Being Mortal
February 10, 2015
54m
FRONTLINE follows renowned writer and surgeon Atul Gawande as he explores the relationships doctors have with patients who are nearing the end of life
Being Mortal
February 10, 2015
54m
Share
FRONTLINE follows renowned New Yorker writer and Boston surgeon Atul Gawande as he explores the relationships doctors have with patients who are nearing the end of life. In conjunction with Gawande’s new book, Being Mortal, the film investigates the practice of caring for the dying, and shows how doctors — himself included — are often remarkably untrained, ill-suited and uncomfortable talking about chronic illness and death with their patients.
Produced by
Transcript
Credits
Journalistic Standards
Support provided by:
Learn More
Most Watched
The FRONTLINE Newsletter

Facing Mortality: How to Talk to Your Doctor

Dr. Atul Gawande: “Hope is Not a Plan” When Doctors, Patients Talk Death

Love and Cancer at 27
Related Stories
Being Mortal
Inside “Being Mortal” with Atul Gawande and Tom Jennings

Podcast: The Long Tail, the Lottery and “Being Mortal”

Love and Cancer at 27

A Very Short History of Death

“It’s Very Hard to Come to the Realization That You’re Dying”

Prolonging Life or Prolonging Death? Two Doctors on Caring for the Critically Sick

Here’s #WhatMattersMost to You

How Would You Spend Your Last Days? Live Chat 3 p.m. ET on Thursday, 2/12

What Matters Most to You in the End?

Dr. Atul Gawande: “Hope is Not a Plan” When Doctors, Patients Talk Death

Facing Mortality: How to Talk to Your Doctor

“As Real as It Gets”: Inside the Making of “Being Mortal”

A Link Across Generations

Why Is It So Hard for Doctors to Talk to Patients About Death?
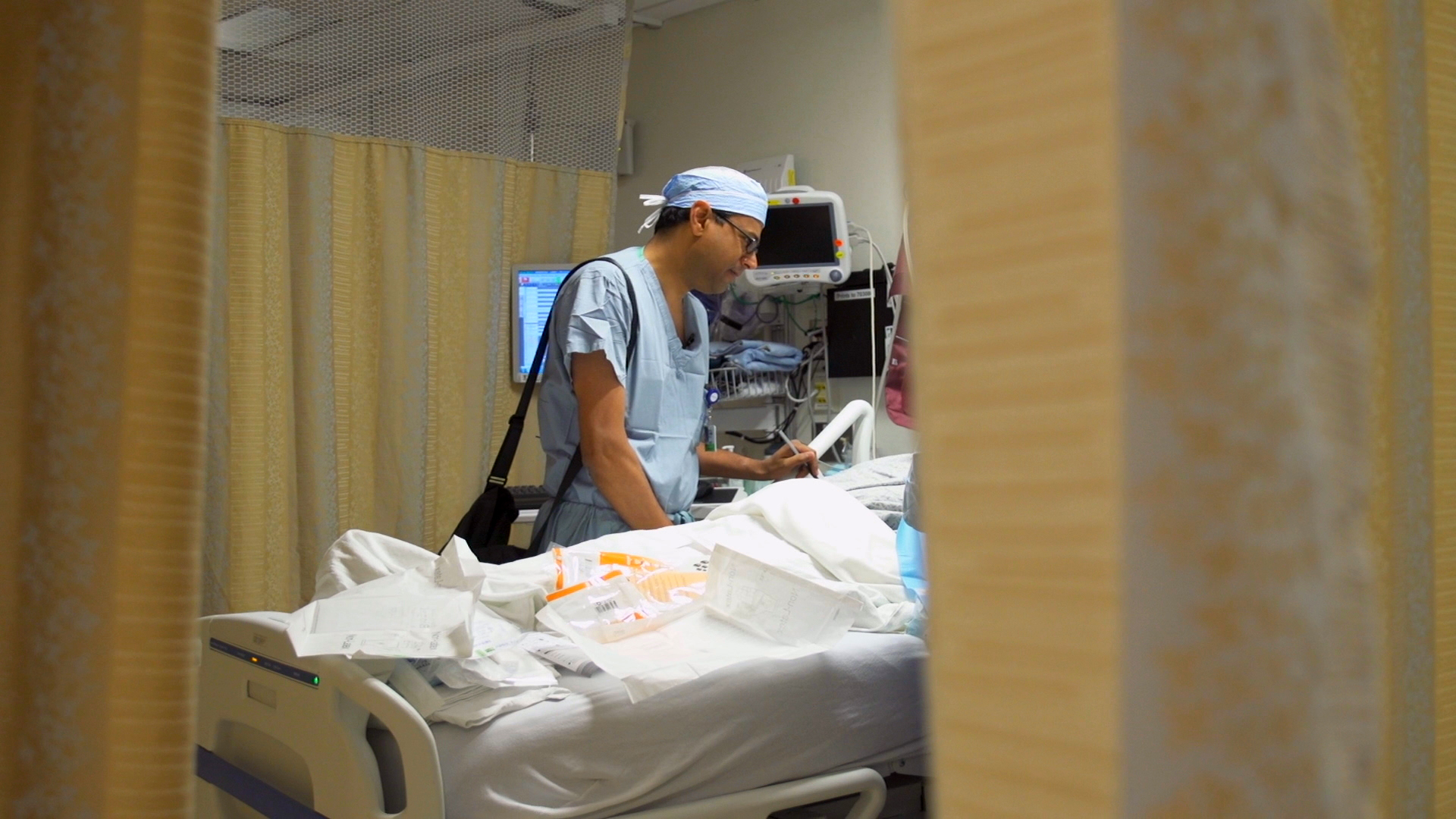
How Should Doctors Help Terminally Ill Patients Prepare for Death?
Related Stories
Being Mortal
Inside “Being Mortal” with Atul Gawande and Tom Jennings

Podcast: The Long Tail, the Lottery and “Being Mortal”

Love and Cancer at 27

A Very Short History of Death

“It’s Very Hard to Come to the Realization That You’re Dying”

Prolonging Life or Prolonging Death? Two Doctors on Caring for the Critically Sick

Here’s #WhatMattersMost to You

How Would You Spend Your Last Days? Live Chat 3 p.m. ET on Thursday, 2/12

What Matters Most to You in the End?

