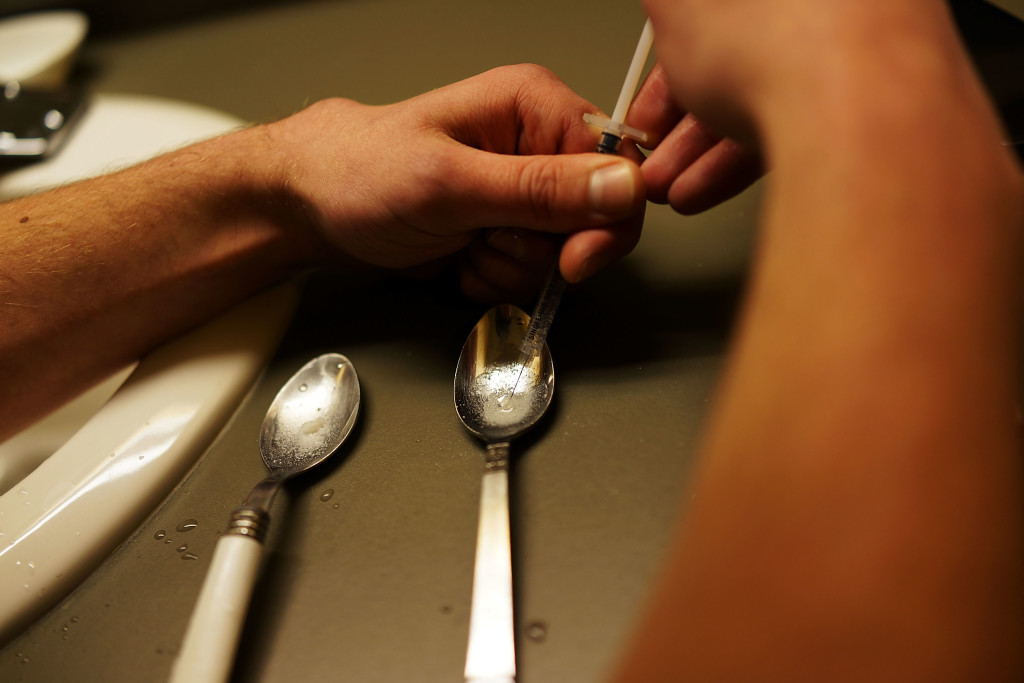
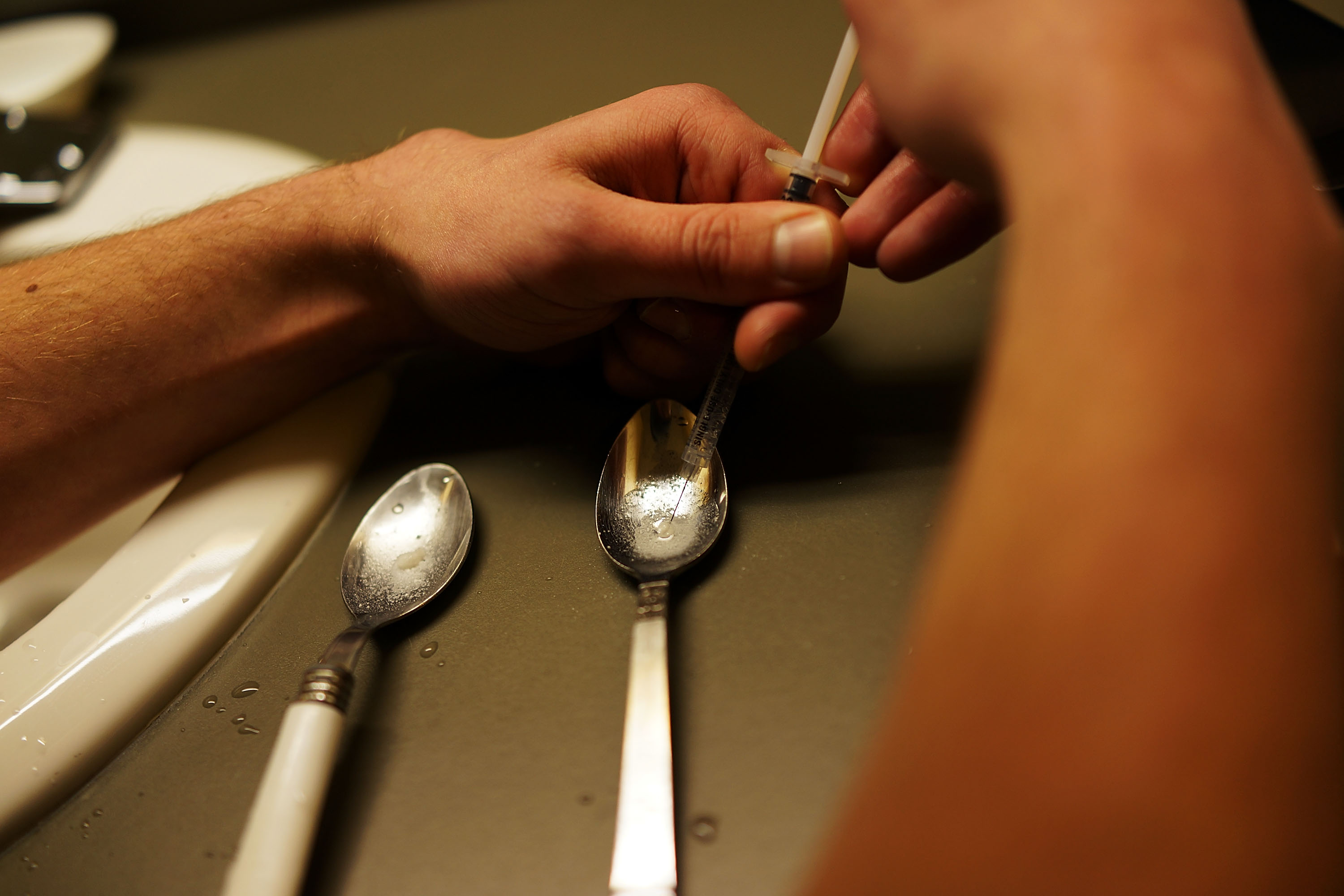
Veterans Face Greater Risks Amid Opioid Crisis
March 28, 2016
Share
As the United States struggles to deal with what’s been called the worst drug crisis in American history, its veterans have also been caught up in the opioid epidemic. About 60 percent of those returning from deployments in the Middle East, and 50 percent of older veterans suffer from chronic pain, according to Veterans Affairs officials. That’s compared to about 30 percent of Americans nationwide.
