Chasing Heroin
February 23, 2016
1h 54m
A searing, two-hour investigation of America's heroin crisis
Chasing Heroin
February 23, 2016
1h 54m
Share
A searing, two-hour investigation places America’s heroin and opioid crisis in a fresh and provocative light — telling the stories of individual addicts, but also illuminating the epidemic’s years-in-the-making social context, deeply examining shifts in U.S. drug policy, and exploring what happens when addiction is treated like a public health issue, not a crime.
Produced by
Transcript
Credits
Journalistic Standards
Support provided by:
Learn More
Most Watched
The FRONTLINE Newsletter

How the Heroin Epidemic Differs in Communities of Color

How Bad is the Opioid Epidemic?

Heroin and Opioid Addiction, In Your Own Words
Related Stories
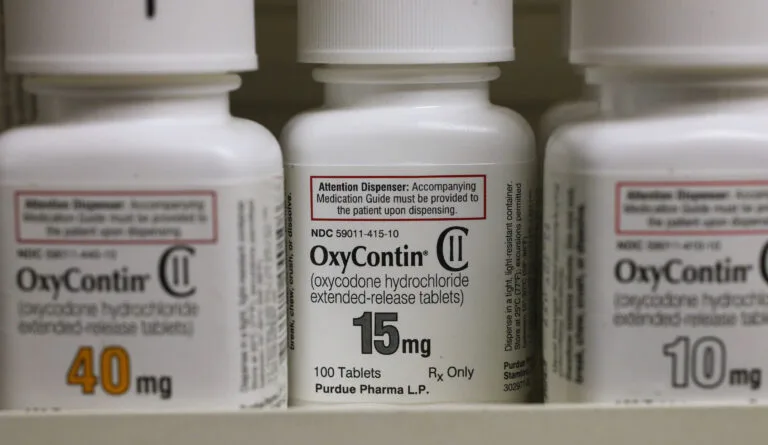
As Purdue Pharma Agrees to Settle with the DOJ, Revisit Its Role in the Opioid Crisis

Revisit Purdue Pharma’s Role in the Opioid Crisis
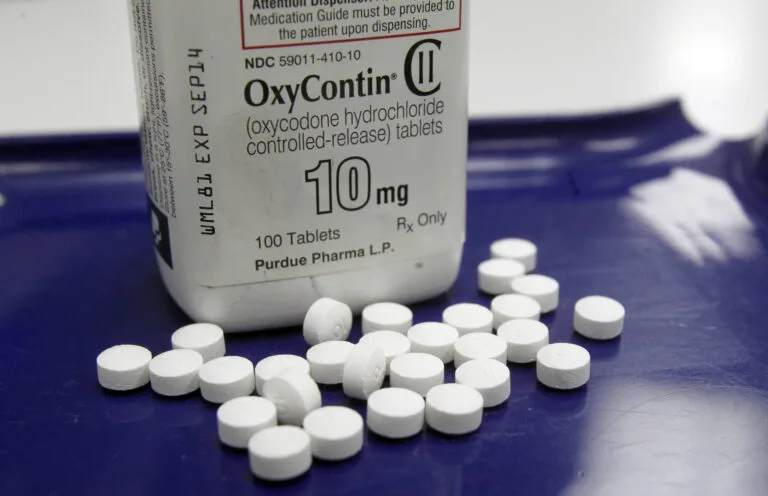
Inside the “Aggressive” Marketing of OxyContin: Revisit Purdue Pharma’s Role in the Opioid Crisis

Can the Death Penalty Actually Stem the Opioid Epidemic?

Opioid Overdoses Are Up Another 30 Percent, CDC Says

Trump’s Opioid Commission Recommends Drug Courts. How Do They Work?

The Opioid Epidemic is Growing More Deadly, New Data Suggests

What It Would Mean To Declare the Opioid Crisis a National Emergency

FRONTLINE Earns Three Peabody Award Nominations
White House Eases Cap on Medication for Opioid Addiction
Veterans Face Greater Risks Amid Opioid Crisis

Heroin and Opioid Addiction, In Your Own Words

Live Chat: Ask Us Your Questions About “Chasing Heroin”
Chasing Heroin

How the Heroin Epidemic Differs in Communities of Color

How Bad is the Opioid Epidemic?

The Options and Obstacles to Treating Heroin Addiction

Eric Holder: If Sentencing Reform Dies, “I’d Be Ashamed”

Drug Czar: Treating Substance Abuse as a Crime is “Inhumane”

How Would the Candidates Fix the Heroin Epidemic?

Watch a Cop’s Surprising Interaction with a Heroin User

Share Your Story About Heroin and Opioid Addiction

Obama Asks for $1.1 Billion to Fight Opioid and Heroin Abuse

Coming in February on FRONTLINE
Related Stories

As Purdue Pharma Agrees to Settle with the DOJ, Revisit Its Role in the Opioid Crisis

Revisit Purdue Pharma’s Role in the Opioid Crisis

Inside the “Aggressive” Marketing of OxyContin: Revisit Purdue Pharma’s Role in the Opioid Crisis

Can the Death Penalty Actually Stem the Opioid Epidemic?

Opioid Overdoses Are Up Another 30 Percent, CDC Says

Trump’s Opioid Commission Recommends Drug Courts. How Do They Work?

The Opioid Epidemic is Growing More Deadly, New Data Suggests

What It Would Mean To Declare the Opioid Crisis a National Emergency

FRONTLINE Earns Three Peabody Award Nominations

White House Eases Cap on Medication for Opioid Addiction

Veterans Face Greater Risks Amid Opioid Crisis

Heroin and Opioid Addiction, In Your Own Words

Live Chat: Ask Us Your Questions About “Chasing Heroin”
Chasing Heroin

How the Heroin Epidemic Differs in Communities of Color

How Bad is the Opioid Epidemic?

The Options and Obstacles to Treating Heroin Addiction

Eric Holder: If Sentencing Reform Dies, “I’d Be Ashamed”

Drug Czar: Treating Substance Abuse as a Crime is “Inhumane”

How Would the Candidates Fix the Heroin Epidemic?