Dr. Atul Gawande: “Hope is Not a Plan” When Doctors, Patients Talk Death

Facing Mortality: How to Talk to Your Doctor

“As Real as It Gets”: Inside the Making of “Being Mortal”

A Link Across Generations

Why Is It So Hard for Doctors to Talk to Patients About Death?

How Should Doctors Help Terminally Ill Patients Prepare for Death?
CORRESPONDENT
Atul Gawande
WRITTEN BY
Thomas Jennings and Atul Gawande
PRODUCED AND DIRECTED By
Thomas Jennings
ATUL GAWANDE, M.D., Author, Being Mortal: I’ve been a surgeon for more than a decade now. In medicine, your first fear as a doctor is that you’re supposed to be able to fix a problem, and our anxieties include wanting to seem competent, and to us, competent means I can fix this. In fact, there’s often a kind of implicit promise, “I’m going to be able to fix this, I’m going to certainly give you the best shot you can have, nobody could have given you a better shot.” And then when things aren’t working, part of your anxiety is, “Was there something I missed? Was there anything else I could have done?
When I started out in my training in surgery, you discover that all the stuff you learned about in the books in medical school is really just a tiny little bit of what it means to be good at doing our jobs. It’s not just about how smart you are anymore as a doctor, it’s about how you have to be able to work with teams and how mistakes get made and how you handle them, and how you learn.
Among the most uncomfortable difficulties was grappling with those cases where we couldn’t solve the problem. The two big unfixables are aging and dying. You know, they’re not— you can’t fix those.
I’m a surgeon and I’m a writer. My writing has become the way that I can focus in and begin to understand the problems that most confuse me. One case in point was a piece I wrote called “Letting Go” about a woman named Sara Monopoli, whom I helped take care of, who was diagnosed with stage 4 lung cancer during the 9th month of her pregnancy at the age of 34.
This was one of the most difficult circumstances. You have a young woman with a brand-new baby. Of course, everybody is fighting for every chance that she’s got. She was young. She’s enthusiastic. She wants to tackle this. You don’t want to be the downer. So you’re looking, you’re grasping for a straw that says, “Well, there’s something here that’s going to be beneficial.”
Stage 4 lung cancer, we know it’s not curable, but suppose she’s the one that somehow gets cured. Maybe she’s the one. And so therefore, we should do all these things to her.
Having any kind of discussion that would begin to say, “Look, you probably only have a few months to live. What do we do to make the best of that time, without giving up on the options that you have?” That was a conversation I wasn’t ready to have. I don’t think any of us were.
Hey, there.
RICH MONOPOLI, Sara’s Husband: Dr. Gawande, how are you?
Dr. ATUL GAWANDE: How are you?
RICH MONOPOLI: Come on in.
Dr. ATUL GAWANDE: Take me back to when she’s pregnant, she’s doing great, 39 weeks, your due date is coming. And?
RICH MONOPOLI: The collapsed lung would not allow for a C-section. It was too dangerous to be opening her up with all that fluid buildup. So Sara had Vivian, basically, pushing with one lung. It was so difficult, but she had the baby.
You want to be part of that 15 percent that survives more than five years. You want to be a part of that group so badly. And you say to yourself, “Why not us,” you know? It wasn’t about, “How can we have good days to the end?” We didn’t focus on that enough. We’re trying to stabilize the situation and try to become a little— spend a little bit of time as a family.
But it— it was just— it was an impossible situation, impossible summer. I mean, it was just excruciating.
Dr. ATUL GAWANDE: When I came on the scene was when she got diagnosed with a second cancer. You know, in my mind, what I was thinking was I wouldn’t offer this surgery because the lung cancer is going to take her life. And yet I didn’t feel I could say that to you all.
I think we started talking about the experimental therapy that you all would like, or were hoping to get on for a trial with the lung cancer. And I remember saying something I sort of regret, which was, you know, maybe that experimental therapy will work for the thyroid cancer, too. [both laugh] I said that, and I know it was complete—
RICH MONOPOLI: Well, you had joined us in our, in our sunny disposition, hoping for the best.
Dr. ATUL GAWANDE: I knew— I knew it was not going to— I mean, I— in other words, the reason I regret it is because I knew it was a complete lie. I just was wanting something positive to say.
RICH MONOPOLI: I did not know it was an outright lie. You could lose your license for this! [both laugh]
Dr. ATUL GAWANDE: I know! But I— you know, I think I— I— I don’t think I was terribly equipped for having that conversation, and maybe you all weren’t.
RICH MONOPOLI: I don’t think we were. I’ve thought often about what did that cost us. What did— what did we miss out on? What did we forego by consistently pursuing treatment after treatment after treatment, which made her sicker and sicker and sicker?
Dr. ATUL GAWANDE: The very last week of her life, she had brain radiation. She was planned for the experimental therapy the following Monday. You woke up, and she wasn’t doing so well— on a Friday. What happened then?
RICH MONOPOLI: So she woke up and was gasping for air. And I tried to crank the oxygen up. I said, “Let’s max this thing out.” Maybe we’d get a bigger oxygen machine. We were so close to getting to the next potential fix. And she said, “I can’t do this. I can’t do it at home. I’m too scared. I’m gasping for air, and I can’t— can’t do this.”
We should have started earlier with the effort to have quality time together. The chemo had made her so weak that she couldn’t hold Vivian. It was exhausting. And that was not— that was not a good outcome for— for the final— final months. It’s not where we wanted to be.
