
|

|
Designing Clinical Trials
by Robert Cooke
High expectations are hard to live up to, especially if
they're someone else's. Judah Folkman found himself in that
position as his two big antiangiogenesis drugs, endostatin
and angiostatin, finally headed toward clinical trials near
the end of 1999. Folkman was expected to cure
cancer—it said so in The New York Times. Now
all he needed was for the drugs to work in people as
unequivocally as they had in mice. But it was not so simple,
of course, and the results would not be known quickly.
|
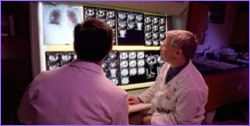 Doctors previewing a candidate for a clinical trial
of endostatin.
Doctors previewing a candidate for a clinical trial
of endostatin.
|
The first phase of the trials, as in tests of all drugs
overseen by the Food and Drug Administration, was designed
to test for safety, not efficacy. So those receiving the
first test doses would be the patients with the most
advanced cancers, patients for whom everything else had
failed, and they would receive very small doses to start
with. Moreover, the experience with mice as well as with
patients like Jennifer LaChance and Tonya Kalesnik, who had
been treated with interferon, indicated that
antiangiogenesis drugs have a slow, cumulative effect,
taking up to a year to eliminate tumors. It stretched the
limits of reasonable expectation to think that the
critically ill patients in the first trials would take a few
injections of low-dosage, slow-acting drugs and waltz out of
their hospital wards, cancer-free.
Obviously, such waltzing wasn't likely. A study that had
recently been done at the Johns Hopkins Medical
Institutions, in Baltimore, showed starkly that very little
about a drug's potential is discernible from the results of
Phase I trials. Because the patients admitted to such trials
are desperately ill, and because the doses of drugs given
are so small, half of the patients fail—they drop out
within 1.8 months, even if the drug being tested ultimately
turns out to be effective. In contrast, in trials of drugs
that turn out to be flops—never making it to the
market—half of the patients drop out by 1.6 months.
Statistically that's almost dead even, and the take-home
lesson is that Phase I toxicity trials generally don't say
much about a candidate drug's ultimate success. Thus, by any
measure, the expectations for Folkman's antiangiogenic
agents were far beyond reason.
 Michael O'Reilly discovered endostatin and
angiostatin.
Michael O'Reilly discovered endostatin and
angiostatin.
|
|
Endostatin on trial
Endostatin, the second of the antiangiogenic agents
discovered by Michael O'Reilly less than half a decade
earlier, was the first to be put to the test, in trials
involving 15 patients at each of three sites: the
Dana-Farber Cancer Institute in Boston, the M.D. Anderson
Cancer Center in Houston, and the University of Wisconsin
Medical Center in Madison. The clinical researchers would
start with very small doses—only 15 milligrams per
kilogram of body weight daily, measures so insignificant
that they were unlikely to have any effect—and then
gradually escalate them to see if there came a point when
the drugs became toxic and should be stopped. The idea was
to see if, and how much, endostatin could be given safely.
If the drug passed that test, proving itself nontoxic, then
the dosages would be increased to levels where they could
begin to be tested for efficacy—to see if they
actually worked against tumors.
Even then, it could be yet another year before the results
were in. Because antiangiogenesis works by shutting down the
growth and migration of blood-vessel cells, it's a far
slower process than poisoning or blasting tumor cells with
radiation or chemotherapy. The tests in mice had made it
clear that the antiangiogenic drugs had to be continued for
a very long time, and that stopping too early would allow
the blood vessels to regrow, reigniting tumor growth. Slow
and steady was the rule. So the first patients selected for
the trials had to wonder how lucky they were: The protocols
of the studies made it unlikely any of the first patients
would be saved by the new drugs.
|
 Studies in mice have shown that, to be effective,
antiangiogenic drugs must be administered for an
extended period.
Studies in mice have shown that, to be effective,
antiangiogenic drugs must be administered for an
extended period.
|
Still patients lined up, brave and desperate people who knew
their chances were worse if they didn't try at all. The
first endostatin trials were scheduled for October 1999 at
Dana-Farber, and as news of that first opportunity got
around, thousands of patients called, wrote, and e-mailed,
frantically hoping to qualify for one of the 30 slots in the
small toxicity test. The same rush happened a few months
later in Wisconsin, and again in Texas, when the two other
Phase I endostatin trials were opened under auspices of the
National Cancer Institute. Most of the applicants were
disappointed. Some patients arrived with complications
beyond cancer, such as high blood pressure or diabetes, or
even the wrong kind of cancer. People with brain tumors, for
example, were excluded because the doctors could not know
whether endostatin might weaken the blood vessels feeding
the brain tumor so much that hemorrhaging into the brain
might occur.
Unlike most clinical trials, in which all the treatment
centers do exactly the same things, the doctors running the
three endostatin trials were allowed to set some of their
own rules, select the kinds of tumors they would treat, and
decide how to enroll their patients. This was because
antiangiogenesis was so new and untested that no one really
knew how to use endostatin. "Since no one knows," explained
Dr. Mark Kieran, director of pediatric neurooncology at
Dana-Farber, "having one person write the protocol would be
very arbitrary."
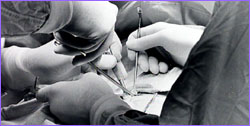 Patients chosen for the endostatin trial had to
have tumors that defied all other treatments,
including surgery.
Patients chosen for the endostatin trial had to
have tumors that defied all other treatments,
including surgery.
|
|
In Boston, patients were selected almost on a first-come,
first-served basis, while in Houston and Madison they were
chosen from among patients who were already under care at
the hospitals. There were only two things patients in all
three trials had to have in common: Their malignancies had
to have defied all previous treatments, and the patients
couldn't be so near death that they might succumb in just a
week or two, before they could be evaluated for signs of
drug toxicity. Such an immediate death would be seen as a
waste of the precious drug while raising serious questions
about why the patient died. Was it the cancer or the drug?
Continue: Watching and Waiting
Dr. Folkman Speaks
|
Cancer Caught on Video
Designing Clinical Trials
|
Accidental Discoveries
| How Cancer Grows
Help/Resources
|
Transcript
|
Site Map
|
Cancer Warrior Home
Editor's Picks
|
Previous Sites
|
Join Us/E-mail
|
TV/Web Schedule
About NOVA |
Teachers |
Site Map
|
Shop |
Jobs |
Search |
To print
PBS Online |
NOVA Online |
WGBH
©
| Updated February 2001
|
|
|