Watch a Cop’s Surprising Interaction with a Heroin User

Share Your Story About Heroin and Opioid Addiction

Obama Asks for $1.1 Billion to Fight Opioid and Heroin Abuse

Coming in February on FRONTLINE
PRODUCED BY
Marcela Gaviria
Will Cohen
COPRODUCER
Brian Funck
CORRESPONDENT
Martin Smith
WRITTEN AND DIRECTED BY
Marcela Gaviria
NEWSCASTER: There are some alarming new numbers out from the CDC showing a dramatic rise in the heroin epidemic.
NEWSCASTER: Painkillers is an expensive habit, many now turning to a cheaper way to chase that high.
NEWSCASTER: The number of heroin overdose deaths nearly quadrupled.
NARRATOR: It’s been creeping up on us for a long time, America’s heroin problem.
NEWSCASTER: The sudden rise in heroin overdoses is occurring in cities big and small.
NARRATOR: Overdoses from heroin and other opioids now kill more than 27,000 people a year. And the numbers keep rising.
NEWSCASTER: Authorities say the drug is increasingly making its way to wealthy suburbs, into the hands of young Americans.
SOCIAL WORKER: In the last 12 months, have you done speedballs?
KRISTINA BLOCK: Yes.
SOCIAL WORKER: Goofballs?
KRISTINA BLOCK: Yes.
SOCIAL WORKER: Heroin by itself?
KRISTINA BLOCK: Yes.
SOCIAL WORKER: Last three months, have you done pain meds— Oxys, Vicodin?
KRISTINA BLOCK: No.
SOCIAL WORKER: And how many times have you overdosed from opiates in your life?
KRISTINA BLOCK: Never.
SOCIAL WORKER: And how many times have you witnessed someone else overdose from opiates?
KRISTINA BLOCK: Three times.
KRISTINA BLOCK: I don’t have a cooker.
FRIEND: I got one.
KRISTINA BLOCK: David took my last cooker.
FRIEND: This isn’t clean.
KRISTINA BLOCK: Dude, I have cleans. Here, that’s clear.
NARRATOR: Kristina Block says she first tried smoking heroin when she was a teenager.
KRISTINA BLOCK: When I was 14, I tried heroin. And it just, like, made everything feel, like, safe and OK.
Did I give you enough cleans?
I think I got really trapped in it because, I mean, I guess I didn’t know too much about what addiction was, and it just became so second nature. It just— it consumed me.
NARRATOR: She moved to injecting by the time she was 16.
KRISTINA BLOCK: I was friends with this girl who was, like, 24. And she was shooting up— like, that’s how she did it. And I just was kind of interested in it and I asked her to hit me one time.
NARRATOR: Kristina is now seven years into her addiction.
KRISTINA BLOCK: It’s just so insane what this drug, like, can— can make you do. Like, it literally has a brain. And it shares mine, you know?
MARCELA GAVIRIA, Producer: Right now, how much heroin is in your system?
KRISTINA BLOCK: Probably, like, $40 worth.
MARCELA GAVIRIA: So what determines how much you use?
KRISTINA BLOCK: Well, the number one thing that determines how much I use is how much money I have, or how much dope I have.
NARRATOR: There are many different reasons why people turn to heroin. Four years ago, Johnny Bousquet, 38, says he started using to cope with the breakup of his marriage.
JOHNNY BOUSQUET: I felt like it alleviated the pain that I was going through. It just made me feel like I can make it through that moment. And then eventually, I needed it to get through every moment.
NARRATOR: Johnny’s mother was also a heroin addict. She was gone by the time he was 19.
JOHNNY BOUSQUET: One day, me and my sister, we found her dead in her room with a needle in her arm. She lost her battle with heroin then. I know she loved us and I know she really cared about us. And I would always wonder if she loved heroin more than she loved us.
NARRATOR: He’s now living in a homeless shelter and struggling to stay clean.
JOHNNY BOUSQUET: At least a few times a day, I think, “Man, it would be a really good time to get loaded right now.” You know, you can pull through and be OK, or even just get a little bit high. That’ll be fine. And then something else takes over. And then next thing you know, it’s two days later.
I’ve just been, like, fighting that, you know? I can’t seem to get a hold of myself no matter how hard I try.
MARTIN SMITH, Correspondent: How does the street look to you tonight?
MIKEL KOWALCYK, Outreach Coordinator, LEAD: Right here, it’s pretty quiet. When we turn the corner, it might be different.
Are you taking a right, Felix?
OFC. FELIX REYES, SPD: Yes.
MIKEL KOWALCYK: OK.
NARRATOR: As the heroin epidemic has spread, cities and states have grown desperate to come up with solutions. Here in Seattle, beat cops are four years into a radical experiment to deal with drug use on their streets.
OFC. FELIX REYES, SPD: Oh, [expletive deleted] the cops! Hate that! Do me a favor. Do me a favor! Stop moving. Stop moving. OK, good, because when you’re moving, I don’t know what you’re doing. I get— Oh! And when you stop moving, I got you. You’re getting well. Not a big deal. All right, I’m not going to jam you up. I just— you know, we got to find out who you are, OK? Cool.
Lt. LESLIE MILLS: The girl on the ground just is getting well. She’s shooting heroin.
Stop crying, babe. We don’t care.
NARRATOR: These officers are making fewer arrests. They are more likely to refer addicts they encounter to social services.
Lt. LESLIE MILLS: Where’s the syringe? Because I want to be safe.
MARTIN SMITH: So you’ve become a social worker.
Lt. LESLIE MILLS: We are social workers.
MARTIN SMITH: You are social workers.
Lt. LESLIE MILLS: Yeah.
MARTIN SMITH: But a viewer—
Lt. LESLIE MILLS: But yeah, how many—
MARTIN SMITH: —listening to you now would say, “Gee, you’re taking an awfully,” you know—
Lt. LESLIE MILLS: Bleeding heart.
MARTIN SMITH: —“gentle approach.”
Lt. LESLIE MILLS: We could not incarcerate these people or arrest our way out of the problem. You would arrest a person, they’d be in jail for 20 or 30 days. They would get sober. They would start using again. We continued to arrest them. And then they would use, and continue to arrest.
Lt. LESLIE MILLS: How much do you use a day?
GIRL: Like, $5.
Lt. LESLIE MILLS: OK. And how long have you been using?
GIRL: I just got out of jail!
Lt. LESLIE MILLS: I’m not putting you in jail. Are you a meth user too?
GIRL: No.
Lt. LESLIE MILLS: Do you have any desire to get on methadone and get well or—
GIRL: That’s what I’m trying to do.
Lt. LESLIE MILLS: If you have a problem, come and see me at this office. I’ll give you something to eat. I’ll let you call your parents. We’ll sit down and we’ll have a talk. Are you— do you still need that cooker?
GIRL: Yeah.
Lt. LESLIE MILLS: OK.
NARRATOR: The most recent surge of heroin abuse has altered our approach to addiction and our views on the war on drugs.
POLICE RADIO: We got a 31-year-old male. He’s unconscious, breathing.
SAM QUINONES, Author, Dreamland: Cops and prosecutors and epidemiologists, public health nurses, county coroners— all of this is being fought by really anonymous folks all across the country because this epidemic is also the quietest epidemic. It’s filled with shame.
EMT: Obvious overdose, known history of heroin use. Admitted using heroin today. He was found unconscious. They kind of roused him. They’re going to start an IV on him.
SAM QUINONES: You don’t have a lot of violence. People die alone in a McDonald’s bathroom toilet. And then when the people die, when the kids die, the parents are so mortified, so ashamed that they keep quiet, too. And the thing is left to perpetuate and spread.
NARRATOR: How did this epidemic begin? It’s a crisis 30 years in the making.
NEWSCASTER: Bottom line, so many Americans are suffering from too much pain, and doctors aren’t doing enough to stop it.
BARRY MEIER, Author, Pain Killer: In this country, there was a long-running puritanical attitude towards pain, and it resulted in almost a barbaric under-treatment of pain, particularly when it came to people with cancer and in the terminal stages of cancer.
Prof. SCOTT BURRIS, Dir., Temple Univ. Center for Health Law: There had to be better treatment for people in serious pain. So there was a whole effort to open up minds, to allow hospice care and good pain management for people with cancer. And then that spread into AIDS because people with AIDS often had very serious pain problems.
NARRATOR: Doctors had long avoided prescribing opioid painkillers for fear of addicting their patients. That changed with the emergence of the hospice movement.
BARRY MEIER: That movement collides with an opportunistic drug company in the form of Purdue Pharma. They see the opportunity to expand the use of these drugs beyond the cancer wards, kind of into the mainstream of medicine. And the drug that becomes the vehicle through which they do that is a drug called OxyContin.
NEWSCASTER: OxyContin is one of America’s new prescription wonder drugs. It’s a powerful painkiller—
KATHERINE EBAN, Fortune: OxyContin was not really a new drug. The molecule had been around since 1916. What they did is they took this old, existing drug and they introduced a time-release mechanism into it so that it would be significantly less addictive because it wouldn’t be released up front all at once. That’s how they pitched it to the FDA.
SAM QUINONES: Purdue Pharma marketed it to doctors who were prescribing drugs for all manner of ailments to common, ordinary folks who were not dying of cancer. To them, OxyContin initially looked like a godsend. It looked like this wonder drug. Like, all of a sudden, we can give this, and we don’t need to prescribe eight Vicodin a day.
BARRY MEIER: There is no question that the marketing of OxyContin was the most aggressive marketing of a narcotic drug ever undertaken by a pharmaceutical producer. The FDA allowed them to make the claim that because it was a long-acting drug, it might — the stress being on the word “might” — be less prone to addiction and abuse than traditional drugs.
There was absolutely no science to support this idea, zero.
ANNOUNCER: [Purdue Pharma video] The under-treatment of pain is a major public health problem—
NARRATOR: To urge doctors to treat pain more aggressively, Purdue Pharma launched a series of promotional videos.
[Purdue Pharma video]
1st PAIN PATIENT: The pain that I have basically covers my neck to my feet.
ANNOUNCER: Thirty-four million adults suffer from chronic pain.
NARRATOR: The company used prominent pain specialists, like Dr. Russell Portenoy, to ease concerns about addiction.
[Purdue Pharma video]
Dr. RUSSELL PORTENOY: The likelihood that the treatment of pain using an opioid drug which is prescribed by a doctor will lead to addiction is extremely low.
ANNOUNCER: Opioids are safe and effective—
ANDREW KOLODNY, M.D., Chief Medical Officer, Phoenix House: The message in these programs was that real addiction in your patients treated with opioids is exceptionally rare.
PURDUE SPOKESPERSON: Less than 1 percent of patients taking—
Prof. KEITH HUMPHREYS, Ph.D., Stanford University: Purdue Pharma managed to persuade a lot of good people in medicine that they needed to dramatically up their prescriptions of opioids. Now, part of the reason they were able to do that is that there was clear evidence there were some people in pain who didn’t need to be in pain, and we had underused them. There’s no doubt about that. But it’s also no doubt about it that they were commercially driven.
NARRATOR: By 2001, Purdue was selling more than $1 billion worth of OxyContin a year. Prescriptions for other opioids soared, too, for drugs like Percocet and Vicodin.
SAM QUINONES: We went from a country that used almost no opiate painkillers, like in the ‘50s and ‘60s, to being a country where we used 83 percent of the world’s oxycodone, and almost 98 percent of the world’s hydrocodone. It’s night and day. It’s a stunning statistic.
NARRATOR: Most of the users were white men and women living in towns and suburbs. Cari Creasia, a stay-at-home mom living in Kent, Washington, was prescribed Vicodin after the birth of her second child. When her prescription ran out, she wanted more.
CARI CREASIA: I just pursued it. I went to a doctor and I made up an ailment. I said, “I have terrible migraine headaches.” In order to get more, I got on the phone the next day and said, “This one’s not working. I think I’m allergic to it.” “OK. Are you sure? We’ll prescribe something different.” Before all was said and done with this doctor, he was prescribing me 3 to 400 pills per month.
PROMOTIONAL WEB VIDEO: Highly-regarded by his patients, they rate him 3.5 out of 4 stars—
NARRATOR: Her prescribing physician was a doctor with top credentials.
PROMOTIONAL WEB VIDEO: He has won a number of awards—
CARI CREASIA: He was a young doctor. I think he was fairly new in the field, early 30s. For a couple of years, it worked. He never once said, “This is a problem.”
NARRATOR: No one in her family seemed to notice.
CAROLYN CREASIA, Cari’s Daughter: She still was functional. She would still have the facade of looking like she was completely together, like the poster child PTA, you know, mom that everybody looked up to and everybody wanted to be.
NARRATOR: During that period of her life, she says she was consuming around 15 to 20 painkillers a day.
CARI CREASIA: It felt that good to me. And it made me feel that comfortable in my own skin. I felt like I was a better mom, a better person, easier to be around. It made me feel like I was functioning on a higher level.
NARRATOR: The supply from her doctor remained steady for the next two years. But then one day, Cari ran out of pills.
CARI CREASIA: He was on vacation. Nobody ever told me, “Now that you’re taking these pills, you can’t just stop. You’re going to get ill.” And getting sick was kind of like truth serum for me. It made me want to talk. It made want to reach out. So I asked my ex-husband to help me.
NARRATOR: Cari’s husband confronted her doctor about the dozens of bottles of painkillers he had prescribed.
CARI CREASIA: He said, “I thought she was smarter than that. You’re going to have to wean her. He scolded me. I left there feeling rather shamed and like I had done him wrong.
NARRATOR: Cari promised to stop, to go cold turkey, but she couldn’t.
CARI CREASIA: I began seeking pills in various ways. And it started with going through people’s medicine cabinets, the neighbors, people from church, family members, grandparents.
I even went to real estate open houses and then asked to use the bathroom to obtain pills and I’d call in refills on these medications, calling these automated lines at Walgreen’s, posing as the nurse from this doctor’s office, “Please refill this,” go through the drive through and pick it up. “I’m so-and-so’s daughter or friend and she’s sick. I have to pick up her script.” No questions asked.
NARRATOR: After two years of stealing other people’s prescriptions, one morning she ran into trouble at Walgreen’s.
CARI CREASIA: I went to the drive-up window and the pharmacist said, “This isn’t your script. We called the doctor. This is fraudulent.” He called the police. They came to the house. “Do you have small children here? Well, put them on the computer downstairs. We’re not going to arrest you if you’ll go and turn yourself in.”
So my neighbor and friend drove me down to the police station. And that became a deferred prosecution. And as a result of that, I went into in-patient treatment.
NEWSCASTER: More and more Americans are ending up in the hospital after overdosing on prescription drugs.
NARRATOR: It was a time when the country was waking up to the opioid crisis.