ATUL GAWANDE: [voice-over] In the last three months of her life, almost nothing we’d done — the radiation, the chemotherapy — had likely done anything except make her worse. It may have shortened her life.
[on camera] What was interesting to me was how uncomfortable I was and how unable I was to deal well with her circumstances. It felt like a revelation in that here was a case which I could unpack enough to understand. Why do we always go off the rails?
[voice-over] It made me want to explore what other doctors were doing in these extremely difficult circumstances. What I hoped was that maybe I might learn something that I should be doing differently.
[on camera] I work at the Brigham & Women’s Hospital and Dana Farber Cancer Institute in Boston. They’re connected together across one street.
[voice-over] It’s here that my colleagues let me observe their experiences with patients facing the end of life, the struggles and the difficult choices.
One was Lakshmi Nayak. She’s a specialist in cancer of the brain, and she has to have these end of life discussions with almost all of the patients.
[on camera] You picked a pretty tough field, right? So how many of your patients will you cure or help them have a better life?
LAKSHMI NAYAK, M.D., Neuro-oncologist: It’s almost always fatal. We have— you know, each of us has an odd patient who’s survived for 10 years or 15 years, but that’s less than 5 percent of all of the patients that suffer from the most common malignant brain tumor. So yes, I don’t get to tell people, “I’m going to cure you.”
ATUL GAWANDE: Yeah.
[voice-over] One of Dr. Nayak’s most challenging cases at the time was a man named Bill Brooks. He was 46 years old.
Dr. LAKSHMI NAYAK: Bill has brain cancer. That, basically, in his case, has led to raised pressure in his head. But he feels really well. Bill’s sister had also died of a brain tumor, and that was what he was worried of the most.
MARY BERNARDO BROOKS, Bill’s Wife: How do they look?
BILL BROOKS: They look delicious.
MARY BERNARDO BROOKS: [laughs] They always look delicious. Everything is good for you. You eat anything.
You know, we’re so lucky. We have each other. We have great families. We have great friends. We’ve got great jobs. We live in a beautiful home. We’ve been lucky. And then, you know, all of a sudden, it’s like our world was turned upside down.
BILL BROOKS: It’s a battle. You know, some people say “Don’t listen to the numbers,” and I always say, “Well, that gives me something to shoot for.” You know, if they tell you 5 years, let’s go for 6, 7, or 10.
Dr. LAKSHMI NAYAK: So Bill’s story from the very beginning has been challenging because when I first saw him, I thought he had 5 to 10 years. That changed. His symptoms started getting more aggressive.
Dr. ATUL GAWANDE: The headaches.
Dr. LAKSHMI NAYAK: The headaches, the not being able to lie down. I actually called Mary. I said, “We don’t have much time. We probably have a few days to a month.” And I told her she should take time off work.
MARY BERNARDO BROOKS: He started having pressure in his head. And we— [weeps]
BILL BROOKS: It’s OK. It’s OK.
MARY BERNARDO BROOKS: We just never have enough paper towels! So Dr. Nayak gets very—
BILL BROOKS: She takes it very personal.
MARY BERNARDO BROOKS: She takes it very personally when she wants— has to give us bad news. She basically just told us to get ready. And so, you know, of course, you have your pity party. And then you kind of, like, don’t give up hope!
BILL BROOKS: It’s OK, sweetie.
Dr. ATUL GAWANDE: [voice-over] So after the phone call, Dr. Nayak ordered a series of spinal taps to relieve the pressure in Bill’s brain, and it worked. The pressure came down. He felt better. And they had new hope. But the disease was still progressing.
Dr. LAKSHMI NAYAK: You started to have some pressure? Can I check a few things?
BILL BROOKS: Yes. Absolutely.
Dr. LAKSHMI NAYAK: Like your eyes. Eyes wide open— what I was looking into your eyes was not the way your pupils reacted was— but to see what the pressure might be. And I’m worried that the disease will be growing.
SANDRA RULAND, R.N., Oncology Nurse: I think that it’s important for us, even though it would be easier to sort of skip over this today, that we should talk about, if things are not going as we hoped, to just talk about worst case scenarios a little bit.
Dr. LAKSHMI NAYAK: And then best case scenario, too.
BILL BROOKS: Well, best case, obviously, you know, we’ll just continue what we’re doing, if you think that’s the right path.
Dr. ATUL GAWANDE: [on camera] What made you jump in to say “best case,” as well as worst case?
Dr. LAKSHMI NAYAK: I think that I’d scared them the first time.
Dr. ATUL GAWANDE: You’re thinking back to when you talked about it before.
Dr. LAKSHMI NAYAK: Yeah.
Dr. ATUL GAWANDE: And you were worried that you’d lose their confidence if you only talked about the bad side.
Dr. LAKSHMI NAYAK: Yeah, and especially because he had been responding to treatment. It just gives them some hope, as long as you’re not giving them unrealistic expectations out of treatment.
MARY BERNARDO BROOKS: It’s worth a shot.
BILL BROOKS: What’s the third option?
MARY BERNARDO BROOKS: There’s no third option.
BILL BROOKS: There has to be a third option.
SANDRA RULAND: We do things together. We often are finishing each other’s sentences. If Dr. Nayak had said, “Let’s talk about worst case scenarios,” then I would have said, “and we’ll talk about best case scenarios.”
Have you thought at all, as far as worst case scenarios go, if you would want hospice at home or hospice at a facility or—
BILL BROOKS: Do it at home.
SANDRA RULAND: When we talked about hospice, I was reading Mary’s body language that was sort of saying to me, “Don’t go there.” But given all the things that were going wrong, I felt like we had to do that.
