A new drug has the potential to prevent malaria transmission and stem resistance—all in a single, low dose.
The promising drug is the first to target an essential protein that the parasite uses in all stages of its life cycle. Attacking every stage could be the key to eliminating malaria in a single dose.
So far, it has been tested in mice, where it eliminates infections of
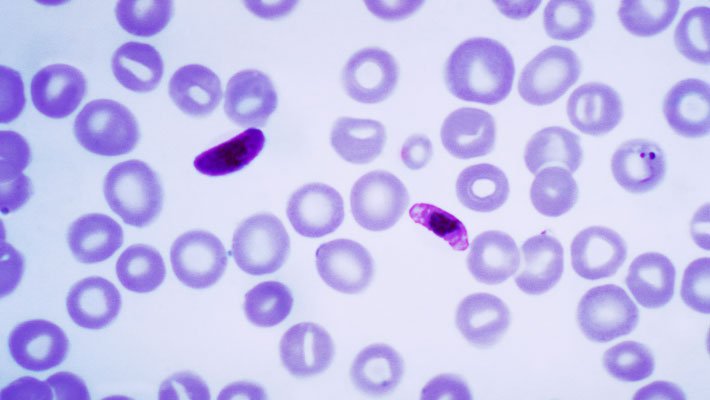
“With new chemistry, we discovered an antimalarial with a mechanism of action that no one has ever seen before,” said Eamon Comer, the lead chemist of the study. The study screened a 100,000 compound library inspired by molecules found in nature but not typically represented in pharmaceutical screenings.
Traditional pharmaceutical libraries are cheap to make, but the compounds are often flat, like sheets of paper. The compounds created by Comer and his team were more three dimensional and thus more likely to be successful drugs. “We can access compounds that nature can’t access,” Comer said. “There are certain reactions available to us that are not available in a living cell.”
While the techniques used to create the library were newly developed, sorting through the candidate compounds relied on an established method, the phenotypic screen. Phenotypic screens compare the drug potential of compounds by assessing the health—or ideally death—of the whole parasite when it’s raised with each compound.
The return of phenotypic screening is recent. At the dawn of the genome era, scientists turned toward a target-based approach, a method that first chooses a protein of interest and then systematically flips through compounds to find one that would inhibit that specific protein. Nobutaka Kato, the lead biologist of the study, said that antibiotic drug discovery projects using target-based screening don’t have a good track record.
Unlike target-based screening, phenotypic screens initially leave more to chance by not starting with a specific target in mind. “At the time, we don’t know what the target is, so it’s almost shooting in the dark,” Kato said. Researchers instead start by finding a compound that kills the parasite and then investigate how it works.
Once Kato found an effective compound, he added it to parasite cultures over months, eventually breeding resistant in the parasites. He then compared their genomes to an untreated parasite genome. In the resistant parasites, Kato found several single base-pair mutations in the gene that corresponds to a tRNA-synthetase protein, which is essential for replacing old, degraded proteins in all parts of the cell and for making new proteins when the parasite is dividing. The new compound is effective against blood-stage, transmission-stage, and liver-stage parasites.
The group made variations of the compound—a bicyclic azetidine—to make it more water soluble, a key quality of orally administered drugs. The variants were then tested in mouse models of human malaria. All mice treated with a single oral dose remained parasite-free for the 30-day monitoring period.
Comer and Kato are optimistic about the compound’s potential. “Some targets gain resistance faster, so there are some on the market that get resistance very quickly,” Comer said. “As for this target, we will have to see when it becomes a therapeutic.”
Drug resistance often arises when an infection goes on and off the drug. This can happen when people don’t finish a course of antimalarial pills, but it can also be a result of the complex lifecycle of malaria, which travels from mosquitos into human livers, to blood, then reproduction in blood, then back to mosquitos. Even if a patient takes their medication regularly, the parasite might not be exposed to the drug for enough time. Dormant parasites in the liver are often the cause of relapse and contribute to creating drug-resistant malaria.
“I think it’s reasonable that [the new compound] would be better for clearing the parasite and making it less likely to develop drug resistance, but it’s hard to know until you actually test it,” said Alexis Kaushanksy, assistant professor at the Center for Infectious Disease Control. Kaushansky studies factors in humans that the malarial parasite needs for survival, an approach that will ultimately combat resistance by eradicating liver-stage parasites.
Despite promising results, in an interview on The Naked Scientists podcast, Comer said it would be about 12 years until a drug from this screen would be on the market.

