In Seattle, Early Help for Homeless Residents During the Coronavirus Outbreak

April 22, 2020
Share
As Seattle residents prepared to shelter in place last month, there were an estimated 12,000 struggling to find homes.
One of them was Theresa Paulson. At 59, she’d been staying in a women’s shelter, where living quarters can be crowded. A few days before the stay-home order took effect, she invited me into her temporary new home — a room in a Travelodge motel.
“Come on in! Here’s the room.” The tiny Alaska Native woman — she can’t be more than 4’11” — welcomed me with a proud smile. “It has a coffee maker, a king-sized bed and even a safe,” she told me. Then, with a giggle: “In case you have a million dollars.”
She cranked up the heater against the chill outside, and keeping my distance, I helped her learn how to use the Keurig machine. Then, she sat on the foot of her bed, turned the TV to cartoons and said: “I wish I could stay here forever, man.”
Paulson is able to self-isolate here thanks to a small nonprofit organization that supports tribal elders experiencing homelessness. It’s one of many organizations that sprang into action amid the pandemic to help the region’s most vulnerable.
Home to the first U.S. epicenter of the pandemic, Seattle, its surrounding King County and the state of Washington, led the nation as the first responder to the outbreak. But in the early days, even as the city, county and state bureaucracy churned into action, there were already small groups of dedicated aid workers acting independently to help people experiencing homelessness.
Those struggling with homelessness aren’t initially at high risk to contract COVID-19: they don’t travel internationally and are often isolated. But if someone in the homeless population were to contract it, the contagion could spread rapidly through crowded shelters or makeshift encampments. On a day last month, I went out with FRONTLINE Correspondent Miles O’Brien to understand how aid workers were supporting this most vulnerable population.
Colleen Echohawk runs the Chief Seattle Club, the day center that found the motel room for Theresa Paulson. Seattle is home to one of the largest populations of people experiencing homelessness in the country. Ten percent are native people, even though they make up less than one percent of the area’s total population.
The club, which is supported by a mix of public and private funding, typically provides meals, showers, laundry and other basic services to native people who need help, including some housing, Echohawk said, speaking from her sunlit office decorated with dream catchers and small totem poles. But the pandemic presented additional challenges, she said.
“Our relatives out there who are experiencing homelessness may not quite get it yet and so, we’re doing tons and tons of communication about what is happening and how we have to respond,” Echohawk said. “They need us to do more than we’ve ever done for them, and we have to take extraordinary measures so, that we can support them in staying safe and healthy and staying alive.”
Of particular concern: older people with medical problems, who are at greater risk for mortality if infected with coronavirus.
“If we can get them into those hotel rooms, we’ll be saving lives,” she said. By the end of last month, the club had received around $160,000 in private donations — enough to support 30 tribal members for several months.
In addition to getting people inside shelters and motels, aid workers also worked to correct misinformation and rumors about the government’s response to the outbreak. It’s a problem that has made it difficult to reach a population already skeptical of the government, as we discovered in an encampment a few miles south of downtown Seattle.
About a dozen people live here in tents or shelters made from tarps, tents and scrap material tacked together. We met three social workers from non-profit organizations who were making a routine visit, but with a new mission to deliver health and safety information about coronavirus.
On this day, in the golden light of early sunset, one man was crouched over a campfire, cooking sausages in a cast-iron skillet. Another was eating oatmeal from a pot, and others were tending to their dogs. Our film crew and the social workers drew the group’s attention.