Dr. LAKSHMI NAYAK: Have you thought about anything after the MRI?
BILL BROOKS: My thought — and Mary’s heard me say it a lot — is I want to see the next one to kind of see if it’s showing anything or not before I start to get worried or get too hopeful.
MARY BERNARDO BROOKS: Thank you.
BILL BROOKS: Thanks. Good to see you.
Dr. LAKSHMI NAYAK: Good to see you.
Dr. ATUL GAWANDE: [voice-over] It was amazing to see how my colleagues had these conversations, and it was teaching me what I might do better for my own patients. It turned out it also taught me how to do better for my dad. He got some bad news back home in Ohio.
[on camera] I remember I took notes in my journal around that time. Do you remember when Dad first started to get pain in his neck?
SUSHILA GAWANDE, Atul’s Mother: He had pain in his shoulder, and he thought that either playing too much tennis or just muscle. So when the result came, we were in a shock.
Dr. ATUL GAWANDE: [voice-over] He’d gotten an MRI. And as a surgeon, he knew the results were not good.
[on camera] He emailed the images. I opened them up, and it’s a huge mass and it’s concerning. He called me up, and as we’re piecing it together over the phone, we’re kind of realizing this is right in the middle of the spinal cord. So the puzzle is how do you get this out.
We’re two surgeons looking at a mass. It’s like two carpenters looking at a house. You know, you’re not saying, “Oh, yeah, we can’t fix this.” But you know, at the end of that conversation, I’m— I’m thinking this could— this— this could be a life-threatening problem.
[voice-over] It was hard for us, as a family, to talk about this. And that’s despite three of us being doctors. In fact, talking with anyone near the end of life about their decisions is so difficult that there are actually physicians who specialize in the process.
They’re called palliative care physicians— people like Kathy Selvaggi, who works at the Dana Farber. Her technique is as much about listening as it is about talking.
[on camera] What would be on your checklist for what I should make sure I do when I’m doing it next time?
KATHY SELVAGGI, M.D., Palliative Care Specialist: First of all, I think it’s important that you ask what their understanding is of their disease. I think that is first and foremost because, oftentimes, what we say as physicians is not what the patient hears. “And if there are things that you want to do, let’s think about what they are and can we get them accomplished.”
Dr. ATUL GAWANDE: You know, people have priorities besides just living longer.
Dr. KATHY SELVAGGI: Yes.
Dr. ATUL GAWANDE: You’ve got to ask what those priorities are.
Dr. KATHY SELVAGGI: Yes.
Dr. ATUL GAWANDE: Then you’ve got to tune the treatment to those priorities.
Dr. KATHY SELVAGGI: Exactly. And if we don’t ask and if we don’t have these discussions, we don’t know.
Hello. I’m Dr. Selvaggi. I’m Kathy.
Dr. ATUL GAWANDE: [voice-over] Dr. Selvaggi works with doctors throughout the hospital to help with their hardest patient conversations.
AYMEN ELFIKY, M.D., Oncologist: So how are you feeling?
NORMA BABINEAU: A little better than I was.
Dr. ATUL GAWANDE: [voice-over] Aymen Elfiky was one of those doctors. He’s an oncologist who, like me, grapples with reaching good decisions with his patients about dying. He’d been caring for a patient named Norma Babineau for two years. He said that during that time, he had tried to broach how dire her prognosis was, but he had not been successful.
Dr. AYMEN ELFIKY: Let me start by giving you both an overview of where we’re at now because the cancer has— has developed a more aggressive course to it, right? It’s a more resistant type, and that just keeps marching along. This is where the tough discussions come up. The disease, we knew, has been acting up. Right now, in this state, more treatment would hurt you more than help you. That’s just a fact. And you would not get the benefit of it.
PAUL BABINEAU: Is there a time, you think, a timeline, or—
Dr. AYMEN ELFIKY: We could be talking about three to four months. We can be longer. It can certainly be shorter, if it— if the pace picks up.
NORMA BABINEAU: There’s miracles that can happen in between.
Dr. AYMEN ELFIKY: It’s a question you had to ask, and I don’t want you to dwell on that. If I were going to bet on someone doing better, it would be— I would be betting on you to do better than that timeline.
Dr. KATHY SELVAGGI: Our goal is, for whatever time is left, is to make it the best quality that we can.
NORMA BABINEAU: But I need to take the baby to—
Dr. AYMEN ELFIKY: To where?
NORMA BABINEAU: To Walt Disney!
Dr. KATHY SELVAGGI: To do Walt Disney.
NORMA BABINEAU: Yeah. Yes, I’m going to take her for Christmas. We’ve got to find the right medicine to get me better so I can take my trips.
Dr. ATUL GAWANDE: [on camera] So the really hard part, I find, in these situations is, you know it’ll come to this point, when do you help them understand that? What— what’s going through your mind, though? What does it feel like to you?
Dr. AYMAN ELFIKY: That I wish I could do better.
Dr. ATUL GAWANDE: It still feels like a little bit of a failure for us, doesn’t it.
Dr. AYMAN ELFIKY: It’s very much a failure. And it’s hard.
Dr. ATUL GAWANDE: Even though you knew from the beginning you weren’t going to be able to— you weren’t curing this problem.
Dr. AYMAN ELFIKY: Right. It’s just a fight mentality that perhaps goes back to training in med school and just the way we are wired, and we’re not trained for that other mode.
Dr. KATHY SELVAGGI: Yeah, that’s where we have to take our cues.
Dr. ATUL GAWANDE: [voice-over] Palliative care doctors like Kathy Selvaggi are different. They’re teaching us there might be a better way in these circumstances.
Dr. KATHY SELVAGGI: You know, I think, in— I think it’s hard to hear sometimes the timeline. But I think it’s also important to have a sense because if there are things that you want to say or do or people that you want to see, it helps you to find that time a little better.
