November 18, 2023 - PBS News Weekend full episode
11/18/2023 | 26m 45sVideo has Closed Captions
November 18, 2023 - PBS News Weekend full episode
November 18, 2023 - PBS News Weekend full episode
Problems playing video? | Closed Captioning Feedback
Problems playing video? | Closed Captioning Feedback
Major corporate funding for the PBS News Hour is provided by BDO, BNSF, Consumer Cellular, American Cruise Lines, and Raymond James. Funding for the PBS NewsHour Weekend is provided by...

November 18, 2023 - PBS News Weekend full episode
11/18/2023 | 26m 45sVideo has Closed Captions
November 18, 2023 - PBS News Weekend full episode
Problems playing video? | Closed Captioning Feedback
How to Watch PBS News Hour
PBS News Hour is available to stream on pbs.org and the free PBS App, available on iPhone, Apple TV, Android TV, Android smartphones, Amazon Fire TV, Amazon Fire Tablet, Roku, Samsung Smart TV, and Vizio.
Providing Support for PBS.org
Learn Moreabout PBS online sponsorshipJOHN YANG: Tonight on PBS News Weekend, new airstrikes killed dozens across Gaza and the West Bank today, as the Israeli military search of Gaza's biggest hospital forces hundreds to flee.
Then as U.S. funding for Ukraine stalls on Capitol Hill, the humanitarian situation of the war torn country gets worse.
WOMAN: It's become a daily reality for this generation of violence, trauma, destruction and displacement.
JOHN YANG: And how nurse practitioners are filling a much needed healthcare gap and a push to allow them to provide care without a physician's oversight.
(BREAK) JOHN YANG: Good evening, I'm John Yang.
In Gaza tonight more Palestinians are on the move as restored communications have allowed the United Nations to resume critical aid deliveries.
Israel is again urging Palestinians in northern Gaza to go south and patients, staff and displaced people are leaving Gaza's biggest hospital amid conflicting claims about what's triggering the departure.
JOHN YANG (voice-over): On Gaza's main road south (inaudible) can confusion.
Palestinians fled out Al-Shifa Hospital in Gaza City after doctors say Israel ordered an evacuation.
Al shifa physician Ramez Radwan.
RAMEZ RADWAN, Doctor (through translator): In the last moments, the Israeli authorities warned whoever was inside the hospital had to leave except the wounded, the surgeon and some of the medical and nursing staff.
JOHN YANG (voice-over): The Israeli Defense Forces denied that they ordered anyone to leave.
They say the hospital asked them to help those who wanted to leave voluntarily.
The Palestinian health minister said five doctors are staying to care for the remaining 120 or so patients, including some in intensive care and some premature babies.
The minister called on international aid organizations to help transport the infant's to Egypt.
MAI AL-KAILA, Palestinian Health Minister (through translator): The Israeli forces are damaging all wards of the hospital and the hospital has become a military base for the occupation forces.
JOHN YANG (voice-over): And the United Nations said Israeli airstrikes killed dozens of people at a U.N. run school that had served as a shelter for thousands of displaced Palestinians.
The IDF is urging civilians to move to southern Gaza where there is little refuge when the war, Israeli airstrikes hit Huda Mubasher's home where she lived with her husband, daughter and two cats.
HUDA MUBASHER, Gaza Resident (through translator): Suddenly, something fell on us and I found stones in my mouth.
I couldn't breathe or speak.
JOHN YANG (voice-over): In the West Bank city of novelists a funeral procession for victims of an Israeli airstrike in which the Palestinian Red Crescent said five people were killed.
The IDF said it was targeting a terrorist hideout inside the Balata refugee camp.
2,000 miles away in Abu Dhabi, eight injured children and their families arrived from Gaza for medical treatment.
The United Arab Emirates has pledged to care for 1,000 injured Palestinians.
Somaya Taher is pregnant and lost her husband and an airstrike.
Her young son was badly burned.
SOMAYA TAHER, Gazan Refugee (through translator): Thank God we are here the situation was getting worse.
It's difficult to explain.
There's nothing like it experiencing the difficulties of life in Gaza.
JOHN YANG: Elon Musk's SpaceX got its biggest rocket off the ground in a test launch today, but a pair of explosions just minutes into the flight destroyed both the booster rocket and the spacecraft.
SpaceX officials say it appears the crafts self-destruct system blew it up over the Gulf of Mexico after liftoff from South Texas.
The flight lasted only about eight minutes that's twice as long as the first test in April which also ended with an explosion.
