIV-positive. Anthony didn’t think about being at risk.
ANTHONY: When I found out I was positive, I told myself I wasn’t going to let it control my life. I told myself I was not going to let this consume me. And I told myself that I was going to be better than Ronald with this. I was going to inform people of the fact that I’m positive. I was going to give them a choice to choose for themselves, give them the opportunity that Ronald didn’t give me.
NARRATOR: A few months later, he met Jovonte, a football player, whose response surprised him.
JOVONTE: Honestly, it doesn’t bother me. Somebody being positive is not the end of the world. I mean, everybody deserves to be loved. So when I heard he was positive, I’m just, “OK, well, let me talk to Anthony.”
ANTHONY: He came to my house one night after football practice, and we were sitting in my living room and he was telling me that he liked me. And I told him, “Well, there’s something I have to tell you.” And I told him that I was positive.
JOVONTE: And then when he told me, I was, like, “Well, I already knew, and that doesn’t change the way I feel about you.”
ANTHONY: We got an apartment together over in East Oakland. And we had a car and everything, so we basically, I guess, had our dream life, so to speak. We had a puppy. We had our family, I guess.
JOVONTE: Protecting myself when it came to our sexual life, it was a priority. But for me, it wasn’t that big of a priority.
ANTHONY: We used condoms through the course of our relationship. You know, like, he knew I was positive so, you know, we used condoms and everything. But that faded, unfortunately. I kind of hate myself for that, but that kind of faded away.
JOVONTE: A couple of months later, I went to his doctor’s appointment. And I was, like, “Hey, why not get tested?” So I got tested. And when it came back, the way he came into the room already let me know that I was positive. So when he told me— I don’t know what it was. Like, you have a feeling like a ghost walks through you. You just— your whole body gets chills. I mean, you can think of it as a type of poison inside of you that slowly kills you.
ANTHONY: We was young and stupid. And you know, he’s dealing with the consequences from it.
GREGORIO MILLETT: Young black gay men between the ages of 18 and 29 are among the highest rates of the epidemic in the nation. There’s an increase of 50 percent of new infections between 2006 and 2009.
NARRATOR: In the battle against AIDS there have been successes — far fewer cases among injection drug users — and today mother-to-child transmission is almost unknown.
But the epidemic in America is unique in the world. For the past decade, the number of new cases in other countries has gone down. Here it’s stayed the same.
GREGORIO MILLETT: We’ve been running in place in many ways. We’re kind of in a period where it’s stagnant. We had spent 30 years with a completely uncoordinated response for HIV. Even though we were requiring other countries that we were funding to have a national HIV/AIDS strategy, the U.S. never had a national HIV/AIDS strategy ourselves.
NARRATOR: Until now. In 2010, the White House rolled out a national AIDS strategy based in part on lessons from the PEPFAR programs the U.S. funded in other countries. It includes a focus on the 12 hardest-hit cities, among them the nation’s capital.
ROBERT FULLILOVE: Washington, D.C. is a Southern city that has a majority black population largely because that’s where the slaves owned by many members of Congress were going to be housed, and where the servants of many of the Northern members of the Congress were also going to be housed, as well.
Fast-forward to the present day, and suddenly, you’ve got a city which is predominantly black, that has one of the most ferocious AIDS epidemics— not just anywhere in this country, it’s anywhere in the world. Five to eight percent of the adult population is thought to be infected.
NARRATOR: Last year in Washington, D.C., the prevalence of HIV was higher than in Rwanda, Kenya, Burundi, Ethiopia and the Congo.
PHILL WILSON: When you look at the AIDS epidemic in black America and you think about black America as if it were a country unto itself, it would have the 16th worst AIDS epidemic in the world. If black America were a country unto itself, it would be eligible for PEPFAR dollars.
That is the type of response that we need if we’re going to be serious about ending the AIDS epidemic in black America.
NARRATOR: Dr. Lisa Fitzpatrick directed the PEPFAR program in the Caribbean, but the emergency in D.C. drew her back home.
Dr. LISA FITZPATRICK: One of the most surprising findings when I first got here was how close in proximity the Capitol building, even the White House, are to Ward 8, which is the section of Washington, D.C., that has the highest rates of unemployment, illiteracy, poverty and health disparities. They’re not even three miles apart.