I think she knew that she was getting sicker and weaker. One of the goals was to try and get her home with hospice services. But the medications and the things that we’re requiring— it’s just not going to happen.
Dr. ATUL GAWANDE: [on camera] Forget Disneyworld. We’re not even knowing whether we can leave the hospital.
Dr. KATHY SELVAGGI: Exactly.
Dr. ATUL GAWANDE: So we didn’t do that before last Monday. Feels really late in the game, you know?
Dr. KATHY SELVAGGI: It does feel a little bit late in the game. We— you know, we’re all sort of taught that in order to make a difference in our patients’ lives, we have to be doing something. We have to be operating, we have to be giving them medication, we have to be radiating, we have to be giving chemotherapy.
In some ways, I think the medicine is the easy part. It’s all of this other stuff that’s much harder to deal with.
Two days later
Dr. KATHY SELVAGGI: How are you?
NORMA BABINEAU: Good. How are you?
Dr. KATHY SELVAGGI: I wanted to talk with you about— I know the other day, Norma, we talked about where to go from here. You may need more and more IV or intravenous medications to control your symptoms, and I’m worried that we’re not going to be able to do that at home.
NORMA BABINEAU: Right.
Dr. KATHY SELVAGGI: What do you think about that?
NORMA BABINEAU: Yeah, I think it’s coming close.
Dr. KATHY SELVAGGI: When you say “coming close”— that we’re coming near the end?
NORMA BABINEAU: Yeah.
Dr. KATHY SELVAGGI: I worry about the same thing. And what we’ll do is, we’ll— we’ll keep you here and we’ll take care of you here. OK?
NORMA BABINEAU: Yeah.
Dr. KATHY SELVAGGI: All right, Norma. All right. We’ll see you a little later, OK?
NORMA BABINEAU: OK.
Dr. KATHY SELVAGGI: OK. And I’ll get— why don’t I clear this out for you.
Dr. ATUL GAWANDE: [voice-over] Kathy Selvaggi had helped Norma understand that she was dying. Still, Norma had little time to say her good-byes. She died 10 days later.
Dr. KATHY SELVAGGI: These are really important conversations that should not be waiting the last week of someone’s life— between, patients, families, doctors, other health care providers involved in the care of that patient.
Dr. ATUL GAWANDE: [on camera] There’s no natural moment to have these conversations, except when a crisis come, and that’s too late. So I began trying to start earlier talking with my patients, and even my dad. I remember my parents visiting.
My dad and my mom and I had sat in my living room, and I had the conversation, which was, “What are the fears that you have? What are the goals that you have?” And you know, he cried and my mom cried. And I cried. He wanted to be able to be social. He did not want a situation where if you’re a quadriplegic, you could end up on a ventilator. You know, he said, “Let me die” if that should happen.
I hadn’t known he felt that way. This was an incredibly important moment. These priorities became our guidepost for the next few years, and they came from who he was as a person, who he’d always been.
[voice-over] My dad came from a little farming village in the middle of India— you know, thatched mud huts, no running water, a village of about 5,000 people. His father had 13 children. His mother died from malaria when he was about 10. That was when he decided he wanted to be a doctor.
He went to medical school in India. Afterwards, he was offered a job in a hospital in New York City, training to be a surgeon. He met my mom and married her, and they moved to Athens, Ohio, to set up their medical practices and raise a family. There he was part of the community, and that became especially important to him after the cancer.
As the tumor slowly progressed, we followed his priorities, and they led us and him to choose an aggressive operation, and then radiation. But eventually, paralysis set in, and then our options became chemotherapy.
So the oncologist lays out 8 or 9 different options, and we’re swimming in all of it. Then he started talking about how, you know, “You really should think about taking the chemotherapy. Who knows, you could be playing tennis by the end of the summer.” I mean, that was crazy!
[on camera] It made me very mad, because it was— I mean—
SUSHILA GAWANDE: Completely not right. Yeah.
ATUL GAWANDE: [voice-over] You know, this guy’s potentially within weeks of being paralyzed. The oncologist was being totally human, and was talking to my dad the way that I had been talking to my patients for 10 years. It was holding out a hope that was not a realistic hope in order to get him to take the chemotherapy. I then pushed. We were still in the back of our minds thinking, you know, was there any way to get 10 years out of this anymore. And she basically was saying no, and we needed to know that.
Medicine often offers a deal— We will sacrifice your time now for the sake of possible time later. But my father was realizing that that time later was running out. He began really thinking hard about what he would be able to do and what he wanted to do in order to have as good a life as he could with what time he had.
I guess the lesson is you can’t always count on the doctor to lead the way. Sometimes the patient has to do it.
When I first learned of Jeff Shields, he had already gone through three years of treatment for a rare form of lymphoma. Chemotherapy hadn’t worked. He hadn’t given up hope, but he was also recognizing that his odds were diminishing, even as his doctors were offering him more treatment options.
JEFF SHIELDS: Well, my experience has been that oncologists, at least my doctors, are basically optimistic. And they’re always looking for a way to push the disease into remission than they are in talking about the longer-term picture of mortality. I spent time talking to Genie, my wife, thinking about— at least for me, I want to make a decision. I don’t want to linger.