Veterans face a double-edged threat: Untreated chronic pain can increase the risk of suicide, but poorly managed opioid regimens can also be fatal. Veterans are twice as likely to die from accidental opioid overdoses than non-veterans, according to a 2011 study of the VA system.
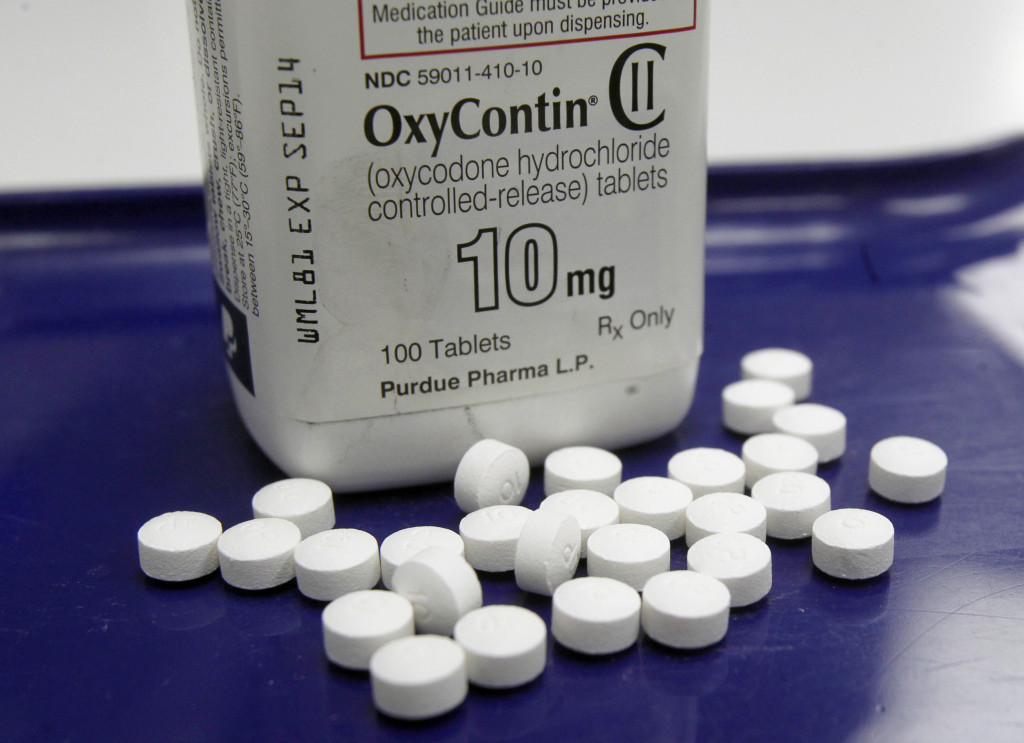
Until a few years ago, the VA was treating veterans’ chronic pain almost exclusively with prescriptions for opioid painkillers. Prescriptions for opiates spiked by 270 percent over 12 years, according to a 2013 analysis by the Center for Investigative Reporting, leading to addictions and a fatal overdose rate twice the national average.