Good morning. I’m Dr. Lisa from Howard. Can I talk to you for a few minutes about HIV?
I love to talk to the community. It gives you so much information.
So do you guys know how HIV is transmitted?
1st WOMAN:From sex partners.
Dr. LISA FITZPATRICK: That’s it?
1st WOMAN:Blood, semen.
2nd WOMAN:Open wounds.
Dr. LISA FITZPATRICK: You’re right. It’s pretty much bodily fluids.
We need to understand what the community is thinking and how they’re perceiving us, so that we can ensure that the decisions we make and the strategies we want to implement make sense.
Are people aware that treatment is available for HIV, and that actually nobody has to get AIDS?
3rd WOMAN:A lot of people don’t know that. It’s for gays, to slow it down.
Dr. LISA FITZPATRICK: What’s for gays?
3rd WOMAN:The medicine that they have now for HIV.
Dr. LISA FITZPATRICK: Have you heard that the treatment is only for gay people?
3rd WOMAN:Yeah, I read it in a book.
Dr. LISA FITZPATRICK: I would completely understand why people would not present for treatment, if this is the perception.
It’s not just for gay people.
One of the questions that I asked almost everybody was, “Do you think we’ll ever end the epidemic?” And almost unanimously, everyone said “No.”
So do you all think we’ll ever end the HIV epidemic?
MAN: I believe that they already have a cure for it, but they’re trying to stretch the dollar bill out of it as long as they can.
Dr. LISA FITZPATRICK: Oh, wow! OK.
YOUNG MAN: They need the Magic Johnson pills.
Dr. LISA FITZPATRICK: What are Magic Johnson pills?
YOUNG MAN: Magic Johnson, whatever he’s getting, that’s what these people out here need.
Dr. LISA FITZPATRICK: But I actually disagree with that. Ending the epidemic is entirely within our power.
4th WOMAN:People should just— you know, people should use condoms.
5th WOMAN:Have safe sex. Stop jumping from partner to partner.
YOUNG MAN: Strap up, man! Strap up! That’s all I can say, man.
Dr. LISA FITZPATRICK: But you know a lot of people won’t strap up.
You think people are not educated about HIV?
MAN: They know.
Dr. LISA FITZPATRICK: They do know, don’t they.
MAN: Yes. Yes.
Dr. LISA FITZPATRICK: People know. They have the information. They know what they do.
MAN: But they still go and have sex unprotected.
Dr. LISA FITZPATRICK: The challenge I see is that we have to have courage to do the things that we need to do that are difficult.
There’s a patient, she’s 22 years old, she’s HIV-positive. She’s known she’s HIV-positive for years. But she’s completely out of control. She has multiple sexual partners. She is a complete mystery to me.
Dr. LISA FITZPATRICK: You haven’t told your mother?
PATIENT: No.
Dr. LISA FITZPATRICK: You haven’t told your siblings. Have you told your boyfriend?
PATIENT: No.
Dr. LISA FITZPATRICK: I’m often at a loss for how to respond to her. So I listen and I ask questions.
Why? Why don’t you want people to know?
PATIENT: Because I just don’t want people to know my situation.
Dr. LISA FITZPATRICK: Why?
PATIENT: People laugh at me, or whatever the case may be. I just don’t want nobody in my business.
Dr. LISA FITZPATRICK: I think it’s important to have patients like her because it helps us realize that we don’t have all the answers, number one. But also, their realities are so different.
We want them to come to the clinics and we want them to take their medications, make sure they’re virally suppressed. But she’s often telling me as a doctor, she says, “I know you’re a doctor, but you don’t really know what the deal is, so let me tell you what the deal is.”
So when you have sexual partners, do you use condoms? Sometimes? Never?
PATIENT: Yes. Yes. When I do have a sexual partner.
Dr. LISA FITZPATRICK: But you don’t tell them?
PATIENT: Right.
Dr. LISA FITZPATRICK: Because you’re— what would happen, do you think, if you tell them?
PATIENT: I’ll get killed.
Dr. LISA FITZPATRICK: You think you’ll get killed?
PATIENT: Look, if I tell them, they would shoot me. Even before we even had sex. They would shoot me on the bed. That’s what’s going to happen.
Dr. LISA FITZPATRICK: People are struggling with so many other social pressures and social issues that HIV is often the last thing that they’re worried about.