A woman named Melanie, who said she has lived at this camp for about two months and has been homeless since 2018, told us she’d heard a rumor that the state had imposed martial law. “They’re saying we might be quarantined,” she said. “Well, how do they quarantine us out here? I mean are they talking about — we have to be arrested to quarantine us or something?”
Rumors and misinformation can spread like viruses too, and they can be just as difficult to contain. Dawn Whitson, one of the social workers with REACH, a Washington addiction treatment nonprofit, explained that martial law hadn’t actually been imposed. She gave Melanie and others who had gathered around a fact sheet on COVID-19, and talked about health and safety information — including the heightened importance, for those who use drugs, of not sharing needles. I noticed one of the nurses hand a needle in plastic packaging to one man.
One of the most challenging hurdles is getting people tested. As it is, the Washington state public health lab can only test up to 300 COVID samples a day. Other labs, like the one at the University of Washington, can test a few thousand. But getting people to test before they show up in hospitals is key.
In the Belltown district of Seattle, family physician Dr. Richard Waters and two nurses had set up a makeshift testing site last month, on a sidewalk with folding chairs and a metal table outside a supportive housing residence. The team works for Neighborcare Health, a non-profit medical group that provides access to health care for people who have trouble affording it on their own. Waters, without clear guidelines or standard protocols, took up the cause and brought 80 COVID-19 test kits in a cooler and offered tests to adults who struggle with homelessness. His goal was to test as many people as possible and refer them to treatment accordingly.
“We’re doing standard guidance that everybody’s heard, try and practice social distancing, be mindful of how you cough, hands not touching face, good hand hygiene. In situations, if we were to find someone who has symptoms and they have troubles isolating or practice social distancing, we’d have conversations about why,” Waters said.
He added, “We’re also going to talk to people about drug use, substances disorders if that is something that inhibits people from being able to self-isolate.”
Dressed in protective gowns, including face shields and masks, Waters and his team were an unsettling sight in public view as they encountered passers-by and assessed them as candidates for testing.
A man with a severe cough declined a test. Several other people did not present symptoms that fit the criteria for COVID-19. Finally, an elderly woman named Patsy Williams rolled up in a walker chair. She said that she has chronic obstructive pulmonary disease and that lately her symptoms have worsened. She asked to be tested for COVID-19.
Waters performed the invasive nasal swabbing on Williams, making her gag and wince. He put the sample in a vial and into the cooler. It was the only test Waters administered on that very first day.
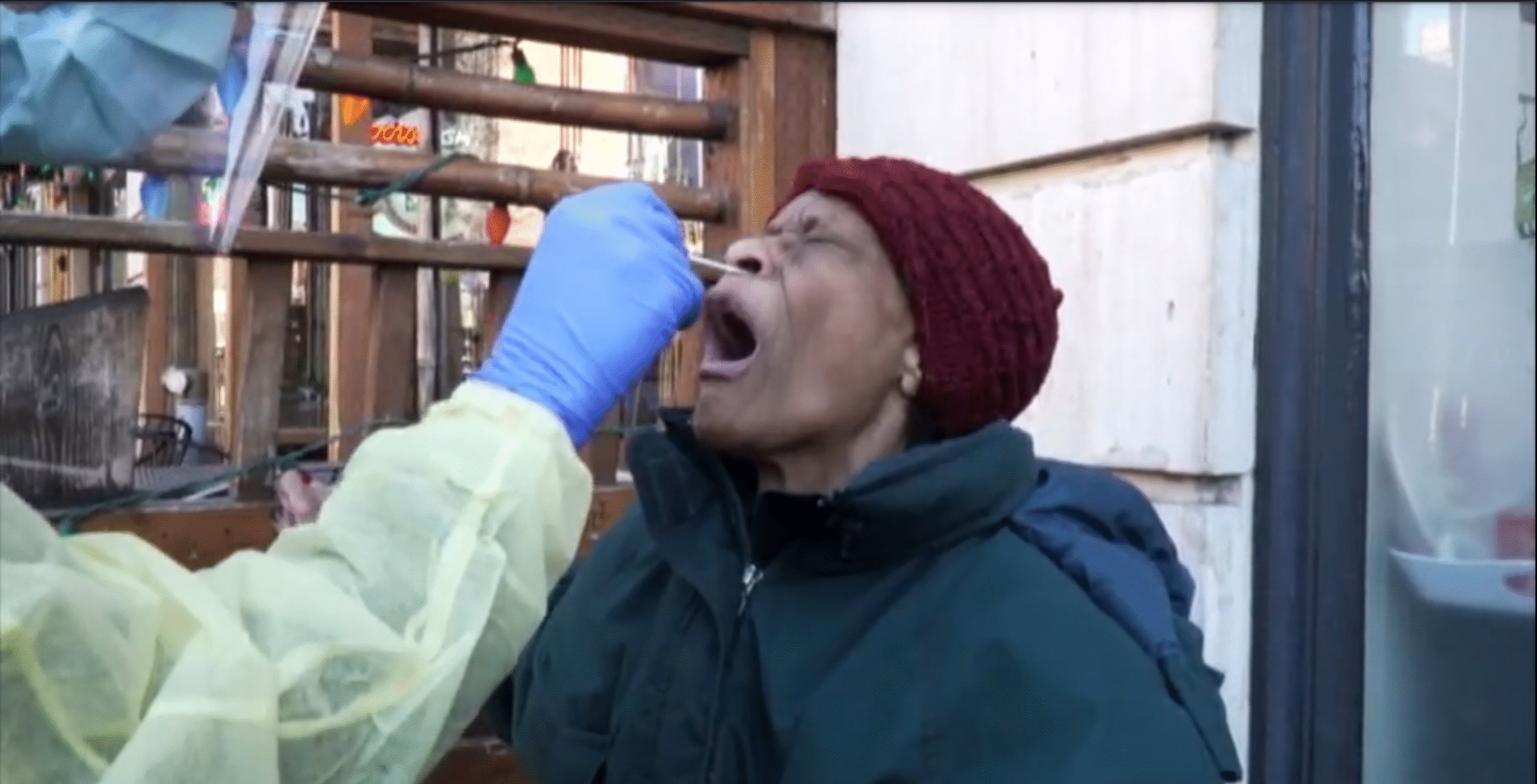
The following week, I learned that Patsy Williams’ lab results came back negative for COVID-19. And as he gained more experience and streamlined his process, Dr. Waters was having more success as well. By mid-April, he said he was testing up to 60 people a day.
Like everywhere else, sufficient testing in Seattle will be key to knowing who’s safe and who’s not. “We will continue to do what we can based on our staffing and the supplies that we have to care for our community,” said Waters.
As for Theresa Paulson, she, too, has tested negative for COVID-19 and remains inside her motel room. The club has enough funding to shelter her here through June.

Related Documentaries
Latest Documentaries
Related Stories
Related Stories
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.






















