What Drives Vaccination Rates?
The federal government, chiefly the U.S. Food and Drug Administration (FDA) and the U.S. Centers for Disease Control and Prevention (CDC), oversees the response to disease outbreaks. But when it comes to vaccinations, decision-making authority—such as about which vaccines are required and who can opt out of being vaccinated—lies with the states. And the states exhibit an almost head-spinning array of differences in their vaccination requirements and exemption laws. What factors influence the development of vaccine policy? And does the policy variability across the 50 states have an effect?
Is there any federal role in vaccine policy?
The CDC's Advisory Committee on Immunization Practices (ACIP) serves as the nation's advisor on vaccine recommendations. Its 15 expert members meet three times a year to review studies, safety data, and other factors related to national vaccination matters. They also participate in working groups all year, as needed, to stay abreast of vaccine-related developments, including availability of vaccines and outbreaks of diseases.
In making their recommendations, ACIP members aim to ensure that specific populations receive vaccine protection at the safest and earliest possible age, before the members of those populations reach peak risk periods. All vaccines must be licensed by the FDA, a process that requires years of safety studies and other testing. Other factors that the ACIP considers include how many children would be at risk of a disease if large numbers of them aren't vaccinated, how a vaccine's effectiveness varies according to the age it's administered, and what the severity is of the target disease.
Some diseases, such as measles, are common and can involve serious complications; the measles vaccine is thus on the recommended childhood vaccination schedule in the United States. But a mosquito-borne disease called Japanese encephalitis, while common in rural areas of Asia, is not at all common in the United States; so although a vaccine for this disease exists, it is
What are reasons for vaccine exemptions?
At the state level, the default position across all 50 states is to require proof of up-to-date vaccination against a defined set of diseases for children who are entering kindergarten and for children age five and older who attend a state-run day care. But parents have three possible ways to opt out of having their children vaccinated: medical, religious, or philosophical/personal-belief exemptions.
Children who need medical exemptions rely on a high level of immunization in their community for protection against vaccine-preventable disease, a concept known as herd immunity.
Sometimes, a child needs an exemption for medical reasons—such as having a suppressed immune system or having an allergy to some ingredient in a given vaccine. Children who need medical exemptions rely on a high level of immunization in their community for protection against vaccine-preventable disease, a concept known as herd immunity. All states allow medical exemptions, typically with a doctor's letter.
But not all states offer exemptions for personal or religious beliefs. Where these other kinds of exemptions are an option, the requirements for justifying such requests vary considerably across the country.
All but two states, Mississippi and West Virginia, include religious exemptions in their vaccine policies. Possibly not coincidentally, as of mid-2014 Mississippi and West Virginia haven't seen a measles outbreak since the early 1990s.

As of 2014 there are 20 states that allow some kind of personal or philosophical opt-out from childhood vaccinations. Of those 20 states, eight—including Colorado, Rhode Island, and Arizona—have made it comparatively easy for a parent to claim a personal-belief exemption. In most cases, all a parent has to do is sign a form. But other states—including Texas, Minnesota, and Arkansas—have rules that are somewhat stricter. Those states require steps such as submitting a notarized form with a clinician's signature, sometimes with a letter explaining the reason for the exemption request.
The laxity or stringency of these requirements seems to affect exemption rates. States with tougher rules have lower exemption rates and vice versa. And tightening existing rules appears to make a difference: When Washington State toughened its personal-belief exemption criteria to require a clinician's signature on the exemption form, exemption rates dropped 25% between 2009 and 2011.
How do policies affect vaccine exemptions?
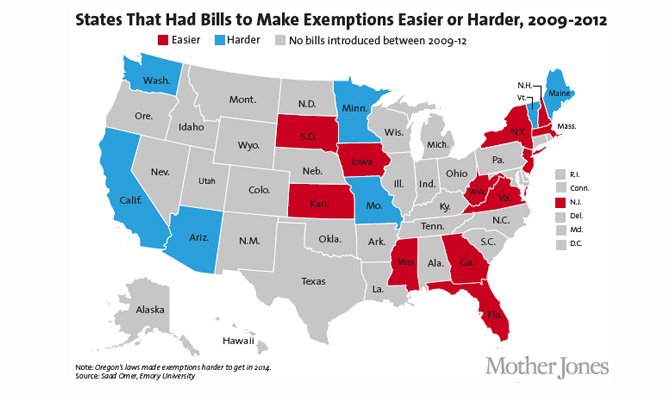
Obviously, then, if public health officials want more parents to vaccinate their children, making nonmedical exemptions more difficult to get is a key tactic. But convincing state legislators of the wisdom of that approach isn't necessarily an easy matter. In fact, in recent years, some states—including include Kansas, Iowa, and Florida—have seen legislative attempts to make exemptions easier to obtain. A 2014 study of vaccine-related legislative proposals found that 36 bills regarding exemptions were introduced in 18 states between 2009 and 2012—and 31 of them were intended to ease the criteria rather than toughen them. But to the likely relief of public health officials, none of the bills aimed at easing exemptions passed, while three of the five bills tightening restrictions were enacted into law.
