Infants of mothers who were infected with the Zika virus in 2016 were 20 times more likely to be born with birth defects than those born just a few years before the epidemic.
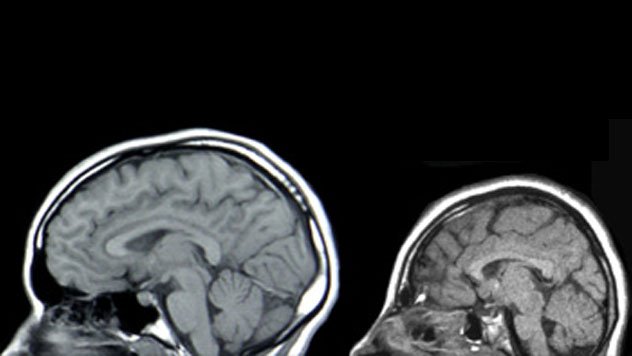
The rate of severe birth defects for healthy mothers in 2013 and 2014 was just three out of 1,000 live births. The most common defects were brain abnormalities and microcephaly—a condition where an infant’s head is significantly smaller than those of babies of the same sex and age.
But among the 442 women likely infected with Zika, 26 fetuses and infants had similar defects—a rate of about 60 out of 1,000. This included live births, miscarriages, and abortions.
The finding comes from the Center for Disease Control and Prevention’s (CDC) Zika Pregnancy Registry—which was created after the outbreak to track infected, pregnant women—and the results were published in the agency’s Morbidity and Mortality Weekly Report. To compare the birth outcomes of women infected with Zika, the CDC compared them birth defects recorded in in Massachusetts, North Carolina, and Georgia.
But even that significantly higher rate may be underestimating the number of potential cases. Here’s Jessica Glenza, reporting for The Guardian:
Experts have warned that infection rates could be much higher than publicly acknowledged. When Zika was first found in the US, testing for the virus was difficult and time-consuming, and no region was undertaking pre-emptive surveillance.
“We know there are at least 300-plus documented cases in south Florida and south Texas, but again because we did not do active surveillance for Zika virus infection on the Gulf coast Texas or Florida where Aedes aegypti mosquitoes are, we still don’t know what the consequences of the 2016 epidemic were,” said Hotez.
“We’ll have to wait and see if babies are born with severe neurologic defects starting around May or June, because it’s a delayed epidemic. There’s a lag.”
Though the method of comparing the outcomes of Zika-affected pregnancies to data from three state registries isn’t ideal, the results offer insight into the considerable risk the Zika virus poses. The study emphasizes the need to keep birth defects registries and continue population-based surveillance to interpret data about Zika-affected defects.
Further limitations of the study include the fact that not every American woman infected with Zika was followed in the pregnancy registry, and some of those who contracted the virus while traveling never developed physical symptoms. A number tests were also inaccurately administered and had to be redone.
The CDC continues to discourage pregnant women from traveling to Zika-affected areas, reiterating the danger of Zika infection during pregnancy.