The VA has taken some steps to address the problem. Since 2012, the height of the VA’s opioid prescribing, the department has reduced the number of veterans receiving opioids by 20 percent, and cut the overall opioid dosages for about 17,000 patients, the VA said. It has also begun screening more patients for depression and potential substance abuse problems, and coming up with more comprehensive approaches to chronic pain.
But the number of veterans with opioid-use disorders continues to grow, spiking by 55 percent over the past five years, from 2010 to 2015. The most recent figure, 68,000 veterans, represents about 13 percent of the total population of veterans currently taking opioids, according to VA data.
Dr. Carolyn Clancy, the VA’s deputy under secretary for health and organizational excellence, attributed the rising tally to an increase in diagnoses. “I’m very pleased to say that we have made substantial progress across the system,” she said, citing the reduction in opioid prescriptions and initiatives to better track veterans’ care. She added: “We’re not done, but it is literally a priority that is part of the fabric across our system, and we monitor this on a regular basis.”
But the VA has also acknowledged continued shortcomings in its handling of veterans with chronic pain, noting in a February letter to Sen. Joe Donnelly, D-Ind., that doctors don’t have enough time to follow up on veterans’ cases and that there is uneven access to care. “Ongoing growth in the number of VA patients with opioid use disorders, and logistical barriers to accessing care” have left some patients without access to comprehensive treatment, it said.
Donnelly, in a statement to FRONTLINE, said more work needed to be done. “Although the VA provided a long list of various efforts undertaken to combat opioid abuse, there is more work to be done to ensure VA has a comprehensive solution to this problem that is effective, efficient, and evidence-based,” he said. “But we need to start changing this culture immediately and begin to see results now.”
68,000 The number of veterans with opioid-use disorders. The figure represents about 13 percent of all veterans currently taking opioids.Perhaps the biggest challenge for the VA is finding a way to manage veterans’ chronic pain without depending solely on opioid painkillers. Addressing chronic pain is complex, Clancy said. “We do not have another silver bullet that we can say, ‘Instead of opioids, take this.’ It’s much more a matter of individualizing and trying different alternatives, and that can be really frustrating for patients as well as clinicians.”
It’s also time consuming. By the VA’s own admission, doctors often don’t have enough time to spend with patients to craft more tailored treatments. Army veteran Joshua Renschler testified before Congress that he developed liver damage after years on a 13-drug cocktail that included opioids to manage debilitating back pain after a mortar blast in Iraq that forced him to retire. Doctors in Washington kept prescribing pills to try to address the pain and side effects from medication, but offered few other solutions, he said.
“When it comes down to opioids, if we’re relying on the VA to provide this care, it almost mandates the need for opioid-based therapy, as sad as that is,” Renschler said. He still struggles with severe pain but now avoids medication because of his liver condition. “I’m just about as good as I’m going to get,” he said.
Some VA centers have started to introduce programs on managing chronic pain with acupuncture, yoga, mindfulness and physical therapy that can either reduce the need for painkillers or eliminate it entirely. But such programming is still lacking in many centers, veterans and advocacy groups say. Change is “happening, but it’s not happening everywhere,” said Jackie Maffucci, research director for Iraq and Afghanistan Veterans of America, an advocacy group, of the VA’s progress. “And it’s not happening 100 percent of the time.”
Jim Reed, an Army veteran and anesthesia provider, worries the VA still relies too frequently on opioids. Reed suffers from chronic pain from a neck injury, and said a doctor at the VA hospital he went to in North Carolina offered one prescription to help him sleep, one to stay awake, and opioids for pain. He declined them all, and instead takes Motrin and practices relaxation techniques.
But many younger veterans don’t question doctors’ orders, he said. Through his years of medical work, Reed said he has “routinely” encountered veterans, many of them in their 20s and 30s, who are taking a “laundry list” of medications.
“We’re sentencing these young people to a life of chemical dependency,” Reed said. “They’re living these lives of despair, because we’re just not doing things that make sense, that are evidence based.”
As the number of veterans diagnosed with opioid addictions increases, the VA has tried to curb opioid overprescribing and abuse. In 2013, the VA launched what it calls the Opioid Safety Initiative to track opioid use among veterans in its health care system. Veterans who take opioids are also required to sign a consent form and submit to urine tests.
The VA has started connecting with state prescription drug monitoring programs, which log controlled substances to prevent patients from obtaining multiple prescriptions from different doctors. As of February 2016, the VA said that it’s currently connected to state programs in 37 states.
By 2011, the year before the VA’s opioid prescriptions peaked, the number of veterans who overdosed on opioids had risen 33 percent, according to the VA. That’s only a fraction of the total that was taking opioids at the time, and the VA didn’t have more recent data.
But the risk of overdose, either accidentally or otherwise, remains high enough that in 2014 the VA began distributing naloxone, the drug that can reverse an overdose, to veterans who might be at risk. VA officials said the drug has been used to save 63 veterans since then.

Related Documentaries
Latest Documentaries
Related Stories
Related Stories
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation, as part of the Plum Bush Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.