Young people are worried about survival on the street. Are they going to be shot? Or are they going to be caught up in some sort of altercation? They’re not really worried about HIV.
Older people, maybe they’re worried about housing. Maybe they’re trying to keep their lights on. They’re trying to keep their children fed. And we want them to worry about HIV.
So until we also figure out and have the courage to address some of these structural issues in society that are creating these competing demands for people, we will have a very difficult time getting them to focus on HIV.
PHILL WILSON: I pray that we will choose to act. I think there are a few things that we have to do in black America to bring about the end of the AIDS epidemic. Some of them are personal, you know, some of them are policy-level, some of them community-level.
We’ve been at this for 30 years. We are at a different point in the evolution of the epidemic. And we need to be talking about end game.
MARSHA MARTIN: We have achieved some things as a group of black people in America because the Civil Rights movement got us to some places. And at the same time, we see what we haven’t been able to accomplish because HIV is in it everywhere. HIV is this unbelievable little string that is wrapping itself around all the places that we have missed. And it’s saying, “Look over here, look over here, look over here, look over here.”
Bishop YVETTE FLUNDERS:[World AIDS Day concert] When folks get together and bring a message of hope in the age of HIV, I remember very well the brothers and sisters who were the first people who fell to this virus. They’re in the balcony, the unseen balcony. Mark Hobbs and Orville Floyd, William Bond. I want to remember those brothers and sisters who have passed on. There are many in my spirit. Maybe you want to stand and call a name into this atmosphere.
AUDIENCE MEMBER: Kevin Osborn—
AUDIENCE MEMBER: Ron Pirmus—
AUDIENCE MEMBER: Wilton Kesafricar—
AUDIENCE MEMBER: Sammy Winslet—
AUDIENCE MEMBER: Teddy Withers—
Bishop YVETTE FLUNDERS:Call the names!
AUDIENCE MEMBER: Vance Tucker—
AUDIENCE MEMBER: Eric Kane—
AUDIENCE MEMBER: Belynda Dunn—
AUDIENCE MEMBER: Edwin Newsome—
AUDIENCE MEMBER: Leon Brooks—
AUDIENCE MEMBER: Darnell Reams—
AUDIENCE MEMBER: Dewite Sheeley—
AUDIENCE MEMBER: Carolyn Winslet—
AUDIENCE MEMBER: Joy Hanes—
Bishop YVETTE FLUNDERS:Call the names until everybody’s standing.
AUDIENCE MEMBER: Sylvester—
AUDIENCE MEMBER: Kevin Swan—
AUDIENCE MEMBER: Leslie Fitts—
AUDIENCE MEMBER: Melvin Williams—
ENDGAME: AIDS IN BLACK AMERICA July 10, 2012
WRITTEN, PRODUCED AND DIRECTED BY Renata Simone
EDITED BY Brian Funck
CO-PRODUCER Sarah Anthony
CINEMATOGRAPHY Daniel Meyers Jason Longo
NARRATED BY Renata Simone
ORIGINAL MUSIC BY John E. Low
ASSOCIATE PRODUCER Karinna Sjo-Gaber
ADDITIONAL CAMERA Andres Cediel Stephen McCarthy Thierry Humeau Hinde Garrison Vincent Wrenn
POLE CAMERA Amos Clarke Todd Horrisberger
SOUND Francis X. Coakley Travis Groves Andrew Twite Tony Wachter Matt Warthen Sam Watson
ADDITIONAL MUSIC “LA CAGASTE”, “HELICOPTER”, and “THE WEST END” Words and Music by Cliff Robert Martinez (c) SONGS OF UNIVERSAL, INC. ON BEHALF OF BLEEKER SONGS (BMI) and FOCUS Films
PRODUCTION CONSULTANT William Cran
DEVELOPMENT CONSULTANT Linda Villarosa
PRODUCTION ASSISTANTS Kim Costantino Layla Crater
