Coronavirus Pandemic
April 21, 2020
54m
FRONTLINE investigates the U.S. response to COVID-19 — from Washington State to Washington D.C. — and examines what happens when politics and science collide
Coronavirus Pandemic
April 21, 2020
54m
Share
How did the U.S. become the country with the worst known coronavirus outbreak in the world? FRONTLINE investigates the American response to COVID-19 — from Washington state to Washington, D.C. — and examines what happens when politics and science collide.
Produced by
Transcript
Credits
Journalistic Standards
Support provided by:
Learn More
Most Watched
The FRONTLINE Newsletter

How America’s First Known Coronavirus Patient Recovered

“We’ve Got to Double Our Efforts”: WA Gov. Inslee Warns Against Reopening Too Early
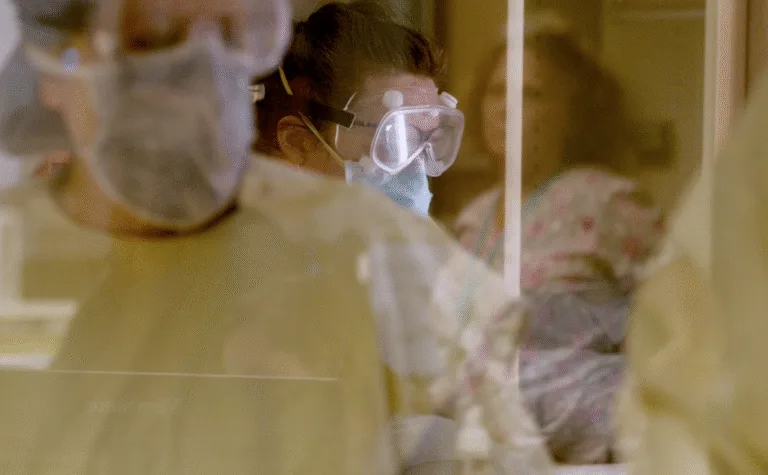
“No Good Choices”: At the First U.S. Hospital Network to Knowingly Battle the Coronavirus, a Struggle Over Protective Equipment
Related Stories

How Are We Preparing For the Next Pandemic?

5 Years Later, A Look Back at How the COVID-19 Pandemic Disrupted the World

The U.S. COVID Death Toll Has Passed 1 Million. These Documentaries Offer Context.

As the U.S. Crosses 500,000 Deaths from COVID-19, These 9 Documentaries Offer Context

Watch 2020’s 10 Most-Streamed FRONTLINE Documentaries

Awaiting Election Results, the U.S. Set a New Daily COVID Record. These 8 Films Offer Context.

Watch FRONTLINE’s 5 Most-Streamed Documentaries of 2020 (So Far)

Covering Coronavirus: A Midnight Rescue
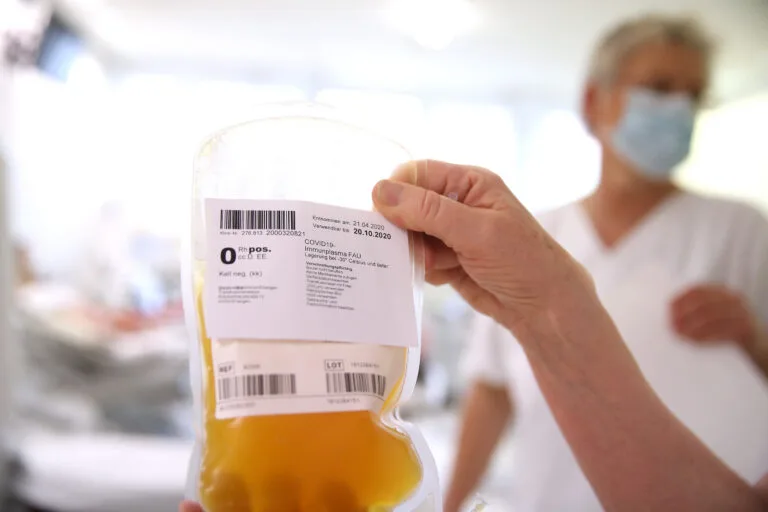
Blood Plasma Provides Possible Therapy for Covid-19 Patients
Coronavirus Pandemic

In Seattle, Early Help for Homeless Residents During the Coronavirus Outbreak

FRONTLINE’s First Major Documentary on COVID-19 Premieres Tonight

“No Good Choices”: At the First U.S. Hospital Network to Knowingly Battle the Coronavirus, a Struggle Over Protective Equipment

How America’s First Known Coronavirus Patient Recovered

Two Washingtons. Two Very Different Coronavirus Responses.

“We’ve Got to Double Our Efforts”: WA Gov. Inslee Warns Against Reopening Too Early

Covering Coronavirus: A Tale of Two Washingtons
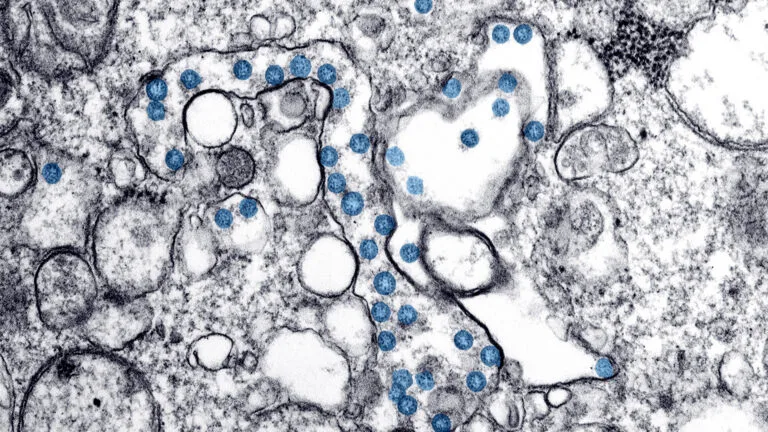
Covering Coronavirus: Seattle, Washington

“This Is the New Reality”: Reporting on the Coronavirus from Washington State

A Message About FRONTLINE’s Coronavirus Coverage From Our Executive Producer
Related Stories

How Are We Preparing For the Next Pandemic?

5 Years Later, A Look Back at How the COVID-19 Pandemic Disrupted the World

The U.S. COVID Death Toll Has Passed 1 Million. These Documentaries Offer Context.

As the U.S. Crosses 500,000 Deaths from COVID-19, These 9 Documentaries Offer Context

Watch 2020’s 10 Most-Streamed FRONTLINE Documentaries

Awaiting Election Results, the U.S. Set a New Daily COVID Record. These 8 Films Offer Context.

Watch FRONTLINE’s 5 Most-Streamed Documentaries of 2020 (So Far)

Covering Coronavirus: A Midnight Rescue

Blood Plasma Provides Possible Therapy for Covid-19 Patients
Coronavirus Pandemic

In Seattle, Early Help for Homeless Residents During the Coronavirus Outbreak

FRONTLINE’s First Major Documentary on COVID-19 Premieres Tonight

“No Good Choices”: At the First U.S. Hospital Network to Knowingly Battle the Coronavirus, a Struggle Over Protective Equipment

How America’s First Known Coronavirus Patient Recovered

Two Washingtons. Two Very Different Coronavirus Responses.