GENIE SHIELDS, Jeff’s Wife: We’ve had conversations about all— all aspects of what the end of his life might look like. And most of all, he says, “I want to be at the farm.” And you know, hopefully, I’m in a position to make sure that happens.
We have an appointment that I hope will result in them saying that the disease is lessened. But they might say, “No, it’s not under control.” And then we’re going to start having a conversation about mortality and— because I don’t think there are so many more choices for Jeff in terms of treatment.
JEFF SHIELDS: Come on in. Hey, Rob.
Dr. ROB SOIFFER, M.D., Oncologist: Hey. Hey, Jeff.
GENIE SHIELDS: Hi, Rob.
Dr. ROB SOIFFER: Hi. How’re we doing?
GENIE SHIELDS: Good.
JEFF SHIELDS: Thanks for coming over.
Dr. ROB SOIFFER: My pleasure.
JEFF SHIELDS: Any results on the biopsy?
Dr. ROB SOIFFER: Yes. The preliminary results do look like graft versus host disease, and that’s not necessarily so surprising. We expected that.
I first met Mr. Shields about two years ago. At that point, he had a bone marrow transplant. And unfortunately, about a year after the transplant, he showed signs that his disease was coming back. In addition to that, he has a complication of transplant, where the donor cells are actually attacking his body. And unfortunately, it’s wearing him down.
It almost goes without saying, but we may have to make a— you know, a new game plan a week from now.
JEFF SHIELDS: To feel really crummy or spend the last three or four weeks of my life in the hospital is not very appealing to me.
Dr. ROB SOIFFER: I bet not.
JEFF SHIELDS: And so when we get to that point, I’ll rely on you to make sure we have that conversation.
Dr. ROB SOIFFER: Right. And it’s a group discussion for all of us.
JEFF SHIELDS: It sure is.
Dr. ATUL GAWANDE: It’s always a hard thing, right? How do you know if they’re coming towards the end versus changing the therapy again?
Dr. ROB SOIFFER: Well, I don’t think we ever know.
Dr. ATUL GAWANDE: Right.
Dr. ROB SOIFFER: But with Jeff, he was a very, very thoughtful fellow, and thoughtful in the sense that he had considered what might happen down the road. And he made it very clear to me that if we thought some therapy might be helpful, might prolong his life with reasonable quality of life, he was happy to go for it. He also made it very clear that if we thought that things were going to go badly or if things looked like they weren’t going to work, he didn’t want to pursue therapy just for the sake of pursuing therapy.
Three weeks later
GENIE SHIELDS: It seems to me there’s such a difference in these last few weeks. And we know the lymphoma is growing and— and sort of rampant. What I’m worried about is, could we be coming to a place where it’s— it’s actually killing you and we don’t have the opportunity to really talk with the children and the—
JEFF SHIELDS: You mean where I am in what I consider in hospice — in other words, end stage —
GENIE SHIELDS: Yes.
JEFF SHIELDS: —and we don’t have a— I’m going to live for four weeks, and we’re thinking, “Oh, maybe there are three months.”
GENIE SHIELDS: Yeah. Yeah.
JEFF SHIELDS: I think we should ask that at our next visit.
GENIE SHIELDS: All right, here. Go into your Benadryl stupor!
Two weeks later
Dr. ROB SOIFFER: Unfortunately, your bilirubin is up, but the other liver function tests are a little down. You know, I can’t put a particularly good spin on that. I don’t know how negative a spin to put on that, but I can’t put a good spin on that.
JEFF SHIELDS: I wanted to clarify something I said.
Dr. ROB SOIFFER: Yeah.
JEFF SHIELDS: I don’t want to go back in the hospital. I want to die at home.
Dr. ROB SOIFFER: Yeah.
JEFF SHIELDS: And that’s really my goal. And so I want you as my doctor, my good friend, to know that. The hospice people will know it.
Dr. ROB SOIFFER: Yes.
JEFF SHIELDS: Genie knows it. That’s my desire.
Dr. ROB SOIFFER: Right.
Dr. ATUL GAWANDE: [voice-over] It’s impressive for a patient — and a family — to be so clear about their priorities, like Jeff Shields was. Accepting that life can be shorter than we want is very difficult. It’s easy for all of us, patients and doctors, to fall back on looking for what more we can do, regardless of what we might be sacrificing along the way. And that’s especially the case with younger patients, and that is where a doctor needs to be skilled, I think.
Dr. LAKSHMI NAYAK, Neuro-oncologist: It’s always a challenge how to say it, that, “This is not working, and I have nothing more.” I try to deliver the bad news in pieces over a period of time. I feel a lot of times, they don’t absorb all of the information, and that’s why you have to keep repeating it and—
Dr. ATUL GAWANDE: You saw that with Bill Brooks.
Dr. LAKSHMI NAYAK: Yeah.
So the MRI— there’s a little change, unfortunately. There’s a small area, a new spot. It’s not super-large, but it’s there.
This is the beginning of the end. I think it’s progressing to an extent that we may not be able to do anything to control it. He’s one of those few people in whom, you know, if there’s something that you could try, it’s worth trying rather than just waiting.
BILL BROOKS: So what do you think about the AbbVie? I just saw it on the news yesterday. They just got FDA approval for one of their brain tumor medications.
Dr. LAKSHMI NAYAK: That drug— we actually have a trial with that drug. I’ll look into it. I’ll look to see what the status of that is and see if it makes sense for you to get it. It’s not going to be on a clinical trial for you. If we do it, we’d have to do it as a compassionate use.
MARY BERNARDO BROOKS, Bill’s Wife: OK.
Dr. LAKSHMI NAYAK: And I wouldn’t want to give you something if it would potentially make things worse, so—
BILL BROOKS: Worse. Sure.
Dr. LAKSHMI NAYAK: But I’ll definitely look into that.
Bill brought up this particular drug, but it is experimental.
Dr. ATUL GAWANDE: Are you at all worried that he would just have toxicity from the drug without benefit?
