More than two decades have passed, but Erika Archer Lewis clearly recalls the fear, uncertainty and struggle required to bring her 42-year-old mother back from the edge of stage 4 breast cancer. Lewis, a senior studying at the University of Texas when her mother was diagnosed, shuttled between Austin and Houston, supporting her through surgery, chemotherapy, radiation and later, reconstructive procedures.
“It was a four-year ordeal,” Lewis recounts, sitting beside her husband one autumn morning in a sandwich shop north of Houston. Her own breast cancer risk didn’t assume center stage until 2013 when, then 42 and a mother herself, she had a series of breast-imaging call backs. Her routine mammogram was abnormal, which led first to an ultrasound, then an MRI, and then a biopsy of several worrisome areas before cancer ultimately was ruled out. “God, it felt like forever,” she says.
Determined to no longer live in a cancer limbo, Lewis got tested later that year for the BRCA gene mutations that can run in families and significantly raise a woman’s risk of developing breast or ovarian cancer. When the results came back positive, she acted quickly. In early 2014, a surgeon removed both of her breasts. Lewis recovered with the help of her husband, Jerry, and her mother, who recently celebrated 23 years cancer-free.
But a thornier dilemma—whether or not to relinquish her ovaries, too—was just emerging. Doctors typically recommend that BCRA carriers remove them, though doing so causes menopause to commence right away. And with the ovaries’ absence comes hormone imbalance that varies from person to person.
“For me, I feel quite a ways away from menopause,” says Lewis, who has two young daughters. “Although we were pretty confident that we were finished having children, I didn’t want to prematurely be thrown into menopause. I was more afraid of that actually than the double mastectomy.”
But an alternative surgery—an experimental approach—may be on the horizon. A small cadre of doctors are exploring whether or not removing the fallopian tubes (and temporarily sparing the ovaries) will enable women like Lewis to preserve hormone balance a bit longer, and perhaps still provide some buffer against ovarian cancer.
More Options, More Choices
On June 13, 2013, the United States Supreme Court ruled against gene patenting, arguing that isolated genes are a part of nature—not human inventions—and therefore cannot be patented. Since the decision, genetic testing for the BRCA mutation has become more common, and clinicians are meeting with more and more women like Lewis, who have been blindsided in the prime of their reproductive lives by the knowledge that they carry a potentially life-threatening mutation.
Women with BRCA mutations face an ovarian cancer risk of up to 40%, compared to 1.3% in the general population. No reliable screening test has been developed, which means nearly two-thirds of ovarian cancers aren’t caught until they’ve spread beyond the lymph nodes. By then, the five-year survival rate is 27%.
But these women can radically reduce their risk of cancer by removing their breasts and ovaries and, along with them, the tissue and estrogen supply that fuel the vast majority of these malignancies.
Some women, though, refuse to shut down their childbearing options or be thrown into menopause prematurely, says Denise Nebgen, a gynecologist at the MD Anderson Cancer Center in Houston. Nebgen is the principal investigator of a pilot research study led by the Center, one of several research efforts now looking at the alternative fallopian tube surgery. This controversial procedure is based on research that suggests the fallopian tubes may be responsible for between 40 and 70% of the most common form of ovarian cancer.
The hypothesis is a dramatic shift in thinking, says Douglas Levine, MD, a gynecologic oncologist at New York City’s Memorial Sloan Kettering Cancer Center who counts himself among the early skeptics. “For about 30 years, almost everyone thought that ovarian cancer came from the surface of the ovary.”
The MD Anderson study began enrolling patients in late 2013. Their goal is to follow 40 BRCA mutation carriers who will choose one of three paths: screening only, the recommended ovarian removal, or the experimental tube removal followed by ovarian surgery three years later. In France, scientists will be monitoring cancer rates among a small group of BRCA mutation carriers who’ve elected to remove their fallopian tubes. Meanwhile, a coalition of U.S. medical centers is developing a clinical trial to study tube removal in roughly 250 premenopausal BRCA mutation carriers aged 30 to 49.
Depending on how you look at it, these trials could either reduce cancer risk in BCRA mutation carriers who might otherwise avoid ovarian surgery entirely—or throw women onto a third rail of experimental uncertainty.
These women are “guinea pigs” assuming an unknown degree of risk, says Christopher Crum, a pathologist at Brigham and Women’s Hospital in Boston, is considered one of the pioneers in making the connection between the fallopian tubes and ovarian cancer.