“We’ve Got to Double Our Efforts”: WA Gov. Inslee Warns Against Reopening Too Early

Covering Coronavirus: A Tale of Two Washingtons

Covering Coronavirus: Seattle, Washington

“This Is the New Reality”: Reporting on the Coronavirus from Washington State

A Message About FRONTLINE’s Coronavirus Coverage From Our Executive Producer
MAYOR JENNY DURKAN, (D) Seattle:
It was one of the most vibrant cities in America. Our economy was strong; the port, that was one of the leading ports in the country. We had one of the most vibrant restaurant scenes. Small businesses flourishing. And we went from that to almost zero overnight.
MILES O’BRIEN, Correspondent:
I arrived in Seattle in mid-March, a city and state in the process of shutting down before that was the norm in the rest of the country.
I’ve covered science stories for nearly 30 years, but this felt more like science fiction. The deadly disease, COVID-19, was about to bring the country and the world to its knees.
RYAN KEAY, M.D., Providence St. Joseph Health:
It’s like watching a slow-moving landslide move towards you.
MILES O’BRIEN:
How did it evade our warning systems? Our best science?
DOW CONSTANTINE, (D) King County Executive:
A lot of people died because we weren’t ready.
MILES O’BRIEN:
Why was our government so slow to act, so unprepared?
SCOTT SEDLACEK:
I haven’t cried ever as much as I have in the last week.
MILES O’BRIEN:
And what lies ahead?
MILES O’BRIEN:
I came to Seattle looking for answers. My first stop: Providence Regional Medical Center in nearby Everett.
FEMALE NURSE:
And have you traveled outside the U.S. in the last 30 days?
MILES O’BRIEN:
I have.
FEMALE NURSE:
So we’re going ask you to put on a mask.
MILES O’BRIEN:
OK.
This is the hospital that treated the first known case of COVID-19 in the country.
FEMALE NURSE:
There we go, 97.6.
MILES O’BRIEN:
I met Dr. George Diaz, an expert in infectious diseases who treated “patient one,” a 35-year-old local man who’d flown into Seattle on January 15.
GEORGE DIAZ, M.D., Providence Regional Medical Center Everett:
He was having cough, he had been having fevers at home, he hadn’t been eating well, he generally felt poorly and he had been complaining of diarrhea at home.
MILES O’BRIEN:
Now, he’s 35 years old and otherwise healthy.
GEORGE DIAZ:
Totally healthy person. He began developing symptoms the day after he arrived.
MILES O’BRIEN:
He went to this walk-in clinic and described his symptoms and told them where he had been for about six weeks: Wuhan, China.
MALE NEWSREADER:
A preliminary investigation into a mysterious pneumonia outbreak in Wuhan, China, has identified a previously unknown coronavirus—
MILES O’BRIEN:
That was a crucial detail.
FEMALE NEWSREADER:
The mysterious new pneumonia virus has sickened dozens of people—
MILES O’BRIEN:
For weeks, Wuhan had been the center of a growing storm—
MALE NEWSREADER:
Scientists in China are trying to determine if a new virus—
MILES O’BRIEN:
—as news trickled out about cases of a strange new pneumonia.
FEMALE NEWSREADER:
—still a lot that is unknown, the WHO has said—
MILES O’BRIEN:
In Seattle, a city known for cutting-edge medicine and technology as well as ties to Asia, officials told me they had been on alert.
DOW CONSTANTINE:
it clearly had the attention of our public health folks, and they in turn were starting to line up the other departments, starting with human services, about how we were going to respond when and if it arrived on our shores.
MILES O’BRIEN:
At the clinic where the man returning from Wuhan was seeking treatment, they took no chances.
GEORGE DIAZ:
At that point the clinic appropriately isolated him. The health district contacted the CDC, who advised testing, and fortunately that clinic had the appropriate gear to be able to safely test the patient. He was then advised to go home and quarantine.
MILES O’BRIEN:
The clinic sent a nasal swab they’d taken from the man to the Centers for Disease Control and Prevention in Atlanta.
GEORGE DIAZ:
And then within 24 hours, we had a call from the CDC saying that the test was positive and that they wanted us to admit him for observation.
MILES O’BRIEN:
The first COVID-19 patient had been confirmed in the United States.
Around 10 p.m. on January 20, “patient one” was brought to the Providence Regional Medical Center.
This is a photograph of his arrival, encased in what’s called an isopod, designed to keep a patient quarantined.
“Patient number one” arrived here in this?
GEORGE DIAZ:
He did. When we were going through the transportation plan with the ambulance company, they wanted to keep their staff safe. Completely contained, doesn’t allow any possibility of infection. So our patient was placed in this by EMS and brought to our hospital and unloaded in his room.
So, it took us about two hours from the time the CDC called for us to get all our staff, personnel, supplies and the facilities all in place to be able to give the EMS folks a green light to come in.
MILES O’BRIEN:
You did that in two hours?
GEORGE DIAZ:
In two hours. We were ready for it.
MILES O’BRIEN:
One of the reasons they were so ready: Less than three weeks earlier, Diaz and his colleagues had conducted an elaborate simulation: pandemic training.
GEORGE DIAZ:
We were aware of what was going on in Wuhan at that point, but it was part of our routine structure already to prepare.
MILES O’BRIEN:
You really had a go-to plan.
GEORGE DIAZ:
We had a game plan in place already. We had everyone involved, including the local EMS, those people that bring the patients from point A to point B; public health officials; and other partners we have in the community to drill. And so we had a variety of scenarios we went through.
MILES O’BRIEN:
By the time “patient one” was hospitalized, local public health officials were going into high gear.
SCOTT LINDQUIST, M.D., M.P.H., Washington State Department of Health:
The reason Washington state found that first case is we were ready for it. The ambulance service was ready, they knew the right personal protective equipment to wear. It was one of those absolute coordination between the health care, local health, state health and the CDC. It went perfectly. That’s how we were able to find the first case in the country.
MILES O’BRIEN:
It was a critical early warning sign that the highly contagious coronavirus could be spreading in the U.S. But in his first public comments, President Trump dismissed any threat to the rest of the country.
JOE KERNEN:
Have you been briefed by the CDC?
PRESIDENT DONALD TRUMP:
I have.
JOE KERNEN:
Are there worries about a pandemic at this point?
PRESIDENT TRUMP:
No, we’re not at all. And we’re—we have it totally under control. It’s one person coming in from China, and we have it under control. It’s going to be just fine.
JOE KERNEN:
All right. Safe travels—
PRESIDENT TRUMP:
Thank you.
MILES O’BRIEN:
In Seattle, doctors and scientists weren’t so sure. They didn’t have a way to test for coronavirus on their own. And while the CDC had been able to test the sample from “patient one,” it didn’t yet have a test it could deploy on a massive scale around the country.
GEORGE DIAZ:
The way to really know the burden of disease in your community is to be able to test. So the testing piece was a huge piece of the puzzle that we didn’t really fully—we weren’t fully able to address.
MILES O’BRIEN:
By early February, with the virus spreading around the globe, the World Health Organization was recommending test kits that had been developed in Germany. But U.S. officials made a fateful decision to go their own way.
JULIETTE KAYYEM, Former assistant secretary, Department of Homeland Security:
If you look at a moment when the United States may have lost its ability to control what’s happening, it begins with the decision early on in 2020 by the CDC not to utilize the test kits and the capabilities that were being shared by the World Health Organization and other nations.