NEWSCASTER: A national epidemic of pill popping so bad, it’s being called “pharmageddon.”
NEWSCASTER: OxyContin was once marketed as something of a wonder drug, one that could stop pain without getting patients addicted. As it turns out, that was a lie, and deliberate one.
NARRATOR: In 2007, after a four-year investigation by federal prosecutors, Purdue Pharma admitted to charges of fraudulent marketing.
NEWSCASTER: The executives conceded they ignored widespread reports of deaths and addictions.
NARRATOR: The company paid $600 million in fines and settlements.
NEWSCASTER: —admitted they misled the public—
NARRATOR: In a statement, Purdue Pharma said they accepted responsibility, and most significantly, reformulated OxyContin with abuse-deterrent properties. Their most prominent medical consultant, Dr. Portenoy, publicly expressed regret.
By 2009, a newly appointed team at the Office of National Drug Control Policy was coming to grips with the magnitude of the opioid crisis.
KEITH HUMPHREYS, Ph.D., Office of Natl. Drug Control Policy, 2009-10: You know, all you had to do, really, was pick up the paper and just see every day, you know, there was a story about, you know, people dying, or you know, doctors getting arrested for running pill mills, those kinds of things.
NEWSCASTER: —shady pain clinics that will prescribe just about anything for a price—
NARRATOR: The new deputy drug czar, Dr. Tom McLellan, was poring over data on overdoses, but it was outdated.
TOM McLELLAN, Ph.D., Dpty. Dir., Office of Natl. Drug Control Policy, 2009-10: One of the problems is you don’t get the results of opiate overdose for three years. There’s a lag of two years. So it’s like driving by looking in the rear-view mirror, OK?
MARTIN SMITH, Correspondent: So you knew that there was a rise in the prescription rates.
TOM McLELLAN: Oh, yeah. But we didn’t realize that the statistics had already started to really go way, way up.
NARRATOR: At the Centers for Disease Control, director Tom Frieden was looking at health data for the whole country.
TOM FRIEDEN, M.D., Director, CDC: I was just stunned. The only thing that was getting worse was deaths from opiates. Everything else was getting better. But then I began looking through the whole of the Centers for Disease Control and Prevention, and I was seeing the impact of opiates everywhere— birth defects, neonatal abstinence syndrome, hepatitis-C and HIV. This is an unusual and horrific phenomenon.
Dr. TOM FRIEDEN: It’s an emerging problem.
NARRATOR: Frieden started raising the alarm.
Dr. TOM FRIEDEN: —a substantial increase in fatal overdoses, and we need to get a much better handle on it.
NARRATOR: One day in the spring of 2010, Frieden approached an official at the drug czar’s office, Dr. Keith Humphreys.
KEITH HUMPHREYS: We meet privately. And he says, “You guys in the White House need to start using the word ‘epidemic’ for opioids. This is an epidemic. Look at all these people dying. This is like the early parts of AIDS. We need to really ramp up concern about this. This is killing lots of people.”
NARRATOR: The team at the Office of National Drug Control Policy decided it was time to get President Obama’s attention.
TOM McLELLAN: We said that it was going to be an even bigger problem.
MARTIN SMITH: Did you see that that was going to lead to a rise in heroin addiction?
TOM McLELLAN: Oh, yeah. I mean, prescription opiates is heroin prep school. The inevitable thing is going to be a reduction in the availability of those. Once that happens, you have to turn to something. And that is going to be high-potency street opiates, heroin.
MARTIN SMITH: And did you take those warnings to the— to the White House?
TOM McLELLAN: Yes, we did.
MARTIN SMITH: And?
TOM McLELLAN: “Thank you for sharing.” I mean, they’re— they get warnings all the time about dire things that are— that are going to happen. Some happen, some don’t.
It was not the main thing for the Obama administration. They had a few other tiny little problems like the Affordable Care Act, America still reeling from the bank collapse and real estate collapse and all that. Little things.
NEWSCASTER: —push to stop a real epidemic of prescription painkiller abuse—
NARRATOR: One year later, the White House called for more prescriber education and additional prescription monitoring.
NEWSCASTER: —prescribing fewer pills at one time—
NARRATOR: By that time, doctors were writing enough prescriptions a year to give a bottle of painkillers to every American adult.
NEWSCASTER: —medications like Percocet, Vicodin, oxycodone—
NARRATOR: As for Cari, despite a stint in rehab, she couldn’t shake her addiction. Ten years after she first got hooked on opioids, she moved out of her house, leaving her husband and two kids.
She eventually started a new relationship and began a new life. But then one day, she ran into an old friend from high school.
CARI CREASIA: I said, “I’m in recovery.” That’s how we started talking. She says, “I’m supposed to be, too. Maybe we should talk sometime.” So I went to her house to talk. And instead of having coffee, we smoked a bowl of meth because that was her drug of choice. And it went from there.
NARRATOR: Cari’s addiction was slowly progressing. She would start abusing meth, but would return to opioids.
CARI CREASIA: At the bus stop one day, I started talking to a gentleman and brought it up. “I’m looking for opiates.” “Well, I’ve got something for you.” Walked over to the— to the honey pot, you know, the green temporary bathrooms at construction sites. I went in there to do it. I came out. “Did you like it?” “I loved it. Get me some more.” So he did.
NARRATOR: Cari, like some opioid addicts, had moved on to street heroin. It wasn’t long before she began living in this house, now renovated, with 20 other addicts.
CARI CREASIA: And I wound up living in a house down at the bottom of the hill. Oh, man! The animals weren’t taken outside to relieve themselves. We were living with animal feces. It was a very filthy environment. And before long, that was my home.
CAROLYN CREASIA, Cari’s Daughter: It was gross. It was never like a place I’ve ever been before. And I was seeing people pretty much overdosing in other rooms. It was, like, people’s eyes rolling in the back of their heads.
And it was shocking to me because she would just act as if that wasn’t happening when she was hanging out with me. Like, “How’s your day been,“ you know? And this was the point where I was, like, “You’re not even trying anymore. You’re not even— you’re not even trying to pretend that this isn’t happening anymore.
CARI CREASIA: Addiction is weird. It gets very weird. During that time, I lost it all. And it really didn’t matter to me. As long as I could get high, it was OK.
NEWSCASTER: A heroin boom—
NEWSCASTER: I have never seen the amount of heroin that’s on the streets of America today—
NEWSCASTER: The Mexican drug cartels are flooding the U.S. with cheap heroin—
NARRATOR: As painkillers opened the way for heroin, Mexican drug suppliers were ready.
NEWSCASTER: —moving narcotics across the border—
NARRATOR: They would take the epidemic to a whole new level, bringing cheap and highly addictive heroin to towns and suburbs across America.
SAM QUINONES, Author, Dreamland: They’re selling heroin as if it were pizza. They were the first drug-trafficking group to understand that the pill market was essentially priming the heroin market.
NEWSCASTER: A quiet, unsuspecting neighborhood was the perfect cover for a cartel—
SAM QUINONES: Wherever there was a town that had a lot of pill users, they would set up a store there. They call them stores.
NEWSCASTER: A multi-billion-dollar drug empire—
SAM QUINONES: What you need is a large community of pretty well-to-do kids with money to buy the dope, with cell phones to call the dealer, with cars to go get the dope, and private bedrooms to shoot it up.
NARRATOR: Teenagers in middle class and wealthy suburbs now had easy access to black tar heroin, kids like Marah Williams.
PENNY LEGATE, Marah’s Mother: Marah was a born athlete. By the time she was about 13 or 14, she could throw a pitch about 65 miles an hour.
MIKE WILLIAMS, Marah’s Father: One pitching instructor that had for a while named her “The Rocket.” Everybody knew who Marah Williams was. Everyone.
NARRATOR: Marah appeared to have the happiest of childhoods, full of privileges— ballet lessons, piano, a close-knit family.
PENNY LEGATE: Her early childhood was just ideal. We lived in a beautiful bedroom community in Seattle. I had a great job. We were a very tight foursome, my husband and I and our two children. It was a great middle America life, very happy.
NARRATOR: Her mother was a local news anchor. Her father was a stay-at-home dad who doted on his girls.
MIKE WILLIAMS: [home video] When did you learn to do that, Marah?
Our children went to good schools. The neighborhood was safe. We never locked the door. Marah was a very happy child.
NARRATOR: But by the time she reached middle school, Marah was struggling.
PENNY LEGATE: A lot of anxiety, a lot of depression. By this time, she’d been diagnosed with ADHD. It was clear she had some eating disorders issues. We were just trying to find the right mix of therapy, meds.
Sister: [home video] Marah, how old are you this year?
MARAH WILLIAMS: Thirteen!
NARRATOR: Marah was also self-medicating.
MIKE WILLIAMS: What happened a couple days before Christmas?
MARAH WILLIAMS: I snuck out and drank alcohol. And then I slept at a boy’s house.
PENNY LEGATE: She started experimenting with marijuana and alcohol. So I always kind of kept a close eye. I was looking under the bed. Are there bottles? I don’t know, I was always looking.
Sister: [home video] Careful! Don’t fall on the tree!
PENNY LEGATE: I think I was making her bed or something, and I found a locket. And I opened it. I thought, “Oh, this is interesting.” And out poured white powder. It was cocaine.
NARRATOR: They found a highly regarded treatment center out of state that cost them $40,000 out of pocket. The program they chose followed a model of strict abstinence. Marah spent 90 days in intensive rehab, three times longer than the average patient stay.
PENNY LEGATE: We didn’t think 90 days was going to be long enough, but we chose the best place we thought we could for her, where she’d have the best chance of success.
FAMILY: [home video] Happy birthday to you, happy birthday to you—
PENNY LEGATE: She was clean for a while. She looked good. She looked healthy. She seemed determined to live more responsibly. And for a long time, she did pretty well. But this is the thing about treatment, it’s not a magic bullet.
NARRATOR: The program didn’t work. A few months after Marah got out, she started using OxyContin. Her mother found out after Marah was caught stealing pills. But that was only the beginning. One day, Marah’s father got a call.
MIKE WILLIAMS: I was at work one day, and I had one of her friends’ fathers calling me frantically. And he said, “My daughter and your daughter were using heroin.”
PENNY LEGATE: She was a junior in high school, and she was caught in the bathroom cooking heroin. And I was, like, “Oh, my God.” I had no idea it had gone to heroin. So when we talked to her about it, she didn’t deny it. She goes, “I’m in trouble. I need help.” She says, “Can I go to detox tonight?”
NARRATOR: After another 30 days in rehab, Marah came out finally ready to embrace sobriety. She went to AA meetings regularly, worked hard at school and delighted her family when she finally graduated from high school.
MARAH WILLIAMS: I’m Marah. And first off, I got to thank you guys. I definitely wouldn’t be here without you, and you guys gave me a fourth chance. And I’m really, really, incredibly grateful to you guys. Thank you. And my beautiful family. Look at all of them hanging out! I love you guys. [applause] Thanks for showing up, guys. I’m sorry about all the crap I put you through. [laughter]
GRADUATION ANNOUNCER: Marah Williams.
AUDIENCE: Whoo-hoo! [applause]
NARRATOR: At one of her AA meetings, she met someone.
JORDAN ZULAUF: She just kind of knocked me off my feet when— when I first saw her, you know? She just had this— this thing about her that some people have. And she was able to get through my barriers, you know?
NARRATOR: Jordan Zulauf was just back from his third tour in Iraq and was trying to kick his addiction to heroin.
JORDAN ZULAUF: We’re both into metal music, punk music, you know, activism. We’re just really like-minded in that way and just kind of goofballs together. We just had a good time. We were both sober and living that life, and it’s, like, at the forefront of our relationship and what we did. You know, a lot of it was based around that, being sober and being healthy and proactive.
PENNY LEGATE: They were both in AA. They were working their AA program together, going religiously, working the 12 steps. She’d say, “I really like sobriety. I like the way I feel. I can’t believe how clean and clear my brain is.” She was just doing a great, great job. She was doing a great job.
NARRATOR: But heroin is considered one of the most addictive drugs. Up to 60 percent of addicts relapse in the first year after treatment. Marah managed to stay off for a year-and-a-half.
JORDAN ZULAUF: Penny told me— she’s, like, “I think Marah’s using again.” I was, like, “There’s no way. There’s no— there’s no way that could be happening,” you know? I didn’t believe it. And then I asked her, she’s, like, “Yeah, I did once,” you know what I mean? But I’m, like, “But you’re not continuing to do that. We’re going to— you’re going to get help and we’re going to deal with this, right?”
NARRATOR: Six months later, Marah was dead.
PENNY LEGATE: Found the needle in the sink, the water running, and her dead on the floor. Had to have happened really fast.
JORDAN ZULAUF: She was clean for a long time, and you know, and then— and that’s what happens. You pick up again and take a hot shot, and that’s that, you know? It’s too much and you die. It happens all the time, you know? She was an amazing girl. I love her very much.
MARCELA GAVIRIA, Producer: How do you remember her?
JORDAN ZULAUF: As a big part of my soul and my heart. She’s always there, you know? Yeah. And a grenade, you know? [laughs] She was an explosive person, you know?
NEWSCASTER: Long-time Seattle media figure Penny Legate did everything she could to help her daughter break the grip of heroin.
NEWSCASTER: —former local high school football player who became addicted to heroin—
NEWSCASTER: Another local family buried a teenage daughter today, another heroin overdose.
NEWSCASTER: Her son was an Eagle Scout on a pre-med scholarship—
Prof. SCOTT BURRIS, Dir., Temple Univ. Center for Health Law: When people started to overdose, the group that got hit pretty hard were young people, college kids, white kids, high school kids. Kids in suburbs were dying of this, not the sort of stereotypical heroin user.
NEWSCASTER: —always at the top of her class, she became addicted to heroin—
NEWSCASTER: —two young people found dead of an overdose—
NARRATOR: Ninety percent of new heroin users are white. A rising number are middle-class or wealthy.
Prof. SCOTT BURRIS: Because the stereotypes turn out to be so very important to people’s attitudes towards drug use and the war on drugs and drug users, this has been a really huge development.