Crum worries that he hasn’t been able to trace some advanced malignancies back to the tubes, at least so far. One possibility is that there is another route to ovarian cancer, one that doesn’t involve the tubes. “There could be things happening that we don’t understand,” he says.
“If you have BRCA, and somebody made a mistake [about the tubal connection], you’re not going to see your grandchildren,” he says. “That is to me the issue.”
There are two BRCA genes: BRCA1 and BRCA2. The proteins they encode help repair damaged DNA in cells. Scientists believe that people with mutations in either of these genes are more vulnerable to cancer because the ability to repair errors in cellular DNA is impaired.
Women who carry these mutations face stark choices, as the actress Angelina Jolie highlighted in 2013 when she underwent a double mastectomy after testing positive for BRCA1. Lewis, despite years of trying not to fret about her familial risk, recalls the shock of seeing her own BRCA2 mutation stated in all caps on a letter from the genetic testing company Myriad: “POSITIVE FOR A DELETERIOUS MUTATION”.
Amy Starr, who also lives near Houston, hoped against hope for a negative test result. Sitting in her living room, the 39-year-old surgical nurse pulls a family photo album down from a shelf. She runs her finger along the faces as she names which of her father’s siblings have developed cancers linked to a BRCA mutation.
Beginning with her grandmother’s generation, seven relatives were diagnosed with some form of cancer (primarily breast or ovarian). Four of them died. Most recently, Starr’s aunt Susie passed away in 2011 at age 61 from a type of ovarian cancer, primary peritoneal, after testing positive for BRCA1 nearly a decade before.
“I thought, ‘I’m going to put my mind to rest,’ ” Starr says. “ ‘I’m just going to prove to myself that I don’t have it.’ That was the goal,” she says, with a nervous laugh. “But that didn’t work.” In 2010, she tested positive for BRCA1.
Early Signs
Lewis and Starr are among at least 1,100 women, most of them BRCA mutation carriers, who have visited MD Anderson’s high-risk ovarian screening clinic since 2010. On an autumn morning, the clinicians there meet with a steady stream of patients with turnstile efficiency, reviewing ultrasounds and blood work results, and discussing the significant benefits of ovarian surgery in protecting against cancer.
In one room sits a young woman in her early 30s, her head wrapped in a pink scarf, partway through treatment for breast cancer. In another, a 34-year-old without a history of familial cancer explains that she’d prefer to postpone any surgery to keep her options open. “I’d like to have one or two more kids,” she tells Nebgen.
As testing for these mutations increases, clinicians are encountering more women in their 20s and 30s. While ovary removal is not recommended until at least the mid-30s, Nebgen says, some of these younger women seek counseling earlier on.
“It’s life-changing to have your breasts and your ovaries removed 10 to 15 years before that [menopause] would happen naturally,” says gynecologic oncologist Karen Lu. One frequently voiced fear, she says, is loss of libido.
That possibility haunts Starr. “It’s hard to give up your sexuality,” she says. “Who knows how bad it’s going to be?” These days Starr pursues a vegan diet, a change she made while waiting for her genetic results. The slim mother of two boys, aged 5 and 12, stays active by walking and running.
Although it seems drastic, the current recommendation to remove the ovaries and adjacent fallopian tubes has a good track record. The operation slashes the risk of ovarian, fallopian and peritoneal cancer, according to a recent study that followed nearly 5,800 BRCA mutation carriers from Canada, Europe and the U.S.
And the payoff doesn’t stop there: removing the ovaries also shuts down the estrogen supply that fosters growth of some other cancers, including those of the breast. Women who had the procedure were 77% less likely to die by the age of 70.
But Lewis and Starr, who are both enrolled in the MD Anderson study, are holding out. Though they got their fallopian tubes taken out last year, they’ll be keeping their ovaries for now. But they’re certainly not alone. Just 46% of women with a BRCA mutation but no history of breast or ovarian cancer consented to the ovarian surgery within five years of learning their genetic risk, according to a 2012 study that followed 700 women from England.
Starr says she understands the risks, and emphasizes that the MD Anderson researchers didn’t promise anything specific in terms of the benefits of tube removal. “I didn’t want to have my ovaries out yet,” she says. “But I wanted to feel like I was doing something as far as reducing my risk.”