MILES O’BRIEN:
The CDC wouldn’t talk to me on camera but told me they took the swiftest path, and using another nation’s test would have caused worse delays.
Former CDC Director Tom Frieden said the decision made sense.
TOM FRIEDEN:
There’s never been a time previously when there was a need to use a test from outside because the CDC system has not failed in the past.
MILES O’BRIEN:
The CDC began shipping its own test kits to public health labs around the country.
But in Seattle and elsewhere, it was quickly obvious that something was wrong. One of the three chemical probes was faulty, generating inconclusive results.
SCOTT LINDQUIST:
There was checks and balances within the test. And when we validate it—can it detect the virus and can it not overdetect it—that balance was not correct.
LAURIE GARRETT, Author, “The Coming Plague”:
Research and implementation laboratories said, “This doesn’t work. You’ve given us a bogus kit, and we’re not going to use it. Fix it, fast, or give us the right to use our own kits.”
MILES O’BRIEN:
At the University of Washington, I met virologist Alex Greninger, who’d been trying to do just that.
ALEX GRENINGER:
You got to have the supply of testing, absolutely do. We need to be able to detect where the virus is and then try and snuff it out, right? Prevent its transmission. That’s the name of the game in the coming months.
MILES O’BRIEN:
But he ran into a bureaucratic brick wall: The Food and Drug Administration had instituted emergency procedures to make sure any new tests were accurate.
ALEX GRENINGER:
You can make your own test, but you have to send it to the FDA and get it reviewed and then authorized. And I’ll admit, I’m in my first couple of years here in this particular job. I had not been through this process of before.
MILES O’BRIEN:
The FDA application was 28 pages long and required him to run tests that would take at least two weeks. And that wasn’t all.
ALEX GRENINGER:
One of the things is they needed a document FedExed across the country before they could look at the document.
MILES O’BRIEN:
You couldn’t electronically transmit it?
ALEX GRENINGER:
I could electronically transmit it, but they couldn’t look at it until it was FedExed. And then they changed that regulation.
And so from a couple days after February 4 all the way to February 26, they didn’t have a test. They were completely blind, too.
MILES O’BRIEN:
This had to be incredibly frustrating.
ALEX GRENINGER:
It was frustrating. It was.
So we try to prioritize things in the top tier—
MILES O’BRIEN:
The FDA told me it did review Greninger’s application, but it was incomplete. They also said they were balancing the need for tests with concerns about accuracy.
MALE NEWSREADER:
Major developments: a global health emergency as the coronavirus reaches its 20th country.
MILES O’BRIEN:
In Seattle and around the world, the clock was ticking.
MALE NEWSREADER:
The coronavirus is now considered a global health emergency, and the U.S. is warning people not to travel to China.
MILES O’BRIEN:
The WHO had declared a global emergency, and the CDC was beginning to screen passengers at U.S. airports, including Seattle.
PRESIDENT TRUMP:
We are coordinating with the Chinese government and working closely together on the coronavirus outbreak in China, relentlessly—
MILES O’BRIEN:
President Trump was still not raising alarms, though he banned foreign travelers from China.
PRESIDENT TRUMP:
My administration will take all necessary steps to safeguard our citizens from this threat.
MILES O’BRIEN:
But by that time, flights from the outbreak zone had been landing at U.S. airports for weeks.
JULIETTE KAYYEM:
The travel ban may have bought us some time, but in all actuality, people were leaving Wuhan, going to Beijing, traveling to Western Europe and ultimately to the United States in late 2019 and early 2020 anyway.
FEMALE NEWSREADER:
Chinese health officials said today another 46 people have died from the coronavirus—
MILES O’BRIEN:
In those critical first weeks after the arrival of the virus in the U.S., administration officials—and the president himself—continued to insist that the risk was small.
ROBERT REDFIELD, M.D., Director, CDC:
I want to emphasize that this is a serious health situation in China, but I want to emphasize that the risk to the American public currently is low.
SEAN HANNITY:
How concerned are you?
PRESIDENT TRUMP:
Well, we pretty much shut it down coming in from China. We’ve offered China help, but we can’t have thousands of people coming in who may have this problem, the coronavirus. So we’re going see what happens, but we did shut it down, yes.
MILES O’BRIEN:
That attitude didn’t sit well with Washington’s senior Democratic senator, Patty Murray. She spoke to me from her home.
SEN. PATTY MURRAY:
I felt like at the time I lived in two different worlds. I lived here in Washington state, where people were going, “Oh, my gosh, we have a problem,” and in Washington, D.C., where they’d say, “Oh, you guys worry too much out on the West Coast.”
MILES O’BRIEN:
A tale of two Washingtons.
PATTY MURRAY:
Yeah. We should have pulled out all the stops and checked everything, but it was more like, “Oh, you guys, quit worrying out there.”
MILES O’BRIEN:
There was a lot to worry about. In isolation at Providence Hospital, “patient one” was deteriorating.
GEORGE DIAZ:
He began developing more shortness of breath. And because of that we got an X-ray, which looked like he had a developing pneumonia. His oxygen levels in his blood were also decreasing.
MILES O’BRIEN:
That worried Dr. Diaz, who’d been following the dire medical reports out of Wuhan.
GEORGE DIAZ:
It appeared, based on their data, that once patients begin developing pneumonia that many of them end up in the ICU on a ventilator and die.
MILES O’BRIEN:
“Patient one” was slipping fast, and there was no known treatment.
Dr. Diaz told me he heard about an antiviral drug called remdesivir that some experts thought could potentially help. It would be an experiment, he said, but the patient was willing.
GEORGE DIAZ:
At that point, I contacted the FDA and Gilead, the manufacturer, to see if they would approve it. So, the FDA gave us an approval to try it on compassionate use basis, knowing that it had not been approved yet and that there were no trials available to base that decision on.
We infused it the next day. He was still having very high fevers and still was requiring oxygen the day that we gave it to him.
By the next day, his fevers resolved and they stayed gone. He felt much better. He felt like he had started beating the virus.
MILES O’BRIEN:
No one knew if the drug had an impact or if the virus was taking its natural course.
Here’s the thing: You have one data point here.
GEORGE DIAZ:
One person.
MILES O’BRIEN:
Right.
GEORGE DIAZ:
In the world.
MILES O’BRIEN:
Yeah, in the world.
GEORGE DIAZ:
It is an anecdote, and so we were happy that the patient got better and was ultimately to continue to get better and able to go home. So that part was fantastic for the patient. We knew that we needed to study this in a formal clinical trial.
MILES O’BRIEN:
Although “patient one” was well enough to be sent home, for public health officials in Washington state, there were many more questions to answer.
They needed to find out who “patient one” might have come in contact with after returning from China and send samples from them to the CDC, as well.
SCOTT LINDQUIST:
So, we find contacts, someone that you spent at least 10 minutes of time talking face to face with.
We identified 60-plus contacts. We swab them multiple times to see was there transmission of this virus, and we found absolutely no transfer amongst those contacts that this first case had.