CARLY FIORINA (R), Fmr. Presidential Candidate: Drug addiction is an epidemic. And it is taking too many of our young people.
Gov. CHRIS CHRISTIE (R-NJ), PRESIDENTIAL CANDIDATE: We have a huge problem, and I think the big reason is because we’re not treating it like the disease that it is.
KEITH HUMPHREYS: It’s been true throughout American history that when drugs penetrate into the middle class, particularly the white middle class, politicians panic much more they do when the drugs are concentrated in poor neighborhoods. And it’s not fair and it’s not right, but that’s the kind of country that we’re living in.
HILLARY CLINTON (D-NY), PRESIDENTIAL CANDIDATE: We need much more in the way of treatment and—
ERIC HOLDER, U.S. Attorney General, 2009-15: It’s heartening for me to see how this nation has reacted to the heroin problem we’re now seeing around the country, where we are coming up with public health responses to it and dealing with the underlying problems that caused that addiction in the first place.
MARTIN SMITH: Not to be too glib, but isn’t that because a lot of white kids are doing heroin?
ERIC HOLDER: I mean, I think that’s certainly a factor, you know—
MARTIN SMITH: Richard Pryor said about cocaine that it’s an epidemic now because white people are doing it.
ERIC HOLDER: Well, you know, when things seep into the majority community, the nation pays a greater amount of attention than when it is confined to minority communities. And so, yeah, there’s an element of truth— there’s an element of truth to that.
NARRATOR: One community hit hard by this new heroin epidemic gripping the nation is a short ferry ride from Seattle, Bremerton. It’s the kind of place where the epidemic too hold early on, a working-class town, home to 40,000 residents, a Navy shipyard, and a mayor who decided to try a different approach to the epidemic.
PATTY LENT, Mayor, Bremerton, WA: Make sure it doesn’t become an eyesore—
NARRATOR: It all began when Mayor Patty Lent received some alarming news. The town’s bathrooms were clogging up with used needles.
Mayor PATTY LENT: We had to install sharps containers at all of our public buildings. We’re trying to keep those syringes from getting into our parks, on our streets and in our landfill.
JOSH FARLEY, Reporter, Kitsap Sun: It was like a wave of heroin. I mean, we just started to see it wash over this county.
ROBERT PARKER, Local Business Owner: You couldn’t walk down streets in Bremerton without finding hypodermic needles laying in the gutters and laying in the parks and on the children’s equipment. And it was kind of shocking for everybody. It used to be nobody knew somebody that was on heroin. Then all of a sudden, I knew 50 people that had an issue with heroin.
NARRATOR: Trevor Mercer, a Bremerton native, says he began using painkillers when he was 18 and moved to heroin because it was that much stronger.
TREVOR MERCER: When I first started doing heroin, I was already taking pills, and I knew it was the same thing. An opiate is an opiate, you know? I was just smoking it at first. Wasn’t until I injected it that I realized why heroin is better than taking a pill. And by better, I mean worse.
NARRATOR: But when his girlfriend got pregnant with their first child, he decided he needed to find a way out. He had already tried to quit, and it hadn’t worked.
TREVOR MERCER: I went through the 12 step program, and everything like that. It’s just not worked for me. So I knew I needed to do something because I certainly couldn’t take care of myself. How am I supposed to take care of somebody else? And getting on the methadone clinic kind of just fell into my lap, and so I figured I’d give it a shot.
NARRATOR: But finding a nearby methadone clinic was another story. Trevor would have to wake up at 3:45 AM to drive to the nearest clinic and get back to work by 7:30.
TREVOR MERCER: The thing with methadone is you take it once a day, instead of doing heroin, like, five or six times a day. It’s certainly worked in my favor ever since. It’s been a long time since I’ve even seen a syringe.
NARRATOR: Methadone is a tightly restricted drug. It was originally formulated as a painkiller, but it was embraced in the 1970s as an effective way to treat heroin users in withdrawal.
SCOTT LINDQUIST, M.D., Health Director, Kitsap County, 2001-14: Every physician can prescribe methadone for pain. They cannot prescribe it for addiction medicine. That’s what methadone clinics can do. The concept is, if you walk into a methadone clinic, you get your dose for the day, so you don’t go into withdrawal. You can go to work. You can achieve your daily functions. And you’re not out doing things like stealing or prostitution of yourself just to earn the next hit.
NARRATOR: Dr. Scott Lindquist was the head of public health for Kitsap County. Alarmed by the growing epidemic, he approached the mayor about starting a clinic.
Mayor PATTY LENT: He told me that people were living normal lives by having a treatment that they had to go in and have it administered. He said it was anyone that had a normal life that had gone through an addiction to heroin. I think I didn’t realize how much controversy would be generated. I didn’t look at any other unintended consequences. So we moved forward in that capacity.
NARRATOR: Robert Parker, who owned a shop in the area, woke up one morning to the headline in the local paper.
ROBERT PARKER: “Methadone clinic coming to Bremerton.” And I went, “What? Wait a minute! We can’t put in a facility that’s selling meth or giving meth out.”
NARRATOR: Josh Farley, a reporter at The Kitsap Sun, wrote the article.
JOSH FARLEY: For a lot of people, it’s really hard to wrap your mind around words like opiate and methadone maintenance. And then the very base of the word “methadone” I think probably confused some people thinking that it’s methamphetamine.
Mayor PATTY LENT: And then the telephone starting ringing, my email, people coming to my office. And they were there in droves.
NARRATOR: The most vocal were shop owners next to the proposed site. One day, the owner of a gas station approached Robert Parker.
ROBERT PARKER: He said, “Look,” he said, “they’re not telling you the truth.” He said, “I own two gas stations in Seattle. They’re right next to methadone clinics.” He said, “These things are destroying our neighborhoods over there, and the police can’t get it under control right now.” He said, “I invite you to come over to Seattle for a day,” and he says, “and let’s go visit.”
And I did. And I spent the entire day photographing what was happening. We had a lot of drug-addicted people that were just kind of hanging out. There were taxis coming from all over the region at the taxpayers’ expense. It was absolutely shocking.
BREMERTON RESIDENT: Good evening, City Council. Good evening, Mayor Lent.
NARRATOR: When the city council held hearings to discuss the matter, dozens of people came to express one idea— “Not in my back yard.”
BREMERTON RESIDENT: I come before you tonight to stand strongly opposed for this methadone clinic coming in—
BREMERTON RESIDENT: My main concern is the safety—
BREMERTON RESIDENT: —loitering, theft, vehicle prowl—
Mayor PATTY LENT: They came to all the council meetings and they said, “Not just not in my back yard, but this is the worst place that you could ever have a methadone clinic.”
BREMERTON RESIDENT: I don’t lack empathy for people that need treatment, but I am concerned about the impact—
BREMERTON RESIDENT: —bars on my windows and more security—
BREMERTON RESIDENT: —a lot of overdoses from methadone clinics—
SCOTT LINDQUIST: Fear trumps science most of the time. And it’s easy to be scientific, but when you’re scared, how easy is it, really, to listen to that science?
COUNCILMAN: Good evening. Welcome to the Bremerton City Council meeting for Wednesday—
NARRATOR: And it went on for months. Even the location, in Bremerton’s red light district, was not acceptable to the community.
BREMERTON RESIDENT: I would not put it in the middle of a problem area, where you have easy access to drugs, prostitution, bars, sex shops—
TREVOR MERCER: I thought it was kind of funny because we’re talking about a block with sex shops, porno theaters, you know, late night bars. But I also wanted to say that, you know, I’m— I’m a human, and I’m normal enough. I have a family. I do probably the same stuff they do.
COUNCILMAN: Anybody have any other comments? Anybody really feel the need—
NARRATOR: Trevor Mercer felt compelled to testify.
TREVOR MERCER: Hi. My name’s Trevor Mercer. Ever since I’ve been on methadone, I’ve come farther in life. I own my own home. I raise my son. I don’t have any issues anymore as far as going backwards. Methadone treatment is what helped.
1st COUNCILMAN: Thank you.
2nd COUNCILMAN: Thank you, Mr. Mercer.
NARRATOR: But the loudest voice against the clinic was having second thoughts by the time he testified.
ROBERT PARKER: When the thing hit the front paper, I was upset, and admittedly now, I didn’t understand the whole issue, and I think we’ve all—
NARRATOR: Robert Parker was dealing with a crisis in his own home. His son was slipping into drug addiction.
ROBERT PARKER: It tore through our family. You know, the first few times, we went running down to the jail, paid whatever the bail was. But it got worse and he slid down further. And finally, when we wouldn’t bail him out anymore, we lost him. He quit communicating with us completely.
I was extremely conflicted about the clinic. I had my son, and at that point, I knew that he may be one of the patients that needed it.
COUNCILMAN: I will call to order the special meeting of the Bremerton City Council—
NARRATOR: Despite his reservations, it was too late. The long campaign against the clinic had swayed Bremerton’s council. In 2011, the council put a halt to the methadone clinic.
Meanwhile, the epidemic continued to spread.
Mayor PATTY LENT: The epidemic today is so much greater than it was back then. The degree today that we have drug addiction is more than I ever anticipated.
JOSH FARLEY, Reporter, Kitsap Sun: You have people who are hooked and they have no option for treatment. Like in many communities, we see the same people go in and out of jail. There is little that we seem to do as a society to eliminate that revolving door. And I see people who— who have died because of this.
ROBERT PARKER: There was a cost to that fight. We lost the methadone clinic, which this community needs. What we didn’t have, and we got the hard way, was the education along the line. And it’s been a hard lesson for all of us.
NARRATOR: Since the city council decided against the methadone clinic, more than 40 people have died of overdoses in Kitsap County.
NEWSCASTER: There are nearly 200,000 inmates in federal prisons, and almost half are drug offenders.
NEWSCASTER: —non-violent offenders sentenced for drug crimes—
NEWSCASTER: That’s 1 in 110 adults behind bars—
NARRATOR: For many heroin addicts, rehab begins not in a methadone clinic but in a county courthouse. One in three people referred to drug treatment come in through the criminal justice system.
PROSECUTOR: Judge, Mr. Green is in custody. The state has no objection—
NARRATOR: Drug courts first appeared in the 1980s as a way to divert low-level drug offenders away from jail and into treatment. The idea caught on.
PROSECUTOR: Three months in a row, the defendant has come into contact with law enforcement with his drug use—
ROBERT DuPONT, M.D., Dir., Natl. Institute on Drug Abuse, 1973-78: We have a system that identifies the drug use as a problem and that requires them to stop. And drug courts do a wonderful job. You don’t just refer them to treatment, you require them to go to treatment. You got to use that stick to get people in there and get them to stay there so they get well.
JAMIE KVISTAD, Drug Court Public Defender: Mr. Holmes is here to ask for another chance—
NARRATOR: The program is designed to closely supervise participants, who must submit to frequent drug tests and intensive drug therapy for at least 12 months.
Judge CHERYL CAREY, King County Drug Court: So here’s the situation, though—
NARRATOR: In this courthouse in Seattle, defendants must waive their right to a trial if they want to participate in drug court. If they fail the program, they’re at the mercy of the court.
Judge CHERYL CAREY: If you are not successful with the program, you’ve given the courts the right to find you guilty of the charge beyond a reasonable doubt.
JAMIE KVISTAD: Now, their other choice is prison. So I mean, they’re kind of between a rock and a hard place. They have given up their right to challenge the evidence. All that happens is the judge reads the police report, and then sentences them to the crime.
PROSECUTOR: We’re all in agreement with giving Mr. Hassan another chance here.
NARRATOR: If they graduate, the charge is dropped.
Prof. SCOTT BURRIS, Temple Univ. Law School: Drug courts represent in some ways a violation of fundamental human rights in that people must essentially plead guilty and give up their due process rights in order to participate in drug court.
Judge CHERYL CAREY: You are looking at prison. You can’t say, “Gee, I want to change my mind.”
Prof. SCOTT BURRIS: But drug courts also represent innovation, experimentation, practicality. They represent the attempt of people who are right there on the street facing the problem every day to do something different, not just keep repeating the same mistakes, to treat people as individuals.
NARRATOR: In the fall of 2014, 17 years into her addiction, Cari Creasia found herself in drug court.
ATTORNEY: Your Honor, this is Ms. Creasia, and she’s represented by Ms. Vargas—
NARRATOR: She was offered a choice. She could either face trial or agree to the conditions of the court.
CARI CREASIA: They said, “We can mainstream your case. But we can tell you right now you’re going to do one to two years at the very least for this crime.”
JUDGE: You need to attend an empowerment class.
CARI CREASIA: OK.
JUDGE: Either one.
CARI CREASIA: OK. I’ll take care of that.
NARRATOR: It was the second time she had been in trouble with the law. For four months, she had been running drugs to support her habit.
CARI CREASIA: There’s all kinds of ways that people get what they need. I would run drugs. And I eventually was selling it in large quantities. As I became a trusted part of this network, I graduated to that level.
MARCELA GAVIRIA, Producer: Were you part of a drug cartel?
CARI CREASIA: I imagine I was. The individual that I dealt with was dealing directly with individuals that were part of a drug cartel.
NARRATOR: She was an ideal distributor, an unassuming housewife from the suburbs.
CARI CREASIA: I was selling half ounces, ounces to people who would in turn go sell the smaller sacks to their customers. I built a reputation. “She’s the lady that has the good stuff. She’s really nice. She shows up on time. She puts smiley face stickers on her baggies.” That was me.
NARRATOR: But a narcotics unit had been watching. Cari had twice sold heroin to a confidential informant, giving prosecutors all the evidence they needed. Facing certain conviction, Cari decided to opt in.
CARI CREASIA: They explained what they could do for me and that I had an opportunity to get clean and sober. And for some reason, something just clicked inside of me. And it— I told myself, “Take this and run with it. Do it. They’re going to help you get clean.”
