Transplanting Hope
Witness organ transplants as they unfold, and meet patients awaiting lifesaving donations.
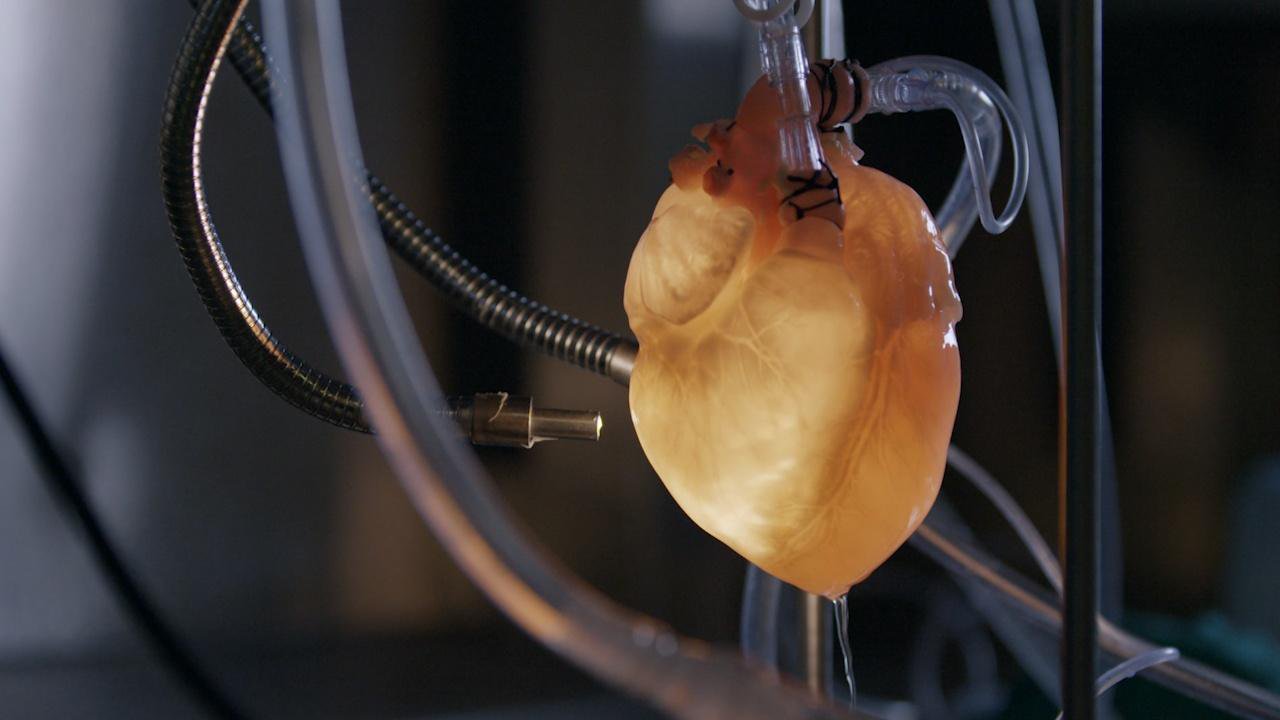
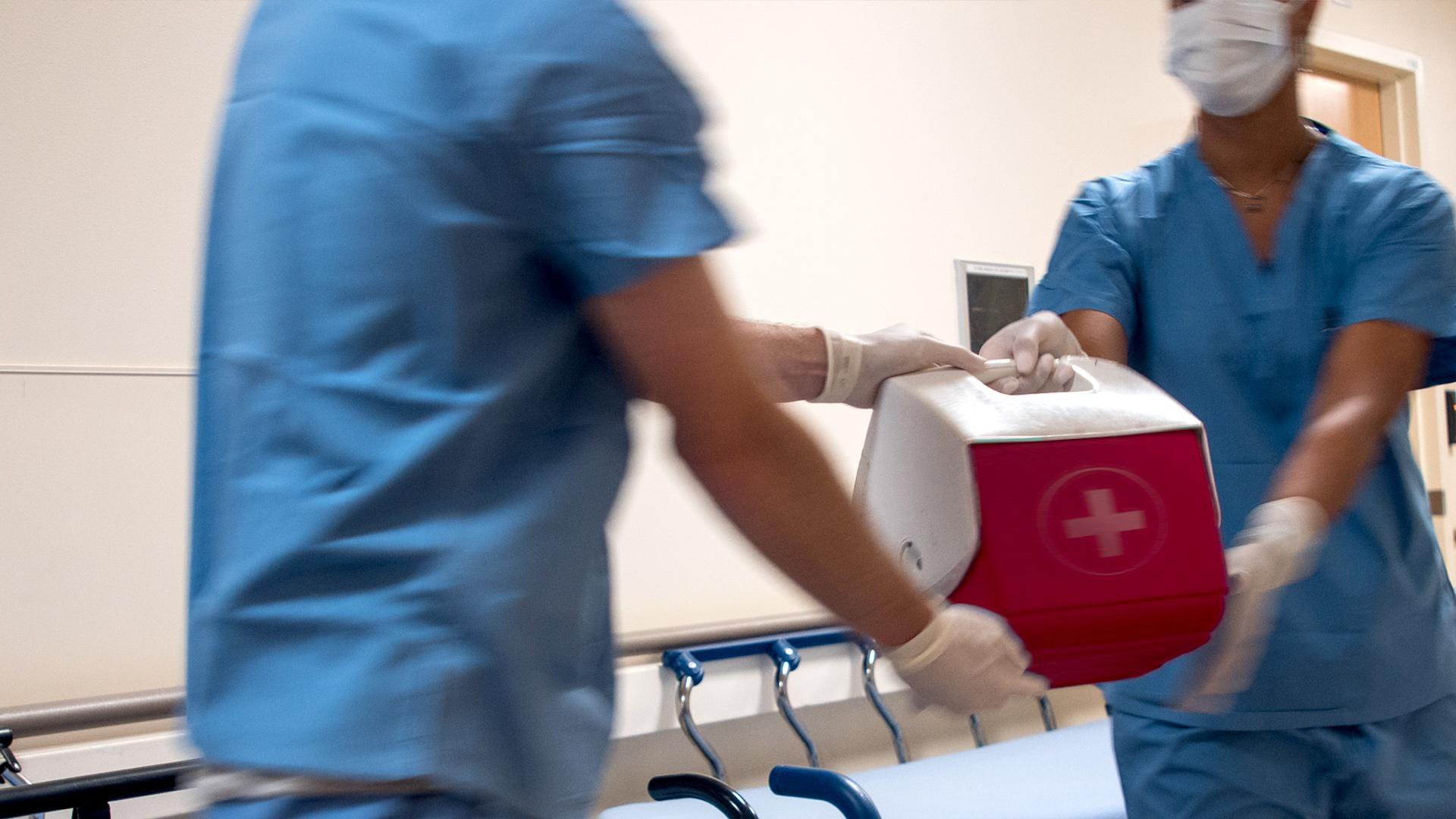
(This program is no longer available for online streaming.) NOVA takes you inside the operating room to witness organ transplant teams transferring organs from donors to recipients. Meet families navigating both sides of a transplant, and researchers working to end the organ shortage. Their efforts to understand organ rejection, discover ways to keep organs alive outside the body, and even grow artificial organs with stem cells, could save countless lives. (Premiered September 26, 2018)