Dr. LAKSHMI NAYAK: Yes and no. At this point, I knew that he wasn’t going to live for too long without anything. So whether he— at least he felt that he could try.
Dr. ATUL GAWANDE: [voice-over] Bill was only able to get one dose of the experimental drug because he was getting sicker. The spinal taps were beginning to stop working. The pressure in his head continued to build, and the effects were becoming undeniable. That was when he began to prepare.
BILL BROOKS: I’m really declining quickly. I need a lot more help even doing basic— you know, basic walking and things like that. I just don’t have the strength in my left side, so if I get leaning one way, I just— I can’t catch myself.
MARY BERNARDO BROOKS: Can I flip them?
BILL BROOKS: Yeah. It took me 15 years to collect this. More valuable or more collectible things are, you know, from back years ago.
MARY BERNARDO BROOKS: Is it just this pile here? No, you have more than that.
BILL BROOKS: If I die tomorrow, she’s not going to know how to dispose of this properly, to get the most bang for her buck.
MARY BERNARDO BROOKS: Want me to just move all these canvas ones?
BILL BROOKS: Well, those are going to be the good ones.
MARY BERNARDO BROOKS: These are the good ones?
BILL BROOKS: The canvas ones, yeah.
MARY BERNARDO BROOKS: Oh, OK.
BILL BROOKS: Yeah, that one’s a good one.
I’m just overwhelmed with everything. The mental roller-coaster has been the hardest thing to deal with. It’s just like, “OK, am I dying? Am I not? Can I function? Can I not?” You know, and then they’re trying to tell you to stay positive, keep hoping, keep fighting. And I’m, like, “I’ve been doing that for two-and-a-half years.” I’m— I’m at the end of my ropes as far as that goes.
I can’t take any more bad news. I’d rather go into the meeting and have her just pull a gun out and shoot me than have to listen to her try and be nice while she’s giving me bad news. Like I said, I’m a positive person, but I’m— I’m at the end of my ropes with it. I’ve fought as best I can.
Dr. ATUL GAWANDE: Accepting death comes with incredibly complex emotions. Bill’s hopes for more years had turned to weeks, and the question became when to let go of treatments if they’re not helping, to accept what Dr. Nayak and Sandra had been conveying about considering hospice.
Dr. LAKSHMI NAYAK: I think we need to talk about what’s been going on for the last few days, the fact that you didn’t respond to the spinal taps. I wouldn’t want to put you through any more spinal taps. There’s going to be a time when we’re not going to be able to deal with the pressure with the steroids.
MARY BERNARDO BROOKS: OK.
Dr. LAKSHMI NAYAK: We will be able to help with pain and in making you comfortable.
BILL BROOKS: OK.
Dr. LAKSHMI NAYAK: I’m worried that your disease is progressing quickly. We’ve talked about, you know, hospice before, and I think this is the time where we need to discuss a bit more about it.
BILL BROOKS: Well, Mary and I have talked many times. My thought again is I’m not afraid to die, but I’m afraid of all the suffering that goes beforehand. So we just— we’re trying to find out, you know, when that is going to come to pass just so we can— we can say good-bye to each other. [Mary weeps]
SANDRA RULAND, R.N., Oncology Nurse: Maybe we should just pause for a minute. It’s so much information.
MARY BERNARDO BROOKS: You go through this in your head over and over again, but you just don’t even want to think it’s a reality!
Dr. LAKSHMI NAYAK: I know.
MARY BERNARDO BROOKS: I’m sorry.
SANDRA RULAND: It’s really hard.
Dr. ATUL GAWANDE: [on camera] It’s impressive just being able to be silent for a while. Were you deliberately trying to be silent and let— let it happen?
Dr. LAKSHMI NAYAK: Yeah. I think it’s important to pause at the right time, some time. It’s a lot of information.
BILL BROOKS: Pleased to see you. Hopefully, I’m your last bad news for the day.
Three weeks later
MARY BERNARDO BROOKS: At this point, it’s just making sure he’s as comfortable as he can be, you know, and that’s the most important thing. You know, what’s working against him in a way is that he’s young and strong. It’ll just mean that he’ll linger longer.
This is it, yeah. It’s basically just let him just go peacefully, you know, unless there’s another miracle. [weeps] It’s OK. But anyway, my guess is that it just depends. It all depends on him, so— yeah, I’m just going to go check on him. I just want to make sure he’s OK.
Are you OK? I’m right here, sweetie. I just want you to be comfortable.
Dr. ATUL GAWANDE: Bill died two days later.
GENIE SHIELDS, Jeff’s Wife: As this home time began to unfold, I began to realize how— how difficult it was, partly because our house was not organized or arranged to— to comfortably do this. You know, suddenly, you have a hospital bed in the middle of your living room.
JEFF SHIELDS: Then I need you to help me bring my feet up.
GENIE SHIELDS: Here, Malcolm. We’re going to help Pop-Pop take his slippers off. Can you do that?
You want it to be as comfortable and happy a place for him as it can be. And at the same time, it’s— you know, it’s sort of the elephant in the room.
JEFF SHIELDS: Have I talked to you at all about my thoughts on dying and—
GRANDSON: No.
JEFF SHIELDS: Is it too hard? OK. Let me just tell you this. I’m not afraid of dying. I’ve had a long and wonderful life. And one of the nice things about being at the farm is that you realize everything dies. There’s a cycle of life. The cows die, the trees die, the grass dies, the fish die, and people die.
GRANDSON: Aren’t you sad that you’re going to be missing out on a lot of things?
JEFF SHIELDS: Well, I will be. And you know, I had hoped to have another 10 or 15 years, but you don’t always get what you want. I love you.
GRANDSON: I love you, too.
JEFF SHIELDS: See you in a few minutes.