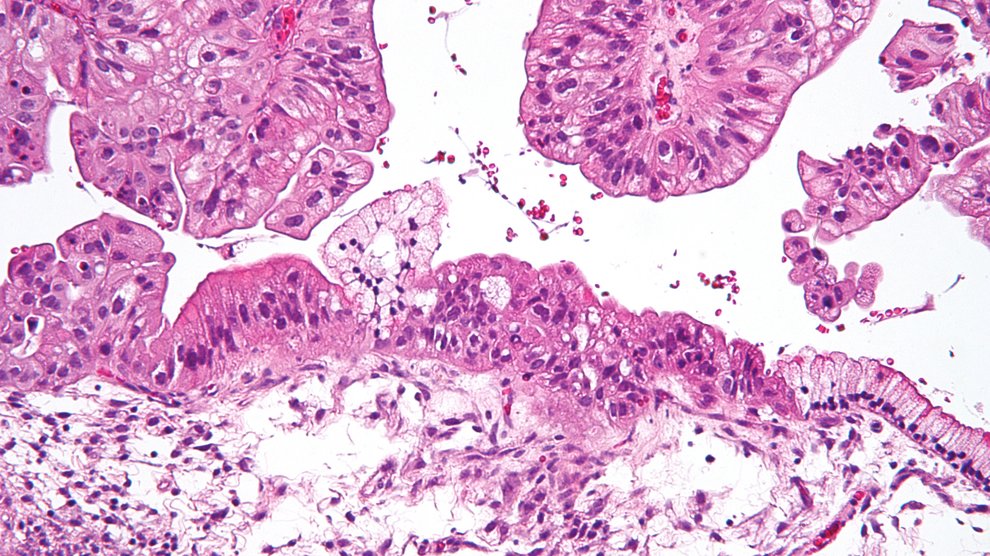
Detecting ovarian cancer early has proved difficult because it seems to emerge full force from nowhere. By the time cancerous signs are spotted from blood work or a vaginal ultrasound, the cancer has more than likely spread beyond the ovaries. So where does ovarian cancer begin?
Until recently, the most common form, high-grade serous carcinoma, was believed to stem from some breakdown related to the egg’s release each month, Lu says. As that egg emerges through the outer skin of the ovary, the minuscule tear has to be repaired.
“When that happens, you have little pockets that form,” she says. “And so the original thinking was that ovarian cancer developed when there was a kind of a pocket of epithelial cells [cells from the outer surface] that got stuck inside the ovary. And then those cells within the ovary became cancerous.”
It was the first waves of ovarian surgeries on BRCA mutation carriers beginning in the late 1990s that provided a front-row seat to cancer’s development. Pathologists then began to stumble across early signs of cancer in the fallopian tubes; several papers published between 2000 and 2004, were the first to postulate that at least some of these high-grade serous cancers originated in the nearby tubes.
The underlying theory, according to Crum, the Boston pathologist, is that if tumours emerged in the tubes, they would be more likely to appear in that fimbriated end nearest the ovaries, as they’re rarely found in the tube’s mid-section. Soon after reading the papers, Crum developed a pivotal dissection technique—dubbed the SEE-FIM protocol (Sectioning and Extensively Examining the FIMbriated end)—that continues to be used today. The technique fillets the fimbriated end of each slender tube into numerous tiny sections, reducing the likelihood of missing a cancer, even if it’s just a fraction of an inch in size, Crum says.
Crum and his colleagues went on to discover cancers in the tubes, typically in the fimbria, without any sign of cancer in the ovaries. Another breakthrough linked pre-malignant cellular changes in the tubes, called precursors, to later malignancies.
Opting for Transparency
As they counsel patients about the new study, clinicians at the MD Anderson clinic must educate women about the tubal research without overstating its potential. “Is that a theory or is that a fact?” one articulate 36-year-old woman keeps asking as clinicians outline the evidence to date. “Is that for sure going to reduce my ovarian cancer risk or not?”
The evidence is “pretty strong,” Nebgen tells the woman. Along with outlining some of the pre-cancerous changes that have been identified during dissections, Nebgen also cites the benefits that women already reap when they get their tubes tied—a procedure technically known as tubal ligation—once they’ve finished having children.
That common procedure, which damages some of the tubal tissue, reduces the rate of later ovarian cancer by 34%, according to a review of studies. Taking the tubes out completely could reduce your risk by at least that much, and hopefully more, Nebgen tells the woman and her husband.
Given the number of women who have routine pelvic surgery, why not just take out the tubes completely during the procedure? A group of Canadian researchers have been pursuing that line of thinking in a large initiative in Vancouver, dating back to 2010, which focuses on women at normal ovarian cancer risk. More than 11,000 women to date have had their fallopian tubes removed during common pelvic surgeries.