And Elon Musk got more bad news today as Comcast joined the list of advertisings stepping away from his social media platform X formerly known as Twitter over concerns that their ads were showing up next to antisemitic content of the company's pausing their ads on X include IBM, Disney and Paramount global.
Musk has been accused of tolerating and even encouraging antisemitic messages on X.
He drew fire earlier this week for agreeing with a post accusing Jews of hating white people.
Still to come on PBS News Weekend, the growing need for nurse practitioners and the fight over how they provide care and the spread of mosquitoes and the diseases they carry.
(BREAK) JOHN YANG: In a Washington Post op-ed today, President Biden urged support for Ukraine.
He's asked Congress for tens of billions of dollars to support the nation and its war with Russia.
Most of that would be military aid, but it also includes money to address the humanitarian situation which as Ali Rogin tells us gets worse by the day.
ALI ROGIN: As Russia increases its attacks on critical infrastructure in Ukraine, some 18 million Ukrainians, about 40 percent of the population are in need of humanitarian aid.
Humanitarian organizations on the ground are working in a hostile environment, trying to help civilians caught in the crossfire who are searching for safe haven.
And those groups are concerned that support for their mission in the international community is flagging.
Zoe Daniels is the Senior Director for the Ukraine crisis at the International Rescue Committee, a humanitarian organization.
Zoe, thank you so much for joining us.
Can you first take us through what are the most pressing humanitarian needs right now in Ukraine?
ZOE DANIELS, Senior Director, International Rescue Committee: So really, as you said, heavy fighting carries on, particularly in the southeast of the country.
It's damaging homes, hospitals, schools, other civilian infrastructure and really driving those humanitarian needs.
I'm in an area of Ukraine, approximately the size of Florida is now riddled with landmines, which nearly two years into a full scale war.
And after 10 years of conflict in eastern Ukraine, people's ability to cope is severely weakened.
We've got alarming statistics about the massive mental health impact of the war, including the rise of intimate partner violence at home.
4.1 million children inside Ukraine need humanitarian aid.
It's become a daily reality for this generation of violence, trauma, destruction and displacement.
Children are being killed and wounded.
They're deeply traumatized by violence, which leaves really long lasting scars.
It's really affected their future.
There's been prolonged disruption posed by the war and then before that, there was the preceding COVID-19 pandemic.
And so this is four years of educational challenges for students.
They have been displaying clear signs of extensive learning and psychosocial setback, attacks on schools, really deprived children of safe spaces to learn, leave some very distressed from February '22 when the invasion started through to October '23, 3,428 educational facilities have been damaged, 365 completely destroyed.
So 11 percent of young people lack access to quality education.
ALI ROGIN: I know you've also been tracking the impact on students who have been displaced outside of Ukraine refugees elsewhere in Europe, how are they faring?
ZOE DANIELS: So for example, if you look at the refugees and Ukrainian refugees in Poland, more than half of those Ukrainian refugee children are not enrolled in schools in Poland, many children participate in distance learning, either because they've been enrolled in schools that were damaged or reside in areas of active hostility, or because they can't travel to other schools due to distance or lack of access to transportation.
So, some but not all distance learning involves online classes, then, sometimes they're subjected to electricity and internet outages.
So that disrupts learning as well.
ALI ROGIN: We're entering the second winter period of this fallout invasion.
How do you anticipate the changing seasons to impact the effects of war on the civilian community?
ZOE DANIELS: The prediction this year is that Ukraine is going to be battling with even more severe winter than last year.
Previously, we're in homes and power grids from last winter have not been fully repaired as temperatures plummet.
We anticipate that Ukraine is going to really suffer from intensified beverages of missile strike and even more widespread destruction.
So this combination of ongoing armed conflict this destroyed infrastructure in harsh weather conditions will make life incredibly tough for people in affected areas.
ALI ROGIN: Are you concerned that international attention is turning away from Ukraine, ZOE DANIELS: There's always competing priorities in the world and the humanitarian response plan for Ukraine is only funded at 46 percent, even though for example, the United States has outstanding he contributed 2.6 billion in life saving humanitarian aid, which really helped Ukrainians to the constant shelling last year's harsh winter.
The needs are currently estimated at 3.95 billion USD, which, you know, currently, humanitarian funding to Ukraine is half of what it was in 2022.
There's political will in the country and among key allies, that really remains high.
But funding shortages really hamper humanitarian stability to assist more people.
ALI ROGIN: Zoe Daniels with the International Rescue Committee, thank you so much for your time.
ZEO DANIELS: Thank you.