GENIE SHIELDS: In those last weeks, you know, as his— as his space narrowed and narrowed to that bed, it grew in terms of the people he was drawing in. I hate to cry! Sorry. Oh! But— but that’s another one of those paradoxes. You know, as your— as your world comes closer and smaller and smaller, it becomes bigger and bigger. And— and he was seeing that.
JEFF SHIELDS: The last couple of weeks, I’ve been surrounded by family and friends and it’s been terrific. You know, some of the best days of my life, I must say. But then there’s a downward trend that’s more rapid than I had expected. I felt great during that time, and my body was in rapid decline. Since then, my mind has been in rapid decline. I get confused, so— but I’m still a happy guy.
Dr. ATUL GAWANDE: [voice-over] Jeff Shields’s words about his last weeks being his happiest seemed especially profound to me because they were among his last words. He died just hours afterwards.
In medicine, when we’re up against unfixable problems, we’re often unready to accept that they are unfixable. But I learned that it matters to people how their stories come to a close.
The questions that we ask one another just as human beings are important. What are your fears and worries for the future? What are your priorities if time becomes short? What are you willing to sacrifice and what are you not willing to sacrifice?
My father answered these questions. He entered hospice four months, as it would turn out, before he died. And he was a person mostly during that time. He was not a patient.
[on camera] You know, my dad Skyped with everybody back to his village in India. He had me and my sister come there and be with him, and he remained in control of the priorities that were most important to him.
[voice-over] I remember sitting in a chair, reading the newspaper, light coming in the window. My mother and my sister were having a conversation. And then we realized he wasn’t breathing. We waited to see if there would just be one more breath. And there wasn’t.
My dad made his wishes for what his life would be like, to the very end, very clear to us, including for what should happen even after the very end. He wanted to be cremated in the traditional Indian way, and he wanted his ashes spread on the Ganges River.
We took his ashes, my sister and my mother and I, to the ancient city of Varanasi, one of the oldest cities in the world, with a swami and a boatman taking us out in a dingy. And it was an amazing thing.
Millions, literally millions of families have brought the ashes of somebody in their family who’s died to the Ganges. That connection to people going back that many years makes you feel like you’re connected to that many years going forward, as well. You’re just this speck in time.
I felt he had brought us there and connected himself to all that was important to him. How is dying ever at all acceptable? How is it ever anything except this awful, terrible thing? And the only way it is is because we as human beings live for something bigger than ourselves.
BEING MORTAL
February 10, 2015
PRODUCED AND DIRECTED BY Thomas Jennings
WRITTEN BY Thomas Jennings and Atul Gawande
CORRESPONDENT Atul Gawande
PRODUCER Lauren Mucciolo
CONSULTING PRODUCER Annie Wong
FIELD PRODUCER Carla Borras
SENIOR PRODUCER Frank Koughan
EDITORS Steve Audette Chad Ervin
ADDITIONAL EDITING Molly Bernstein Barry Clegg Michelle Mizner
DIRECTORS OF PHOTOGRAPHY Brian Dowley Tim Grucza
PRINCIPAL PHOTOGRAPHY Mrinal Desai Travis Fox Thomas Jennings Stephen McCarthy Josh Weinstein
ADDITIONAL CAMERA Lauren Mucciolo Anna Belle Peevey Eric P. Gulliver Megan McGough Christian Jabari Canada
LINE PRODUCER Julie Rasquin
ORIGINAL MUSIC John E. Low
ONLINE EDITOR/COLORIST Jim Ferguson
SOUND MIX Jim Sullivan
SOUND Carla Borras Lauren Mucciolo
ASSISTANT EDITOR Jaclyn Lee
PRODUCTION ASSISTANTS Jabari Canada Sarah Jones
ADDITIONAL NARRATION Will Lyman
INTERN Hillary Hubley
INDIA PRODUCTION UNIT
DIRECTOR Nisha Pahuja
DIRECTOR OF PHOTOGRAPHY Apal Singh
FIXER Ashish Singh
PRODUCTION MANAGER Shenni Italia
THANKS Susan Block Zara Cooper Jane deLima Thomas Janet Abraham Michael Belkin Richard Stone Nick Sadovnikoff Joaquim Havens Ann Lacasce Tony Massaro
IN MEMORIUM Isabel Armstrong Norma Babineau Fran Brennan William Brooks Allen Chou Clyde Earle Rachel Johnson Anet James Mary Murphy Mary Pivero Rose Richards Geoffrey Shields Dennis Weron Debbie Whitmore
FOR FRONTLINE
PRODUCTION MANAGER Megan McGough Christian
ON-AIR PROMOTION PRODUCER Missy Frederick
ON-AIR PROMOTION EDITOR Barry Clegg
ASSISTANT EDITORS Eric P. Gulliver Lindsey Rundell
POST PRODUCTION ASSISTANT Kenzie Audette
FOR WGBH OUTPOST
DIRECTOR OF POST PRODUCTION Chris Fournelle
SENIOR DIRECTOR PRODUCTION TECHNOLOGY Tim Mangini
SERIES MUSIC Mason Daring Martin Brody
DIRECTOR OF AUDIENCE DEVELOPMENT Pamela Johnston
PUBLICITY ACCOUNT MANAGER Patrice Taddonio
DIGITAL ENGAGEMENT EDITOR Tim Molloy
DIGITAL COMMUNITY SPECIALIST Shauna Stuart
SECRETARY Christopher Kelleher
EDITORIAL SECRETARY Sophie Gayter
RECORDS MANAGER John Campopiano
CONTENT MANAGER Lisa Palone
LEGAL Eric Brass Jay Fialkov Janice Flood
SENIOR CONTRACTS MANAGER Gianna DeGiulio
UNIT MANAGER Sue Tufts
DIRECTOR OF BUSINESS Tobee Phipps
PODCAST PRODUCER/REPORTER Lu Olkowski
DIGITAL RESEARCH ASSISTANT Priyanka Boghani
DIGITAL ASSOCIATE PRODUCER Jason Breslow
DIGITAL VIDEO PRODUCER Michelle Mizner
SENIOR DIGITAL REPORTER Sarah Childress
MANAGING EDITOR, DIGITAL Sarah Moughty
POST COORDINATING PRODUCER Robin Parmelee
SERIES COORDINATING PRODUCER Carla Borras
SPECIAL COUNSEL Dale Cohen
SENIOR EDITORIAL CONSULTANT Louis Wiley Jr.
SERIES SENIOR EDITOR Andrew Metz
SERIES MANAGER Jim Bracciale
DEPUTY EXECUTIVE PRODUCER Raney Aronson-Rath
EXECUTIVE PRODUCER David Fanning
A FRONTLINE production 2over10 Media
© 2015 WGBH Educational Foundation All Rights Reserved
FRONTLINE is a production of WGBH/Boston, which is solely responsible for its content.
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.



