FIELD ASSISTANTS Nana Kofi Nti Alvin McElveen
ONLINE EDITOR/COLORIST Jim Ferguson
SOUND MIX Jim Sullivan
ASSISTANT EDITORS Arnie Harchik Maureen Barillaro
SPECIAL THANKS Terry M. McGovern Diana Echevarria David Ho, MD Song.Studio – a Program of Next Step The SPARK Center of Boston Medical Center
ARCHIVAL MATERIALS ABCNEWS VideoSource AP Photo/Bill Hudson AP Photo/Werner Slocum AP Photo/Kathy Willens Jesse Brooks Marvelyn Brown Birmingham, Ala. Public Library, Department of Archives and Manuscripts Jean Carlomusto Corbis Tom Cosgrove Myrtis Nell Davis Michel du Cille Michael Emery Fantasy Archives Tony Fischer Photography Lisa Fitzpatrick, MD Brian Funck Jovonté Haynes AleXander Hirka Eric N. Hong, Courtesy of Alvin Ailey Dance Foundation, Inc. Billy Howard – Epitaphs for the Living Marilyn Humphries Aaron J. Kansas State University Division of Communications and Marketing Manuscripts and Archives Division, The New York Public Library National Archives at Atlanta NBA Entertainment James Nachtwey NBC Universal Archives Shawn Nee Pablo Perez Steve Schapiro Kelly Sheehy Michael Siebielec Ellen Spiro The Birmingham News Keith Thompson Robert Turner Nuri Vallbona / Miami Herald Paul Volberding, MD Dan Weiner: Copyright John Broderick WGBH Media Library Anthony Whittley
EXECUTIVE PRODUCER FOR NBPC Jacquie Jones
FOR FRONTLINE
DIRECTOR OF BROADCAST Tim Mangini
ASSOCIATE DIRECTOR OF BROADCAST Chris Fournelle
ON-AIR PROMOTION PRODUCER Missy Frederick
ON-AIR PROMOTION EDITOR John MacGibbon
POST PRODUCTION EDITORS Michael H. Amundson Jim Ferguson Mark Dugas Shady Hartshorne
ASSISTANT EDITOR Eric P. Gulliver
POST PRODUCTION COORDINATOR Megan McGough
SERIES MUSIC Mason Daring Martin Brody
DIRECTOR OF AUDIENCE DEVELOPMENT Pamela Johnston
SENIOR PUBLICIST Diane Buxton
PUBLICIST Diane Hebert-Farrell
ONLINE ENGAGEMENT COORDINATOR Nathan Tobey
INTERNS Caitlin Birch Kyna Doles Rachel Gordon Marilyn He Jared Pelletier Mindy Yuen
SECRETARY Christopher Kelleher
EDITORIAL SECRETARY Katie Lannigan
COMPLIANCE MANAGER Talya Feldman
CONTENT MANAGER Lisa Palone
LEGAL Eric Brass Jay Fialkov Janice Flood Scott Kardel
CONTRACTS MANAGERS Lisa Sullivan Emily McNamara
UNIT MANAGER Varonica Frye
BUSINESS MANAGER Tobee Phipps
DIGITAL RESEARCH ASSISTANT Jason Breslow
ASSOCIATE PRODUCERS FOR DIGITAL Gretchen Gavett Azmat Khan
PODCAST PRODUCER/REPORTER Arun Rath
DIGITAL TECHNOLOGIST Bill Rockwood
DIGITAL REPORTER Sarah Childress
SENIOR DIGITAL PRODUCER Sarah Moughty
WEBSITE DESIGN AND TECHNOLOGY Entropy Media, LLC
DIRECTOR OF NEW MEDIA & TECHNOLOGY Sam Bailey
DEPUTY STORY EDITOR Carla Borras
COORDINATING PRODUCER Robin Parmelee
SENIOR EDITORIAL CONSULTANT Louis Wiley Jr.
EXECUTIVE PRODUCER SPECIAL PROJECTS Michael Sullivan
DIRECTOR OF DIGITAL MEDIA/SENIOR EDITOR Andrew Golis
MANAGING EDITOR Philip Bennett
SERIES MANAGER Jim Bracciale
SERIES SENIOR PRODUCER Raney Aronson-Rath
EXECUTIVE PRODUCER David Fanning
A Renata Simone Production, Inc. Film for WGBH/FRONTLINE in association with the National Black Programming Consortium (NBPC)
©2012
WGBH EDUCATIONAL FOUNDATION
ALL RIGHTS RESERVED
FRONTLINE is a production of WGBH/Boston, which is solely responsible for its content.
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation, as part of the Plum Bush Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.



