JOHN YANG: A fourth of all medical visits are now provided by non-physicians.
A lot of that's due to the growing number of nurse practitioners who are filling critical health care gaps, but nurse practitioners say their work is hampered by outdated restrictions on their ability to provide care without physician supervision and collaboration with the global health reporting center and with support from the Pulitzer Center.
Stephanie Sy reports from Ohio for our series, critical care the future of nursing.
WOMAN: I can fill it with us on this side.
STEPHANIE SY (voice-over): Lois Prunty, a food service worker in her mid30s first came to the Total Health and Wellness Clinic at Ohio State East Hospital three years ago.
It was one of the few providers in the area that took her Medicaid plan.
LOIS PRUNTY, Patient, Total Health and Wellness: I think is excellent care.
STEPHANIE SY (voice-over): The care at this federally qualified health center is also unique.
It's led entirely by nurse practitioners or NPs.
These nurses have graduate degrees and anywhere from 500 to more than 3,000 hours of supervised clinical training.
Beyond the preparation of a standard bedside nurse, they can diagnose conditions, order and perform tests and prescribe medication.
Candy Rinehart is the director of the clinic located in Columbus.
CANDY RINEHART, Director, Total Health and Wellness, Ohio State University: From the very beginning, we had a pharmacist, a social worker, a Mental Health Counselor, registered nurses who do case management, and that's the approach we take in nursing as we're looking at the whole person and how they're being cared for.
STEPHANIE SY (voice-over): Total Health and Wellness Clinic sees patients regardless of their ability to pay, filling a critical gap in care.
LOIS PRUNTY: I didn't have a regular doctor in years, certain places you only take certain insurances and stuff like that, because I know I got turned away from a doctor I got recommended to because they didn't accept my insurance.
So I had to go back to square one.
STEPHANIE SY (voice-over): The nurse practitioner role was created in the 60s due to a need to increase patient's access to care.
Even before the COVID era, nearly two dozen states allowed NPs to practice on their own without physician supervision.
NPs call this full practice authority.
And the movement has picked up steam since the pandemic with four more states granting full practice authority to NPs.
But national physician groups warn that nurse practitioners are veering into their lane and risking patient safety.
That's not true, says Candy Rinehart.
CANDY RINEHART: For the most part, you know, we collaborate constantly with specialists.
If a person needs to be sent to a nephrologist, then, you know, you collaborate with that nephrologist.
So we all stay in our lane as far as what we are educated to do, and work together.
STEPHANIE SY (voice-over): Still in Ohio and 22 other states, NPs can't provide care without mandated physician oversight.
NPs must secure what are known as collaborative practice agreements.
Tying nurse practitioners to a physician in their specialty.
Jennifer Gross is an NP and also a state lawmaker.
JENNIFER GROSS, Ohio State Representative and Nurse Practitioner: Having been a nurse practitioner board certified since 2005.
I've carried that at every turn, in order to practice.
So if we practice without one of those we will be fined and our license can be removed.
STEPHANIE SY (voice-over): The Ohio State Medical Association which opposes any change to the current arrangement wouldn't comment for this story.
But Marc Parnes would.
He's a retired OB/GYN who still manages a medical practice in Columbus.
DR. MARC PARNES, Retired Board-Certified OB/GYN: My bias is knowing how lovely that coordinated care of a physician and a nurse practitioner can be working together.
STEPHANIE SY (voice-over): He says that even with their expanded training, NPs typically have fewer hours of clinical practice than physicians do.
MARC PARNES: There's an art to medicine.
And it's not that nurse practitioners can't practice it, they definitely can.
But there are different levels of developing that art and different opportunities to develop it.
STEPHANIE SY: How do you decide at what point you really need to see a primary care physician with all those thousands of hours of residency versus being okay, with seeing an advanced practitioner?
MARC PARNES: I think initially, it would be access.
And so that is one of the things I like about having more and more nurse practitioners is it increases the access.
STEPHANIE SY (voice-over): But Gross says the state's restrictions on NPs makes it harder for ordinary Ohioans to access health care.
JENNIFER GROSS: Let's talk about our elderly.
Let's talk about our Medicaid.
We're one of the -- we're a Medicaid expansion state.
Those patients that are Medicaid and Medicare have better access to care when nurse practitioners are not required to have collaborative agreements.
STEPHANIE SY: Nurse practitioners in rural areas say they're especially impacted by laws mandating physician collaboration, and studies show that when allowed to practice independently, not only does access to care improve, but patient outcomes are no worse off, and in some cases better.