NARRATOR: At first, she struggled with the program. She was in withdrawal. The court suggested she start taking methadone.
CARI CREASIA: If I dose at 6:30, I think if I dose right at 6:30—
NARRATOR: But the nearest clinic was 20 miles away. Like Trevor Mercer in Bremerton, she would have to commute a long distance to get her dose.
CARI CREASIA: That reminds me every day what that heroin addiction caused. I have to go every day in order not to use. That’s pretty serious. And that— that’s a message to me every morning that because of the life that you led, because of your addiction, this is what you have to do. And I never forget.
GROUP PARTICIPANT: So yeah, Halloween’s coming up, and that is difficult. And it’s going to be a lot of triggers because I’ve always used and got messed up on Halloween. So what we’re planning on doing is we’re going to have a group of friends that are all sober, all in treatment and stuff, and we’re just going to hang out and—
NARRATOR: The court mandated that Cari attend sober support meetings three times a week.
CARI CREASIA: —because depression can make you want to use, too, so I’m just saying—
GROUP MEMBER: I don’t— I don’t get to where I want to use. Like, my sobriety’s too important to me. Like, I was a complete addict piece of [expletive] for a decade-and-a-half. And you know, I got 14 months clean. I don’t want to [expletive] that up and go through that first 14 months again.
GROUP MEMBER: Why take chances on something—
CARI CREASIA: I don’t think an addict ever gets well. It is a disease.
GROUP MEMBER: What I really wanted to do all the time was get high.
CARI CREASIA: You have to deal with the substance abuse. You have to get treatment. You don’t just put it down. If it were that simple, there wouldn’t be an addiction problem.
GROUP MEMBER: Most of my friends are dead, gone or in jail. And it was just a wakeup call for me, so it was a good reminder of where I’m blessed today and I’m glad of where I am today, so—
NARRATOR: For eight months, Cari remained clean, her graduation just months away.
CARI CREASIA: If you graduate from drug court, the charges are dismissed. And some people think that’s odd. I don’t. I think if you prove that you no longer want to lead a life of crime, you deserve a second chance.
NEWSCASTER: Nationwide, the number of drug courts has doubled in the last decade. Studies have shown that they save taxpayer money because they—
CONFERENCE PARTICIPANT —tremendous believer in drug courts, saw lives changed—
NARRATOR: Drug courts have grown into a movement.
CONFERENCE PARTICIPANT: —but that anyone who knows drug courts, well, they love them.
NARRATOR: Once a year, judges, prosecutors and court administrators gather to cheer their profession at a national conference.
MICHAEL BOTTICELLI, Dir., Office of Natl. Drug Control Policy: Drug courts have blazed the trail for today’s drug policy and criminal justice reform. And drug courts have literally changed the lives—
NARRATOR: In the summer of 2015, the keynote address was given by the White House’s new drug czar, Michael Botticelli.
MICHAEL BOTTICELLI: Twenty-six years ago, I would never have dreamed I would be standing in front of you today. And it was a very wise judge who offered me care and compassion, along with accountability, that led to my path to recovery.
As a result of a drunk driving accident, I was offered a choice by a judge. And so I had the opportunity at that point to get care and treatment and was diverted away from the criminal justice system. And that’s what I want to see for everybody.
NARRATOR: Botticelli helped make drug courts a priority at the White House.
MICHAEL BOTTICELLI: We’ve come to really understand that our punitive, largely punitive responses to people with substance use disorders is ineffective, it’s inhumane, and it’s costly.
NARRATOR: Over at the Justice Department, Attorney General Eric Holder had also been working on rethinking drug enforcement with its toll on low-level offenders, especially minorities.
ERIC HOLDER: I made a determination early on that we had to make some really fundamental shifts in the way in which we were approaching this whole struggle with— with drugs. We need to take some different approaches, and it shouldn’t all be seen as just a criminal justice problem. It ought to be seen as a public health issue.
NARRATOR: Drug courts were high on Holder’s agenda.
ERIC HOLDER: These programs give no one a free pass. They are strict and they can be extraordinarily difficult to get through. But for those who succeed, there is the real prospect of a productive future.
And I wanted to try to highlight alternatives to this emphasis on incarceration. And I found, you know, federal judges and prosecutors who, once exposed to these alternatives, all became enthusiastic.
NARRATOR: Holder’s own conversion happened years before.
ERIC HOLDER: I had been a judge here in Washington, D.C., in the late ‘80s, early ‘90s, when the drug wars were really at their most intense, where I had these mandatory minimum sentences that I had to impose on people who had drug problems, who were selling, you know, relatively small amount of drugs in a non-violent way to support a drug habit that they had and who had to go to jail for a 5-year mandatory minimum or a 10-year mandatory minimum. And I didn’t feel comfortable doing it.
NARRATOR: As attorney general, Holder announced that he would no longer support mandatory minimums for low-level drug crime.
JUDGE: Good morning.
CARI CREASIA: Good morning, your honor.
JUDGE: How’re you doing?
CARI CREASIA: Good. How are you?
NARRATOR: Instead, he helped steer nearly $100 million a year toward the expansion of drug courts.
ERIC HOLDER: I’ve said that in every federal district within the next five years there ought to be a drug court. That ought to be a goal that we set for ourselves as a nation.
Judge CHERYL CAREY: You’re looking at 20 to 60 months in prison.
NARRATOR: But critics say drug courts can be harsh and inflexible.
PROSECUTOR: Your expectation is that the defendant follow all the rules and regulations of the King County jail.
Judge CHERYL CAREY: Absolutely.
PROSECUTOR: You have to obey. Is that clear?
DEFENDANT: Yeah.
SCOTT BURRIS: Drug courts represent prohibition with a human face and the idea that people have to hit rock bottom and that drug users can never change until, you know, someone takes them by the ear and pulls them towards sobriety.
JASMINE TYLER, Drug Policy Analyst, Open Society Foundations: The problem with drug courts is that they continue to think that there’s a moral failing in the individual and that, somehow, waking them up and shocking them with the criminal justice apparatus will create some level of sobriety for that individual. And it’s just not realistic.
NARRATOR: Those with the toughest addictions often drop out. While graduation rates vary from county to county, about half of participants fail to complete the program.
Gailen, who is 24, was sent to drug court in Seattle after he was caught selling heroin to an undercover officer. He was charged with four counts of delivery.
JAMIE KVISTAD, Drug Court Public Defender: A lot of these people that were roped in, they were addicts who were just delivering enough to kind of feed their own addiction. And I guess the question is, who are we really looking for?
ATTORNEY: Your honor, I know he would like to address the court about—
NARRATOR: When we met him, Gailen was just beginning the program. Because of the severity of his case, the court determined that he needed 60 days of in-custody drug treatment.
GAILEN: I wrote this in my room when I was in jail. Can I read it to you?
Judge CHERYL CAREY: OK.
GAILEN: All right—
NARRATOR: After spending two months in custody, Gailen was asking the court to grant him a temporary release.
GAILEN: I want to address the court to let everyone know I will be mindful and responsible and aware of my triggers. Thank you, and sorry for wasting your time.
Judge CHERYL CAREY: Thank you. I appreciate that. Mr. O’Leary?
PROSECUTOR: Your Honor, the state strongly disagrees with the defense request. He is one point away from looking at 60 to 120 months if he picks up another point. So I think he needs to stay right where he is, finish his business. Thank you—
GAILEN: Can I say something?
Judge CHERYL CAREY: Certainly.
GAILEN: I’m not going to use. I can’t. I cannot screw up. I know I’m one point away from going to 60 or 120, but 10 years of my life isn’t worth it. It’s not worth it.
Judge CHERYL CAREY: I believe every single word you just told me. Truly. I also know you have a disease. This is a brain addiction. I don’t know what will happen if I release you right now. I’m going to deny your request because I’m not willing to—
NARRATOR: After completing in-custody treatment, Gailen was released. But he relapsed and soon found himself back behind bars. He had given up on drug court and was angry.
GAILEN: Drug court really tries to scare you into taking any deal because they want as many people possible so they can be, like, “This is our success rate, this is our flunk rate.” I mean, a lot of people are— you know, a lot of people fail. But everyone’s not a failure, you know?
NARRATOR: Gailen is one of thousands cycling in and out of jail. Each time he’s out, he goes right back to using.
GAILEN: See this? That right there, that’s 350 bucks’ worth. This is some A-1 stuff right here. And this’ll make a lot of people OD. All right, I need a cooker.
DAN SATTERBERG, King County Prosecuting Atty.: Drug court stood alone for 20 years as our one answer. But it really doesn’t answer the question of people who are so addicted, who are homeless and who are mentally ill, who can’t keep court appointments, who we know are going to fail drug court.
I think a lot of this is about learning the realities of addiction, and we don’t have a great understanding of that within the criminal justice system. But we’re learning more and more and more about, you know, the human physiological reaction to drugs and to drug addiction and what it takes to get somebody to do less harm to themselves.
GAILEN: All right, look, I’m going to show you what I got—
ALISON HOLCOMB, American Civil Liberties Union: A large majority of Americans now agree that there has to be a more compassionate way, and at the bare minimum, a more effective way of responding and trying to stop what’s happening.
GAILEN: [expletive] yeah! Oh, my God. Good job.
ALISON HOLCOMB: And so the question, I think, is what is the alternative? What’s the solution that we offer people? What can we do differently from sending people to jail?
NEWSCASTER: Another Massachusetts town is trying a new approach to reckoning with its growing problem of drug dealing and addiction.
NEWSCASTER: In Indiana, health officials are now offering a needle exchange program—
NEWSCASTER: Nineteen other police departments across the country have also started using—
NEWSCASTER: —program that will offer rehab instead of—
NARRATOR: Cities all over the country are now starting to embrace public health approaches to the heroin problem.
NEWSCASTER: As part of a pilot program, heroin—
NARRATOR: Seattle had a head start.
Lt. LESLIE MILLS, Dept. of Corrections WA: OK, now, we’re coming up to the major corner here. This is what we call “The Blade.”
NARRATOR: The city has long been known for its progressive approach to drugs, for embracing legal marijuana and for exploring new policing models.
Lt. LESLIE MILLS: This particular corner right here is the most prolific drug-dealing, drug-using, hand-to-hand exchange, drug-loitering corner in Seattle, just open-air drug trafficking. You can clean it up and you can go back 20 minutes later and it’s filled. It’s just quicksand.
NARRATOR: Four years ago, in the city’s downtown core, Seattle’s police department began an experiment which is drawing national attention.
We spent a year following cops, counselors and addicts, seeing how the program works.
LEAD TEAM MEMBER: Look, do me a favor. While we’re in here, just keep your hands out of your pockets, OK?
GUY: Of course.
LEAD TEAM MEMBER: OK.
NARRATOR: It’s known as Law Enforcement Assisted Diversion, or LEAD, and it stops just short of decriminalizing drug use.
LEAD TEAM MEMBER: Have you ever heard of the LEAD program? So instead of taking you to jail today for drug possession, we’re going to help you out. You don’t have a violent history, so you are a perfect candidate for the program.
Lt. LESLIE MILLS: So normally, we arrest a person. We put them in jail. With LEAD, we stop them from what they’re doing. We take the drugs away from them. We take the syringes, or the crack pipe away from them.
Officer VICTOR MAES, Seattle Police Department: The crack cocaine’s inside a foil that’s in there.
Lt. LESLIE MILLS: A LEAD counselor is contacted at that time, and we take the person back to the LEAD counselor.
MARTIN SMITH, Correspondent: Everybody who you find is shooting up heroin, you put in the LEAD program?
Lt. LESLIE MILLS: Nope. Nope.
MARTIN SMITH: So, how does it work?
Lt. LESLIE MILLS: So we have the discretion. We’re police officers. If that person’s committing a violation or a crime, we can arrest them and put them in jail right now. But the program, the philosophy behind the program, is treatment and assistance on demand, and no incarceration.
MIKEL KOWALCYK, Outreach Coordinator, LEAD: Are you interested in medical detox? You can go into treatment. Are you interested in a methadone or Suboxone program? Like, what do you think would help you?
NARRATOR: In addition to enrolling new participants, they go out looking for clients they’ve already enlisted to see how they’re doing. There are now over 300 addicts in the program.
MIKEL KOWALCYK: Are we looking for Wade? OK, so I have a couple people down here—
NARRATOR: Mikel Kowalcyk is in charge of outreach for LEAD.
MIKEL KOWALCYK: That is Felicia. She was just in the office. She’s Christine’s client. She went to treatment.
I used to be a wine salesman, and I got into some issues myself with drugs and alcohol and being arrested and had an opportunity to turn my life around. I’ve been to jail. I’ve looked at the police and not had a good relationship. And I’ve done drugs and I get how that works. And I think that my personal experiences help me with this job. I can relate to the clients.
If you see him, like, tell him Mikel would really love to see you.
LEAD CLIENT: Yeah. I got your number. Look.
MIKEL KOWALCYK: [laughing] How’d you get my number on your hand?
LEAD CLIENT: I got it off my wall.
MIKEL KOWALCYK: You’re awesome!
NARRATOR: Her immediate goal is not to stop her clients from using drugs but to limit the harmful behavior brought on by their addiction.
MIKEL KOWALCYK: The harm-reduction model is, “People are going to use drugs. Let’s make it safe for them to use drugs until they’re ready to do something different.”
How long are you going to stay out here, man? I thought you’d be done by your birthday.
It’s really that simple. And that means if somebody is shooting heroin every day when we meet them, that’s OK. Not everybody is ready at that moment to change their life.
LEAD TEAM MEMBER: Mikel wants to talk to you!
MIKEL KOWALCYK: Yes! Stop him.
NARRATOR: While LEAD doesn’t penalize clients who continue to use, Mikel does offer incentives to steer them towards treatment.
