Dilemmas of Wartime Medicine
In this guest article, Dr. Dave Lounsbury, a physician and colonel in the U.S. Army Medical Corps, delves into the complex ethics of medical care in combat situations. With their allegiance to both the Hippocratic Oath and military guidelines sometimes in conflict, how do combat doctors decide whom to treat?
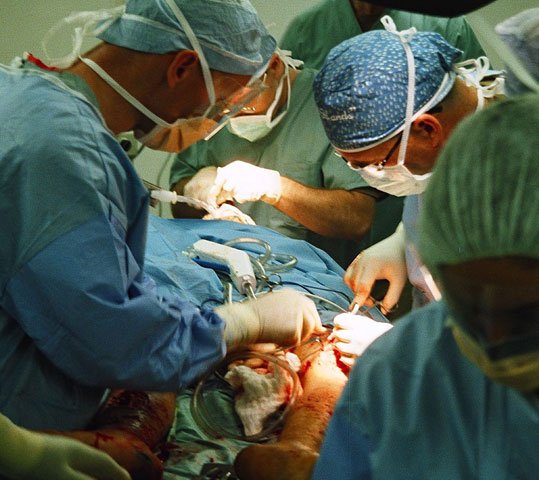
The ethics behind whom American combat doctors should treat in a war zone is complicated. At its most challenging, it can leave physicians like myself and other military medical personnel feeling they're serving two masters: Hippocrates and Uncle Sam. The one calls for treating whomever needs our help; the other, through the agency of the armed forces, has restrictions on whom we can and cannot take under our care. In the end, I believe the battlefield doctor has a duty to a third master: him- or herself. For in the complex circumstances of a combat zone, decisions of how best to resolve this dichotomy between care-for-all and care-for-some should ultimately rest with each doctor.
In my 20-plus years as a doctor in the military, I have served field units in the first Gulf War, the Balkans, and Turkey, and in February 2003 I deployed to the Gulf with the 10th Combat Support Hospital (CSH). It was during and after this deployment that the true intricacies of combat medical ethics really came home to me.
Rules of engagement
As could have been the case with my own career, few military nurses, and fewer physicians, ever deploy to a combat environment. The vast majority of my colleagues serve either an obligation of a few years or sometimes an entire career safe at home in comfortable, state-of-the-art medical facilities. Some have not ventured from the medical centers in which they trained. Instead they provide care to stateside active-duty soldiers, sailors, airmen, and marines and their dependents. Foremost among their patients are retired servicemen and their spouses. Very few expect ever to stand at the gates of a CSH or MASH (Mobile Army Surgical Hospital) determining who is or is not eligible for care. Nor should they.
Some do, however, and they quickly come to understand the inherent difficulties. Iraq, for instance, is a nation of 25 million. It has never been a consideration that mobile U.S. military medical units would or could provide sufficient personnel, equipment, or facilities to care for Iraqis in lieu of their own, albeit hobbled, civil medical establishment. Rather, CSHs necessarily prioritize care to American and coalition forces first. In accord with Geneva Convention protocols, we understand and accept that we must attend Iraqi Enemy Prisoners of War as well. Lastly, we provide care to Iraqi civilians, giving priority to those injured by Allied fire over those presenting with acute or chronic medical problems not related to Allied action.
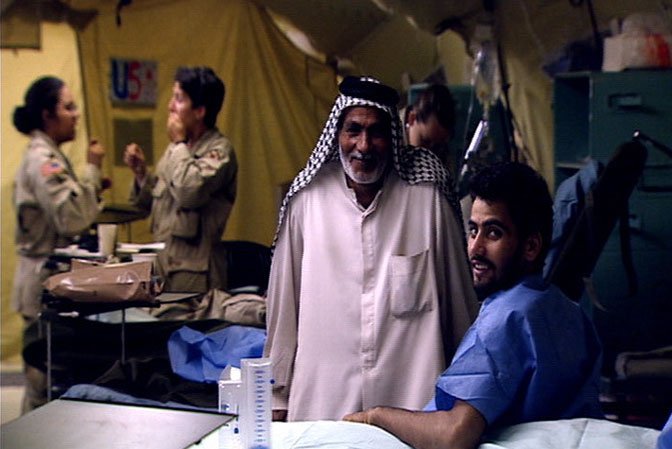
Overriding these levels of priority is an understanding that any individual—friend or foe, civilian or military—who is at risk of losing life, limb, or eyesight will receive emergency care as best we can supply it.
