Covering Coronavirus: Seattle, Washington
March 21, 2020
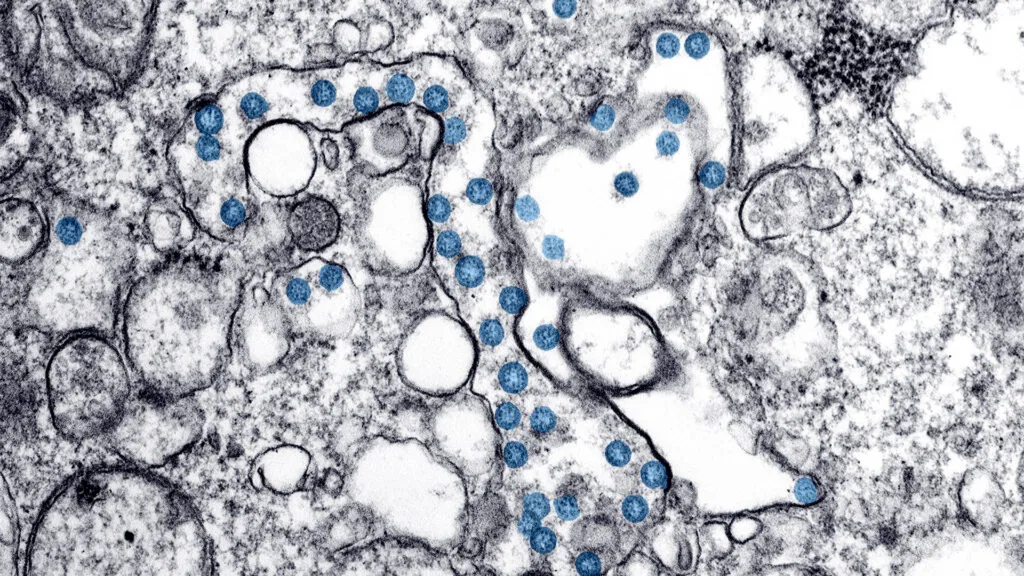
Lessons learned from Seattle — an epicenter of the COVID-19 outbreak. Veteran science reporter and FRONTLINE correspondent Miles O’Brien takes us inside the state where coronavirus was first believed to hit U.S. soil, where he finds, “They’ve put science at the center of their policy, and they’ve let the data drive the decisions.”
Latest Documentaries
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation, as part of the Plum Bush Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.




















