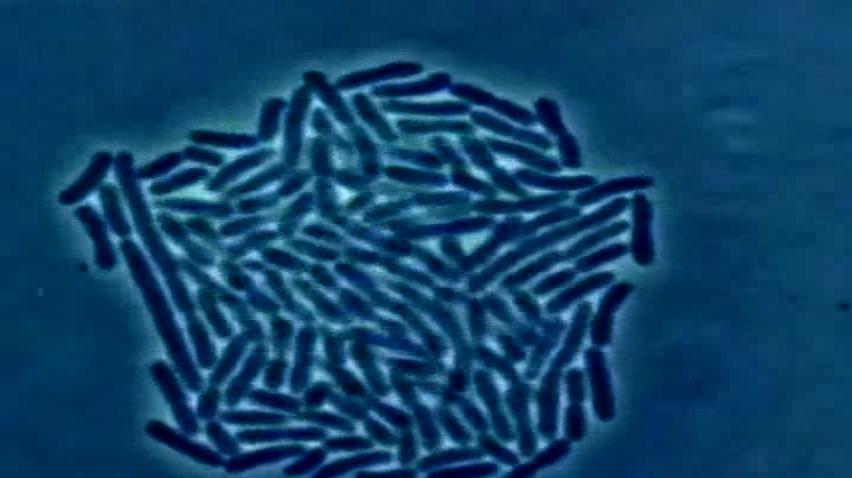
Can E. Coli in Supermarket Meat Cause UTIs?
October 14, 2014
Share
Any urinary tract infection is bad, but some are getting worse. Along with the burning, piercing pain that typically accompanies a UTI, these infections pose another challenge: They’re getting much harder to treat.
For the past 20 years, doctors have been tracking a troubling rise in antibiotic-resistant UTIs, which primarily affect women. There are an estimated 8 million UTIs in the United States each year, and though most of these infections are still treatable with more powerful antibiotics, some otherwise healthy patients find themselves in need of IV treatment — and in some cases can develop deadly bloodstream infections.
“You don’t have a normally healthy 30-year-old woman come in, who’s never been in a hospital, with a resistant urinary tract infection that’s moved to her blood,” Elizabeth DuPreez, an infectious disease pharmacist who helped treat cases in Flagstaff, Ariz., explained FRONTLINE. “Where did she get that organism from?”
Dr. Lance Price, a George Washington University microbiologist working in Flagstaff, believes that in some cases, the answer is supermarket meat.
Watch the video:
After testing more than 1,200 samples from Flagstaff-area infections, Price says he’s genetically linked more than 100 of them to supermarket meats. A quarter of those were resistant to several antibiotics.
Price’s work hasn’t yet been peer-reviewed, but he shared his preliminary findings with FRONTLINE for The Trouble With Antibiotics, airing tonight on PBS (check local listings). While Price and his team can’t conclusively connect the Flagstaff infections to antibiotic use on the farms where supermarkets get their meat, he believes his use of sophisticated whole-genome sequencing points back toward the farm.
“When we see this, when we see such genetic relatedness like this, the alternative explanations become, you know, impossible,” he told FRONTLINE.
Related Documentaries
Latest Documentaries
Related Stories
Related Stories
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.




