MIKEL KOWALCYK: I talked to Lisa about your housing. They’re willing to put you on a 30-day contract. You’re going to have a curfew. You’re going to have to go to meetings every day for 30 days. Can you do that?
LEAD CLIENT: I can do that. I can do that.
MIKEL KOWALCYK: Why are you still down here right now? That makes me a little concerned.
LEAD CLIENT: No, I just left the welfare office early. I just left the LEAD program today.
MIKEL KOWALCYK: So you know I know what you look like loaded, right?
LEAD CLIENT: Oh, no, no, no. No. No. No. No.
MIKEL KOWALCYK: OK. So if you’re home by 9:00, she’ll work out your housing. She could change her mind, so I don’t want you to lose your housing.
LEAD CLIENT: All right. Sounds like a plan.
MIKEL KOWALCYK: OK? You can go home.
LEAD CLIENT: Thank you. Thank you. Thank you.
MARTIN SMITH, Correspondent: Somebody looking at this from the outside would say, “Wait a minute, you’re allowing them to continue to use.
MIKEL KOWALCYK: Yes.
MARTIN SMITH: That doesn’t seem right.”
MIKEL KOWALCYK: So in my perspective, and a social worker perspective is you can’t make somebody stop using. So not allowing them to use is absurd.
MARTIN SMITH: People will say that LEAD is taking away the stick that is an essential part of motivating somebody to— to get their act together.
MIKEL KOWALCYK: OK. So they go to jail for 30 days, and when they’re out, they continue to use. What interrupts that cycle? Nothing.
MARTIN SMITH: They’re going to continue to use indefinitely?
MIKEL KOWALCYK: They could.
MARTIN SMITH: And they will never be taken out of the program?
MIKEL KOWALCYK: No. They will not, not for use.
MARTIN SMITH: So they can continue to use as long as they want.
MIKEL KOWALCYK: Yes. It’s their life. The goal is to reduce overdose, to reduce theft, nuisance, trespassing, reduce recidivism.
So I know Chris is advocating for you, even if you haven’t connected with him.
NARRATOR: Mikel says most of her clients seem to be improving.
MIKEL KOWALCYK: And you’re wearing the helmet!
CLIENT: Fifteen days clean.
MIKEL KOWALCYK: How many?
CLEAN: Fifteen.
MIKEL KOWALCYK: Oh, my God!
CLIENT: Isn’t that nice?
MIKEL KOWALCYK: That is so awesome!
It doesn’t mean that they’re completely clean and sober, but they’re doing better than they were.
MIKEL KOWALCYK: Oh, hey, Johnny.
JOHNNY BOUSQUET: Hey.
MIKEL KOWALCYK: How’s it going?
JOHNNY BOUSQUET: All right.
MIKEL KOWALCYK: Come on.
NARRATOR: Johnny Bousquet was, for a time, one of Mikel’s greatest success stories.
MIKEL KOWALCYK: How’s things at the shelter?
JOHNNY BOUSQUET: It’s fine.
MIKEL KOWALCYK: What’s fine look like?
JOHNNY BOUSQUET: I’m still there.
MIKEL KOWALCYK: OK.
JOHNNY BOUSQUET: I haven’t gotten in any fights.
MIKEL KOWALCYK: Right.
JOHNNY BOUSQUET: I’m learning how to get stuff stolen from me and not go nuts.
MIKEL KOWALCYK: Johnny was my first client. He came into the office the day after his arrest, and I sat in a room and did all of his paperwork. He said that he wanted to “go to treatment and/or methadone.” Those were his words. And I said, “Well, which would you rather do?” And he said, “Whatever you can get me in quicker.”
And I made a phone call and got him an assessment, and literally five days later, he went to treatment for 60 days. And then he stayed clean for almost nine months. A day is a miracle. Thirty days is a miracle. Eight months is a big deal.
NARRATOR: It was Johnny’s longest time clean in a while. He then relapsed in December 2014 and got sober again with the help of a medication that blocks his cravings. But the medication doesn’t work for meth, which was his new drug of choice.
JOHNNY BOUSQUET: I wanted to look good for this interview, and I don’t look nowhere near as good as I wanted to look. Meth makes you obsess about stuff, so like, I’ll be in the bathroom here picking at my face and make it 15 times worse. I don’t come out until I look like Frankenstein.
My addiction sort of makes the decisions for me when I’m actively in it. I know that I don’t want to do any drugs right now, and that’s never my intent. I kind of hate myself a little bit for the— for the situation I put myself in.
NARRATOR: Four years ago, Johnny led a very different life. On YouTube, there is still a trace of that young musician with an outsized ego and big aspirations.
JOHNNY BOUSQUET: I just used to radiate this kind of can-do attitude that nothing can stop me. 1999 to 2012— it was the best time of my life. It’s when my ex-wife and I were still together. I had about seven years clean and sober at that time and had just finished college and I was top producer in the town.
NARRATOR: Things began to fall apart when he started doing hard drugs.
JOHNNY BOUSQUET: I always wake up really confused, like, “Is this happening for real? Did I really go from that to this?” But it’s pretty real because as soon as I wake up, I think about what my kids might be wearing to school and what my daughter’s hair smells like. She’d always have this really good, fluffy-smelling hair. And I think about what kind of shoes my son has on and if he’s behaving at school.
I haven’t seen my kids since Christmas Eve 2012. I haven’t even been able to talk to them, seen a picture of them, heard how they’re doing, or anything.
I’m kind of scared. It’s life or death for me. It’s real. I’m not saying that because I want somebody to feel sorry for me or something. It’s because I’m scared of that. [weeps] I’m going to— I’m going to keep fighting.
MIKEL KOWALCYK: Jennings is doing really well. Christopher’s doing really well. Thomas is not doing so well, but he’s still working on stuff and he’s claiming to go to treatment. John Bousquet goes back to treatment tomorrow. That was—
NARRATOR: Twice a month, the LEAD team meets to discuss how each client is progressing.
POLICE OFFICER: If he doesn’t get services, he’s probably going to end up dead because he’s overdosing all the time because even though he’s a hard-core heroin addict, he mixes anything he can get—
DEVIN MAJKUT: I think we are doing things differently in a really big way. We all meet at the same table, case managers, social workers, law enforcement, the prosecutor’s office. And I think it allows us to do our work better.
POLICE OFFICER: Anything you can do for Andre because from what I understand, he’s out there chronically. I would prefer to see him get the treatment he needs because he is—
NARRATOR: They brainstorm ways to help clients access services and they compare notes.
CASE MANAGER: Now he’s facing jail time for this warrant that he got picked up on that nobody really knew about. So of course, he relapsed because this happened on—
Lt. LESLIE MILLS: The hardest thing about LEAD is that the philosophy behind LEAD is let them be on their own timetable, which is frustrating for a cop. Greatest thing about being a cop, greatest thing about being a parole officer, you can solve that problem right now. Boom, you’re in handcuffs. You’re in jail. It’s nice and clean.
LEAD’s not clean. LEAD’s gray. LEAD is about, “We have to have a conversation about him,” and, “We have to give him another chance,” and that’s frustrating.
DEVIN MAJKUT: She just doesn’t like the police. Like, it’s not about you as a person. She just doesn’t like the police, and she’s not going to, like, warm up about it. She’s not going to be warm and fuzzy— like, her life experiences, she’s not going to play nice with anyone she doesn’t trust. But for her, I think it’s the first real program she’s ever been in since she got out of prison in 1994.
NARRATOR: Devin Majkut has over 30 clients. Her newest is 20-year-old Kristina Block. Kristina was interested in what the program could do for her, including help erasing pending drug charges.
DEVIN MAJKUT: Some of the sheriffs were concerned about her. They could tell that she had an active addiction. They knew that she was involved in some, you know, illegal activities in the last year. And she had had a pending case on an arrest from December. And instead of filing that case, they referred her for the program.
NARRATOR: We followed her to her intake session.
DEVIN MAJKUT: Hey.
KRISTINA BLOCK: Hi.
DEVIN MAJKUT: I’m Devin.
KRISTINA BLOCK: Hi. Nice to meet you.
DEVIN MAJKUT: Nice to meet you. Come on in.
DEVIN MAJKUT: OK. You know you have a pending charge right now. OK. So when you complete this assessment, the court will not file that charge—
KRISTINA BLOCK: OK.
DEVIN MAJKUT: —OK, which is a felony charge.
KRISTINA BLOCK: Right.
DEVIN MAJKUT: So that’s great. Feel free today to just share as much as you feel comfortable with. You can mess up a thousand times, and the door here would still be open. The goal that we have for you is that your quality of life increases, that you just feel happier and healthier overall, whether you continue to use or not, and that you have less interaction with the police, that you don’t—
Our role is to take an individual and to meet them exactly where they are. To say, “Well, you have to get clean in order for me to provide you services,” is probably going to mean that person doesn’t get services. And so for us, we start with the relationship building.
So where typically can we find you?
KRISTINA BLOCK: The Blade.
DEVIN MAJKUT: The Blade? OK.
KRISTINA BLOCK: Anywhere downtown.
DEVIN MAJKUT: Where do you get your money from, now that you’re not working?
KRISTINA BLOCK: Any way that I can.
DEVIN MAJKUT: OK, like, are you hustling? Are you dealing? Are you borrowing from people?
KRISTINA BLOCK: I sometimes deal.
DEVIN MAJKUT: OK.
KRISTINA BLOCK: I sometimes do dates.
DEVIN MAJKUT: OK.
KRISTINA BLOCK: I steal.
DEVIN MAJKUT: OK.
KRISTINA BLOCK: I boost.
DEVIN MAJKUT: And about how much money would you say you’re making in a week right now?
KRISTINA BLOCK: Maybe, like, a thousand? It’s pretty crappy right now.
DEVIN MAJKUT: Yeah. And is most of your money going—
KRISTINA BLOCK: All of it goes to dope, yeah.
DEVIN MAJKUT: —to your use. OK. Are you interested in treatment right now?
KRISTINA BLOCK: I’m not sure if I’m ready—
DEVIN MAJKUT: OK.
KRISTINA BLOCK: —like, right this second.
DEVIN MAJKUT: I hear that.
KRISTINA BLOCK: [weeps] I really would like to be ready!
DEVIN MAJKUT: OK.
KRISTINA BLOCK: I just feel really, like, overwhelmed with the thought of treatment, and I just feel like I need some time.
DEVIN MAJKUT: OK. When you are or if you are ever ready for treatment, I’ll bust ass to get you into somewhere that feels good.
NARRATOR: Kristina has been living on these streets for the past three years. It’s a hard turn from her childhood in a middle-class neighborhood in Seattle. It was here that her addiction began while she was still a teenager.
KRISTINA BLOCK: I had been smoking every single night, sneaking out and being out all night, smoking the bubble, like, all night, like, in a stolen car, breaking into cars, breaking into houses with these junkies, you know, at 17, on a school night. And then I’d go to school and I’d go to the bathroom, sit on the toilet and do drugs until it was 6:00 o’clock at night, and then go home.
NARRATOR: Her father says he was slow to pick up on the signs that there was an addict in the house.
RAFAEL BLOCK, Kristina’s Father: It was a little bit of a shock when I first found out about it because I thought, you know, “This is not supposed to happen to us.” I felt that we had been very honest with her about drug use. Sometimes, I wonder, you know, should I have had more conversations with her, or was I assuming that she was smart enough to know better?
KRISTINA BLOCK: My dad has begged me to get clean so many times. He’s, like, cried so many times. I’ve just totally shattered every dream and hope that he’s had. But I do really want to believe that I’m capable of doing a whole lot more than just what I’m doing right now.
I’m really excited about LEAD. I’m hopeful, I guess. Most programs are kind of, like, you need to reach a certain point, and if you fail, you kind of get penalized and you get set back. With LEAD, it’s kind of like on your own terms. And I could [expletive] up a thousand times and still have the opportunity to get help.
KRISTINA BLOCK: Thank you.
GUY: Appreciate it.
KRISTINA BLOCK: Do you have that lighter? Do I have it? I have it. I don’t have it.
I don’t plan on being like this forever. Like, I want things in life, you know? I want to go to beauty school. I want to— and that’s something that the LEAD program is probably going to help me with. The lady told me that they’ll help with housing and treatment and funding to, like, go to beauty school and stuff.
NEWSCASTER: Because of the rampant outdoor drug use and crime, throughout downtown Seattle, businesses are going to stay away—
NARRATOR: LEAD began as a way to deal with drug crime on the streets.
NEWSCASTER: Police here are cracking down on crack dealers—
NARRATOR: Its origins go back to the crack epidemic of the 1990s.
Officer VICTOR MAES, Seattle Police Department: The downtown area was infested with drug users, pill sellers, shoplifters, individuals who were out there to buy stolen items. And many of the citizens were just tired.
NEWSCASTER: —drug dealers hawking their wares on a street corner. This scene on a Seattle street is a familiar one.
Lt. LESLIE MILLS, Dept. of Corrections WA: At any given time, you could literally see 50 or 60 people smoking crack or doing hand-to-hand exchanges.
MARTIN SMITH, Correspondent: But there was a war on drugs in the sense that we took a militarized approach to busting people that were using drugs—
Lt. LESLIE MILLS: Yup. Yup. Yup. We did. If you’re using open-air, drug trafficking, or you’re using drugs in public, you’re going to get charged.
NEWSCASTER: —today sweeping arrests all over Seattle, street sales of cocaine.
NARRATOR: The problem was that in a predominantly white city, most of those arrested were black.
NEWSCASTER: This block right here has always been a hotspot. On this block, there were—
NARRATOR: A hard-charging public defender accused the police of racial bias, Lisa Daugaard.
MARTIN SMITH: There was a lot of hostility towards you coming from the police. A lot beat cops—
LISA DAUGAARD, Public defender, King County: I think that’s an understatement. [laughs]
MARTIN SMITH: A lot of beat cops didn’t like you.
LISA DAUGAARD: A lot of everyone throughout the hierarchy didn’t like me.
NEWSCASTER: The police in Seattle are facing racially-charged criticism—
NEWSCASTER: A new study claims officers are four times more likely to arrest black dealers than white.
NARRATOR: The tension with the police escalated as Daugaard pressed her case.
LISA DAUGAARD: We’re talking about hundreds, if not thousands of case that these officers have been involved in that could be—
DAN SATTERBERG, King County Prosecuting Atty.: We were in the middle of this seemingly endless round of litigation. And one day, we just sat down, Lisa and I and a police lieutenant from the Seattle Police Department. And she said, “Well, we just want the police to have another option, to take somebody to treatment.” And that’s when the Seattle police lieutenant said, “Well, that’s what we want, too.”
And by putting down the law books and sitting down and looking at each other, we realized that we could work together and accomplish a lot, that the courts could not fix this problem.
TASK FORCE MEMBER: We’re also looking at— to point some of our resources elsewhere—
NARRATOR: For several years, the prosecutor, the police and the public defender debated possible solutions.