MILES O’BRIEN:
Washington’s governor, Jay Inslee, remembers this as a brief, optimistic moment. I interviewed him remotely from his office at the state capital.
GOV. JAY INSLEE, (D) Wash.:
What we were thinking is we were very much on top of it because we did very extensive contact tracing with all of the contacts that the person had who was the first patient, and did everything epidemiologically that you could ask a public health system to do.
MILES O’BRIEN:
But soon, more signs of trouble began to appear across Lake Washington in the city of Kirkland, at the Life Care skilled nursing and rehab center.
Scott Sedlacek had brought his 86-year-old father there to recover from a bad fall.
SCOTT SEDLACEK:
He hit his head hard enough that he had some brain trauma and bleeding on the brain and he broke his right ankle. And the bed that opened up was at Life Care, and so, on February 20, we moved my dad to Life Care. And then we started seeing some of the staff wearing respiratory gear, wearing face masks, wearing gloves. It was kind of like, “What’s going on?”
MILES O’BRIEN:
Inside Life Care, residents had been getting sick with an unknown respiratory infection. The sickest were brought to the nearby EvergreenHealth Medical Center.
Dr. Francis Riedo is the medical director of infection control here.
FRANCIS RIEDO, M.D., EvergreenHealth:
Remember, this was flu season and we’d already had a peak of influenza B in December, and now we were going through the peak of influenza A. And so, the unit was full of individuals with severe respiratory infections.
In the meantime, in the background, we’re watching these events unfold with increasing alarm, not only in Wuhan, but now spreading across the globe and wondering when our turn was coming.
MILES O’BRIEN:
Until that point, federal guidelines for testing potential cases were very narrow—patients had to have been in a hot spot like China or in contact with someone infected.
Then, the rules changed. Dr. Riedo wasted no time.
FRANCIS RIEDO:
We settled on two individuals and we tested them the following morning. I had a regular day, saw patients in clinic, saw patients in the hospital, was sitting there as I usually do trying to complete my notes and received a call at 7:40 p.m., and both of the tests were positive.
MILES O’BRIEN:
What goes through your mind?
FRANCIS RIEDO:
My initial honest response was skepticism. I thought, the odds of both tests in two randomly selected individuals being positive, with no history of travel, no history of exposure to anybody, was fairly astronomical.
This was a huge shift. Incident command was activated, and we made a quick decision to test nine additional people that night. Eight of those nine were positive.
MILES O’BRIEN:
Wow.
FRANCIS RIEDO:
Right.
MILES O’BRIEN:
Kind of stunning, actually, isn’t it?
FRANCIS RIEDO:
It was. And within the first five days we had 32 positives.
MILES O’BRIEN:
Many were from Life Care, but crucially, some had no connection to the nursing home.
FRANCIS RIEDO:
We then knew that this was a much bigger outbreak than you could have imagined.
MILES O’BRIEN:
At least 41 Life Care residents and two visitors would eventually die, with more than a hundred others linked to the home testing positive, including Scott Sedlacek’s father, Chuck.
SCOTT SEDLACEK:
He has never shown symptoms.
MILES O’BRIEN:
So, how worried are you that symptoms might appear?
SCOTT SEDLACEK:
Extraordinarily. Because we don’t know. This is new. It’s uncharted waters.
MILES O’BRIEN:
The Sedlacek story hit home for me: My 84-year-old father is in assisted living in Florida.
Hello there! Can you tilt down a little bit?
MILES O’BRIEN’S FATHER:
I’m sorry, what?
MILES O’BRIEN:
Tilt down. Tilt down. A little more down. There you go, that’s good. How are you feeling?
MILES O’BRIEN’S FATHER:
Why, I’m fine, how are you?
MILES O’BRIEN:
No coronavirus so far, but he’s pretty much in isolation—no visitors allowed.
It’s the same at Life Care, but the Sedlaceks have found a way around that.
SCOTT SEDLACEK:
My sister’s here, and we’ll go up and we’ll say hi through the window. We brought a big white board today so we can actually write notes for him because they’re double-pane windows to seal the noise out. [Laughs]
Can you hear us? [Laughs]
SCOTT SEDLACEK’S SISTER:
OK, we’ll let you finish, then. Love you!
SCOTT SEDLACEK:
Keep getting better. Keep listening to the nursing staff. They’re looking out for you.
He has to get the love from the family to get better. Without it, he will become not just physically but mentally ill. It’s the worst thing you can do to an older person. The worst thing you can do.
MILES O’BRIEN:
Scott himself also got the virus. Unlike his dad, he got sick.
SCOTT SEDLACEK:
I was hospitalized through the emergency room with the full-blown list of symptoms, extraordinary difficulty breathing, light-headed, dizziness. You name the symptom, I had it.
MILES O’BRIEN:
What was it like being in isolation, sick with this disease? Were you scared?
SCOTT SEDLACEK:
Hell yes, I was scared. It’s an unknown. I was hooked up to an IV and they started an albuterol nebulizer, which they had to give two full rounds of it, but after those two full rounds I was breathing normally, and after six hours, they had all my symptoms under control. Within 12 hours, they moved me to a full isolation unit, and 10 hours later, they released me with zero symptoms.
MALE NEWSREADER:
But the number of coronavirus cases at home and abroad continue to climb, the financial markets rocked and more-aggressive steps to fight the spread—
MILES O’BRIEN:
By this time in early March, COVID-19 cases were multiplying, here and around the country.
MALE NEWSREADER:
Breaking news: Washington is in a state of emergency—
MILES O’BRIEN:
Gov. Inslee had put Washington under a state of emergency—
FEMALE NEWSREADER:
Washington state has declared a state of emergency—
MILES O’BRIEN:
—the first governor to do so.
MALE NEWSREADER:
—the governor declaring a state of emergency.
MILES O’BRIEN:
But like many here, he was increasingly concerned that President Trump was continuing to downplay the threat.
PRESIDENT TRUMP:
It’s going to all work out. Everybody has to be calm. It’s all going to work out.
MILES O’BRIEN:
Inslee, a Democrat and former presidential candidate, tweeted that the administration should stick to science and tell the truth. It would ignite an escalating war of words.
During a visit to the CDC, Trump fired back.
PRESIDENT TRUMP:
—because that governor is a snake, OK? Inslee. Let me just tell you, we have a lot of problems with the governor and—the governor of Washington, that’s where you have many of your problems.
I said, no matter how nice you are, he’s no good. That’s the way I feel. Goodbye.
MILES O’BRIEN:
At that point, did you get the sense that you as governor and the state of Washington were sort of on their own and the federal cavalry was not coming?
JAY INSLEE:
Yes, but we didn’t ever depend on that leadership coming out of the White House, so it’s not something that we were surprised by. We always knew that we would have to lead the charge, given the president’s reluctance to really exercise leadership on this. And we sort of knew that he had an intent of downplaying what was an emerging problem that could only be explained by someone who had their eye on the Dow Jones rather than an eye on the epidemiological curve.
MILES O’BRIEN:
Seattle’s mayor, Jenny Durkan, shared those sentiments.
MAYOR JENNY DURKAN, (D) Seattle:
We are not going to be distracted by any rhetoric that the president or anyone else uses. We’ve got to act. We’ve got to act to protect the people, and I think those actions are what matters.