STEPHANIE SY (voice-over): Over 2 million Ohioans roughly 20 percent live in areas that suffer a shortage of primary care professionals.
ELISHA CLARK, Nurse Practitioner, Clark Family Practice: Health care access before I started my practice here was pretty scarce and few between/ STEPHANIE SY: The quaint village of Byesville is in rural southeastern Ohio.
Elisha Clark, graduated from the local high school has been a nurse practitioner for 12 years in the area and opened her own practice in January.
ELISHA CLARK: That was my main goal in life to open a facility where patients feel like they're an extended family.
STEPHANIE SY (voice-over): But she cites the collaborative agreement as a major hurdle.
ELISHA CLARK: First, you have to find someone that you trust and that trusts you.
And then you have to talk to them about what kind of details they require in order to sign a physician agreement with you.
STEPHANIE SY: How long did it take to find that person?
ELISHA CLARK: A little over a year.
STEPHANIE SY: What does the collaboration look like?
Is this somebody that you consult with regularly?
ELISHA CLARK: No, this is someone that has to be present in some way, shape or form for you to contact if you have a question about something.
And this is someone that you generally have to pay.
STEPHANIE SY (voice-over): Clark says her collaborating physician is in his 70s, making her ability to provide care long term uncertain.
ELISHA CLARK: I have a little over 1,600 patients that are seeing me.
So if he God forbid has some health issue or if he retires, we are in a great bind here for the health care of Guernsey County.
STEPHANIE SY: What would happen exactly?
ELISHA CLARK: I would immediately have to within 30 days find a different physician agreement partner to have signed a contract with me, STEPHANIE SY (voice-over): She and other NPs say the requirement is also a financial burden.
JENNNIFER GROSS: You have to enter into an agreement with a physician that would cost you about $500 to roughly $5,000 a month.
So, you can see that that's pretty cost prohibitive.
Those costs are then passed on to the patient.
STEPHANIE SY (voice-over): 71-year-old Susie Khune has been seeing Clark for several years, moving with her to her private practice when she opened up and Byesville.
SUSIE KHUNE, Patient, Clark Family Practice: That was one of my biggest complaints about some of the doctors that I have seen previously, that they asked you a question and then they answered it before you get a chance to.
She listens.
And then she goes through the options with you not saying do this, do this.
You decide together with Elisha.
STEPHANIE SY (voice-over): She and her adult children are all patients of Clark for primary care.
STEPHANIE SY: What would you guys do that if the practice was forced to close because she couldn't find a physician to, you know, collaborate with her?
SUSIE KHUNE: It's scary.
I didn't realize it until earlier.
I can't imagine going having to go to someone else besides Elisha.
STEPHANIE SY (voice-over): She's worried about losing that listening ear and that choice for her own health care.
For PBS News Weekend, I'm Stephanie Sy in Ohio.
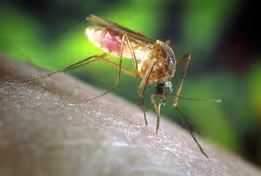
JOHN YANG: With that annoying buzzing your ear the itching bite that leads to frenzied scratching.
For many of us here in the United States mosquitoes are merely a summertime nuisance.
But Ali Rogin is back to tell us that around the world, mosquitoes and the diseases they carry are a growing public health concern.
ALI ROGIN: The tiny mosquito is responsible for more deaths than any other animal, killing billions over the course of human history.
Mosquitoes transmitting malaria killed more than 600,000 people in 2021.
In that same year, another 247 million people were infected.
Now these deadly vectors of disease are expanding their reach, showing up in parts of the world never seen before.
A new multi-part investigation by the New York Times looks at the global fight against mosquito borne diseases, and how years of progress in that battle have been reversed.
Stephanie Nolan covers global health for the New York Times, and spent a year tracking mosquitoes and the diseases they carry.
Stephanie, thank you so much for joining us.
As we just mentioned, humans, we're winning the war against malaria, against mosquito borne diseases for so long.
But you write in this series that now mosquitoes are winning, what changed?
STEPHANIE NOLAN, Global Health Reporter, The New York Times: What changed is that mosquitoes are crafty, Ali.
They evolve very quickly.
Every generation of mosquito has lots of mutations, it means that they're very good at developing resistance, the things that we come up with to kill them.
So mosquitoes around the globe are resistant to the insecticides.
And so every time we come up with something that we think is going to be the silver bullet to fight back, mosquitoes get around it.
And of course, the time differences in mosquito generation is six or 710 weeks, whereas designing testing and bringing to market and anti-mosquito product generally takes a minimum of 10 years.