TASK FORCE MEMBER: —and members of the community to help us, you know, drive the crime rate down.
NARRATOR: It all came together when they agreed on one thing— that police should be given more options at the point of arrest.
LISA DAUGAARD: There are going to be crimes, and that means that the police are going to be there one way or another, and we had to figure out how working from that point of contact, everything could turn out very differently.
Lt. LESLIE MILLS: Any weapons?
MAN: No.
Lt. LESLIE MILLS: Any drugs?
Capt. DEANNA NOLLETTE, Seattle Police Department: This was the first program that actually said, “No, we’re going to start with a law enforcement-led program that intervenes at the time of arrest.”
DEANNA NOLLETTE: We’re not going to put people through the entire system and spend all of the resources to prosecute them. We’re going to try to move the intervention back a little bit on that timeline and try to see if we don’t get better outcomes.
MARTIN SMITH: So to those who look at the LEAD program and say, “What are they doing? They’re decriminalizing the use of heroin and meth and crack cocaine?”
DAN SATTERBERG: What LEAD has done is to turn the— the moment of arrest into an intervention. It has shown us another way for people who are severely addicted, who, you know, could use some help, that giving them that help actually makes the community safer. And it’s more effective and it’s cheaper than just going in and arresting people.
MARTIN SMITH: You spent your whole career being a prosecutor, enforcing the law, putting people away. And suddenly, you’re going to say, “No, no, no, that was all wrong.” It is a big switch.
DAN SATTERBERG: There’s an old saying that just because wisdom is slow to arrive doesn’t mean you should reject it when it does.
NARRATOR: LEAD was officially rolled out in 2011, and an unprecedented experiment in American drug policy was born.
NEWSCASTER: Police and the FBI are calling it one of the city’s biggest drug busts ever—
NEWSCASTER: Two hundred undercover buys, heroin, meth and cocaine taken off the street and dozens of suspects arrested. However, many may never see the inside of a prison. Instead, the bulk of these suspects will be allowed to enter a crime diversion program where they’ll receive drug treatment and opportunities for things like housing, rather than a felony conviction.
NARRATOR: It wasn’t long before the program was in the national spotlight.
NEWSCASTER: A University of Washington study found that LEAD has been remarkably successful.
NEWSCASTER: —showing a drop in repeat offenses from people who enter the LEAD program.
NARRATOR: It was also being replicated across the country.
NEWSCASTER: —Santa Fe’s three-year pilot program—
NEWSCASTER: It’s known as LEAD, and Albany is just the third city in the country—
NARRATOR: Washington, D.C., took notice. In July 2015, the team was invited to the capital to talk about the lessons of their four-year experiment.
DAN SATTERBERG: It’s been a remarkable day, and I first of all need to do a shout-out to my favorite public defender, Lisa Daugaard—
DAN SATTERBERG: I think that we created a lot of momentum. We got a lot of people excited about it, and I can sense that the administration wants to use their— their last 18 months or so as a way to shine the spotlight on criminal justice reform issues.
Lt. LESLIE MILLS: And the reason we know it works is because people come into my office every day, and say, “Officer Mills, I have cocaine in my pocket. Will you please arrest me and put me into your program.”
LISA DAUGAARD: Fundamentally, it is a program in which individuals—
NARRATOR: They also shared the results of a study produced by the University of Washington which found that LEAD participants have a 58 percent lower likelihood of being arrested than addicts outside of the program.
LISA DAUGAARD: LEAD participants do shoplift. Some LEAD participants do engage in other low-level property crime, and occasionally in serious crime. It’s just that they do that a lot less frequently than people who are not in LEAD who started out in the same situation.
MARTIN SMITH: And that’s what the University of Washington study showed.
LISA DAUGAARD: Yes.
NARRATOR: But does LEAD help participants reduce their drug use? A new study will soon be released.
We came back to Seattle. Kristina was three months into the program. She wasn’t taking advantage of LEAD’s services and had missed most of her appointments with her case manager.
KRISTINA BLOCK: —6, 8, 10, 12, 14, 16. Can I just get, like, two bags?
Right now, I think I’m kind of, like, at a, like, standstill. The reason why I’m not going to treatment right now is because I don’t want to let myself down and everyone else down. I’m always so busy and hectic and sidetracked, and my mind’s in a million different places.
Yeah, but I mean, I already gave you guys, like, two bags. Like, I—
Like, my parents ask me why I don’t put my all into getting clean.
Wait. What?
And it’s really not that I don’t want to. It’s really just that I’m not there yet.
But you need to pay me back 20, so that leaves you with 60.
NARRATOR: Her days were busy dealing drugs. She was still doing heroin and relying on meth to keep her going.
KRISTINA BLOCK: Wait. I got a few people that need something. Hola.
NARRATOR: Kristina had met a dealer who she said cut her a good rate.
KRISTINA BLOCK: And If I wasn’t dealing, I’d probably be living dime bag to dime bag, like, paycheck to paycheck, you know?
NARRATOR: She was buying a ball of heroin, about three grams, and selling it at a profit. The money from the sales allowed her to consume even more drugs. Seeking treatment was not a priority.
KRISTINA BLOCK: Hey, Fro! How was it?
GUY: Good.
MARCELA GAVIRIA, Producer: Do you think jail would be the solution for you?
KRISTINA BLOCK: Literally, that, like, makes me panic so bad that I would probably have a heart attack. Jail is the worst place on Earth. I wouldn’t wish jail on my worst enemy.
MARCELA GAVIRIA: Have you ever called the cops on her and said, “I’m just going to throw her in jail”?
RAFAEL BLOCK: I’ve wanted to lots, but putting her in jail doesn’t do anything to treat her addiction. It’s a completely negative experience. She’s not out harming people. She’s doing something that people have decided is illegal and not a health issue. And so she winds up being a criminal when she’s not actually a criminal.
The thing that the LEAD program does for her is it keeps her out of jail, basically. But if you’re not tackling the root issue, then what are you really accomplishing? I can only kind of hope that she finds a resource within herself and pulls herself out of it.
It’s been going on for a long time. Had a thing on NPR today about some guy who’s gone viral because he went on his Facebook and was talking about his daughter that died at 24.
KRISTINA BLOCK: I’m not going to die.
RAFAEL BLOCK: Well—
KRISTINA BLOCK: I’m not going to die.
RAFAEL BLOCK: You can’t guarantee—
KRISTINA BLOCK: Dad, I will not let this kill me.
RAFAEL BLOCK: —that something is accidentally going to happen to you.
KRISTINA BLOCK: What is accidentally going to happen? You can’t live life thinking like that. You just can’t. I’ve never OD’d.
RAFAEL BLOCK: Twice last year, she was hospitalized with life-threatening illnesses directly related to her drug use and was still getting high in the hospital, and then was getting kicked out of the hospital because she was using in the hospital. And I would have thought that would be a wakeup call. That didn’t get her to change her behavior.
MARCELA GAVIRIA: Why is she doing this?
RAFAEL BLOCK: I don’t know that I fully understand it. All I can kind of do is love her as much as I can and help her as much as I can.
KRISTINA BLOCK: I will not find myself at 50, you know, with a needle in my arm.
No, you didn’t. We shared our rinses together. [phone rings] Oh, [expletive] That’s my case manager. I can’t answer that right now.
I know everybody thinks they’re special. I know everybody thinks they’re different. And maybe it’s just a lie that I have to tell myself just to make myself feel better. And I’m only 20, like, almost 21. So it’s, like, how— like, how— like, how much longer is it going to take? And how many times more is it going to be until I actually get it?
NARRATOR: Just outside Washington, D.C., scientists at the National Institute on Drug Abuse are trying to understand addictions like Kristina’s.
MARTIN SMITH: Kristina is addicted to heroin. What exactly is happening inside her brain?
NORA VOLKOW, M.D., Dir., Natl. Institute on Drug Abuse: Heroin is among the most addictive drugs. That means that the probability of someone becoming addicted to it is much higher than the probability of someone, for example, getting exposed to alcohol.
NARRATOR: Dr. Nora Volkow says all addictions have a strong genetic component.
Dr. NORA VOLKOW: Fifty percent of our vulnerability to become addicted is genetically determined. And the other 50 percent relates to multiple factors, including the age at which you start taking the drugs or the alcohol. The younger you are, the greater the likelihood that you will become addicted.
NARRATOR: Dr. Volkow believes that over time, exposure to drugs like heroin disables the part of the brain that regulates impulse control.
Dr. NORA VOLKOW: All of these drugs will with repeated administration erode the function of the frontal cortex. The easiest metaphor is driving a car without brakes. You may very well want to stop. If you don’t have brakes, you will not be able to do it.
MARTIN SMITH: So you’re saying that the drug itself, the experience of taking the drug, will damage the brain.
Dr. NORA VOLKOW: With repeated exposure, yes.
MARTIN SMITH: And I still don’t understand quite what’s happening in the brain. And I suppose as scientists, you don’t fully understand what’s happening.
Dr. NORA VOLKOW: That’s what I was going to say, you know, you are not the only one. The brain is too complex. We are starting to get a sense of the major changes, but our understanding of the human brain is just that it’s very early stages.
MARTIN SMITH: If you ask most people, I imagine that they would say treatment doesn’t work because everybody has an experience with somebody who’s been in and out of treatment numerous times
Dr. NORA VOLKOW: Correct. I mean, and the problem is that we have this magical thinking about treatment. You say you put someone into treatment for one month and they are going to be cured. And that’s why I make this emphasis, we do not cure addiction. We treat it.
NARRATOR: Johnny has tried many different kinds of treatment.
JOHNNY BOUSQUET: I’ve been in inpatient treatment four times in the last three years. And I don’t know what’s going on. No matter how hard I try, it’s— it’s not going away. I just wish that there was something available to help me.
MIKEL KOWALCYK: OK. Let me keep this until you get out.
NARRATOR: Again and again, Mikel has tried to find a new drug treatment facility that will take him.
MIKEL KOWALCYK: There’s not enough beds for people. It’s very difficult to get somebody into detox. So Johnny goes to inpatient treatment on the 16th. So it’s just this hoping he makes it to the 16th. That’s where we are right now.
MARCELA GAVIRIA: He’s in the middle of a life-threatening moment, and he’s got to wait for 11 more days?
MIKEL KOWALCYK: Yep. And he’s lucky he only has to wait 11 more days because there’s a lot of people that don’t even have that bed date.
JOHNNY BOUSQUET: I have to do it, like, a minute at a time. I have to do— whatever I have to do to get high, I have to do that to be sober. But more than anything, I don’t want to go another— another day living like this.
MIKEL KOWALCYK: They are going to purchase the bus ticket at the Greyhound—
NARRATOR: Johnny was finally offered a spot in a rehab center four hours by bus from Seattle.
MIKEL KOWALCYK: So are you ready for this?
JOHNNY BOUSQUET: Yeah.
MIKEL KOWALCYK: Yeah? Feeling good about it?
JOHNNY BOUSQUET: I’m more than ready. I wish it was today.
MIKEL KOWALCYK: I know. Hang in there, OK?
JOHNNY BOUSQUET: OK.
MIKEL KOWALCYK: Five days and a wake-up, right?
JOHNNY BOUSQUET: Yeah.
MIKEL KOWALCYK: OK. Was that a smile?
JOHNNY BOUSQUET: Yeah.
MIKEL KOWALCYK: It’s really nice to see you smiling.
JOHNNY BOUSQUET: I’ll smile more. Thank you, Mikel.
MIKEL KOWALCYK: OK. You’re welcome, Johnny. Get something to eat OK? All right.
JOHNNY BOUSQUET:
Got about 30 minutes until we get there. I’m excited, I’m hungry.
NARRATOR: Johnny made this video on his way to the center.
JOHNNY BOUSQUET:
I’m ready to take on the world.
NARRATOR: But when he arrived, he was told there was no bed.
JOHNNY BOUSQUET:
I’m kind of devastated and pissed off. I just want to get back to my kids and to my music and back to being me because I don’t know who I am right now. I just want to change.
MARTIN SMITH: So he gets on the bus, goes out there, and they say, “Sorry”?
MIKEL KOWALCYK: “Sorry, we don’t have a bed for you.” And he hung in there. But so much went wrong in that timeframe.
MARTIN SMITH: Do you feel that you have enough resources to provide your clients the services that they need?
MIKEL KOWALCYK: No. Absolutely not.
MARTIN SMITH: How sustainable is LEAD, given those shortages?
MIKEL KOWALCYK: That’s a systemic issue. We’re there in the interim. A lot of people don’t make it during that wait.
MIKEL KOWALCYK: [on the phone] Hi, Santa. This is Mikel. I’m trying to confirm that a client made it to class.
MARTIN SMITH: So you’re that bridge, but it seems, like, if we’re going to, as a society, commit to a program like LEAD, we’ve got to do a lot more to provide the services that you’re set up to connect them with.
MIKEL KOWALCYK: Absolutely. It all starts with funding from the top down.
MARTIN SMITH: You have launched a program that provides addicts with services, but the services aren’t there.
LISA DAUGAARD, Policy Director, Public Defender Assn.: Well, that’s true, but that’s not a critique of LEAD because even with those limitations, we do better than the alternative, the incarceration and prosecution alternative.
MARTIN SMITH: It may not be a criticism of LEAD, but it is saying that we’re— we’re not there yet. As one person put it, “We’ve put a plane into the sky, but we don’t have a runway.”
LISA DAUGAARD: Well, the truth is you can’t divert people to nothing. We have to divert folks who otherwise are going to jail and into the court system to a robust public health system. And most communities don’t have that yet.
HEARING: Committee will come to order. This hearing today will examine the scientific evidence for treating drug addiction—
NARRATOR: Even if services are available, there is a shortage of quality care, and very little information to guide families.
TOM McLELLAN, Ph.D.: Very few medical, nursing, or pharmacy schools provide even basic training—
NARRATOR: It’s a reality that President Obama’s deputy drug czar, Dr. Tom McLellan, experienced first-hand.
MARTIN SMITH: You’d had your own personal tragedy. You’d lost a son to a drug overdose. You had another son who was in recovery by that time from a drug addiction.
TOM McLELLAN: I had become an expert in the addiction field. And then my son became addicted, and I had no idea what to do. All that training, all that knowledge about addiction did not prepare me for the most fundamental question of all. Where do you send your kid for treatment? I didn’t know the answer, and none of my expert friends knew the answer.