Facts and science. Got to rely on them. That’s the only thing that’s going to get us through this, and fortunately, we’ve got a really vibrant health and science community here in the state of Washington and Seattle, and we listen to them.
MILES O’BRIEN:
She and other political leaders here had some hard decisions to make after hearing grim predictions.
JENNY DURKAN:
We had researchers here telling us that within six weeks, we would have over 70,000 positive cases and hundreds of deaths if we didn’t act. And so we had a choice to make. The choice was know that you’re going to have enormous pain in shutting down parts of your economy, or have those same impacts later and overrun your health system.
As we move forward it will be increasingly necessary and important that we are unified in our efforts.
MILES O’BRIEN:
Seattle was starting on a trajectory that the rest of the country would soon follow.
JAY INSLEE:
There is no magic silver bullet at the moment medically, but there is a very successful effort that we can take to slow the spread of this disease, and that’s to reduce the social interactions that are not necessary in our lives.
MILES O’BRIEN:
You, the county executive and the governor were early out of the box on taking these actions, pretty proactive. Did you feel at the time a little nervous about all that?
JENNY DURKAN:
I think it was—all of us felt a great deal of sense of obligation and concern because we were the first to go.
MILES O’BRIEN:
Mayor Durkan actually had a pandemic response plan on the shelf, which she and her cabinet had updated in early February.
JENNY DURKAN:
We pulled out the pandemic planning and knew that one of the first things we had to do to separate people from one another was have them telecommute, those that could, so our largest employers acted immediately.
MILES O’BRIEN:
That included Seattle icon Microsoft, with a workforce of more than 50,000, one of the largest private-sector employers in the region.
BRAD SMITH:
So, we had a call on Sunday afternoon, March 1. We had the business leaders from the largest employers—
MILES O’BRIEN:
Microsoft President Brad Smith spoke to me from his home.
BRAD SMITH:
So we went from Monday, telling people they should work from home if they were more comfortable; Tuesday, telling people feel free to work from home, it might be better; to Wednesday, work from home unless it is essential you come to work.
MILES O’BRIEN:
The decision you made was a big one. Did you hesitate?
BRAD SMITH:
No, it was interesting. Once we decided at Microsoft that we would be decisive and base our decisions on public health advice, then we knew what to do.
JENNY DURKAN:
It’s the hardest decision I’ve ever had to make because all of our instincts are to grow the whole economy for your city, to make a stronger community for everyone. And what we’re saying is, we’ve got to stop that kind of community and we have to stop doing work.
MILES O’BRIEN:
Almost overnight, the vibrant city shut down. Businesses closed. Storefronts boarded up. Empty restaurants. The famous Pike Place Market, nearly deserted.
At a local soccer field usually filled with kids and families, preparations for a surge of COVID patients.
DOW CONSTANTINE:
We knew already that one of the biggest challenges would be having the hospital system overwhelmed by way of cases. We were trying to figure out how we could get testing. We were trying to figure out whether we would receive material help in the form of field hospitals or large facilities, encampments for people who were unhoused. And there wasn’t a lot of concrete offers of help coming from the federal government.
So, we were left with the reality that we’re going to have to take on a lot of this ourselves.
FEMALE NEWSREADER:
More than 140 people lost their lives yesterday, bringing the death toll to over 590 in this country.
GOV. J.B. PRITZKER, (D) Ill.:
He’s not doing everything he can do.
MILES O’BRIEN:
As coronavirus was sweeping the country throughout March—
GOV. CHARLIE BAKER, (R) Mass.:
And I can’t tell you how frustrating it is.
MILES O’BRIEN:
—so was the frustration among governors scrambling for resources they needed to respond.
GOV. GRETCHEN WHITMER, (D) Mich.:
We’re bidding against one another. It’s really not a great system.
GOV. LARRY HOGAN, (D) Md.:
The states are taking action to try to find these things on our own, and we’re also—
MILES O’BRIEN:
The president was now feuding with multiple governors.
GOV. ANDREW CUOMO, (D) N.Y.:
Four hundred ventilators? I need 30,000 ventilators.
MILES O’BRIEN:
And like he’d done with the virus in the beginning—
PRESIDENT TRUMP:
I don’t believe you need 40,000 or 30,000 ventilators.
MILES O’BRIEN:
—he disputed there was a scarcity of crucial medical equipment like masks and ventilators.
PRESIDENT TRUMP:
Many of the states are stocked up. Some of them don’t admit it, but they have—we have sent so many things to them, including ventilators.
MILES O’BRIEN:
Amid the feuding, doctors and nurses have struggled to get the personal protective equipment, PPE, they need.
AMY COMPTON-PHILLIPS, M.D., Executive VP, Providence St. Joseph Health:
Good morning and welcome, everyone!
MILES O’BRIEN:
In Seattle, that’s been the top issue for Dr. Amy Compton-Phillips, the chief clinical officer of the Providence Hospital Network.
AMY COMPTON-PHILLIPS:
Last year across all of Providence we used 250,000 masks. In the first three months of this at Everett, they’ve used 250,000 masks. We cannot have our own caregivers going down from COVID while they’re trying to take care of the community, because you know the supply chain is just not keeping up with our needs.
FEMALE VOICE [on phone]:
Amy, I have to say if I can’t assure them that they’re safe, then I don’t think the rest of this is worth anything.
MILES O’BRIEN:
Inside Providence’s emergency department, tensions around PPE had been high. Dr. Ryan Keay is the department’s medical director.
RYAN KEAY, M.D., Medical director, emergency department:
It’s exhausting to constantly think about the sequence that you put things on and take things off and where you’re sanitizing during that sequence. Every nurse, every tech, every physician I’ve talked to has said, “I’ve been working for years and I’ve never been so exhausted.” And it leaves people just on edge all the time.
We have enough N95 masks that people should not have to be able—should not have to bring in their own masks at this point in time.
FEMALE PHYSICIAN [on phone]:
Is the recommendation still one N95 per five patients, or are we using these the whole shift now?
RYAN KEAY:
We’re using them with a face shield for as long as you need to use them. You just store them in a paper bag until they become moist or soiled.
FEMALE PHYSICIAN [on phone]:
OK, so, forever.
RYAN KEAY:
Well, not forever. [Laughs]
MILES O’BRIEN:
Reusing masks and storing them in paper bags wasn’t the only DIY workaround I saw. I caught up with Dr. Compton-Phillips at the otherwise-vacant Providence headquarters. Inside a large meeting room, she and a handful of her team were spread out a safe distance cranking out face shields.
KAREN BOUDREAU, M.D., Senior VP, Providence St. Joseph Health:
Our caregivers would normally have protective goggles on and a surgical mask underneath this and then this goes in front and basically protects against droplets.
MILES O’BRIEN:
They had raided a half-dozen craft stores to scrounge up supplies.
KAREN BOUDREAU:
We’re at 288 now, we’re going to get to 1,000 by tomorrow.
We’re retooling our resources, going in to war against COVID.
FEMALE MEDICAL STAFF:
I feel like Rosie the Riveter.
FEMALE MEDICAL STAFF 2:
—499, 500! Woo-hoo! Good job, guys.
MILES O’BRIEN:
On the one hand, this is really—it’s kind of heartwarming. But it’s also really sad.
AMY COMPTON-PHILLIPS:
Desperation? [Laughs]
MILES O’BRIEN:
Yeah, I can’t decide which way to go in this. What are your thoughts?
AMY COMPTON-PHILLIPS:
I would rather offer our caregivers something than nothing, and at the moment, if the choice is not having PPE or having homemade PPE, were going to offer them homemade PPE. So.
MILES O’BRIEN:
That’s what motivated Jeff Kaas. His small family business builds and sews furniture for aviation and retail customers. He decided to pitch in and start making masks.
MILES O’BRIEN:
There’s not a shortage of the raw materials, at least. That would be bad. Or not yet, anyhow.
JEFF KAAS, President, Kaas Tailored:
Well—there will be. Yeah, there will be, yeah. So I think we’ve enough to make 2 million masks.
MILES O’BRIEN:
But how long will that take you to do?
JEFF KAAS:
Well, it depends on how fast we want to go.
MILES O’BRIEN:
How fast do you want to go?
JEFF KAAS:
We’re going to solve the problem.
My assumption is that we’ll be ramping up for several weeks and then drop off a cliff. Nobody will need me in the health care business anymore and then survival becomes a question for my company. So that’s probably the next scary thing, which is less scary than what our health care friends are going through right now. That’s the bigger issue for me.
JULIETTE KAYYEM:
We knew in January what we would need. We knew we would need gloves and masks and respirators and ventilators. Two and a half months later, we’re dependent on sewing circles to supply our frontline heroes with what they need. It may be a nice American story. I find it pathetic.
MILES O’BRIEN:
Washington state officials, like others in the country, say this was an avoidable crisis.
JENNY DURKAN:
Because we’ve lacked the federal leadership we needed, it’s been mayor versus mayor, city versus city, state versus state, trying to get access to the limited resources to protect our communities. Whether it’s ventilators or masks for our health care workers, all of that has become this “Hunger Games” process where everyone’s trying to figure out a way to outbid each other. Washington state had a line on masks that were coming into the country, and at the port in California, suddenly multiple states were bidding on them. That shouldn’t be the way that it happens.
JAY INSLEE:
We’re searching the world for every potential warehouse that have any of this personal protective equipment. That has been a constant struggle, and we are bidding against each other, and I’m sure that the suppliers are having a field day bidding the price up while states are bidding against one another. It would be much more efficient, economically and otherwise, if the federal government was playing a more vigorous role in that regard.
MILES O’BRIEN:
The tensions between states and the federal government had been escalating.
MALE NEWSREADER:
Another 5 million Americans file for unemployment benefits last week, and that would bring the total—
MILES O’BRIEN:
Not just over the response to the outbreak—
FEMALE NEWSREADER:
—see market down 10% in relatively short order. There’s a lot of bad news still to come.
MILES O’BRIEN:
—but now over what it will take to get the country up and running again.
FEMALE NEWSREADER:
This is a massive meltdown on a national scale.
MALE NEWSREADER:
—with more jobs lost in a matter of two weeks than in the entire 18 months of the Great Recession.
PRESIDENT TRUMP:
Our team of experts now agrees that we can begin the next front in our war, which we are calling Opening Up America Again.
MILES O’BRIEN:
The president has been pushing governors to reopen soon, even as soon as May 1.
PRESIDENT TRUMP:
Our country has to get opened, and it will get open, and it’ll get opened safely and hopefully quickly.
MILES O’BRIEN:
But some of them have been pushing back.
GOV. PHIL MURPHY, (D) N.J.:
We cannot be guided by emotion. We need to be guided by where the facts on the ground, science and public health take us.
J.B. PRITZKER:
What’s best for the people of Illinois, their safety and health, and listening to the scientists and the doctors.
ANDREW CUOMO:
Because if you do it wrong, it can backfire.
MILES O’BRIEN:
And many, like Inslee, say it will come down to one thing: mass testing.
JAY INSLEE:
This is the No. 1 challenge for the United States right now, is we need a huge ramp up of our testing capacity, even greater than was needed early in the outbreak.
MILES O’BRIEN:
To increase testing, Inslee says Trump needs to order U.S. industry to help using the Defense Production Act, which the president has only just begun to do.
JAY INSLEE:
We need the president to help ignite a national mobilization of the manufacturing base of the United States. That is absolutely imperative so that we can restart our economy.
MILES O’BRIEN:
But President Trump has also thrown this back on the states.
PRESIDENT TRUMP:
The governors are responsible. They have to take charge. They have to do a great job.
MILES O’BRIEN:
There are limits to what a state can do, though, as I saw at Washington’s Health Department laboratory. They can only complete about 300 tests a day, and that requires a mad scramble. The raw materials for test kits are hard to come by.
SCOTT LINDQUIST:
We have a lot of testing lab capability, but we don’t have the equipment to swab everybody’s nose. I think the current status in Washington state is limited by the supplies to actually run the test.
MILES O’BRIEN:
They also don’t have enough PPE for the health care workers administering the tests.
SCOTT LINDQUIST:
If we don’t have enough gowns, gloves, masks to treat patients, how are we going to prioritize a gown, a glove and a mask to swab somebody? Because that is the requirement.
MILES O’BRIEN:
The state Health Department isn’t alone in struggling to meet the demand.
ALEX GRENINGER:
We can’t have that level of cross-contamination.
MILES O’BRIEN:
After getting approval for his test from the FDA, Alex Greninger has dramatically ramped up testing at the University of Washington School of Medicine Virology Lab.
ALEX GRENINGER:
For inpatients, health care workers, institutionalized populations, but mostly inpatients and people who needs supportive care, we’ve got to get that fast turnaround time that reduces the use of protective—
MILES O’BRIEN:
Because they’re in the hospital.
ALEX GRENINGER:
Yes.
MILES O’BRIEN:
On this day they completed about 3,000 tests.
ALEX GRENINGER:
To get 3,000, 4,000, 5,000 specimens a day, it takes a lot of focus.
MILES O’BRIEN:
Just like in the state lab, Greninger says it is difficult to get the raw materials he needs.
One of the hardest things to find: the single-use plastic tips that contain the chemicals and the specimens.
ALEX GRENINGER, M.D., Ph.D., University of Washington School of Medicine:
Some automated pipetters use four tips a test, and others use three, so, just getting the tips into your facility so we can run that many tests.
This is what we’re looking for, basically. We tweeted at Roche and the world to get these things in, like you would tweet like Delta had lost your bags or something like that, right?
I mean, we have two people whose entire job right now is to manage our FedEx shipments. Basically, we blow up our hallway and it goes down to a single file. And then it takes over the next six to eight hours we’re able to actually move those boxes into our local warehouses—we bought other space here in the building. It’s—the supply chain has been really the No. 1 thing we do.
MILES O’BRIEN:
Despite the problems, they’re still managing to return results the same day, in many cases.
This is crucial to keep up with a fast-moving virus and help health care workers on the front lines reduce their need for personal protective equipment.
ALEX GRENINGER:
When you send a test for COVID-19, you have to treat the person as if they are infected until we give you a result says they aren’t. And during that time you have to use all the personal protective equipment. So the speed at which we get those test results back allows us to conserve our personal protective equipment. It really touches so many things.
