'Suspicious' Cluster of Amnesia Cases Might Be Tied to Opioid Use
In November 2015, Jed Barash knew he had something strange on his hands. He’d encountered a seemingly random cluster of amnesia cases that all demonstrated one eerie similarity.
That month, Barash, a neurologist at Lahey Hospital and Medical Center in Burlington, MA, reported these four peculiar amnesia cases to the Massachusetts Department of Public Health, which then led to the discovery of ten very comparable cases by other medical specialists in the area.
The common theme? Nearly all of the patients had a history of substance abuse.
In total, fourteen patients with early onset amnesia identified during the period of June 2012 to July 2016 displayed complete, bilateral hippocampal ischemia, or a deficiency of blood supply to the short term memory center on both sides of the brain.
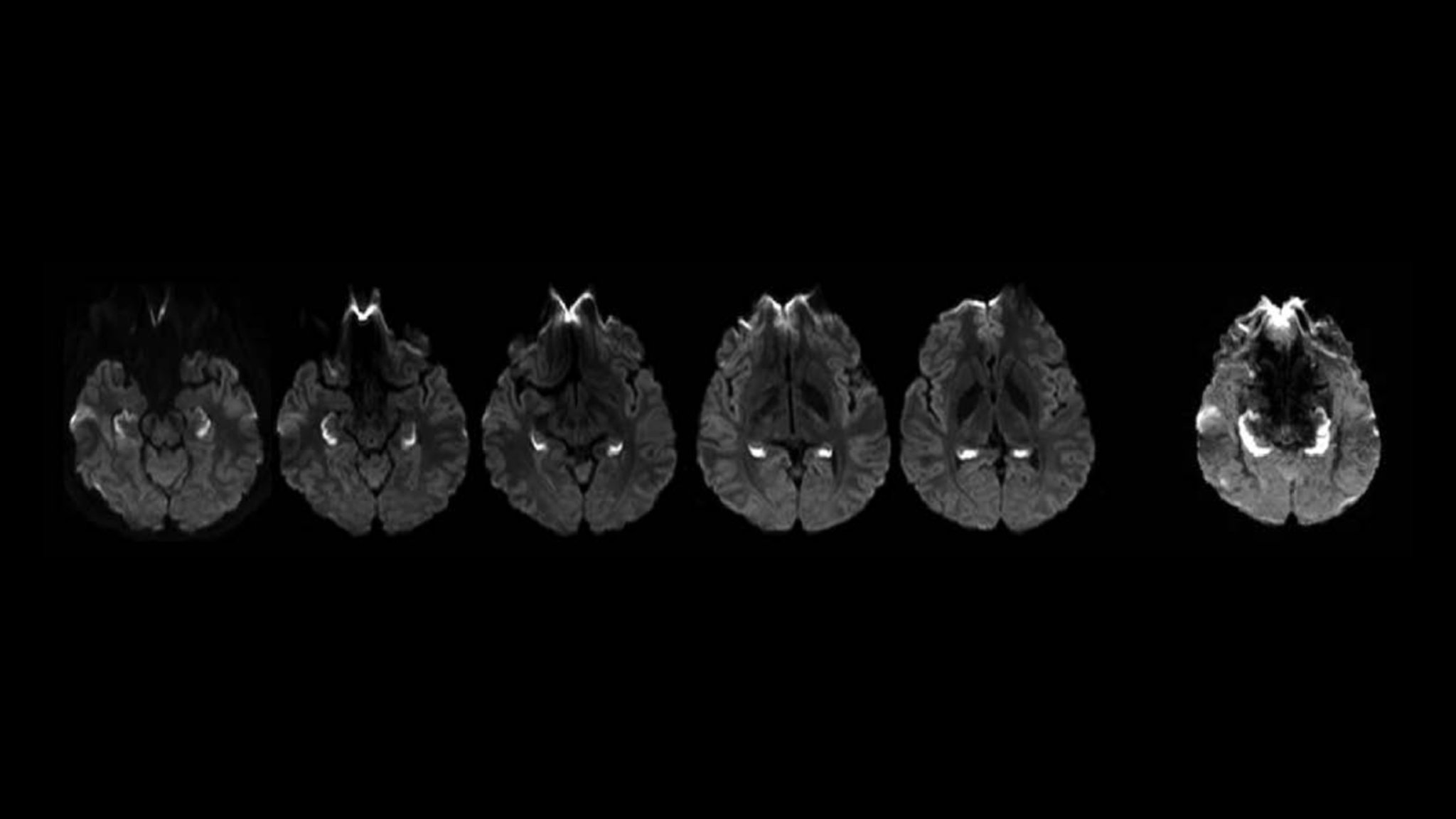
The patients were relatively young, with ages ranging from 19 to 52, with a median age of 35. Of the 14 patients, 13 tested positive for opioids or had a documented history of opioid use. MRI scans revealed that the hippocampus, which is responsible for long-term memory, emotions, and learning, was directly affected.