Crum says he has no problem with that preventive step, given that those women aren’t genetically vulnerable to breast or ovarian cancer. But the equation is much different for mutation carriers, given their genetic risk and other uncertainties, he says.
For one, studies don’t agree regarding what percentage of these common ovarian malignancies can be linked back to the tubes. Physicians in Canada site data showing that at least 70% of all high-grade serous cancers are seeded in the tubes. But other studies report the figure as low as 19% or as high at 59%.
Why these risky cells migrate beyond the tube remains a mystery. Most women start menstruating in their early teens, MD Anderson’s Lu notes. “It may be that the at-risk cells that are at the end of the fallopian tube drop into the ovary—they are probably getting shed—and they become incorporated into the ovary at a very young age, let’s say in the teens or the 20s,” she says. “So if that happens, removing the fallopian tubes at 30 may be too late.”
Despite the uncertainties, Lu and Nebgen fall into the camp thinking that it’s better to offer BRCA carriers this option if they would otherwise stall on ovarian surgery, perhaps indefinitely.
Steven Narod, a Canadian physician and senior scientist at Toronto’s Women’s College Research Institute, is critical of that stance. He argues that even suggesting the tubes-only option allows at-risk women to equivocate about having their ovaries out.
In his practice, he estimates that 90% of women with a BRCA mutation consent to the traditional surgery. “If they chose not to have it, you can be sure the doctor is not giving them full disclosure of the benefits.”
Starr flares at a recounting of Narod’s comments, calling that attitude paternalistic. She recalls a particularly tone-deaf comment about her ovaries, tossed off by the first gynecologic oncologist she consulted prior to visiting the MD Anderson clinic. “He said something like, I’d be better off when they were in a jar. And that was just a horrendous thought. I had just had a baby the year before. I never went back to him ever again.”
Personalized Paths
Lewis, who thought she’d bought herself some time before having to endure menopause, learned several weeks after her tubal surgery that the window might be closing anyway. Nebgen had called with her pathology results. The tubal dissection had revealed precancerous changes, albeit so early that they had scarcely advanced beyond normal, as Nebgen explained it.
At this point, there’s considerable debate in the medical community regarding what these precancerous changes mean, and to what extent they’ll progress, if at all. So Nebgen took the pathology report to MD Anderson’s multidisciplinary conference, which recommended that Lewis’s best option was, in fact, to get her ovaries removed.
For women like Lewis and Starr, women who live in the shadow of cancer risk, time is not on their side. A BRCA1 carrier aged 40 faces a 20% risk of developing breast cancer and a 6.7% risk of ovarian cancer before she turns 50.
Perhaps most unsettling, Lewis’s experience has illustrated, more than once, how these highly personal decisions are constructed upon the shifting sands of scientific knowledge, where even highly experienced and respected experts do not necessarily agree upon the best path.
After she and her husband have met with Nebgen to talk things over, Lewis seems resigned to ovarian surgery—possibly in late 2015, after her body has fully recovered from the battery of 2014 surgeries. “I certainly didn’t go through a double mastectomy and the fallopian tube removal just to get ovarian cancer,” she says.
Then Lewis was thrown another curveball shortly before the year’s end. Nebgen unexpectedly called while Lewis was out shopping. Her case had been reviewed by another group of experts, who didn’t feel that surgery was necessary so soon. “The irregularities in my cell work were not enough to cause alarm, or to at this time warrant removing my ovaries,” Lewis says.
Yet another group will take a look at her case this spring. This back-and-forth is frustrating for Lewis, but she is relieved that she might be able to push back the surgery for another year or two. She’ll continue to receive ultrasounds, although she acknowledges their limitations. “I’m just not up for going into menopause right now,” she says.
Neither does Lewis regret her decision to choose the experimental tube removal, even if she does end up returning to the operating room sooner than she’d prefer. If the traditional ovarian removal had been the only surgical option, she remains convinced that she would have stuck with screening indeterminately. She would have been given the warning signs that her fallopian tubes revealed—knowledge that will help her make potentially life-changing decisions in the years to come.
Starr, who has seen various risk charts, continues to struggle. As part of the research study, she’s agreed to have her ovaries removed by 2017, the year she turns 42. “I’m supposed to,” she says, her brown eyes steady behind wire-rimmed glasses. “I think I will. I want to live.”
This article was originally published in Mosaic .