ALI ROGIN: It does seem though, that mosquitoes are getting seemingly even more impervious to these efforts.
Have we hit a real perfect storm here?
STEPHANIE NOLAN: No, I don't think so.
And I'll tell you after a year of looking at this, I'm still kind of hopeful.
I think you're really right to be you know, striking a note of alarm, because we're seeing mosquitoes that carry viruses like Dengue fever and Chikungunya turning up in places like France and the southern United States that have never had that problem.
I wrote about an invasive mosquito from Asia that's now gone into Africa and is threatening African cities with malaria, which maybe doesn't sound so shocking, except that malaria is a rural problem in Africa, not an urban one.
And so this puts hundreds of millions of new people at risk.
But in places that don't have the infrastructure to respond, because of climate change, you're seeing dangerous mosquito species adapting to live in all kinds of new places.
And I also looked at Big Picture projects at big efforts.
One of them is genetic modification of mosquitoes so that they wouldn't be able to transmit disease, those kinds of strategies that might work for multiple diseases and in multiple places.
Those are the ones that I think, keep me from completely panicking.
ALI ROGIN: And you mentioned how some of these diseases Dengue gay have shown up in the United States.
In Florida there were nine cases of malaria reported in U.S. states this last summer, how is it and why that this disease has made it to the United States to this degree?
STEPHANIE NOLAN: So you know, nine cases is maybe not yet a cause for panic.
I would say that, that those malaria outbreaks are like a tiny little like just a little, hey, you should be paying attention to this because we're starting to lose the grip do I think there's going to be tens of thousands of malaria cases in the US south within the next couple of years?
I don't.
What's really interesting to me about U.S. malaria, and the way that it reminded people that there is an issue is that it makes us think about how did we get rid of malaria in the U.S., right?
Ultimately, what made a difference was where people lived relocating communities out of swampy vulnerable places, and making sure that people had adequate housing that protected them, we spend more than $22 billion a year fighting mosquitoes.
So, we could continue to pour money into those things, new chemicals, more poisons, more poisons, or we can talk about what kind of investment it would take to get the people who are currently vulnerable into the same kinds of standards of housing that protected people in the U.S. south who used to live in malarial zones.
ALI ROGIN: Who are the people that are the most vulnerable here?
STEPHANIE NOLAN: I would say to malaria.
It's as always, it's the poorest people in the poorest places.
Tanzania has one of the highest malaria burdens in the world.
80 percent of the cases in Tanzania take place in the people who live in the 10 percent lowest quality of housing, right.
So poorest people, poorest places.
Dengue fever and the arboviruses I think are going to be an interesting one to watch Dengue Zika yellow fever Chikungunya, the mosquito that carries them is not you know, biting people in fact houses in rural in Tanzania.
It lives happily in cities.
It'll live on the balcony of your chic apartment building in Miami, it will breed our, you know, around your house, it will live in your closet.
And so it has a much more equalizing effect in lots of ways.
Many of us are either now or soon to be vulnerable to these mosquitoes.
ALI ROGIN: Stephanie Nolan with the New York Times.
Thank you so much for your time.
STEPHANIE NOLAN: It's a pleasure.
JOHN YANG: And that is PBS News Weekend for this Saturday.
I'm John Yang.
For all of my colleagues, thanks for joining us.
See you tomorrow.
In Ohio, a fight over how nurse practitioners provide care
Video has Closed Captions
In Ohio, nurse practitioners push to lift restrictions on how they provide care (8m 45s)
More Gazans flee south as IDF searches Al Shifa Hospital
Video has Closed Captions
More Palestinians flee south as Israeli troops search Gaza’s largest hospital (2m 31s)
Ukraine’s humanitarian crisis worsens as U.S. funding stalls
Video has Closed Captions
Humanitarian crisis in Ukraine worsens as U.S. funding stalls (5m 19s)
Why the threat of mosquito-borne diseases is on the rise
Video has Closed Captions
Why the threat of mosquito-borne diseases is on the rise worldwide (5m 32s)
Providing Support for PBS.org
Learn Moreabout PBS online sponsorship
- News and Public Affairs

FRONTLINE is investigative journalism that questions, explains and changes our world.

- News and Public Affairs
Today's top journalists discuss Washington's current political events and public affairs.












Support for PBS provided by:
Major corporate funding for the PBS News Hour is provided by BDO, BNSF, Consumer Cellular, American Cruise Lines, and Raymond James. Funding for the PBS NewsHour Weekend is provided by...