“These people generally have decent, longer-term recall but they have more trouble with remembering new information that’s presented to them from the time of the event going forward,” Barash said, “They had very profound memory deficits for learning new things.” This type of amnesia is called anterograde amnesia, and is characterized by the inability to create new memories after the event (or series of events that caused the amnesia).
Nine of the 14 patients who were evaluated arrived to the hospital unconscious. After regaining consciousness, all nine patients were found amnestic. Family members, friends, and acquaintances had also observed severe memory loss in the other five patients prior to their hospitalization. Other shared symptoms included deficiencies in attention and executive function. For example, they were unable to recognize family members or retain information about rules to board games.
Thirteen of the 14 patients were documented with a history of substance use disorder. The remaining patient tested positively for unprescribed opiates, cocaine, amphetamines, and benzodiazepines. “Just because we don’t have a history of opioid use documented or on a toxicology screen doesn’t mean necessarily that he never used opioids,” Barash said.
If the culprit is identified, this new mechanism for amnesia could have much broader implications.
In 1982, 42-year-old George Carillo was hospitalized in San Jose having exhibited symptoms identical to those of Parkinson’s disease, a neurodegenerative disorder that attacks a patient’s motor skills. When it was discovered that MPPP (which is used to cook up synthetic heroin) was made by accident instead of MPTP (which is toxic to dopamine-producing neurons), scientists we able to pave the way to significant medical advancement. MPTP has since allowed researchers to develop an animal model of Parkinson’s disease to further examine surgeries to repair damaged areas of the brain and replace damaged stem cells.
It could be that the case of “frozen addicts,” as these patients were called a few decades ago, could be a fitting analogy—Barash’s findings could do for amnesia research what the frozen addicts did for Parkinson’s disease.
“It’s one of those historical instances that raises our concerns that we’re missing something here,” said Dr. Alfred DeMaria, Medical Director of the Bureau of Infectious Disease in the Massachusetts Department of Public Health. “It may teach us something about how the hippocampus operates.”
Dr. Chun Lim, assistant professor of neurology at Harvard University, who cared for and referred two of the patients included in the study, said, “The advantage of creating an animal model is that you can look at the pathways. It can help our understanding of how people get Parkinson’s disease.”
He says there isn’t an isolated disease that targets the hippocampus that results in amnesia or memory difficulties. There are a number of diseases that affect the hippocampus; however, unlike with Alzheimer’s, the neurodegeneration process in these specific cases are acute. “If we identify the causative agent in Dr. Barash’s cases and determine how it selectively affects the hippocampus, it may provide an avenue to treat the memory loss seen in Alzheimer’s.”
“It’s certainly crazy,” said Dr. Elena Chartoff, assistant professor of psychiatry at Harvard University, who was not involved in the study. “What it me made think of is that in people—and in animals, too—all drugs of abuse muck up glutamate homeostasis, and the hippocampus is particularly sensitive to that. So it could be there was too much glutamate in the hippocampus, and that caused the ischemia and the pathology scene in the MRI.”
Chartoff said that her work has suggested that opioids change the variety of protein expression that’s necessary to maintain glutamate balance. But if the hippocampus is weathering a blast of glutamates, that would disrupt hippocampal functioning.
While Chartoff acknowledged that this research could assist in the development of animal models for anterograde amnesia or other memory disorders, she said that it could help treat addiction, as well. Moreover, she noted that 70% of the patients in question were male. “That’s interesting—it could be that women are protected from this, or that men are sensitive to it.”
Still, further observation and investigation is necessary to determine whether or not the rare clustering, relatively young onset age, and lack of known cause can accurately be related back to extensive substance use. “Maybe there’s nothing going on here, which probably would be the best outcome for people,” said DeMaria. “We just think it’s very suspicious that all of a sudden, we’re noting these cases.”
Image credit: Centers for Disease Control and Prevention