California is among the states that have sought to follow Washington State's lead and toughen requirements for nonmedical vaccine exemptions. The Golden State is home to hot spots of vaccine opt-outs, with rates higher than 60% in some schools. And personal-belief exemptions for California kindergartners tripled between 1979 and 2008. In response, in January 2014, a new California law came into effect, requiring parents to obtain a clinician's signature when claiming a personal-belief exemption. In signing the bill, however, California Governor Jerry Brown told the Department of Public Health to add a religious exemption option that would not require a clinician's signature. This addition concerned some public health experts in California, not least because exemptions in that state had already climbed at least 12% from 2012 to 2013, before the law came into effect. Time will be the final arbiter of whether exemptions go up—a sign that the requirements made opting out easier—or go down—a sign that the bill had the intended effect.
Is there a role for publicity?
When legislative measures fail or require backup, health authorities in some states are turning to a kind of naming-and-shaming policy. Not only do they determine which locales have high exemption rates, but they also publicize that information. Colorado, which has a relatively high rate of kindergartners with vaccine exemptions, is considering this tactic.
The effect of publicity can go beyond simply informing state residents about where herd immunity might be low. Exemption enforcement often lies in the hands of local school personnel. Studies suggest that even in states like Massachusetts and Missouri, which disallow personal-belief exemptions, almost 20% of schools allowed them anyway. Publicizing hot spots of vaccine exemptions could spur improved oversight at the local level.
How is policy set on the front lines?
Some pediatricians have decided not just to encourage parents to have their children be vaccinated—and sign the exemption form for those who decline to do so—but also they have refused to take patients whose parents opt out of having them vaccinated. This practice is not in keeping with the policy of the American Academy of Pediatrics, however. But given that an outbreak in southern California was traced to a physician's waiting room, doctors feel they have good reason for strict constraints of this nature. Some physician practices don't mince words in communicating their belief in the importance of vaccination. One California practice, for example, notes that, "by not vaccinating you are putting your child at unnecessary risk for life-threatening illness and disability, and even death."
The threat to others is relevant to the policy discussion as well, some have argued, suggesting that the repercussions of not vaccinating should go beyond calling out schools with low vaccination rates. One bioethicist, Arthur Caplan, has proposed that families who opt out of vaccination should be held liable if an outbreak is traced to their door.
Vaccine policy also finds its way into the courts. New York City allows religious exemptions, for example, but bars unvaccinated children from attending public school if another student at the school has a vaccine-preventable illness, such as chickenpox. In response to a suit from some parents whose unvaccinated children were barred from school on these grounds, a judge ruled in favor of the city. He cited a 1905 U.S. Supreme Court ruling that a man who was fined $5 for refusing the smallpox vaccine during an outbreak did, in fact, have to pay up.
Does money matter?
A legal threat might influence parents who opt out of vaccination for philosophical reasons, and courts and local authorities may draw exemption lines in the sand. But vaccine refusal isn't always a matter of philosophy and may not even be an active choice. Sometimes, it's about money and time. Research suggests that so-called "exemptions of convenience" also contribute to low vaccination rates, particularly when signing a form is simply cheaper and easier for struggling families than finding the funds to pay for childhood vaccinations and taking time off of work to take their child to the doctor.
Studies suggest that children with vaccine exemptions are as much as 22 times more likely than vaccinated children to contract measels in an outbreak.
While no one can buy parents more time, the 2010 Affordable Care Act (ACA) might take care of the cost barrier. The law requires that health plans offered under the ACA cover all childhood immunizations administered by an in-network provider, with no deductibles or copayments. The federal government also offers the Vaccines for Children program, which provides no-cost vaccines for those who meet eligibility requirements.
Why do exemptions matter?
Whether people are cajoled, encouraged, or mandated to have their children vaccinated, the need to keep exemptions at a minimum is real. Studies suggest that children with vaccine exemptions are as much as 22 times more likely than vaccinated children to contract measles in an outbreak. And although recent pertussis outbreaks can be traced in part to waning immunity in children who did receive the vaccine, one study showed that children who were not vaccinated had an six-fold greater risk of contracting the disease than did fully vaccinated children.
According to a 2014 report, the recommended U.S. schedule of vaccinations against 13 diseases saves 42,000 lives each year, prevents 20 million cases of illness, and saves $13.5 billion in direct costs and $68.8 billion in indirect costs. Regardless of the focus of cost calculations—lives or money or both—vaccines are clearly the better policy and public-health bet.


