In Race Against TB, Testing Struggles to Keep Up
March 25, 2014
Share
One of the first signs that the fight against tuberculosis had entered a frightening new phase came in the village of Tugela Ferry in central South Africa. Starting in 2005, 53 patients checked themselves into the Church of Scotland Hospital there with a rare strain of extensively drug-resistant tuberculosis — XDR-TB for short. Within 16 days of being tested, on average, all but one of the 53 were dead.
The outbreak left global health officials deeply puzzled. As recently as the 1980s, TB, a disease as old as antiquity itself, appeared close to eradication. Suddenly, it was resurfacing in a virulent new form.
Just as concerning was the realization that flaws in how the medical community tested for the disease were partly to blame for allowing such dangerous new strains to evolve and spread.
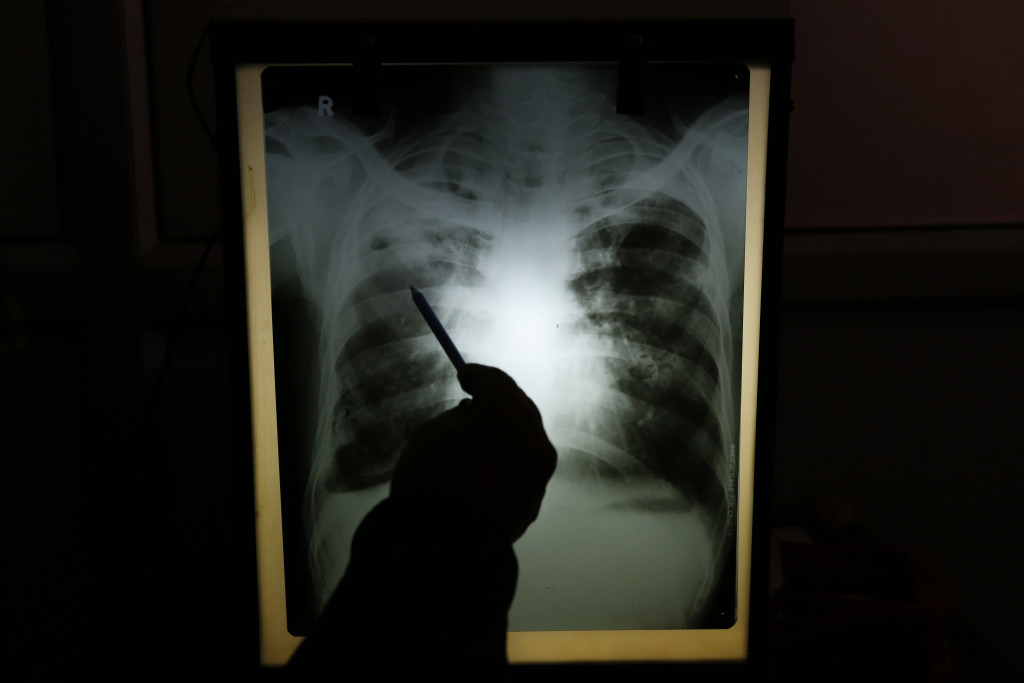
The standard test for tuberculosis was developed more than a century ago, in the 1880s. Doctors use a microscope to examine a patient’s sputum — the mucus that comes up from the lungs when you cough. It’s hardly a perfect process, and as Michael Specter noted in a 2010 New Yorker story, the instructions can get “comically complex”:
“Spread sputum on the slide using a broomstick,” a typical recipe, posted on the wall of a clinic in Patna, begins. “Allow the slide to air dry for 15 to 30 minutes. Fix the slide by passing it over a flame from three to five times for three to four seconds each time.” If the slide isn’t held over the flame long enough, false stains will appear — suggesting that people are sick when they are not. Hold the slide too long, though, and the stain will disappear and show nothing at all.”
At a cost of around $3 per test, sputum smears are among the most affordable options on the market. Roughly half the time, though, the diagnosis is wrong.
“The problem is it’s a bad test,” says Mercedes Becerra, an associate professor of global health and social medicine at Harvard Medical School. “It’s cheap and it’s easy but it doesn’t work and that’s what we’ve relied on against this pandemic. It’s really extreme.”
Because the smear test is unable to identify drug-resistant forms of the disease, experts still don’t know the full scale of the problem. The most recent data from the World Health Organization found that in 2012, less than 5 percent of newly confirmed TB cases and 9 percent of those previously treated for TB were tested for MDR-TB. In all, less than 25 percent of people estimated to have MDR-TB have been detected, according to the WHO.
A second test, known as a culture test — where a patient’s sputum sample is grown in a lab to see if it is drug resistant — is much more accurate than the smear test, but costs more and takes weeks to yield results. Culture is the gold-standard for diagnosis, but in poorer nations especially its adoption has been limited by the test’s technical complexity and the need for sophisticated laboratory infrastructure. WHO guidelines call for at least one culture lab for every 5 million people, but in 2012 that target was missed by 14 of 27 nations with the highest burdens of MDR-TB.
Another challenge is that sputum is not particularly useful when it comes to testing children for TB. That’s because children are often just as likely to develop the disease in the brain or in their bones, rather than in the lungs. Even if the disease is pulmonary, children carry a smaller bacterial load, which makes using a microscope to test for child TB disease effective in just 5 percent of cases. Sputum cultures can identify the disease in 15 percent of cases.
“Part of the problem is that people haven’t invested enough in these tests,” says Salmaan Keshavjee, an associate professor of global health and social medicine at Harvard Medical School. “When we had the anthrax outbreak in the United States after 9/11, the government invested in machines that could look at our mail and tell if they had anthrax. Money was put to the problem. There aren’t a lot of resources going toward creating new TB diagnostics.”
There is one promising test, the GeneXpert, that has recently come onto the market. The machine, which looks like a high-end espresso maker, analyzes DNA sequences that are specific to TB and can deliver results in about two hours. GeneXpert can also test for resistance to rifampicin, one of four main first-line drugs used to treat TB.
Its early success so far has been seen as a game changer. In 2010, a study in The New England Journal of Medicine found GeneXpert exams caught active TB infections in 98 percent of cases. That same year, the WHO endorsed GeneXpert and by June 2013 more than 1,400 machines and 3.2 million test cartridges had been acquired by 88 of 145 countries eligible for discounted pricing through the WHO. In a potential sign of things to come, South Africa became the first country to adopt GeneXpert as its primary diagnostic test for TB, replacing sputum smear analysis.
Yet despite its capacity to deliver faster and more accurate results, wider use of GeneXpert has come with a catch: Specifically, can nations that are already overburdened by TB cases keep pace with a surge in new patients identified by GeneXpert?
In South Africa alone, use of GeneXpert is expected to increase the number of TB diagnoses per year by as much as 37 percent, and the number of MDR-TB cases by as much as 71 percent, according to a 2012 study in the journal PLOS ONE. That’s likely to raise the cost of diagnosis per patient by 55 percent, the study found.
“People say it’s unethical to test somebody and not give them treatment,” says Keshavjee, but “it’s more unethical to not test somebody, not give them the opportunity to get treatment, and let them just go on infecting their family and friends and community without any knowledge.”
The cost of inaction is way too high, he warns. Already, 20 percent of previously identified TB cases and 3.6 percent of new cases are drug resistant, according to the WHO. XDR-TB, meanwhile, has spread to 92 countries, including the United States. The most recent case was identified this month, 10,500 miles from Tugela Ferry, in Los Angeles County.

Related Documentaries
Latest Documentaries
Related Stories
Related Stories
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.