And that changed my life. I’ve been to easily 300 addiction treatment programs in the United States over my career, probably more. I saw why lots of things that sound so good in academic circles and are so theoretically compelling simply cannot work in a real-world setting. Relapse rates are 50 percent within 90 days, typically, of discharge from treatment. You’re left with the conclusion that either treatments don’t work or addicts can’t be treated.
NARRATOR: Dr. McLellan believes that heroin addiction should be treated like a chronic illness, with long-term outpatient therapy and access to methadone or newer medications like Suboxone. But because those medications can be addictive, they are highly restricted.
Prof. SCOTT BURRIS, Dir., Temple Univ. Center for Health Law: There’s a real geographic problem. There are just whole stretches of the country where clinics are not readily available. Methadone is tightly regulated. It’s confined to specific authorized clinics and given under a very rigid system. And you have to actually get to the physical location. It’s not— every doctor can’t prescribe to those who need it.
MARTIN SMITH: Old-style drug warriors will say that giving a person methadone is simply replacing their heroin addiction with another addiction.
SCOTT BURRIS: As long as they’re against— also against giving people insulin for diabetes, which merely replaces one chemical for another. There are people who need ongoing stimulation of, you know, certain receptors in their body to be healthy, and giving them the medication that does that is valid medical treatment.
NARRATOR: Johnny is one of those patients. Last spring, after one of his relapses, he found a primary care doctor who was able to prescribe Suboxone.
JOHNNY BOUSQUET: Hey, what’s up, Dr. Capp?
PHIL CAPP, M.D., Swedish Medical Center, Seattle: Good to see you.
JOHNNY BOUSQUET: The Suboxone blocks heroin. So even if you want to get high on heroin, you won’t be able to because it has a blocker in it that stops that. And that’s the main reason why I got on it.
Dr. PHIL CAPP: How’re you doing?
JOHNNY BOUSQUET: I’m doing good.
Dr. PHIL CAPP: I don’t think we should make any move on the Suboxone dose. I think you’re stable on three a day.
When I walk into these rooms, I’ll have someone next door who’s 50-year-old, diabetes is out of control, blood pressure’s through the roof. And I’ll go in and have a discussion with them about, “Boy, you know, I— I’ve got some concerns here. And this is what I see if we don’t make some changes.”
And what I— I run up against all the time is the ambivalence around people wanting to change. And I walk out of that room, and I think, “I just don’t know how it’s going to go for that fellow.” And I wash my hands, and I walk into the next room, and there’s Johnny. And he wants to change. I got all the time in the world for that because that takes real steel, and there’s not anything he wouldn’t do to get better.
NARRATOR: Suboxone is significantly more expensive than methadone, but it’s also considered more effective. But Dr. Capp can only prescribe it to 100 patients per year.
Dr. PHIL CAPP: I can only prescribe so much Suboxone. I’m limited by the federal government on how many people that I can follow at any given time.
MARTIN SMITH: Why?
Dr. PHIL CAPP: It’s a good question. I— I think that the DEA wanting to keep a very close eye on prescribers to make sure that prescribers don’t turn into pill mills, where medicine’s not being used appropriately.
MARTIN SMITH: But let me understand this. We’ve had doctors and pharmaceutical companies promoting OxyContin, and doctors have been freely prescribing OxyContin without any limitation on how much they can prescribe.
Dr. PHIL CAPP: The irony is not lost on me. You can— I can prescribe enough OxyContin to put half of this city to sleep.
MARTIN SMITH: Wait a minute. You can prescribe as much OxyContin as you want, but you’re limited by the DEA on how much Suboxone you can prescribe?
Dr. PHIL CAPP: That’s right. That’s the current state of affairs.
NARRATOR: Johnny credits the drug for helping him in his recovery.
JOHNNY BOUSQUET: And right here, it says, “Hey, Johnny, you’ve been clean and sober since July 23rd, 2015.” Day by day, that’s 90 days. Hour by hour, that’s 2,173 hours, 130,412 minutes, 7,824,729 seconds.
Yeah. I did all of that, one second, one minute, one hour at a time.
NARRATOR: Last August, Johnny finally moved into his own room in clean-and-sober housing paid for by LEAD.
JOHNNY BOUSQUET: I definitely wouldn’t have this if I was still on drugs. It’s not much, but it’s money. And that’s my son Johnny and my daughter Leona. And this is right when I first started to use drugs. Kind of sucks. Actually, it sucks a lot because there’s two kids out there that probably wonder if I love them or not. I wonder if they love me or not.
I’ve been carrying this around for three years. I bought this for my son’s 3rd birthday, and I never got to see him for that. So I’ve been hoping that I could give this to him some time. But he’s 6 now. He’s probably not going to think it’s very cool. But I’ve been saving it for him. Yeah.
I just have a higher quality of life right now, even though I’m nowhere where I want to be. I’m still at the bottom. I’m a— couple steps below the bottom. And I’m just trying to be a normal person and reintegrate myself back into society. And it’s hard because I’m adjusting. I want to get back to my kids.
DEVIN MAJKUT, Case Manager, LEAD: [on the phone] Hey, Kristina, it’s Dev. I’m hoping that we can meet up tonight. Can you give me a call as soon as you get this? Yeah, I want to come by and see you, so— thank you.
If I don’t hear from someone for a while, I usually go looking for them. So I’m looking for Kristina. I haven’t seen her in person in about two weeks. And that’s not abnormal. People get really caught up in active addiction and street life, and time flies. I mean, the time schedule that they’re on is really different.
[knocking on motel room door] Kristina? Kristina, it’s Dev.
NARRATOR: In October, we found Devin still trying to get Kristina to keep her appointments.
DEVIN MAJKUT: The last time I saw her, she was struggling a lot. And so yeah, it’s discouraging when you go and look for people and you can’t find them, or you wonder, like, what they’re up to.
NARRATOR: After several hours of searching, Kristina finally resurfaced.
DEVIN MAJKUT: Hi.
KRISTINA BLOCK: I’m sorry.
DEVIN MAJKUT: It’s OK.
KRISTINA BLOCK: No, it’s really— I’ve been on this roller-coaster of trying to stay well every day, you know? And that seriously consumes every waking, breathing, functioning moment of my life right now.
DEVIN MAJKUT: Right, and it, like, becomes overwhelming.
KRISTINA BLOCK: I haven’t been to see you. I got two more tickets now because I haven’t— [weeps]
DEVIN MAJKUT: So it’s, like, totally consuming.
KRISTINA BLOCK: And it’s like really [expletive] cold outside, man! [weeping]
DEVIN MAJKUT: You’ve been sleeping out here?
KRISTINA BLOCK: Yeah.
It’s pouring rain every day outside and it’s freezing cold, and I’m sleeping on the sidewalk. And I don’t have any money, and I’m, like, dope-sick every day, and I have, like, no way of getting well and— it’s kind of like a point in my addiction where that’s like a repetitive thing every day.
DEVIN MAJKUT: When’s the last time you stayed with your dad?
KRISTINA BLOCK: Several weeks.
DEVIN MAJKUT: OK.
RAFAEL BLOCK: I don’t want to completely cut her off, and that’s just really hard to do week after week, month after month, year after year.
KRISTINA BLOCK: Can I request for you to hit me up a little bit more?
DEVIN MAJKUT: Yup. How often?
KRISTINA BLOCK: Like, whenever you think about me.
RAFAEL BLOCK: You know, if somebody came up to me and said, “This is what works, this is the way you need to do it,” then I would do that. But right now, there are people that are chipping away at the corners of it, trying to do something. But there’s no tool for us.
KRISTINA BLOCK: Thank you. I love you. Thank you so much.
NARRATOR: The CDC recently released its most current data on the epidemic, another 14 percent rise in overdose deaths from heroin and other opioids.
MARTIN SMITH: Any predictions on how long it’s going to take for us to turn the corner and start to see a decrease in the number of overdose deaths?
TOM FRIEDEN, M.D., Director, CDC: Well, it took 15 years for it to get this bad. I don’t think it’s going to be turned around in 15 months. It depends on how quickly we work, how intelligently we work, how quickly doctors improve prescribing patterns, and how quickly communities establish support systems, for people with addiction or at risk of addiction, that decreases the risk that they will get addicted to and die from an addictive substance.
NARRATOR: Earlier this month, the Obama administration requested more than a billion dollars in new funding for addiction treatment. It is also considering relaxing the rules on prescribing medications like Suboxone.
TOM McLELLAN, Ph.D., Chair, Treatment Research Institute: Of all the things that society has tried to reduce addiction and the devastating problems that occur— they’ve tried punishments. They’ve tried to legislate. They’ve tried religion. They’ve tried lots and lots of things. The best by far so far is treatment.
We’re going to continue to pay the price for thinking of this as a lifestyle issue, a personality disorder. We’re going to pay that price for a very long time because it’s standing in our way of medical progress, of public health progress.
NARRATOR: This month, Cari was set to graduate from drug court. She had completed all the requirements while dealing with the terminal illness of her partner of 10 years. But just days before her graduation, her weekly drug test came up positive for opioids. Her graduation was postponed until June.
As for Johnny, a few weeks ago, he got into trouble. He overdosed on synthetic marijuana and ended up in the hospital. He was kicked out of clean-and-sober housing, but he is still enrolled in LEAD.
In December, Kristina was hospitalized with a heart and lung infection– a result of her intravenous drug use. After several weeks in an intensive care unit, she decided it was finally time to quit.
KRISTINA BLOCK: I really don’t want to use again. When you’re on heroin, you’re just always sick, and if you’re sick, you can’t do anything. Methadone gives us the power to be able to, like, live.
Kristina, and 50 milligrams.
NARRATOR: She is dosing seven times a week.
CLINIC WORKER: Here’s your medication.
KRISTINA BLOCK: Thank you.
NARRATOR: The hospital found her a spot in transitional housing, where she is staying while she continues to recover.
KRISTINA BLOCK: I’ve managed to make it out of the hospital and stay here and not use yet. I think what sealed the deal for good was the hospital stay. Yeah, for sure. I had two lung surgeries back to back, so I was, like— it was a really bad time.
NARRATOR: But the temptation to use is always there.
KRISTINA BLOCK: Now that I’m clean, I try to spend most of my time away from here because I’m so fragile right now. It’s that addict brain and my actual brain— just a tug of war. But right now, my clear-headedness is overtaking the addict brain a little bit more because I’ve seemed to stay clean for this much time, right? So—
Devin and I were talking about getting into housing, like, me saving up for my own place, like, me getting into Oxford.
NARRATOR: For now, her father drives her to the methadone clinic.
KRISTINA BLOCK: It feels really good to make my dad smile, make my dad happy. Yeah, it feels good.
RAFAEL BLOCK: I’m just— I’m, like, really hopeful, but I’m trying not to get my—
KRISTINA BLOCK: Because I’ve failed so many times.
RAFAEL BLOCK: —expectations up too high. Yeah, I’d rather—
KRISTINA BLOCK: I know. I’m sorry.
RAFAEL BLOCK: That’s OK. That’s water under the bridge now. And some day, we’ll look back at this as, you know, this thing we can talk about in retrospect.
KRISTINA BLOCK: We’ll see. One day at a time.
WRITTEN, PRODUCED AND DIRECTED BY Marcela Gaviria
EDITED BY Brian Funck Lindsay Utz
PRODUCER Will Cohen
CO-PRODUCER Brian Funck
DIRECTORS OF PHOTOGRAPHY Timothy Grucza Ben McCoy
FIELD PRODUCER Timothy Grucza
CORRESPONDENT Martin Smith
ASSOCIATE PRODUCER Tom Denison
LINE PRODUCER Christine Canedo
NARRATOR Will Lyman
ASSOCIATE EDITOR Charles Farrell
ADDITIONAL EDITING Steve Audette, A.C.E.
ORIGINAL MUSIC Francois-Paul Aïche
ADDITIONAL ORIGINAL MUSIC John E. Low
CAMERA Tim Matsui Jake Swantko Scott Anger Jason Longo
SOUND Drew Levinson Jason Pawlak Steve Roseboom
ONLINE EDITOR/COLORIST Dave Bigelow
SOUND MIX Jim Sullivan
ASSISTANT CAMERA Ryan Kemper Sachi Cunningham
ADDITIONAL RESEARCH Lorena Galliot
ADDITIONAL SOUND Jason Alberts Sam Kashefi
PRODUCTION ACCOUNTANT Amy Carter
INTERNS Kiki Barnes Oscar Dupuy d’Angeac Nathaniel Nelson Katie Moore
ARCHIVAL MATERIALS AP Images Bremerton Kitsap Access Television C-Span Corbis CNN Getty Images House Committee on Oversight and Reform KOMO Television Archives NHNZ Moving Images Wazee Digital
Original funding for this program was provided by Public Television stations, Corporation for Public Broadcasting, John D. and Catherine T. MacArthur Foundation, Park Foundation, John and Helen Glessner Family Trust, Ford Foundation, Wyncote Foundation, FRONTLINE Journalism Fund
FOR FRONTLINE
PRODUCTION MANAGER Megan McGough Christian
ON-AIR PROMOTION PRODUCER Missy Frederick
ON-AIR PROMOTION EDITOR Barry Clegg
POST PRODUCTION SUPERVISOR Eric P. Guliiver
ASSISTANT EDITOR Lindsey Rundell
POST PRODUCTION ASSISTANTS Miles Alvord Kenzie Audette Joey Mullin
FOR WGBH OUTPOST
DIRECTOR OF POST PRODUCTION Chris Fournelle
SENIOR DIRECTOR PRODUCTION TECHNOLOGY Tim Mangini
SERIES MUSIC Mason Daring Martin Brody
SENIOR DIRECTOR OF AUDIENCE DEVELOPMENT Pamela Johnston
ASSISTANT DIRECTOR OF AUDIENCE DEVELOPMENT Patrice Taddonio
AUDIENCE ENGAGEMENT EDITOR Katherine Griwert
COMMUNICATIONS ASSISTANT Anne Husted
SECRETARY Christopher Kelleher
EDITORIAL ASSISTANT Amy Gaines
RECORDS MANAGER John Campopiano
EDITORIAL RESEARCH MANAGER Lisa Palone
LEGAL Eric Brass Jay Fialkov Janice Flood
SENIOR CONTRACTS MANAGER Gianna DeGiulio
BUSINESS MANAGER Sue Tufts
DIRECTOR OF BUSINESS Tobee Phipps
DEVELOPER Ly Chheng
SENIOR DIGITAL DESIGNER Dan Nolan
INTERACTIVE EDITOR Chris Amico
FRONTLINE/COLUMBIA JOURNALISM SCHOOL FELLOWSHIPS
ABRAMS JOURNALISM FELLOW Sara Obeidat
TOW JOURNALISM FELLOW Kattie Worth
DIGITAL RESEARCH ASSISTANT Priyanka Boghani
DIGITAL VIDEO PRODUCER Michelle Mizner
DIGITAL EDITOR Jason Breslow
SENIOR DIGITAL REPORTER Sarah Childress
SENIOR PRODUCER, DIGITAL VIDEO Shayla Harris
MANAGING EDITOR, DIGITAL Sarah Moughty
POST COORDINATING PRODUCER Robin Parmelee
SERIES COORDINATING PRODUCER Carla Borras
SPECIAL COUNSEL Dale Cohen
SENIOR EDITOR AT LARGE Louis Wiley Jr.
SENIOR PRODUCERS Dan Edge Frank Koughan
MANAGING EDITOR Andrew Metz
MANAGING DIRECTOR Jim Bracciale
EXECUTIVE PRODUCER AT LARGE David Fanning
EXECUTIVE PRODUCER Raney Aronson-Rath
A FRONTLINE production RAINmedia, Inc.
©2016 WGBH Educational Foundation ALL RIGHTS RESERVED
FRONTLINE is a production of WGBH/Boston, which is solely responsible for its content.
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.



















