Chadwick Boseman and the rise of colon cancer in young adults
Colorectal cancer is the second-leading cause of cancer deaths in the United States. Boseman’s case illustrates the importance of more screening—and addressing systemic inequities in health care.

Chadwick Boseman speaks at the 2017 San Diego Comic Con International for "Black Panther." Boseman died of colon cancer on August 28, 2020 at age 43. Image credit: Gage Skidmore
On Friday, August 28, actor Chadwick Boseman died at age 43 of colon cancer.
Perhaps best known for his role as King T’Challa in “Black Panther,” the actor starred in numerous other Avengers movies, “21 Bridges,” “Da 5 Bloods,” and a not-yet-released adaptation of “Ma Rainey’s Black Bottom.” This “superstar run” of back-to-back productions “seems all the more miraculous in light of the knowledge that Boseman pulled it off while quietly undergoing many surgeries and rounds of chemotherapy,” David Sims writes for The Atlantic.
The cancer that killed Boseman is the second-leading cause of cancer deaths in the United States after lung cancer. And although the majority of colon cancer cases are found in older adults, rates are rising among young people.
In July 2019, University of Texas at Austin researchers reported that “the proportion of newly diagnosed colorectal patients under age 50 rose from 10 percent in 2004 to 12.2 percent in 2015. Younger patients were also likely to have advanced cases more often than older patients,” Knvul Sheikh writes for the New York Times. (Colorectal cancer includes illness in which tumors are present in the rectum or the colon.) According to the American Cancer Society, about 18,000 people under 50 will be diagnosed with colon cancer in 2020.
Data from Canadian national cancer registries illustrate a similar trend in colorectal cancer rates in younger adults. Colorectal cancer rates increased by 3.47% among Canadian men under age 50 between 2006 and 2015, and by 4.4% among Canadian women under age 50 from 2010 to 2015.
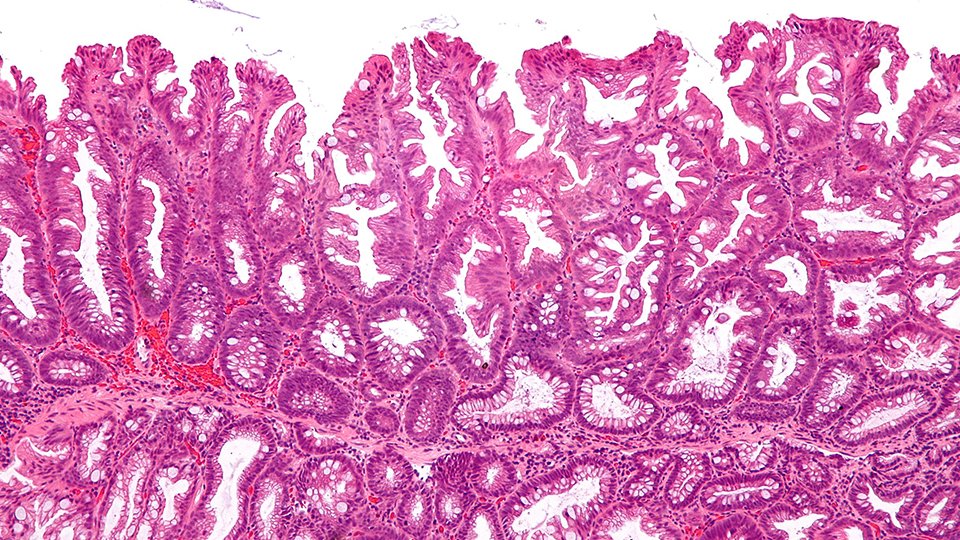
Micrograph of a colorectal sessile serrated lesion, which is most commonly seen in the cecum and ascending colon, and has the potential to lead to colorectal cancer. Image credit: Nephron, Wikimedia Commons
While older patients undergo regular screenings like colonoscopies, which help flag the disease in its early stages so that doctors can remove polyps before cancer develops (colorectal cancer rates have been declining among people over 65, likely because of more regular screenings), neither younger adults nor their healthcare providers are actively on the hunt for colon cancer, Kat Eschner reports for Popular Science. Therefore, younger patients are often diagnosed at the later stages of the disease and are more likely to die from their illness, whether or not their cancer is more aggressive than an older patient’s.
Experts aren’t yet sure why colon cancer rates are increasing among younger Americans and Canadians, but lifestyle changes may be a contributor. “Obesity and sedentary lifestyles, for example, are linked to colorectal cancer, as are poor diets low in fiber,” Sheikh writes. But experts are not entirely convinced these are the only factors at work. Trends in obesity among people of different ethnic and racial backgrounds don’t always correspond to an increase in colorectal cancer, Rebecca Siegel, an epidemiologist at the American Cancer Society Patients, told Sheikh.
Patients with chronic inflammation or Type 2 diabetes have also been found to be at increased risk for colon cancer. According to the National Institutes of Health, because of genetic traits, insulin resistance, and the prevalence of obesity—explained at least in part by systematic racism and allostatic load—African Americans have a high risk for type 2 diabetes.
As a Black man, Boseman belonged to the demographic of people who have the highest rates of colorectal cancer. In another major healthcare inequity, African Americans, particularly men, are more likely to be diagnosed at a younger age relative to other diagnoses, Eschner writes for Popular Science. And Black Americans are less likely to be screened early and are more likely to die of the disease, research shows.
At the Center for Young Onset Colorectal Cancer at Memorial Sloan Kettering Cancer Center, which was opened in 2018 to treat younger patients and study the reasons for their diagnoses, Co-Director Dr. Robin B. Mendelsohn and her colleagues “are exploring whether diet, medications like antibiotics, and the microbiome — which have all changed significantly for generations born in the 1960s and later — might be contributing to the cancer in younger people,” Pam Belluck writes for the New York Times.
As experts attempt to elucidate why colon cancer rates are increasing among young people, physicians should monitor their younger patients for symptoms that might suggest colorectal cancer, Nilofer Azad, a professor of gastrointestinal oncology at Johns Hopkins University, tells Popular Science. In this population, Eschner writes, symptoms like bloody stool, unexpected weight loss, and prolonged cramping can be overlooked or misdiagnosed as conditions like hemorrhoids.
Moving forward, better understanding and detection of colon cancer are crucial. But Boseman’s story and his legacy—an incredible collection of films created in a mere 7 years—also illustrate something else: a continued need to address systemic inequities in health care and beyond.