Alas, "best" in a war zone is a lot different than "best" in the States. When I was in the Gulf last spring, our resources were meager, our supplies finite. Our grasp of future events and future demands was as uncertain and muddled as everyone else's. But we were physicians—medical officers who took the same Hippocratic oath as all our civilian colleagues. In the early days after their deployment to Iraq, American medics were relieved of the mission they feared—wards full of American wounded—but they suddenly faced long lines of Iraqi sick and injured. Some were recently wounded. Some had injuries sustained in the Iran-Iraq war of the 1980s. Some had chronic medical illnesses such as diabetes, kidney failure, or heart disease. And some were civilians who had sustained injuries from burns and accidents occurring at home.
"Mixed agency"
American combat doctors could not care for all of them, and in many cases this was not for lack of willingness. The reason is that these doctors' responsibilities to their patients—any patient in need of care—compete with their responsibility to husband resources so as to be able to care for the American serviceman. Military ethicists refer to this tug of allegiance as "mixed agency." I've heard that one of the physicians featured in the NOVA film declined to accept the role of gatekeeper at the 21st CSH, saying in effect that "if I go out I will accept whatever patient is there." This is the moral imperative of the physician trumping the military imperative.
Some would argue—naívely and wrongly in my opinion—that military medicine is an oxymoron.
The dilemma is a profound one, one that ethicists have wrestled with but not agreed upon. The United States, though a signatory to the larger Geneva Accords of 1949, balked at signing additional protocols in 1977 that would have obligated it to provide all medical support as necessary to an occupied state. Recognizing that it was not equipped to assume what could easily become an open-ended and monumental undertaking, the U.S. did not sign these protocols. Military physicians were therefore not legally bound to accept any and all cases outside of the priorities described above.
In fact, deployed medical units were by and large free to determine for themselves whom they would accept for treatment and how they would deliver care, always with the expectation that they would remain mission-capable and ready to care for American wounded. In the current conflict, I am not aware of anyone in Medical Command going further to define how any one unit is to accept or deny care to Iraqis.
Degrees of care
For admitted patients, CSH doctors expend every effort to provide the same in-house care to Iraqis as to Americans, though after leaving the CSH prospects for Americans and for Iraqis are radically different. Once stabilized by emergency resuscitation and surgery, Americans are air-evacuated out of Iraq to medical centers in the U.S. via our large, fully equipped medical facility in Germany. Iraqis remain in Iraq, dependent for a short time on the best Americans can provide and then upon the limited resources of the surviving civilian medical infrastructure. Neither of these systems can provide long-term intensive burn care or complex subspecialty surgical intervention and intensive care. Lives are lost as a result.
Doesn't the CSH doctor have a moral obligation to consider? Is not the military physician and surgeon as obligated as his or her civilian counterpart to provide care to all those who seek comfort? American military medical commanders are largely free to set their own standards and parcel care as they deem prudent. When I was stationed in the Gulf last year, once the issue of a shifting role for U.S. medical assets became clear, I had a conversation with Col. John Powell, commander of the 10th CSH, on how we would set priorities. Powell was adamant that if need be, the 10th CSH's role would be largely a humanitarian one. This happened with the 28th CSH, which assumed a major role in humanitarian relief, providing orthopedic, surgical, and medical care to hundreds of Iraqis.
To thine own self
There are solutions to the dilemmas posed by mixed agency. The physician's responsibility to treat all who present to him can be codified. That is, the U.S. could decide to become a signatory to the 1977 Geneva Protocols (I and II), thus obligating itself to provide this care.
Alternatively, some would argue—naívely and wrongly in my opinion—that military medicine is an oxymoron. They would claim that no physician can ever don a military uniform and willingly claim to serve at once both patient and country. Rather than military doctors, these ethicists presumably imagine a civilian corps of volunteers untrained in and unprepared for the vicissitudes of the modern war zone and the unique nature of battlefield trauma.
In the end, combat physicians assume their own responsibility, willingly or not. They must set their own priorities and act accordingly, accepting the outcome of their decisions. This could be satisfaction with selfless service at the (unlikely) cost of judicial action. Or it could be living with personal demons born of care denied and patients turned away.