MILES O’BRIEN:
So what do you envision the coming months?
ALEX GRENINGER:
I think personally, right now, this will be with us for some time. A long time. There’s no magic bullet just yet.
MILES O’BRIEN:
This testing marathon could go on for at least a year—that’s how long experts say it could take to develop vaccines.
In the meantime, researchers are racing to finish clinical trials of several therapeutic drugs, including that promising antiviral, remdesivir, the one that seemed to work so well on “patient one.”
GEORGE DIAZ:
So he is on a trial?
FEMALE NURSE:
Yep, he’s on trial. He started on the 15th; so we’re on Day Two.
MILES O’BRIEN:
Dr. Diaz is now leading one of the trials with patients at Providence Hospital.
GEORGE DIAZ:
These are still anecdotes because we haven’t seen the full study being completed, but we’re certainly very optimistic. We want to get these questions answered as fast as possible.
MILES O’BRIEN:
And there may be another way to help people fight off the coronavirus: using the blood of COVID survivors themselves.
ELIZABETH SCHNEIDER:
Hello!
MILES O’BRIEN:
Hey, Elizabeth, looks like you’re on the mend.
ELIZABETH SCHNEIDER:
Yeah, I’ve been recovered now for—
MILES O’BRIEN:
People like Elizabeth Schneider. She was getting ready to become the first person in Seattle to donate her plasma to researchers trying to see what natural resistance she might have developed and whether she can share it.
ELIZABETH SCHNEIDER:
Scientists don’t know how long we have that immunity for this particular virus. But signs so far look like we will have immunity.
MILES O’BRIEN:
Survivors’ blood as therapy. It’s not a new idea—doctors used it in 1918 in the midst of the Spanish flu pandemic.
ELIZABETH SCHNEIDER:
I do feel a little more sense of security going out and doing my day-to-day tasks because I’ve already had this.
MILES O’BRIEN:
She was among the first documented COVID-19 cases in the U.S. A microbiologist who works for a biotech company, she came down with flu symptoms on February 25, three days after attending a party.
On Facebook she learned many of her friends who were there were also sick—15 in all. She told me she and seven others ultimately tested positive for COVID-19.
Which brought her to this moment on this morning, to the blood bank in downtown Seattle.
ELIZABETH SCHNEIDER:
Hi, I am here for plasma donation.
MILES O’BRIEN:
The coronavirus antibodies in her plasma may be a way for others to fend off the virus. It’s called “convalescent plasma therapy.”
MALE MEDICAL WORKER:
Our goal is to get to 840 milliliters today.
ELIZABETH SCHNEIDER:
I’m hoping that some of my plasma ends up in another patient who is suffering from COVID-19, and this could potentially save their life.
MILES O’BRIEN:
There are now signs that COVID cases may be plateauing in some places, like here—
JAY INSLEE:
We have had some success flattening the curve. That has taken place—
MILES O’BRIEN:
—but also spreading to new areas of the country. Washington state recently returned more than 400 ventilators it received from the national stockpile so they could be used where they’re needed more.
MALE NEWSREADER:
Gov. Inslee today announced that 400 ventilators would be leaving the state of Washington and going back to—
MILES O’BRIEN:
But in recent days—
FEMALE NEWSREADER:
Trump’s back-and-forth with governors—
MILES O’BRIEN:
—President Trump’s feud with governors has become an all-out war—
FEMALE NEWSREADER:
In a series of tweets he exclaimed “liberate Minnesota, Michigan and Virginia.”
MILES O’BRIEN:
—encouraging protests against social distancing restrictions.
FEMALE NEWSREADER:
—seeing these protests at state capitals—
MILES O’BRIEN:
Even in Washington state.
FEMALE NEWSREADER:
—gather today in Olympia, demanding that the governor act now.
MALE NEWSREADER:
—this protest in Olympia is the latest in a wave of demonstrations—
PRESIDENT TRUMP:
These are people expressing their views. I see where they are, and I see the way they’re working. And they seem to be very responsible people to me.
FEMALE NEWSREADER:
The governor of Washington state says the president may be inciting violence.
MILES O’BRIEN:
In his own tweets, Gov. Inslee said Trump was “unhinged,” “off the rails” and “fomenting domestic rebellion.”
When I talked to Gov. Inslee, he told me it’s no time to be rushing to reopen.
JAY INSLEE:
All leaders have the biggest challenge to make sure people understand that as the sun comes up and the daffodils come out, we’ve got to double our efforts. Because if you relax too soon, the curve just can rebound and start right back up again. And the most dangerous element in my state today is the virus of complacency, because we have to be just as diligent for the next several weeks as we were the last several weeks.
MILES O’BRIEN:
I wanted to know what pandemic modeler Chris Murray thought of all of this. He runs the Institute for Health Metrics and Evaluation at the University of Washington.
DEBORAH BIRX:
I think if you ask Chris Murray, he would say—
MILES O’BRIEN:
Its models are often cited by President Trump’s Coronavirus Task Force.
So, really, when you think about it, Chris, there’s no scenario of going forward that you can envision that doesn’t demand mass testing, if not testing for everyone.
CHRISTOPHER MURRAY, Ph.D., Director, University of Washington IHME:
The issue will be the capacity to test—how many tests are practically feasible come June, state by state. And it may not be anywhere near enough to be able to do full-scale mass testing. So then if you take measures off May 1, there’s a pretty quick rebound, so by mid-July we’d be right back to where we are now.
MILES O’BRIEN:
Really? Exactly the rate of death and hospitalization that we’re dealing with—
CHRISTOPHER MURRAY:
Pretty much, yeah. So, we’re not going to want to take off measures May 1, let’s put it that way.
PRESIDENT TRUMP:
And the second wave won’t be like the first wave.
MILES O’BRIEN:
That the president isn’t heeding scientific warnings, once again, is causing alarm among those who’ve been dealing with the outbreak since the beginning.
SEN. PATTY MURRAY, (D) Wash.:
I am pessimistic about the next few months. I think it’s going to be really hard, and we need to ramp up, ramp up, hurry. We need a leader at the top who’s willing to go well beyond where he is right now in saying, “Here’s what we need to do in terms of testing and giving people the information they need to get the economy going.” Long-term, I’m optimistic, but it’s a long ways between here and there.
MILES O’BRIEN:
I went back one last time to where the outbreak took hold here, Evergreen Hospital, where those patients from the nursing home were treated in February. It is an apt window into where Seattle and the country are right now.
I met a woman who was recovering from COVID-19, Rosanne Eskenazi.
MAURY ESKENAZI:
How are you? I want to give you a kiss and stuff, but I can’t.
ROSANNE ESKENAZI:
Nope.
MILES O’BRIEN:
At 63, with an immune system disease, her chances of living to see her husband Maury again were not good.
MAURY ESKENAZI:
When they put her on the ventilator, I never thought I’d see her again, and I wasn’t reading about people that were surviving this and coming out of this so I was—it was over.
ROSANNE ESKENAZI:
I don’t even know how many weeks it was, but I don’t remember a lot.
MAURY ESKENAZI:
When we brought her—when the day came that she had—she looked horrible. Her temperature was horrible.
ROSANNE ESKENAZI:
What, it was like 105?
MAURY ESKENAZI:
It was 105.
MILES O’BRIEN:
Oh, my God, really?
MAURY ESKENAZI:
And she was coughing and we had the ambulance come. They sent two ambulances. This was the beginning of the COVID.
