Why is Whooping Cough Back?
Of all immunizations against infectious diseases, the vaccine against whooping cough probably has the most complicated history and the most unpredictable future. Why does whooping cough, also known as pertussis, present such a tough public-health problem?

What is whooping cough?
Bordetella pertussis bacteria cause whooping cough by sticking to the cells lining the lungs and producing a toxin that blocks lung function. The main symptom of pertussis is a gasping cough characterized by a whooping sound that gives the disease its common name. The cough can be intense enough to cause vomiting or break ribs. Although adults and older children usually survive the disease—while enduring considerable discomfort—it can be fatal in infants, the age group with the highest pertussis death rate.
Antibiotics can cure the disease if the infection is identified early enough, but there is no treatment that can neutralize the pertussis toxin once it's present in the lungs. An infected person first shows symptoms of a common cold, including sniffles and a low-grade fever; but once the characteristic cough develops, it can last for weeks. One nickname for pertussis is the "100-day cough."
Pertussis kills about 300,000 people each year worldwide, most of them infants. According to the U.S. Centers for Disease Control and Prevention (CDC), infants under one year old not only are at greatest risk of death from the disease, but they also have the highest reported rate of pertussis. Even in older children, the consequences of the disease can be serious; one in 20 children who contract pertussis has nervous system damage. The disease, which passes from person to person through the air, is highly contagious; one infected person can spread the disease to more than a dozen other people. An infected person is contagious even when symptoms are indistinguishable from those of a cold, before the "whooping" cough begins.
In the United States, pertussis affected more than 200,000 people a year in the late 1930s and early 1940s. The advent of a vaccine against the disease in the 1940s led to a drop in those numbers, to a low point of just over 1,000 cases in 1976. Then, in the 1990s, the numbers started rising again.
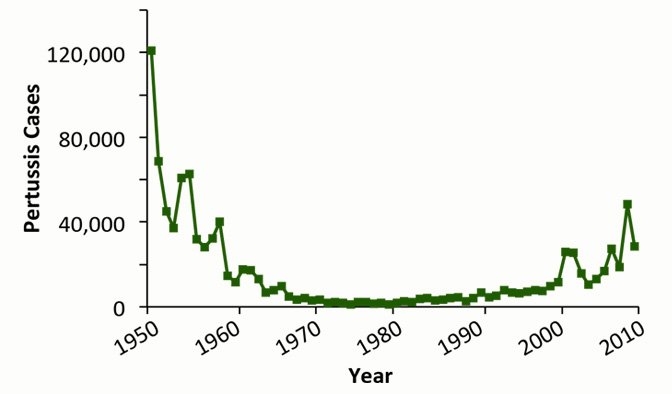
Is there a resurgence of pertussis?
By the first decade of the 21st century, pertussis outbreaks had started to increase in number and size. California has been slammed with two major outbreaks: one in 2010 that hit 9,120 people and left 10 infants dead, and one in 2014 that as of August involved 7,503 cases and three infant deaths.
Whooping cough cases have always waxed and waned in natural cycles, peaking every three to five years. Since the 1990s, though, the number of cases has been on a steady climb. Doctors are recognizing the disease earlier and more often, now that it's back on their radars, and testing for it has improved. But these aren't the only reasons for the increase. Another important factor was a change made in 1991 in the kind of pertussis vaccine used in the United States.
How has the pertussis vaccine changed?
The first pertussis vaccine contained inactivated but complete bacterial cells. Typically, vaccines contain bits of the target microbe, which trigger our immune systems to mount a defense against them and—most importantly—remember them in case of future invasion. The whole cells in the old vaccine offered the immune system a huge selection of pertussis-specific targets to recognize and remember.
But then some people became concerned because the vaccine was causing seemingly alarming reactions, including fever-induced seizures and fainting. Even though these reactions didn't cause any lasting damage, the relatively high rate of these reactions (about one in every 1,000 doses of the vaccine resulted in a seizure event) prompted the development and approval of a new version of the pertussis vaccine. Instead of using the whole bacterial cell, it offers the immune system only select bits of the cell that trigger an immune defense. Because it doesn't rely on complete cells, the new version is called an acellular vaccine.
Is the newer pertussis vaccine less long-lasting?
It turns out that the host of molecules in the whole-cell vaccine probably triggered a stronger and longer-lasting immune response than the newer, acellular vaccine does. Those of an age to have received the newer version exhibit shorter-lasting immunity than those who got the whole-cell vaccine. The numbers are clear: With whole-cell vaccination, cases nationwide stayed in the low four digits for decades. With the advent of the acellular version, the number of U.S. cases climbed again, reaching almost 50,000 in 2012. Meanwhile, in countries such as Thailand that continued to use the whole-cell vaccine, case numbers have remained low and have even continued to decline.
As a result of the waning immunity of the acellular vaccine, U.S. preteens now receive an additional inoculation, at age 11 or 12 years. The first five shots, given from infancy through age four to six years, are in a formulation known as DTaP (for diphtheria, tetanus, and acellular pertussis). The sixth shot, the preteen booster, is referred to as the Tdap—an existing tetanus and diphtheria booster, now with pertussis added in.
Is pertussis a moving target?
The new version of the pertussis vaccine might have had yet another unanticipated effect: opening the door to changes in the bacteria. Some recent samples of the B. pertussis bacterium from infected people contain cells that no longer make the molecules used in the vaccine to trigger the immune system. Without these recognizable molecules, the altered bacteria can slip right past the immune system's defenses. The upshot could be that an already relatively weak vaccine is becoming even weaker.
What is the role of vaccine refusal?
According to the CDC, about 5% of children in the United States have received less than three shots in the DTaP vaccine series. Parental refusal to vaccinate their children against pertussis has been tagged as one factor in the 2010 California outbreak. Regions where more parents requested vaccine exemptions for nonmedical reasons were 2.5 times more likely to also see a high number of pertussis cases.
Protecting a community against pertussis requires that at least 92% of the population be immune. Given the complexities of waning immunity, as well as a weaker pertussis vaccine than was previously used in the United States, maintaining that threshold to achieve "herd immunity" is more critical than ever—especially to protect infants, who are the segment of the population most vulnerable to the disease.