MILES O’BRIEN:
You didn’t really fully appreciate how bad it was, did you, because you were kind of out of it?
ROSANNE ESKENAZI:
Yeah, I was out of it. I saw my parents—my dead parents—when I was here. I don’t know whether—I was saying, I don’t know whether it was a dream or a hallucination.
My parents were here and they were sitting across from me and they all said, “You’re going to be OK. Everything’s going to be OK. You’re going to be OK, and if something happens, your children will be fine. Everything’s going to be great. You have all this family and stuff, so, don’t worry.” And it really helped me not worry.
Oh, there, it says silver that way.
MAURY ESKENAZI:
Yeah, sorry.
ROSANNE ESKENAZI:
Yeah.
MILES O’BRIEN:
Rosanne was on her way home—
ROSANNE ESKENAZI:
Bye!
MILES O’BRIEN:
—but there were others still coming in, needing urgent attention.
I met critical-care and pulmonary physician Michael Bundesmann, who was focused on one particular patient.
MICHAEL BUNDESMANN, M.D., EvergreenHealth:
This is a person who has multi-organ failure and ultimately required mechanical ventilation. And now needs dialysis, kidney replacement therapy. They’re in shock.
MILES O’BRIEN:
Three days earlier, he’d been awake, alert, joking with his doctors.
MICHAEL BUNDESMANN:
Patients come in and they look OK on one day, and some of them are OK to be discharged from the emergency room, and come back a few days later much more sick. That degree of unpredictability I think is very unsettling for everybody.
MILES O’BRIEN:
Dr. Bundesmann says the pace has slackened some since the darkest days.
MICHAEL BUNDESMANN:
We could feel the curve flatten a few days ago, probably even last week. And it’s allowed us to be able to see patients and take care of them at a pace that’s a little bit more used to what our ICU can handle, volume-wise, and it’s certainly made a big difference.
MILES O’BRIEN:
What do you see ahead?
MICHAEL BUNDESMANN:
We are now I think at a stage where I think that we can keep this pace that we have going, and that’s a good thing because of how many people are still susceptible to this infection. It’s going to be a long haul, I think.
Some of the things that worry us are what happens when there’s a next large outbreak in a skilled nursing facility, the next time a susceptible population gets hit within a tight community.
I don’t know when that’s going to happen. I think that until there is some degree of herd immunity, there are going to be people out there who have be planning this out very carefully and cautiously—when people can start returning to work, who can start returning to work and what time frame. Because as that happens, the cases are going to start to pick up again, and we have to be there and be able to support them as best as possible without stretching the capacity of our health care system.
Tough decisions for those people who have to make them.
MILES O’BRIEN:
There have now been more than three-quarters of a million confirmed COVID cases in the U.S., more than 40,000 deaths. What began as a public health crisis here with “patient one” has become a national crisis over response, over science and politics and decisions with devastating consequences.
It’s still a tale of two Washingtons, the story that I found when I arrived. But it’s also a tale of Washington and the states, and how the country will emerge from the crisis.
WRITTEN, PRODUCED & DIRECTED BY Miles O’Brien
PRODUCED BY Caleb Hellerman Kate McMahon
CO-PRODUCED BY Fedor Kossakovski Megan Robertson Will Toubman
CORRESPONDENT Miles O’Brien
SENIOR PRODUCER Frank Koughan
ARCHIVE PRODUCER Megan Robertson
EDITED BY Brian Truglio Steve Audette, ACE Dickran H. Manoogian
DIRECTOR OF PHOTOGRAPHY Ezra Wolfinger
COORDINATING PRODUCER Suzi Tobias
ORIGINAL MUSIC John E. Low
CAMERA Jason Longo Jason Greene Kate McMahon
SOUND Kent Romney
ASSISTANT EDITORS Alex LaGore Kenzie Audette Tim Meagher
DRONE PHOTOGRAPHY Ezra Wolfinger Jeremy Gonzalez
ONLINE EDITOR/COLORIST Jim Ferguson
SOUND MIX Jim Sullivan
ANIMATION Mitch Butler
ARCHIVAL MATERIALS ABC News AP Archive Austin American Statesman CBC CBS LA CBS News Downtown Seattle Association Fox News Getty Images King County Television KIRO KTVB KVUE MSNBC NBC News The Microsoft Corporation Newshour Productions LLC Pond5 Providence Regional Medical Center The Sun Rob Tinworth The Seattle Channel Shutterstock TVW WCVB WDID
Original funding for this program was provided by public television stations, Corporation for Public Broadcasting, John D. and Catherine T. MacArthur Foundation, Ford Foundation, Abrams Foundation, Park Foundation, John and Helen Glessner Family Trust, FRONTLINE Journalism Fund with major support from Jon and Jo Ann Hagler.
FOR FRONTLINE
PRODUCTION MANAGER Megan McGough Christian
SENIOR PROMOTION PRODUCER Missy Frederick
SENIOR EDITOR Barry Clegg
PRODUCTION COORDINATOR Brenna Verre
ASSISTANT EDITOR Joey Mullin
POST PRODUCTION ASSISTANT Tessa Maguire
FOR WGBH OUTPOST
EDITOR Deb Holland
SENIOR DIRECTOR OF PRODUCTION TECHNOLOGY Tim Mangini
INTERNS Juliet Fusco William Gao Colleen Martin Ana Mundaca Olivia Muse Zoe Salvucci Collyn Stephens Isabelle Truong
SERIES MUSIC Mason Daring Martin Brody
EXECUTIVE ASSISTANT Will Farrell
OUTREACH SPECIALIST Joshua Rae
IMPACT PRODUCER Erika Howard
DIGITAL WRITER & AUDIENCE DEVELOPMENT STRATEGIST Patrice Taddonio
DATA ANALYST Ben Abrams
SERIES PUBLICITY MANAGER Anne Husted
DIGITAL PRODUCTION ASSISTANT Lucie Sullivan
PODCAST PRODUCER James Edwards
SERIES PODCAST PRODUCER Max Green
ARCHIVES & RIGHTS MANAGER John Campopiano
FOR WGBH LEGAL Eric Brass Jay Fialkov Janice Flood
SENIOR CONTRACTS MANAGER Gianna DeGiulio
BUSINESS MANAGER Sue Tufts
BUSINESS DIRECTOR Mary Sullivan
SENIOR DEVELOPER Anthony DeLorenzo
LEAD DESIGNER FOR DIGITAL Dan Nolan
FRONTLINE/COLUMBIA JOURNALISM SCHOOL FELLOWSHIPS
ABRAMS JOURNALISM FELLOW Zoe Todd
TOW JOURNALISM FELLOW Karen Pinchin
FRONTLINE/NEWMARK JOURNALISM SCHOOL AT CUNY FELLOWSHIP Shantal Riley
EDITORIAL CONSULTANT Lauren Prestileo
ASSOCIATE PRODUCER Marcia Robiou
DIGITAL REPORTER Katie Worth
DIGITAL REPORTER & PRODUCER Priyanka Boghani
DIGITAL CONTENT CREATOR Miles Alvord
ABRAMS FILMMAKER IN RESIDENCE Ben C. Solomon
SERIES PRODUCER AND EDITOR Michelle Mizner
INVESTIGATIVE PRODUCER Daffodil Altan
EDITORIAL COORDINATING PRODUCER Katherine Griwert
POST COORDINATING PRODUCER Robin Parmelee
SENIOR EDITOR AT LARGE Louis Wiley Jr
FOUNDER, EXECUTIVE PRODUCER AT LARGE David Fanning
SPECIAL COUNSEL Dale Cohen
SPECIAL PROJECTS EDITOR Philip Bennett
SENIOR STORY EDITOR Lauren Ezell Kinlaw
DIRECTOR OF DIGITAL VIDEO Carla Borras
SENIOR DIRECTOR OF STRATEGY & AUDIENCE Pam Johnston
SENIOR PRODUCERS Dan Edge Frank Koughan
SENIOR EDITOR & DIRECTOR OF LOCAL PROJECTS Sarah Childress
MANAGING EDITOR Andrew Metz
MANAGING DIRECTOR Jim Bracciale
EXECUTIVE PRODUCER Raney Aronson-Rath
A FRONTLINE Production with Mobias Media, Inc.
© 2020 WGBH Educational Foundation All Rights Reserved
FRONTLINE is a production of WGBH/Boston and is solely responsible for its content.
Explore
Policies
Teacher Center
Funding for FRONTLINE is provided through the support of PBS viewers and by the Corporation for Public Broadcasting, with major support from Ford Foundation, and The Fialkow Family Foundation. Additional funding is provided the Abrams Foundation, Park Foundation, John D. and Catherine T. MacArthur Foundation, Heising-Simons Foundation, and the FRONTLINE Trust, with major support from Jon and Jo Ann Hagler on behalf of the Jon L. Hagler Foundation, and Corey David Sauer, and additional support from Koo and Patricia Yuen. FRONTLINE is a registered trademark of WGBH Educational Foundation. Web Site Copyright ©1995-2025 WGBH Educational Foundation. PBS is a 501(c)(3) not-for-profit organization.



















